Breast Uplift (Mastopexy) in Turkey




- Breast Uplift (Mastopexy) restores shape and nipple position with technique matched to ptosis grade.
- Transparent safety-first pathway covers anaesthesia options, monitoring, realistic risks, and structured follow-up.
- Recovery timeline you can plan from 6 weeks to 1 year, with scar maturation and return-to-activity guidance.
- Premium value for UK patients through all-inclusive planning, travel coordination, and HBOT/LLLT recovery support.
AI-generated summary, fact-checked by our medical experts.
Breast Lift (Mastopexy): Quick Facts
Duration of Surgery
Type of Anaesthesia
Initial Recovery Period
Hospital Accommodation
Return to Daily Activities
Breast Lift (Mastopexy) Results: Before and After
Breast Uplift (Mastopexy) is not about changing who you are. It is about restoring proportion, position, and balance when time, pregnancy, weight changes, or genetics have shifted the breast shape.
We write this guide for the UK “expert patient”. You want clinical clarity, not vague promises. Fair.
Our approach is simple: rejuvenation, not alteration. The goal is a lifted, natural-looking result that still looks like you.
- What mastopexy is (and what it is not)
- How breast ptosis is assessed and graded
- Which clinical details matter when choosing a technique
Table of Contents
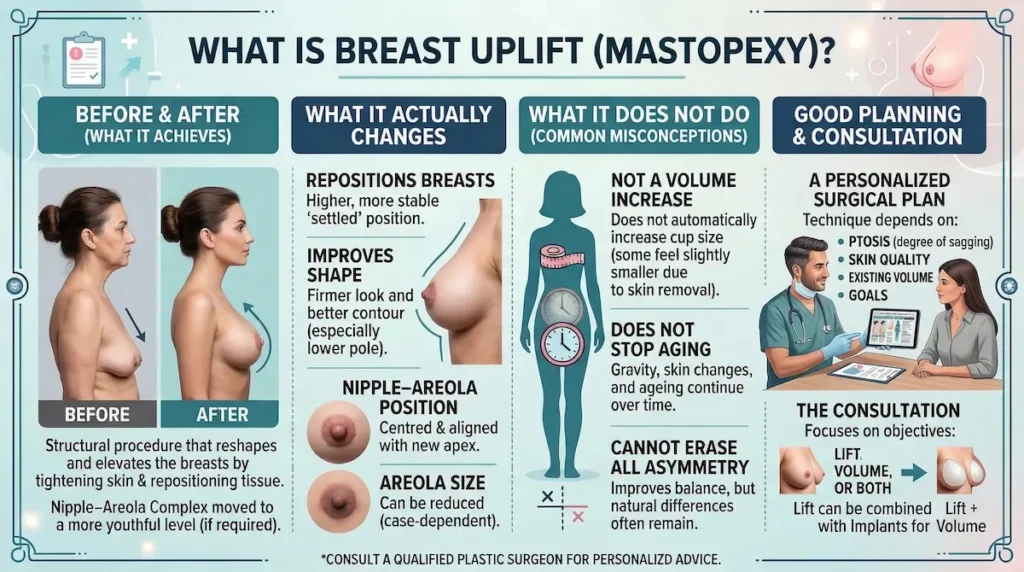
What Is Breast Uplift (Mastopexy)?
A Breast Uplift (Mastopexy) reshapes and elevates the breasts by tightening the skin envelope and repositioning breast tissue to a more youthful level. When required, the nipple–areola complex is moved to match the new breast apex. It is designed to improve position and proportion, not automatically increase cup size. Technique selection depends on your breast ptosis, skin quality, and goals, which is why a personalised surgical plan matters. Some patients combine a lift with implants for volume.
Definition (clear, clinical, no fluff)
A breast uplift (mastopexy) is a surgical procedure that reshapes and lifts the breast by tightening the skin envelope and repositioning breast tissue. When needed, it also repositions the nipple–areola complex to a more youthful level. The aim is improved shape and proportion, not a “bigger” breast.
What mastopexy actually changes
Mastopexy is a structural operation. We work with the breast skin, glandular tissue, and supporting framework to improve the breast’s position on the chest wall.
- Breast position: a higher, more stable “settled” position on the chest
- Shape: improved contour and a firmer look (especially in the lower pole)
- Nipple–areola position: centred and aligned with the new breast apex, where appropriate
- Areola size: can be reduced if it has stretched (case-dependent)
Good planning matters. We consider symmetry, skin quality, existing breast volume, and the degree of ptosis before selecting the surgical pattern.
What mastopexy does not do (common misconceptions)
A lift is not the same as an augmentation. If your primary issue is volume loss (especially upper pole fullness), a lift alone may not deliver the “filled” look you have in mind.
- It does not reliably increase cup size. Some patients appear slightly smaller after a lift because excess skin is removed and the breast is reshaped.
- It does not stop ageing. Gravity, skin quality, and life changes still apply over time.
- It cannot erase all asymmetry. We can improve balance, but natural differences often remain.
This is why the consultation should focus on objectives: lift, volume, or both. When volume is central, combining mastopexy with implants or fat transfer can be discussed later in the guide.
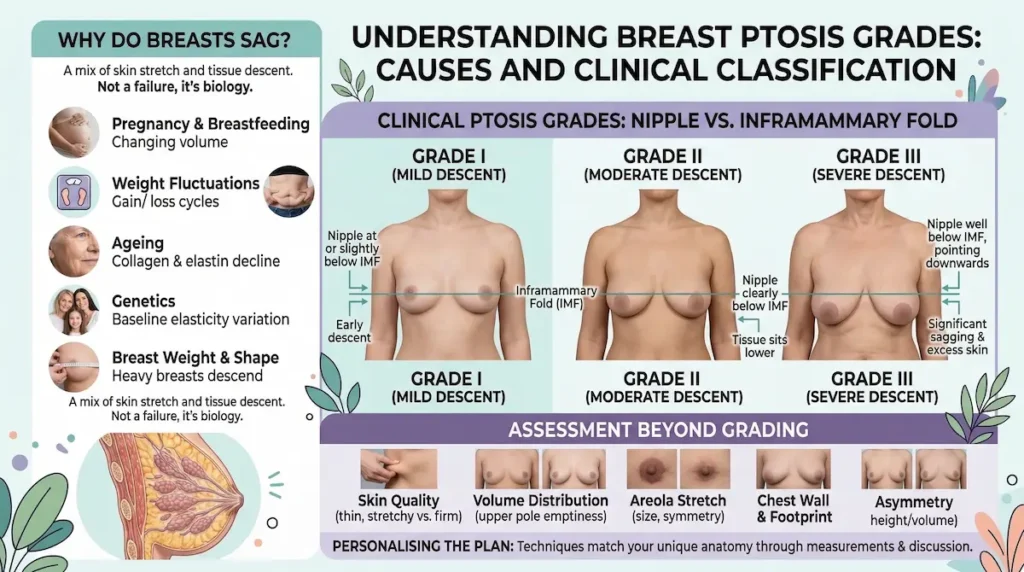
Why Do Breasts Sag? Understanding Breast Ptosis Grades
Breasts sag when the skin and supporting structures stretch over time—commonly after pregnancy, breastfeeding, weight change, ageing, or genetics. Clinically, we assess breast ptosis by comparing nipple position to the inframammary fold. Grade I is mild descent, Grade II moderate, and Grade III more advanced with downward-pointing nipples. This grading guides whether a periareolar, vertical “lollipop”, or Wise pattern “anchor” mastopexy is most appropriate. Skin quality and asymmetry further refine the technique choice.
Why ptosis happens (it is usually multi-factorial)
Breast sagging is typically a mix of skin stretch and tissue descent. It is not a “failure” of willpower. It is biology.
- Pregnancy and breastfeeding: changes in volume can stretch the skin envelope
- Weight fluctuation: repeated gain/loss cycles can thin and loosen skin support
- Ageing: collagen and elastin quality decline, affecting firmness
- Genetics: baseline skin elasticity and breast tissue density vary widely
- Breast weight and shape: heavier breasts can descend more over time
Ptosis grading: the clinical framework
If you have been searching breast ptosis anatomy, you have likely seen grading systems. They are not academic trivia. They shape the surgical plan.
In simple terms, grading is assessed by the nipple position relative to the inframammary fold (the crease under the breast), and how much of the breast sits below that fold.
- Grade I (mild): the nipple is at or just below the fold, with early descent
- Grade II (moderate): the nipple sits clearly below the fold, and the breast tissue hangs lower
- Grade III (severe): the nipple is well below the fold and points downward, with significant excess skin and tissue descent
Higher grades usually require stronger reshaping and more comprehensive scar patterns. Lower grades may be suitable for limited-scar approaches, depending on skin quality and goals.
How we assess you (beyond a single “grade”)
Ptosis is only one variable. Two people can have the same grade and need different surgical strategies.
- Skin quality: thin, stretchy skin behaves differently during healing
- Breast volume distribution: upper pole emptiness vs lower pole heaviness
- Areola stretch: size, shape, and symmetry considerations
- Chest wall and breast footprint: where the breast naturally “sits” on your frame
- Asymmetry: differences in fold height, nipple position, and tissue volume
The outcome should look intentional, not forced. That starts with measurements, honest discussion, and a technique that matches your anatomy.
Share your photos and medical history to receive a personalised assessment from our European Board-certified facial surgery team.
Benefits of Breast Uplift (Mastopexy): what changes (and what stays natural)
A breast uplift is often described as a “lift”, but the benefit is more specific than that. We are restoring proportion between the nipple position, the breast footprint, and your chest wall. Done well, it looks like you. Just more balanced.
There is also a practical side. Bras sit differently. Clothing fits more predictably. Some patients simply feel less “pulled down” by their own breast weight.
Our philosophy stays consistent: rejuvenation, not alteration. The goal is a natural correction, not a dramatic reinvention.
1) Aesthetic benefits: position, shape, and proportion
The headline benefit is a higher breast position with a better-defined shape. How that looks on you depends on your starting volume, your skin quality, and the degree of ptosis.
- Improved breast position: the breast sits higher and feels more supported
- Refined contour: less “bottoming out” and a more stable lower pole
- Nipple–areola alignment: repositioned to match the new breast apex, when appropriate
- Areola proportion: can be adjusted if stretched (case-dependent)
For many UK patients, the preference is subtle. We plan for a result that looks proportionate in real life, not only in a mirror at home.
2) Practical benefits: bras, exercise, and day-to-day comfort
Not every benefit is purely aesthetic. When the breast sits lower, straps often do more work than they should, and fit can become unpredictable.
- Bra fit: improved cup positioning and less “spillage” from shape mismatch
- Wardrobe comfort: necklines and dresses often sit more evenly
- Movement: reduced tugging sensation in some patients, especially after weight loss
We will still be direct: a lift is not a cure for breast heaviness if your core issue is volume. In that scenario, reduction or reshaping strategies may be part of the plan.
3) The “natural look” benefit: results that do not announce themselves
Expert patients tend to care about one thing above all: credibility. The best surgical work should not look surgical.
“The best result is the one that looks unforced. People should notice you look well, not that you have had surgery.”
This is why we focus on structural planning rather than skin tension. Skin-only tightening can look neat early on, then relax in the wrong direction.
Answer a few brief questions about your concerns, health, and goals to discover which treatment options may suit you best.
Am I A Suitable Candidate For A Breast Lift?
Suitability is not a box-ticking exercise. It is a balance of anatomy, health, and the outcome you are actually trying to achieve. Some people need a lift to correct position. Others primarily need volume restoration. A few need both.
We start with your goals, then we map them to clinical reality. That means we assess ptosis grade, skin quality, breast volume distribution, and asymmetry in the same conversation.
We also assess safety. A well-planned mastopexy should feel predictable, from the anaesthetic plan to the aftercare schedule.
1) When mastopexy is usually a good fit
You are typically a strong candidate when the main issue is descent of the breast and nipple position, rather than a desire for a significantly larger breast.
- Visible ptosis: mild to severe sagging, with or without areola stretch
- Post-pregnancy or post-breastfeeding changes: shape change after volume fluctuation
- Weight-loss changes: skin laxity and loss of structural “hold”
- Stable weight: better predictability for long-term shape
If you want a fuller upper pole as the main priority, we may discuss a lift combined with augmentation or fat transfer later in this guide.
Our surgical dates fill up quickly due to high international demand. Secure your consultation today to arrange your preferred travel dates.
2) Who should postpone, or approach with extra caution
Some factors increase risk or make results less predictable. In those cases, we usually slow down and plan properly rather than rushing into surgery.
- Smoking or nicotine use: it can impair circulation and wound healing
- Unstable weight: major changes after surgery can affect the result
- Planned pregnancy in the near term: pregnancy can change breast tissue and skin again
- Uncontrolled medical conditions: your safety comes first
We will also review supplements and medications that may affect bleeding or recovery. If your GP is involved in your ongoing care, that context helps.
3) What we check before confirming your surgical plan
Expert patients appreciate process. So do we. Before we confirm a plan, we look at the details that determine both safety and aesthetics.
- Your anatomy: ptosis grade, skin quality, breast footprint, and asymmetry
- Your objective: lift only, volume change, or a combined approach
- Your healing profile: scarring tendency, lifestyle factors, and support at home
- Your expectations: a realistic outcome that matches what surgery can do
If the goal and the method do not match, we say so. That is not pessimism. It is precision.
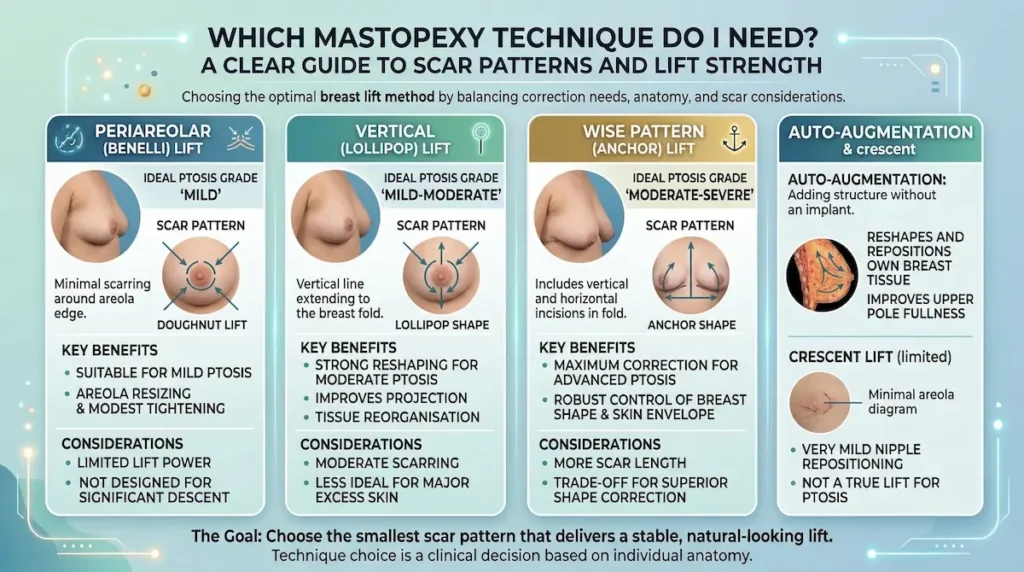
Which Mastopexy Technique Do I Need? A clear guide to scar patterns and lift strength
If you are researching mastopexy techniques, you are already thinking like an expert patient. Good. Technique choice is not a “preference”. It is a clinical decision based on ptosis grade, skin quality, breast volume distribution, and how much reshaping is required.
The trade-off is simple: the more correction we need, the more structured the scar pattern tends to be. The goal is to choose the smallest scar pattern that can still deliver a stable, natural-looking lift.
We also plan for longevity. A lift that relies on skin tension alone can relax in the wrong direction over time. We focus on reshaping the breast tissue first, then closing without forcing the skin.
Below is how the main techniques differ, and why the “right” answer depends on anatomy.
Benelli (periareolar) approach: when the correction is limited
Benelli mastopexy (often called a periareolar or “donut” lift) places the incision around the areola. It can suit mild ptosis and areola stretch when you need modest elevation and modest tightening.
- Best for: mild ptosis, areola resizing, small shape refinements
- Limitations: limited lift power; risk of areola widening in some skin types
- Reality check: it is not designed for significant descent
Vertical (“lollipop”) lift: the workhorse for balanced reshaping
Vertical scar mastopexy is often chosen for moderate ptosis because it provides stronger reshaping without the full anchor scar. It uses an incision around the areola plus a vertical line down to the fold.
- Best for: moderate ptosis, meaningful reshaping, improved projection
- Why it works: it allows tissue reorganisation with good control of the lower pole
- What to expect: a vertical scar that typically softens over time with proper scar care
We choose the smallest pattern that still gives a stable lift. Less scarring is only a win if the result holds.
Anchor lift: maximum correction when ptosis is more advanced
Wise pattern mastopexy (often described as an “anchor” pattern) is typically reserved for higher-grade ptosis, heavier breasts, or cases where skin excess is significant. It uses an incision around the areola, a vertical line, and a line along the inframammary fold.
- Best for: more advanced ptosis, significant excess skin, major reshaping needs
- Strength: robust control of breast shape and skin envelope
- Trade-off: more scar length, balanced against better correction power
Auto-augmentation and “limited” patterns: adding structure without an implant
Auto-augmentation mastopexy reshapes and repositions your own breast tissue to improve upper pole support without adding an implant. It can be useful when you want lift and better fullness, but prefer to avoid an implant-based augmentation.
- Best for: lift + shape refinement where tissue can be repositioned effectively
- What it is not: a substitute for implants when a significant volume increase is the goal
We also see patients asking about a “crescent” lift. It has very limited indications, usually for subtle nipple position refinement. It does not correct meaningful ptosis.
| Technique | Typical ptosis level | Scar pattern | Strengths | Limitations |
|---|---|---|---|---|
| Periareolar (Benelli) | Mild | Around the areola | Minimal scarring, areola resizing | Limited lift power; can widen in lax skin |
| Vertical (“Lollipop”) | Mild–Moderate | Around areola + vertical line | Strong reshaping with moderate scarring | Not ideal for major excess skin |
| Wise Pattern (“Anchor”) | Moderate–Severe | Around areola + vertical + fold line | Maximum correction and skin management | More scar length |
| Auto-augmentation | Case-dependent | Often vertical or anchor-based | Improves shape using own tissue | Does not add large volume |
| Crescent (limited) | Very mild | Small arc at areola edge | Subtle repositioning in select cases | Not a true lift for ptosis |
Combined Procedures: how to maximise your result without compromising safety
A breast lift corrects position and shape. It does not automatically solve volume, heaviness, or proportion with the rest of the body. That is why combination planning matters.
The key is not doing “more”. It is doing the right mix for your anatomy, in a safe order, with a recovery plan you can actually manage.
For UK patients travelling for surgery, we also consider practicality: how many procedures make sense within one trip, and what aftercare is required before you fly home.
We discuss combinations only when they add clarity to the outcome, not when they add complexity for its own sake.
Breast lift vs augmentation: solving the correct problem first
Some patients describe “sagging”, but what they truly miss is upper pole fullness. Others mainly want the nipple position corrected. These are different goals.
- Lift-led plan: best when position and skin excess are the main issues
- Volume-led plan: best when fullness is the main priority (implant or fat transfer may be discussed)
- Combined plan: best when you need both a lift and reliable volume change
Lift + implants: when structure and volume both matter
When we combine a lift with implants, the planning is more technical. We aim to avoid a “tight on top, loose below” outcome by matching implant choice to tissue quality and the lift pattern.
- Best for: clear volume loss plus ptosis
- Core focus: proportion, implant position, and a stable breast shape over time
- What we avoid: chasing an exaggerated look at the cost of long-term tissue stress
Rejuvenation, not alteration. The best combined result still looks like you.
Lift + breast reduction: when heaviness is the problem
If your breasts feel heavy and low, a lift alone may not be enough. Breast reduction can improve comfort and make long-term results more stable because the tissues carry less load.
- Best for: heaviness, bra-strap discomfort, proportion goals
- Added benefit: easier long-term maintenance of shape in some cases
Rejuvenation, not alteration. The best combined result still looks like you.
Lift within a Mummy Makeover plan: timing and recovery logic
Many UK patients look at a broader reset after pregnancy. A Mummy Makeover plan can combine breast and body surgery, but only when the safety profile and recovery timeline make sense.
- Best for: patients who want one consolidated recovery period
- Planning priority: careful staging, realistic downtime, and clear post-op monitoring
- Our role: map the plan to your physiology, not to a trend
Common add-ons: liposuction, tummy tuck, and facelift (when clinically appropriate)
In selected patients, a combined plan may also include liposuction for contour refinement or a tummy tuck to address abdominal skin laxity after pregnancy or weight change. For patients seeking broader facial rejuvenation, a facelift is generally considered as a separate pathway, with its own safety and recovery planning.
If you want, we can review your photos and goals remotely and outline a clinically sensible plan before you commit to travel. Clear planning reduces surprises. That is the point.
Anaesthesia Choices for Breast Uplift (Mastopexy): comfort, control, and clinical suitability
Anaesthesia is not a minor detail. For the UK expert patient, it is often the point where “how it’s done” matters as much as “what is done”. Your anaesthetic plan influences comfort, safety monitoring, and the smoothness of early recovery.
In breast uplift surgery, the most common approach is general anaesthesia. However, in selected cases, twilight sedation (also called conscious sedation) may be discussed. The correct choice depends on your health profile, procedure complexity, and what is clinically appropriate.
General anaesthesia: the standard approach for most mastopexy cases
General anaesthesia means you are fully asleep, with continuous monitoring throughout. For many patients, it offers the most predictable operating conditions, especially when the lift requires more extensive reshaping.
- When it is commonly used: moderate-to-severe ptosis, anchor/vertical patterns, combined procedures
- Why it helps: stable operating conditions, complete comfort, consistent surgical precision
- Key point: the anaesthetic plan is as structured as the surgical plan, with pre-assessment and monitoring
Twilight sedation (“awake” options): when comfort and suitability align
Some patients search for “awake breast lift” or “twilight sedation” because they want a lighter recovery profile or have personal preferences around anaesthesia. In reality, sedation options must be selected carefully and are not suitable for every mastopexy.
- What it is: a sedated, relaxed state with pain control and monitoring, while you remain breathing independently
- Where it may fit: selected cases with limited complexity, shorter operating time, and favourable medical profile
- Where it may not fit: more extensive reshaping needs, significant ptosis, complex combinations, or where a deeper anaesthetic is safer
We do not “force” a sedation preference onto a procedure. We align the plan to what is safe and precise for your anatomy and objectives.
Local anaesthetic: what it can and cannot cover
Local anaesthetic is routinely used in breast surgery as part of pain management, but it is not typically used as the sole anaesthetic for a full mastopexy. You may see it mentioned online, but it generally applies to very limited procedures rather than comprehensive reshaping.
How we decide: the clinical decision-making framework
We choose an anaesthetic plan the same way we choose a surgical technique: by mapping it to the individual patient. Factors we consider include:
- Procedure scope: limited-scar vs vertical vs anchor patterns; whether implants or reduction are planned
- Operating time: longer procedures often favour general anaesthesia for predictability
- Medical history: relevant conditions, medications, previous anaesthesia history
- Comfort profile: anxiety level, pain sensitivity, and recovery expectations
| Anaesthesia option | Typical comfort level | Where it can fit | Main limitation |
|---|---|---|---|
| General anaesthesia | Fully asleep | Most mastopexy patterns; complex reshaping; combined procedures | Requires standard post-anaesthetic recovery monitoring |
| Twilight sedation (selected cases) | Very relaxed / drowsy | Limited complexity cases where clinically suitable | Not appropriate for all lifts; suitability-dependent |
| Local anaesthetic (supportive) | Targeted pain control | Used to support comfort and post-op pain management | Not typically sufficient alone for full mastopexy |
If you are travelling from the UK, we also plan your anaesthesia and recovery with your travel timeline in mind. That does not mean we compromise. It means we make the process predictable and properly supported.
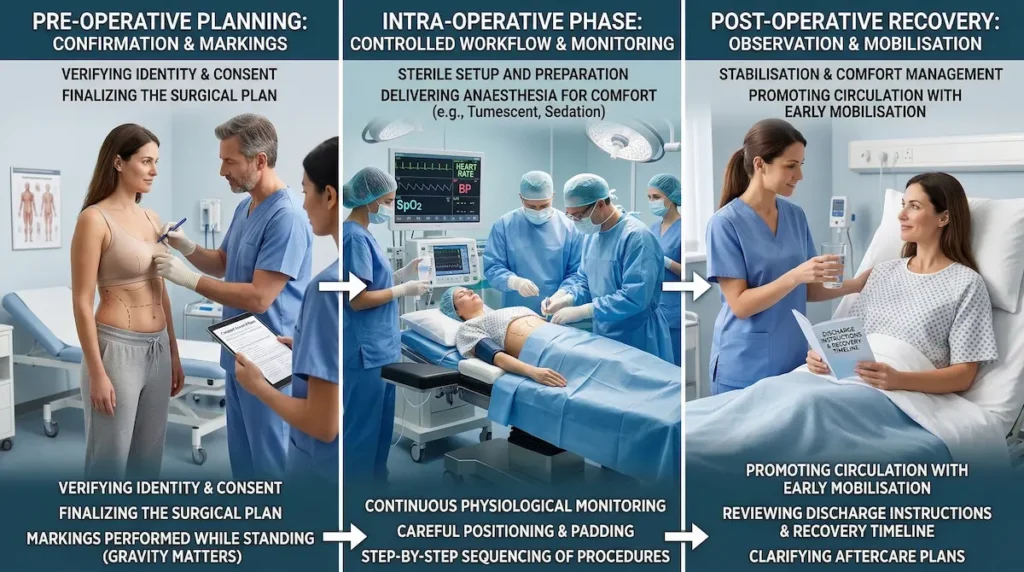
Boob Lift Surgery Step-By-Step: What Happens In The Operating Theatre
A precise result starts before the first incision. In mastopexy, pre-operative assessment, surgical markings, and intra-operative judgement all influence symmetry, nipple position, and long-term stability.
Below is what the process typically looks like when you undergo a breast uplift with us, written with transparency for patients who want a clear clinical overview.
1) Pre-operative assessment and planning
Before surgery, we confirm that the plan matches both your anatomy and your goals. This includes:
- Measurements: nipple position, fold height, breast footprint, and asymmetry mapping
- Skin quality review: elasticity, stretch marks, tissue density (what will hold vs what will relax)
- Technique selection: periareolar vs vertical vs anchor, based on correction required
- Safety checks: medical history review, relevant investigations, medication and supplement review
If your plan includes a combined procedure (for example, lift with implants or lift with reduction), we confirm sequencing and operating time expectations.
2) Surgical markings: why they matter
Markings are not “lines on the skin”. They are the blueprint for proportion and symmetry. They help define:
- The new nipple–areola position in relation to your chest shape
- The amount of skin to be removed without over-tightening
- The scar pattern required to achieve the planned lift
This step is especially important for expert patients because it reflects whether the plan is tissue-led or skin-led. We aim for tissue-led reshaping, with closure designed to heal well.
3) Reshaping and repositioning: the core of mastopexy
During surgery, the main goals are to lift and reshape the breast tissue, manage the skin envelope, and reposition the nipple–areola complex if needed. The specific steps vary by technique, but the principles are consistent:
- Tissue reshaping: internal reconfiguration to create a stable breast mound
- Nipple–areola management: repositioning to match the new breast apex, where appropriate
- Skin envelope tailoring: removing excess skin in a controlled way to support the new shape
For auto-augmentation approaches, we may use your own tissue to add internal support and improve upper pole contour without an implant, depending on suitability.
4) Closure and dressings: planning for clean healing
Closure technique matters for scarring and early wound stability. We aim to close without excessive tension and apply dressings that support the incisions properly.
- Dressings: applied to protect the incision sites and reduce friction
- Surgical bra: supportive compression to reduce swelling and stabilise the shape
- Immediate checks: monitoring circulation, symmetry, and overall stability before recovery
5) Recovery room and discharge plan
After surgery, you move to a monitored recovery area. The focus is comfort, stable observations, and safe mobilisation. Your discharge plan includes:
- Pain management guidance: what is normal, what is not, and how to stay comfortable
- Movement advice: how to protect the repair while staying safely mobile
- Aftercare schedule: wound checks and clear instructions for dressing care
- Travel planning: guidance aligned with your surgical scope and recovery progress
We also set expectations early: shape settles over weeks, not days. Swelling and firmness are normal at the beginning. This is why a structured recovery timeline (covered in the next sections) is as important as the operation itself.

Breast Lift Recovery & Aftercare: a realistic mastopexy recovery timeline
If you are searching for a mastopexy recovery timeline, you are trying to do something sensible: reduce uncertainty. Recovery is not “one-size-fits-all”. It depends on your technique (periareolar vs vertical vs anchor), whether you have combined surgery, your skin quality, and your healing profile.
What we can do is make the process predictable: clear instructions, structured check-ins, and a plan that protects the surgical result while supporting comfort.
The first 72 hours: protection, swelling control, and safe mobilisation
The initial phase is about stability. You will have swelling, firmness, and a “tight” sensation. This is normal early on.
- What you may feel: tightness, pressure, mild-to-moderate discomfort, fatigue
- What we prioritise: pain control, wound protection, circulation checks, safe movement
- What you should do: gentle walking, hydration, sleeping with your upper body slightly elevated
- What you should avoid: lifting, pushing/pulling, reaching overhead, twisting aggressively
Your surgical bra is not “optional”. It stabilises the breast shape, reduces friction on the incisions, and supports swelling control.
Week 1: wound care routine and settling into a safe rhythm
In the first week, comfort usually improves day by day, but swelling can fluctuate. This is also when patients tend to overestimate what they can do. Protecting the repair matters more than proving you feel “fine”.
- Typical focus: incision care, dressing guidance, gentle daily movement
- Activity level: light activities only; no exercise; no lifting children or heavy bags
- Hygiene: follow the specific instructions you are given for showering and dressing changes
If you are travelling from the UK, we schedule check-ups during your stay so you are not guessing what is normal.
Weeks 2–3: returning to routine (without stressing the scars)
Many patients feel significantly better in this window, but internal healing continues. The tissues are still settling, and the scar line is still “immature”.
- Work: desk-based work is often manageable, depending on comfort and travel fatigue
- Movement: gentle walking is encouraged; avoid impact, running, or upper-body strain
- Swelling: may reduce overall, but can still fluctuate by the end of the day
This is also when early scar support becomes important: avoiding friction, avoiding sun exposure on scars, and using any scar-care plan recommended to you.
We utilise advanced Hyperbaric Oxygen Therapy (HBOT) to minimise downtime and enhance your healing process. Safety is our primary commitment.
Weeks 4–6: building strength carefully and protecting long-term shape
In many cases, this is when a gradual return to exercise can be discussed. The key word is gradual. Overloading too early can widen scars, increase swelling, or pull on healing tissues.
- Support garments: continue as advised (this varies with technique and tissue quality)
- Exercise: phased return, often starting with lower body and low-impact activity
- Underwired bras: usually avoided early; timing is personalised to incision placement and healing
Months 3–12: scar maturation and “final result” timing
Breast shape continues to settle. Scars mature slowly, usually over several months. Early scars can look red, raised, or uneven; this does not automatically mean they will stay that way.
- Shape: continues to soften and settle
- Sensation: temporary changes can occur; improvement may be gradual
- Scars: often fade and flatten over time with consistent care
We treat scar management as part of the procedure, not an afterthought. The goal is a result that is not only lifted, but also heals cleanly.
When to contact us (never “wait and see” with these signs)
Most recovery is uncomplicated, but you should seek clinical advice promptly and contact us if you notice:
- increasing redness, heat, or worsening pain around an incision
- fever or feeling unwell beyond expected post-operative fatigue
- unexpected swelling on one side, significant bruising expansion, or concerning discharge
- shortness of breath or chest pain (urgent assessment required)
Safety is a system. Clear instructions and early escalation are part of that system—if anything concerns you, contact us without delay.
Receive a clear, day-by-day itinerary covering arrival, surgery, recovery, and fit-to-fly clearance tailored to your requirements.
Our Rapid Recovery & Safety Protocol: HBOT and LLLT
Expert patients often ask a smart question: “What are you doing beyond the operation itself to optimise healing?” That is where structured recovery support can matter.
Two technologies you may see discussed in premium post-operative protocols are HBOT (Hyperbaric Oxygen Therapy) and LLLT (Low-Level Laser Therapy), also known as photobiomodulation. These are not marketing add-ons. Used appropriately, they are designed to support tissue recovery and comfort as part of a wider aftercare plan.
Important: these therapies are not a replacement for good surgical technique, safe anaesthesia, or correct wound care. They are adjuncts, used selectively, based on suitability.
HBOT (Hyperbaric Oxygen Therapy): what it is and why it may help post-op recovery
HBOT involves breathing oxygen in a controlled, pressurised environment. The clinical rationale in post-operative contexts is support of oxygen delivery to tissues that are healing.
- Potential aims: support tissue recovery, assist with swelling management, and promote overall healing conditions
- Where it may fit: selected patients where enhanced recovery support is clinically appropriate
- What it does not mean: no therapy can “guarantee” a particular scar outcome
We integrate HBOT only when it aligns with your overall medical profile and recovery plan.
LLLT (Low-Level Laser Therapy / photobiomodulation): a supportive approach to tissue comfort and scar care
LLLT uses specific light wavelengths with the aim of supporting cellular activity involved in tissue recovery. In aesthetic surgery aftercare, it is commonly discussed in the context of comfort, swelling, and scar-quality support.
- Potential aims: support the healing environment, reduce discomfort, and assist scar-care strategies
- Practical benefit: non-invasive, clinic-led sessions within a structured aftercare pathway
- Best paired with: correct incision care, appropriate garment use, and realistic activity restrictions
Why the combination can matter: macro support + micro support (without overpromising)
Think of recovery as layered. HBOT is often discussed as systemic support (whole-body healing conditions), while LLLT is often discussed as local support (targeted tissue comfort and scar-quality strategies). Used appropriately, they can complement each other within a broader protocol.
- Comfort: supporting early-phase recovery so you can move safely and rest properly
- Swelling management: assisting the recovery environment while tissues settle
- Scar strategy: pairing technology with practical scar-care steps and follow-up
Who may be suitable (and why selection matters)
Not every patient needs additional recovery technologies. Suitability depends on your procedure scope, your healing profile, and your overall medical picture.
- Procedure scope: anchor/vertical patterns and combined procedures may benefit from more structured recovery support
- Healing profile: skin quality, scarring tendency, and lifestyle factors
- Travel planning: a clear in-clinic aftercare window before returning to the UK
The point is not to “add treatments”. The point is to design a recovery pathway that is coherent, clinically rational, and aligned with your goals.

Breast Lift Before and After Results & Longevity
With mastopexy, your early result is not your final result. Shape settles, swelling reduces, and scars mature over time. The most “expert patient” mindset you can bring is patience: you are watching a biological process, not an instant makeover.
What to expect at 6 weeks, 3 months, and 1 year
At 6 weeks, swelling is reduced but firmness and a slightly “high” look can persist. By 3 months, contours usually soften and movement feels more natural. Around 1 year, scars are more mature and the breast shape is most settled, allowing the clearest assessment of symmetry and refinement needs.
At 6 weeks: “early settling”, not the finish line
By six weeks, many patients feel more like themselves again, but the breasts can still feel firm and look slightly “high” compared with the eventual settled position.
- What’s typical: reduced swelling overall, but fluctuations can still occur
- Shape: improved position is visible, but contour continues to soften
- Scars: often still pink/red and more noticeable than they will be later
This is also when activity increases, which is why we emphasise a phased return to exercise rather than a sudden “back to normal”.
At 3 months: clearer shape and more natural movement
Many patients feel the breasts look more “natural” around this stage. Tissue softness increases and the overall silhouette becomes less tight.
- Shape: more stable contour and improved natural movement
- Sensation: if there were temporary changes, gradual improvement may continue
- Scars: still maturing, but redness often begins to calm in many skin types
At 1 year: mature scars and the most settled result
At one year, scar maturation is typically much further along and the breast shape is generally at its most settled point. That does not mean the result will never change again, but it does mean you are usually seeing the “true” outcome of the surgery.
- Scars: typically flatter and lighter than the early post-op phase
- Shape: the most stable version of your new contour
- Assessment: this is when we judge long-term symmetry and refinement needs most accurately
How long do results last?
Longevity depends on biology and life events. A well-executed mastopexy can be long-lasting, but skin quality, breast weight, and lifestyle factors influence the timeline.
- Weight stability: large fluctuations can stretch tissues again
- Pregnancy: can change breast tissue volume and skin tension
- Skin elasticity: genetics and ageing matter
- Support habits: appropriate bra support during higher-impact activity helps
If you are planning pregnancy soon, it may be clinically sensible to postpone surgery. If pregnancy is not planned, we plan for a durable result based on your tissue behaviour.
Scars After A Breast Uplift: what is normal, what improves, and how scar quality is supported
Mastopexy involves scars. Any clinic suggesting “scarless mastopexy” is not being medically honest. The real question is: where are scars placed, how are they closed, and how is scar quality supported during recovery?
Scar patterns: why the “best” scar is the one that matches the correction
Scar pattern is linked to technique choice:
- Periareolar: scar around the areola (limited correction)
- Vertical (“lollipop”): areola + vertical line (balanced correction)
- Anchor: areola + vertical + fold line (maximum correction)
Choosing a smaller scar pattern than your anatomy requires can lead to a compromised shape or early recurrence of ptosis. The goal is stable correction with a scar strategy designed to heal well.
Scar timeline: what you may see from weeks to months
- Weeks 2–6: scars can look red/pink and feel firm; this is common
- Months 2–6: scars often begin to soften; colour gradually calms
- Months 6–12: scars continue to flatten and fade in many patients
Some skin types develop thicker scars more easily. If you have a history of hypertrophic scarring or keloids, that should be discussed before surgery so the plan can be tailored.
Core scar-care principles (simple, consistent, effective)
- Protect the incisions early: avoid friction and tension on the wound lines
- Support garments: wear your surgical bra as advised
- Sun protection: UV exposure can worsen pigmentation and slow improvement
- Follow-up: small issues become big issues when ignored
Where recovery-support technologies can fit (without overpromising)
Where clinically appropriate, supportive approaches such as LLLT may be integrated within a broader scar-quality strategy. The aim is to support the healing environment and comfort while the body completes the biological work of repair. These therapies do not “override” genetics, but they can be part of a coherent aftercare pathway.
Safety & Risks: Is Breast Uplift (Mastopexy) Dangerous?
Every surgical procedure carries risk. A responsible clinic does not minimise that. The right question is not “Is mastopexy risk-free?” (it is not), but “How are risks reduced, monitored, and managed?”
Risk is influenced by your baseline health, your anatomy, procedure complexity (lift only vs combined surgery), and lifestyle factors such as nicotine use. It is also influenced by systems: pre-op screening, sterile technique, anaesthesia monitoring, and post-op follow-up.
General surgical risks (applicable to most operations)
- Bleeding / haematoma: rare but can require urgent assessment and occasionally a return to theatre
- Infection: typically treatable when identified early; prevention and wound care matter
- Seroma (fluid collection): may require monitoring or drainage
- Adverse reaction to medication or anaesthesia: risk assessed through pre-op evaluation and monitoring
- Thrombosis risk: managed with mobilisation guidance and risk assessment protocols
Mastopexy-specific risks (what expert patients ask about)
- Scarring: all mastopexy techniques involve scars; quality varies by skin type, tension, and aftercare
- Delayed wound healing: more likely with nicotine use, poor circulation, or excessive early activity
- Changes in nipple sensation: can be temporary or, less commonly, longer-lasting
- Asymmetry: improvement is the goal, but perfect symmetry is not realistic
- Recurrent ptosis: skin quality and life events (weight change, pregnancy) influence longevity
- Revision surgery: occasionally required for scar refinement, shape adjustment, or asymmetry correction
How we reduce risk: the “system” behind the surgery
A good outcome is not only surgical technique. It is planning, selection, and aftercare discipline.
- Pre-op evaluation: medical history review, relevant investigations, and medication/supplement checks
- Technique selection: choosing the scar pattern that can deliver the correction reliably (not the smallest scar at any cost)
- Anaesthesia planning: selecting the safest, most predictable option for the procedure scope
- Wound strategy: closure without excessive tension, protective dressings, and structured aftercare
- Escalation pathways: clear advice on what is normal vs what needs prompt review
If your lifestyle factors increase risk (for example, nicotine use), we address them directly. This is not judgement. It is medical reality.
Is A Breast Lift Safe In Turkey? What UK patients should check before choosing a clinic
For UK patients, “safe in Turkey” is a valid question. Safety is not a country label. It is a combination of surgeon expertise, facility standards, peri-operative monitoring, and aftercare systems.
When patients compare Istanbul to London (including Harley Street), the comparison should be clinical: standards, process, and the quality of the surgical journey. If you are evaluating any provider, the checks below protect you.
1) Facility standards: where safety is actually delivered
Ask what you would ask anywhere:
- Operating theatre standards: sterile protocols, appropriate equipment, and trained staff
- Monitoring: anaesthesia monitoring and post-anaesthetic recovery supervision
- Emergency readiness: clear pathways for urgent assessment if needed
Safety is not a brochure sentence. It is an audited process.
2) Surgeon credentials and clinical accountability
Expert patients look for credible signals:
- Relevant training and professional standing (verifiable, consistent, and appropriate to breast surgery)
- Clear case selection principles: willingness to say “not suitable” or “not yet”
- Transparent discussion of scars and risks: no “scarless” claims for mastopexy
Competence shows up in how a surgeon explains limitations and trade-offs, not only in how they describe benefits.
3) Aftercare and follow-up: the part many patients underestimate
Travelling for surgery raises a practical question: “What happens after I leave?” A safe clinic has an answer that is structured, not vague.
- In-person checks while you are in Istanbul before you travel home
- Clear wound care instructions and a plan for scar management
- Remote follow-up schedule with clinical escalation if something concerns you
If aftercare is unclear, your risk increases — regardless of location.
4) Why some patients choose Istanbul as a “premium medical travel” pathway
UK patients often compare the overall journey, not only the operation. The value proposition becomes clearer when it combines:
- Structured surgical planning aligned with expert-patient decision-making
- Enhanced recovery support where clinically appropriate (for example, integrated aftercare protocols)
- Logistics designed for comfort (predictable travel, accommodation, and patient coordination)
In other words: value is the blend of clinical quality and a well-managed process, not a “deal”.

Fees & Value: Breast Lift Cost 2026 Turkey vs UK
UK patients often benchmark against London pricing (including Harley Street) to sense-check value. That is reasonable. The aim is not to chase the lowest figure; it is to understand what you are paying for, what is included, and how the care pathway is structured.
A responsible cost discussion is transparent and clinical. A breast uplift is not one identical operation for everyone, so a single headline figure without context is rarely meaningful.
What influences the fee for Breast Uplift (Mastopexy)?
- Technique complexity: periareolar vs vertical vs anchor patterns
- Ptosis grade and skin excess: more correction typically requires more operative planning
- Combined surgery: lift with implants, lift with reduction, or broader post-pregnancy planning
- Anaesthesia and operating time: longer procedures require more theatre resources
- Aftercare intensity: follow-up structure, dressings, garments, and recovery support
All-inclusive planning: what “value” should mean for UK patients
When UK patients travel, hidden extras create stress. A value-led pathway should be clear about what is included, such as:
- Pre-op assessment and necessary investigations
- The procedure and anaesthesia within an appropriate facility setting
- Post-op garments (such as a surgical bra) and wound care plan
- Scheduled follow-ups during your stay and remote follow-up afterwards
- Logistics support (transfers and coordination) to reduce friction
We avoid “headline pricing” language because it encourages the wrong decision-making. Your plan should be built around clinical suitability, not a number on a screen.
Why Turkey can offer strong value without cutting clinical corners
Patients often ask why costs can differ from the UK. In many cases, it is a combination of operating costs, local economics, and service models. That does not automatically imply lower standards — but you should confirm standards and aftercare systems rather than assume them.
If you want a meaningful quote, it should be based on your anatomy and goals: ptosis grade, desired shape, skin quality, and whether volume change is part of the plan.

Finding Best Breast Lift Surgeon
Searching for the “best” breast lift surgeon is really about finding the safest, most predictable pathway for Breast Uplift (Mastopexy). For UK patients, the strongest indicators are not marketing claims, but clinical transparency: how your anatomy is assessed, how technique is selected, and how risks and scars are discussed.
Start by looking for verifiable expertise in breast surgery and clear accountability. A credible provider will explain why a periareolar, vertical (“lollipop”), or Wise pattern (“anchor”) approach suits your ptosis grade and skin quality—without promising “scarless” results. They should also be comfortable discussing anaesthesia options, monitoring, and what a realistic recovery timeline looks like.
- Credentials and standards: appropriate training and internationally recognised certification where applicable.
- Technique-led planning: a tailored plan based on ptosis grade, asymmetry, skin quality, and goals.
- Evidence of consistency: before-and-after case examples with technique context (not just glamour shots).
- Safety systems: proper screening, sterile theatre protocols, and clear escalation guidance post-op.
- Aftercare structure: in-person checks before travel and remote follow-up once you return to the UK.
Finally, avoid choosing purely on price. In expert care, value is the combination of surgical precision, safety, and a well-managed recovery plan.
From VIP airport transfers to 5-star hotel accommodation, we manage every detail. Enjoy a premier medical travel experience in Istanbul.
Planning Your Trip From The UK: a clear, low-friction patient journey
For many UK patients, the biggest concern is not the flight. It is uncertainty: “How does this work in practice?” A well-run pathway replaces guesswork with structure, from remote planning to in-person checks before you travel home.
Below is what a typical journey can look like when it is designed as premium medical travel — clinically led, not tourism-led.
Step 1: Remote review and clinical planning
- Goal-setting: lift-only vs lift + volume strategy
- Technique discussion: expected scar pattern and why it suits your anatomy
- Medical screening: history, medication review, and suitability checkpoints
At this stage, the most useful outcome is clarity: what is realistic, what is not, and what the safest plan looks like.
Step 2: Arrival in Istanbul and in-person assessment
- Coordinated transfers: to reduce travel fatigue and confusion
- In-person consultation: confirmation of measurements, markings, and final surgical plan
- Pre-op checks: investigations and readiness confirmation
Step 3: Surgery day and immediate aftercare
- Operating theatre process: anaesthesia, monitoring, and structured recovery observation
- Discharge planning: clear instructions, garments, and check-in schedule
- Comfort priorities: pain control, mobilisation guidance, and wound protection
Step 4: Post-op checks before you fly home
Flying is not the main issue; timing and stability are. Before you travel, we confirm recovery is progressing as expected and that you have:
- Wound care clarity: dressings, hygiene, and what to avoid
- Escalation guidance: what requires prompt contact vs what is normal
- Remote follow-up plan: structured check-ins after you return to the UK
Breast Uplift (Mastopexy) Frequently Asked Questions (FAQ):
How painful is a breast uplift?
Most patients describe discomfort, tightness, and pressure rather than severe pain. Pain management is planned as part of your pathway, and discomfort typically improves progressively over the first week. The exact experience varies with technique and whether you have combined surgery.
Will I need implants as well?
Not necessarily. If your main issue is position (ptosis), a lift alone may be enough. If your main issue is upper pole fullness or a desire for a larger size, then lift + augmentation (or a carefully planned alternative such as fat transfer in selected cases) may be discussed. The correct plan depends on your anatomy and objectives.
Will I lose nipple sensation?
Temporary sensation changes can happen. Many patients experience gradual improvement over time, but outcomes vary. We discuss this risk openly during planning, especially when a significant lift is required.
How long before I can fly back to the UK?
Travel timing should be personalised to your procedure scope and recovery progress. The priority is safe early healing, stable observations, and clear aftercare instructions before travel. If you are planning surgery with travel, we build your schedule around appropriate in-person post-op checks before you return home.
When can I return to work and exercise after breast uplift?
Desk-based work is often possible earlier than physically demanding roles, but timing depends on how you heal and whether travel fatigue is a factor. Exercise returns in phases, usually starting with gentle walking, then gradually building back. Rushing upper-body activity too early can affect swelling, scar quality, and long-term shape.
Can mastopexy correct asymmetry?
We can usually improve asymmetry significantly, but perfect symmetry is not realistic. Natural differences in breast volume, fold height, and chest wall shape can remain. We aim for a balanced result that looks harmonious in real life.
Is a “scarless breast lift” real?
No. Mastopexy requires incisions. What matters is selecting the correct technique for your ptosis grade and managing healing with an evidence-led aftercare strategy. Any claim of “scarless mastopexy” should be treated with caution.
Medical Disclaimer
This page is for general information only and does not constitute medical advice. A breast uplift (mastopexy) is a surgical procedure and suitability varies between individuals. A personalised assessment with a qualified clinician is required to determine the safest and most appropriate treatment plan for you. If you have urgent symptoms or concerns, seek immediate medical attention.
Breast Lift (Mastopexy): Patient Stories

Laura


Lisa

Breast Lift (Mastopexy) Surgeons
Breast Lift (Mastopexy) Cost in Turkey
Starting from ~ £3400
* There are no hidden fees or unexpected charges.
- Your PersonalisedBreast Lift (Mastopexy)Procedure
- All Specialist Surgeon & Anaesthesia Fees
- All Pre-Op Tests & Post-Op Check-ups
- 5-Star Hotel Accommodation (incl. breakfast)
- All Private VIP Airport & Clinic Transfers
- 24/7 Dedicated Patient Coordinator & Translation Services
Breast Lift (Mastopexy): A Cost Comparison
| City | Cost |
|---|---|
| London | ~ £11,500 GBP |
| Birmingham | ~ £11,000 GBP |
| Leeds | ~ £10.800 GBP |
| Belfast | ~ £10,500 GBP |
| Manchester | ~ £11,200 GBP |
Breast Lift (Mastopexy): Patient Reviews
Jammal Canada
I have had face and neck lift with AKM Clinic they have been so good to me and my operation went so smoothly🥰 i would like to thank my doctor here and also to the team 💐

Ava Canada
Thank you AKM Clinic for giving me my confidence back! Had facelift + temporal lift 3 months ago and the outcome is already stunning. Special thanks to Hande!

Jakayla USA
Had a deep plane facelift and lower eyelid procedure at AKM Clinic 7 months ago. The results are fantastic - very subtle and natural. I didn’t expect the entire experience to be so comfortable. Hande managed everything and kept in contact even after I returned to USA. I’m beyond pleased with the outcome and the care I received. Would do it again in a heartbeat!

Barbara United Kingdom
It has been 4 months since my surgery. Everything is great, The most important thing is l love the way l look, l look exactly how l wanted. Meaning l look natural, just almost 40 years younger. I pulled Facebook - majority voted 37ys. I also had face, neck, chest, and hands CO2 laser. My skin is flawless.

Lisa Canada
I had a face, neck and arm lift at AKM. I’m just over 4 weeks post and couldn’t be happier with the results. The entire experience was wonderful! My coordinator, Khadija made me feel comfortable from beginning to end! I highly recommend AKM and will definitely go back for other procedures!

Julie USA
I am beyond grateful I went with AKM Clinic for my deep plane face and neck lift, upper eyelid, and co2 laser. Dr. Akif has magic hands and my results are truly incredible! I came from the US and assistant Emine was the best in assuring every detail was coordinated and communicated with me beyond my expectations every step of the way. 10 out of 10 to the entire team! I couldn’t be more pleased!

Ready to Begin Your Own Transformation Journey?
Join the 2,000+ patients who have trusted Dr Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, naturally restored you begins with a simple, no-obligation conversation. Contact us today from the UK for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. There are no hidden fees.
#2: Secure Your Date & VIP Booking
Once you are ready, our dedicated patient coordinators will help you secure your procedure date. We will handle all your bookings, including your 5-star hotel accommodation and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you will meet your specialist surgeon to finalise the details for your natural, subtle, and restored new look.














