Awake Gynaecomastia Surgery in Turkey




- Awake gynaecomastia surgery uses local anaesthesia to avoid general anaesthetic exposure and support safer, controlled recovery.
- Excision vs liposuction clarity: technique is chosen by tissue type, often combining both for natural chest contour.
- UK-to-Istanbul value compares premium standards against UK private pricing, with transparent planning and aftercare support.
- Faster functional recovery focuses on compression protocols, realistic timelines, and optional HBOT/LLLT for smoother healing.
AI-generated summary, fact-checked by our medical experts.
Awake Gynaecomastia Surgery: Quick Facts
Duration of Surgery
Type of Anaesthesia
Initial Recovery Period
Hospital Accommodation
Return to Daily Activities
Awake Gynaecomastia Surgery Results: Before and After
If you’re researching awake gynaecomastia surgery, you’re probably not looking for a “quick fix”. You want clarity. You want to understand the anatomy, the technique, and the real safety profile of avoiding general anaesthesia.
That is how we write at AKM Clinic. We treat you as an expert patient, not a passive consumer. Our job is to give you the same level of transparency you’d expect from a consultant-led discussion in the UK.
Surgeon’s Insight: Our goal is a natural, masculine chest contour. The philosophy is simple: Rejuvenation, not alteration.
Share your photos and medical history to receive a personalised assessment from our European Board-certified facial surgery team.
Table of Contents
What is Awake Gynaecomastia Surgery?
Awake gynaecomastia surgery is male chest reduction performed under local anaesthesia, with you breathing on your own and able to communicate. We numb the breast and chest tissues with carefully dosed lignocaine (often with adrenaline). The goal is to remove excess gland and/or fat. You go home the same day.
Gynaecomastia vs pseudogynaecomastia: why the distinction matters
“Gynaecomastia” is true enlargement of firm glandular tissue beneath the nipple-areola complex. “Pseudogynaecomastia” is mainly fatty volume, often linked to overall weight gain. The correction plan changes depending on what is actually there. For a concise scientific overview and clinical guidance, see evidence-based UK resources on gynaecomastia assessment and management.
In clinic, we do a direct physical assessment, supported by your photos and medical history. A simple self-check can be a starting point, not a diagnosis: the glandular tissue vs fat pinch test (a firmer, rubbery disc under the areola versus a softer, diffuse pinch). If there is doubt, imaging may be advised.
- More gland usually means excision is required for a predictable flattening.
- More fat may respond well to liposuction and weight stabilisation.
- Mixed tissue often benefits from a combined approach.
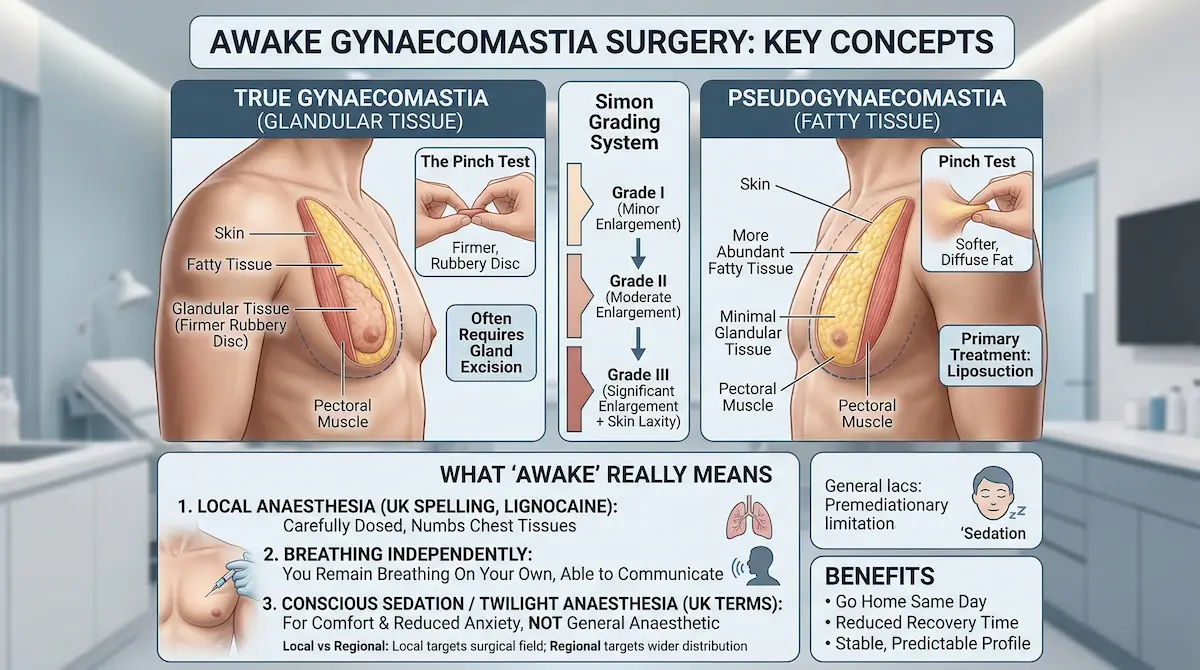
Understanding the anatomy (and the Simon grading system)
The male chest is not “just fat”. It is skin, subcutaneous fat, glandular tissue, and the contour created by the pectoralis muscle underneath. Surgery is about balance: remove what should not be there, preserve what should.
To describe severity and guide technique, surgeons often refer to the Simon classification of gynaecomastia. It grades the degree of enlargement and excess skin. The higher the grade, the more likely skin management and a more structured contour plan becomes part of the discussion.
- Lower grades: less volume, better skin recoil, often smaller incisions.
- Moderate grades: mixed fat and gland, contour refinement becomes essential.
- Higher grades: more skin laxity, longer-term tightening strategy is discussed.
What “awake” really means in theatre
“Awake” does not mean “uncomfortable”. It means local anaesthesia is doing the heavy lifting, not a general anaesthetic. You remain breathing independently and can respond if needed, while your chest tissues are fully numbed.
Some patients also benefit from light, controlled calming medication. In UK search terms, this is often described as twilight anaesthesia or conscious sedation. The aim is not to “knock you out”, but to reduce anxiety while maintaining a stable, predictable recovery profile.
Technically, this is different from regional techniques (which numb a larger area of the body). If you’ve searched the difference between regional and local anaesthesia, the short version is scope: local targets the surgical field; regional affects a broader nerve distribution.
Our surgical dates fill up quickly due to high international demand. Secure your consultation today to arrange your preferred travel dates.
Why Choose an Awake Approach over General Anaesthesia?
Most UK patients who ask about staying awake are not chasing novelty. They are risk-auditing. They want to reduce the systemic load of drugs, avoid airway instrumentation, and keep recovery as functional as possible.
We also see a second group: men who simply do not like the idea of losing control. That is valid. An awake pathway can feel more psychologically contained when it is planned properly and delivered in a calm, monitored environment.
The key is fit. Awake surgery is not “better for everyone”, but it can be a strategically better choice for the right patient and the right technique.
Safety logic: reducing exposure, not cutting corners
The phrase awake surgery safety is often searched in the context of fear. Let’s be direct: every anaesthetic pathway has risks, and every surgery has variables. The advantage of a well-designed awake plan is that it can reduce certain general-anaesthesia-related exposures for suitable candidates.
- No routine airway tube and no deep inhalational anaesthetic requirement.
- Less post-anaesthetic grogginess for many patients.
- A clearer “start-to-finish” recovery timeline, often with earlier mobility.
At AKM Clinic, we combine this with strict pre-operative screening and monitored care throughout the procedure. We do not rely on optimism. We rely on protocols.
Autonomy and functional recovery (the “can I get back to life?” question)
Awake procedures appeal to people who think in practical outcomes. When you avoid a full general anaesthetic, you often avoid the longer “reset” that some patients feel afterwards. That matters if you want to travel comfortably, work remotely, or resume light daily tasks sooner.
This is also where UK intent shows up in very specific queries like “walk-in, walk-out” surgery. The phrase is marketing-heavy, but the underlying desire is reasonable: a controlled outpatient pathway with clear discharge criteria and structured follow-up.
Common worries: nausea, brain fog, and feeling “not myself”
Patients commonly compare feeling sick after local anaesthesia vs. general. Post-operative nausea is more strongly associated with general anaesthesia, opioids, and motion sensitivity, but individual responses vary. Your medication plan matters as much as the anaesthetic label.
Another frequent query is: Does local anaesthesia make you loopy? Local anaesthetic itself is intended to numb tissue, not alter your mind. When patients feel “foggy”, it is more often linked to sedatives, pain medication, poor sleep, dehydration, or anxiety. We plan around that with clear dosing strategy and straightforward aftercare instructions.
Am I a Suitable Candidate for Gynaecomastia Surgery Under Local Anaesthesia?
Suitability is not a marketing question. It is a clinical one. We look at your chest anatomy, your overall health, and the specific risks that matter when you choose an awake pathway. For UK patients, this often comes after a frustrating search around NHS gynaecomastia surgery criteria, or the high fees quoted privately. Our role is to make the decision rational and personalised, not rushed.
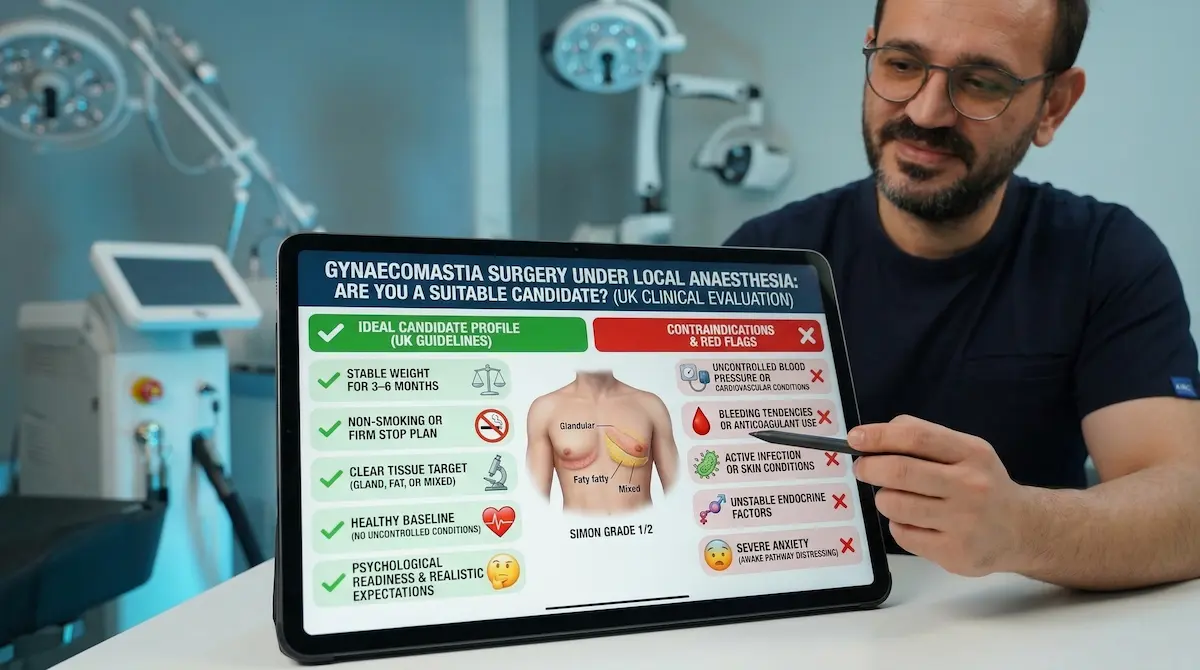
The ideal candidate profile (what we look for)
The best candidates usually have a stable weight, a clear diagnosis, and realistic expectations about scarring and recovery. We also assess whether your concern is mostly gland, mostly fat, or mixed tissue, because that drives the technique. If you are weight cycling or still actively bulking/cutting, we may advise stabilising first. It protects your result.
- Stable weight for at least 3–6 months, with no rapid gain/loss trends.
- Non-smoking (or a firm stop plan), because wound healing and scar quality matter.
- Clear tissue target: fat-dominant, gland-dominant, or mixed.
- Healthy baseline with no uncontrolled medical conditions.
- Psychological readiness: you understand recovery is gradual, not instant.
Who should avoid or delay surgery (contraindications and red flags)
Local anaesthesia is not “risk-free”. It is simply a different risk profile. We screen carefully to reduce the chance of complications and to keep the experience comfortable. If anything looks unstable, we pause and investigate rather than forcing a timetable.
- Uncontrolled blood pressure or poorly managed cardiovascular conditions.
- Bleeding tendencies or anticoagulant use without a safe plan agreed with your prescribing clinician.
- Active infection or untreated skin conditions on the chest.
- Unstable endocrine factors (for example, ongoing hormonal investigation or medication changes).
- Severe anxiety that makes an awake pathway distressing, even with calming medication.
We also discuss supplements and performance-enhancing drugs openly. Some increase bleeding risk or disrupt healing. Transparency helps you. It also helps your result.
When general anaesthesia may still be recommended
Being awake is an option, not an obligation. In a small subset of cases, general anaesthesia may be the better fit based on complexity or comfort. The decision is made on clinical logic, not on convenience. If we think you will do better with a different pathway, we will explain why.
- Higher Simon grades where extensive work is expected and time in theatre is longer.
- Significant skin excess where more complex reshaping is required.
- Revision surgery with scar tissue and altered anatomy.
- Severe needle phobia or inability to tolerate an awake environment safely.
Surgeon’s Insight: The safest plan is the one that matches your anatomy and your psychology. We never force “awake” if it is not the right fit for you.
Answer a few brief questions about your concerns, health, and goals to discover which treatment options may suit you best.
How Severe Is My Gynaecomastia? A Practical Simon Grade Guide
Most men can describe what they see, but not why it is happening. That’s where grading helps. The Simon system gives us a shared language to talk about volume, skin behaviour, and the likely surgical plan. It also protects you from unrealistic comparisons, because “before and after” images only make sense when the starting point is similar. Use the grading below as a structured self-audit, then let us confirm it during consultation.
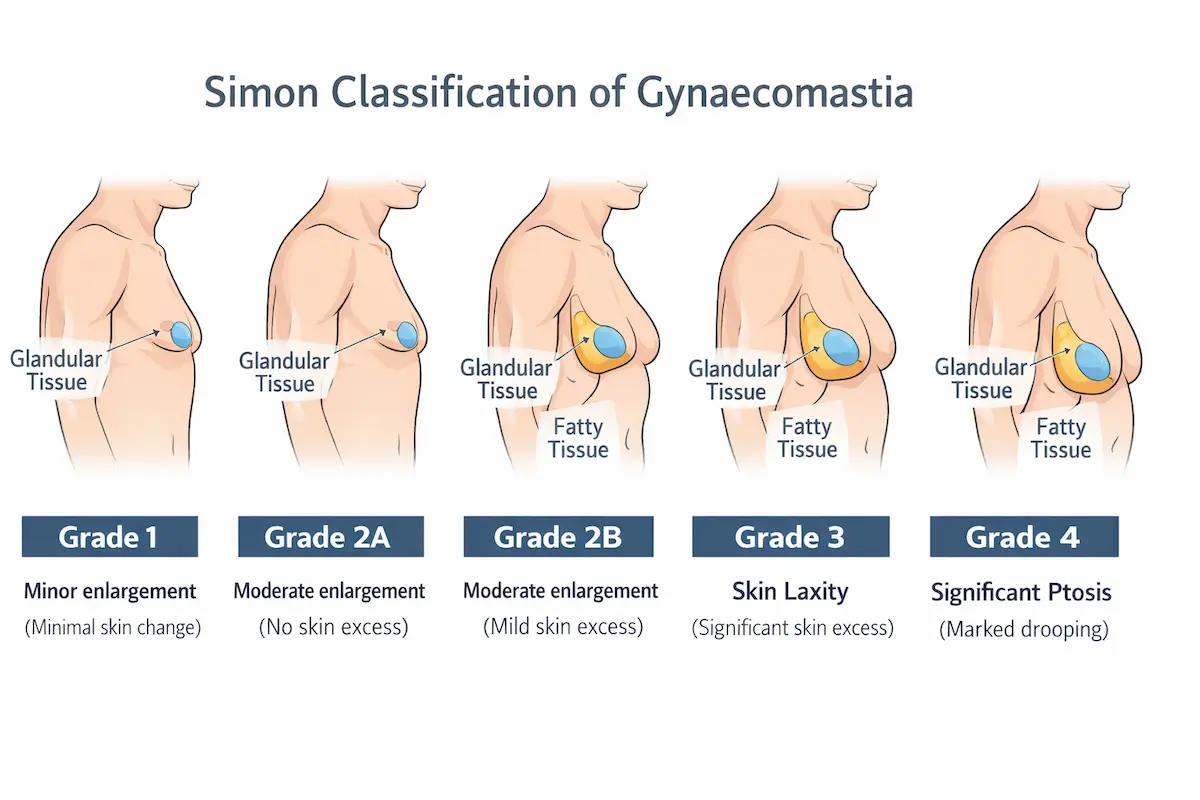
Simon Grade 1–4: what the grades mean in real life
Simon grading is not about judgement. It is about planning. Two chests can look “similar” in a T-shirt yet behave very differently once we correct the tissue. Skin elasticity, areola size, and symmetry change the surgical strategy.
- Grade 1: Small enlargement, minimal skin change. Often a more straightforward correction.
- Grade 2A: Moderate enlargement without significant skin excess. Contour refinement matters.
- Grade 2B: Moderate enlargement with mild skin excess. Technique must account for skin recoil.
- Grade 3: Larger enlargement with clear skin excess. A structured plan is essential.
- Grade 4: Marked enlargement with significant ptosis (droop). Skin management becomes a central topic.
Technique selection by grade: liposuction, excision, or both?
Technique is not a preference. It is a response to tissue behaviour. If the problem is mainly fat, liposuction can be enough. If the problem is firm gland, gland excision gynaecomastia is often necessary to avoid leaving a stubborn “puffy nipple” behind. Many men sit in the middle and need both.
- Fat-dominant cases: Liposuction for volume reduction and contour smoothing.
- Gland-dominant cases: Direct excision to remove the dense disc beneath the areola.
- Mixed cases: Liposuction plus excision for a flatter, more stable contour.
In higher grades, we also discuss skin behaviour. We do not promise “shrink-wrap” tightening. We plan for what your tissue can realistically do.
What changes the plan (and why “similar photos” can mislead)
Small details drive outcomes. Skin elasticity can make two Grade 2 chests behave like entirely different surgeries. Asymmetry is common and must be planned for, not “fixed later”. We also look at areola diameter, nipple position, and how the chest sits on your pectoral frame.
- Skin quality: good recoil vs laxity changes what we can achieve without additional steps.
- Areola characteristics: size and position affect scar strategy and final aesthetics.
- Asymmetry: one-sided gland dominance is common and needs tailored correction.
- Chest shape: pectoral development and ribcage structure influence contour goals.
Our objective remains consistent: a masculine, natural-looking chest that does not draw attention. That is the point.
Which Technique Actually Removes Gynaecomastia: Liposuction, Excision, or Both?
This is where most online content becomes vague. We keep it specific. The technique is chosen based on what is physically causing the chest prominence: fat, gland, skin, or a combination of all three. If you only remove fat when gland is the real driver, the chest can still look “puffy”. If you only excise gland without contouring the surrounding fat, the chest can look flat but uneven. Precision matters.
Gland excision vs liposuction: what each method can (and cannot) do
Patients often search gland excision gynaecomastia vs. liposuction because they are trying to understand why one surgeon recommends one approach and another says the opposite. In reality, neither technique is “better” in isolation. Each solves a different problem.
- Liposuction removes fatty volume and helps refine the overall contour across the chest.
- Excision removes the firm glandular tissue beneath the nipple-areola complex.
- Skin management (when needed) addresses laxity rather than volume.
In true gynaecomastia, gland is common. That is why an excision-capable plan is important, even if liposuction is also part of the strategy.
The combined approach (the most common “expert patient” plan)
For many men, the best answer is not “either/or”. It is liposuction and gland excision in a single, carefully sequenced plan. Liposuction creates the smooth contour. Excision removes the dense core that liposuction cannot reliably break down.
- Why we combine: better shape control, lower chance of residual fullness, more predictable chest flattening.
- Who benefits most: mixed-tissue cases (common in Simon Grade 2A/2B), and men with areolar puffiness.
- What we aim for: a natural male chest, not a hollowed-out look.
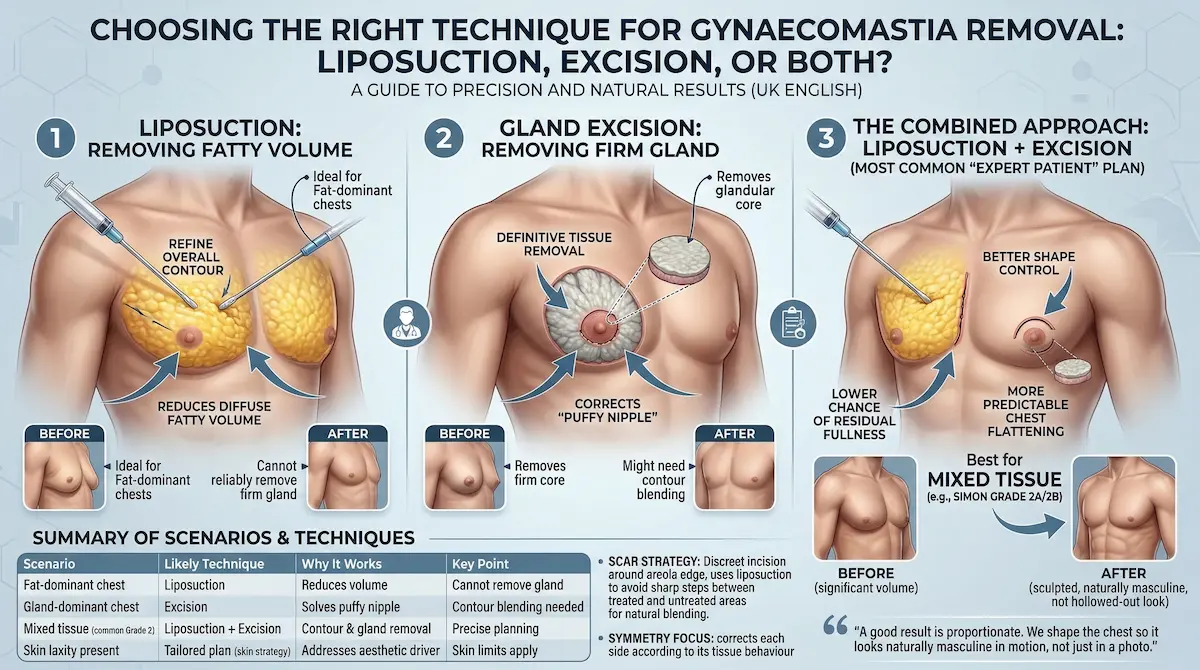
Scar strategy and contour control (small details that change outcomes)
Most UK patients are not frightened of a small scar. They are frightened of a visible “operated” result. We plan incision placement and tissue removal to minimise that risk. Scar position is chosen to be discreet, and contour transitions are softened so the chest looks athletic rather than surgically flattened.
- Incision planning: typically around the areola edge, where the colour change helps camouflage the line.
- Contour blending: liposuction is used to avoid sharp steps between treated and untreated areas.
- Symmetry focus: we correct each side according to its tissue behaviour, not by using a “one-size” template.
| Scenario | Primary issue | Likely technique | Why it works | Common limitation |
|---|---|---|---|---|
| Fat-dominant chest | Diffuse fatty volume | Liposuction | Reduces volume and smooths the contour | Will not reliably remove firm gland |
| Gland-dominant chest | Dense disc under areola | Excision | Removes the tissue causing “puffy nipple” | May need contour blending for a natural finish |
| Mixed tissue (common) | Fat + gland | Liposuction + excision | Combines contour refinement with definitive tissue removal | More planning required to avoid overcorrection |
| Skin laxity present | Excess skin behaviour | Tailored plan (may include skin strategy) | Addresses the aesthetic driver, not just volume | Skin tightening has realistic limits |
Surgeon’s Insight: A good result is not just “flat”. It is proportionate. We shape the chest so it looks naturally masculine in motion, not just in a before-and-after photo.
Local, Regional or General Anaesthesia: What’s the Real Difference?
Men researching awake surgery usually want one thing: a safer-feeling pathway with a clearer recovery profile. That starts with understanding the language. “Local” and “regional” are often used loosely online, and “general” gets presented as either harmless or terrifying. The truth is more balanced. We explain the options in plain clinical terms so you can make a confident decision.

Local vs regional: scope, not just sensation
If you’ve searched the difference between regional and local anaesthesia, the key is coverage. Local anaesthesia numbs the surgical field itself. Regional anaesthesia targets larger nerve pathways to numb a broader region of the body. For gynaecomastia, we typically use local infiltration within the chest tissues, sometimes supported by light calming medication when appropriate.
- Local anaesthesia: targeted numbing where we operate.
- Regional anaesthesia: broader nerve-based numbing across a region.
- General anaesthesia: you are unconscious with airway management and systemic anaesthetic drugs.
How local anaesthetic works (the pharmacology in one clear concept)
The local anaesthesia mechanism of action (MoA) is straightforward: it blocks sodium channels in nerve fibres, preventing pain signals from travelling. That is why the injection technique matters. A well-executed infiltration creates a stable, numb field so the procedure is controlled and comfortable.
- What you feel: pressure and movement, not sharp pain.
- What we control: comfort through careful dosing, slow delivery, and tissue-specific placement.
- What we monitor: your wellbeing throughout, including any early warning signs that dosing must be adjusted.
Post-op experience: nausea, cognition, and “feeling like yourself”
UK patients commonly compare feeling sick after local anaesthesia vs. general because they want to avoid the “wiped out” day that can follow a general anaesthetic. Many men feel more functional on an awake pathway, especially when pain control is sensible and opioid-heavy regimens are avoided. That said, individual responses vary. We plan around your medical history, your anxiety profile, and your recovery priorities.
- Nausea risk: often lower without full GA, but medication choices still matter.
- Clarity: most patients feel more alert sooner, particularly if we keep sedation light and appropriate.
- Autonomy: you stay in control of your breathing and communication during the procedure.
The Local Infiltration Anaesthesia Technique Used in Awake Gynaecomastia Surgery
The comfort of awake surgery is not luck. It’s technique. We build a stable numb “field” by infiltrating local anaesthetic into the exact tissue planes we operate in, then we work methodically within that boundary. Done properly, you feel pressure and movement, not sharp pain.
What “local infiltration” actually means (and why it is different to a quick injection)
Local infiltration anaesthesia technique means we distribute local anaesthetic through the chest tissues in a controlled pattern, rather than relying on one or two superficial injections. The goal is uniform coverage. That is what makes theatre time calm and predictable.
- Layer-specific placement: we numb the pathways where sensation travels, not just the skin.
- Incremental delivery: we place small amounts, reassess, then continue until the field is stable.
- Comfort strategy: slow injection and correct plane selection reduces sting and pressure.
Tumescent technique: why we dilute and distribute
When liposuction is part of your plan, we often use tumescent local anaesthesia. This involves a larger volume of dilute solution to expand the tissue planes. It makes fat removal smoother and helps reduce bleeding.
- Practical benefit: the tissue becomes firmer and easier to contour.
- Safety logic: dilution and staged delivery supports controlled dosing.
- Recovery benefit: less tissue trauma can mean less swelling for many patients.
Adrenaline in local anaesthesia: not “extra drugs”, a precision tool
Many patients ask about adrenaline in local anesthesia. In the right concentration, it narrows small blood vessels locally (vasoconstriction). That matters for visibility, haemostasis, and a cleaner contour.
- Less bleeding: a drier field makes excision and contouring more precise.
- Longer-lasting numbness: it can slow local absorption and extend effect.
- More comfort: fewer “hot spots” as we work across the chest.
Surgeon’s Insight: “Awake” is not a shortcut. It’s a controlled system: correct tissue planes, careful infiltration, and steady monitoring. That’s how comfort becomes reliable.
Receive a clear, day-by-day itinerary covering arrival, surgery, recovery, and fit-to-fly clearance tailored to your requirements.
Lignocaine Safety in Awake Gynaecomastia Surgery: Dosing, Toxicity, and LAST
If you are an expert patient, you will eventually search lignocaine dosing. That’s sensible. Local anaesthetic safety is about calculating limits, staying within them, and having a protocol for the rare event that something feels wrong. We do not brush this off with vague reassurance.
“Maximum dose” is weight-based and context-dependent
Men often ask about the maximum dose of lignocaine for local anaesthesia. The safe ceiling is not a single number that applies to everyone. It depends on your weight, the concentration used, whether adrenaline is included, and your individual medical history.
- Our approach: we calculate a personalised maximum, then plan to stay comfortably below it.
- Why this matters: toxicity risk rises when dosing is rushed or poorly tracked.
- What you should tell us: heart history, liver issues, medication use, previous reactions.
How we deliver lignocaine: the logic behind incremental dosing
The phrase lignocaine injection for local anaesthesia dose sounds like a single “shot”. In reality, safe delivery is staged. We infiltrate, we check the effect, we continue. That is part of the technique to produce local anaesthesia, not an afterthought.
- Slow and steady: comfort improves and dosing remains controlled.
- Field testing: we confirm numbness before moving deeper.
- Monitoring: we watch how you feel, not just the clock.
LAST: what it is, what to watch for, and how we de-risk it
Systemic toxicity and local anaesthetic toxicity (LAST) is rare, but you deserve straight talk. It refers to unwanted systemic effects when local anaesthetic levels rise too high. Transparency is part of safety.
- Early warning signs can include: unusual dizziness, ringing in the ears, metallic taste, or a sudden sense that “something is off”.
- How we reduce risk: proper calculation, incremental delivery, and continuous observation in a controlled theatre environment.
- Our rule: if you report a concerning symptom, we stop and reassess. No ego. No rushing.
This is exactly why medically literate patients often prefer an awake pathway. You stay communicative. You are part of the safety system.
Receive a clear, day-by-day itinerary covering arrival, surgery, recovery, and fit-to-fly clearance tailored to your requirements.
Awake Gynaecomastia Surgery Step-by-Step: What Happens in Theatre on the Day?
On the day of surgery, most anxiety comes from uncertainty. So we remove the mystery. We run a structured pathway: checks, marking, local anaesthetic infiltration, the surgical work, then a monitored recovery period before discharge. Because this is an awake pathway, communication stays open throughout.
Your role is simple: arrive prepared, follow the plan, and tell us how you feel. Our role is more complex: maintain comfort, precision, and safety from the first blood pressure reading to the final dressing.
Pre-op checks, marking, and consent (what we confirm before anything starts)
We start with medical checks and a final review of your plan. This is where we confirm your tissue diagnosis, your Simon grade, and the technique we are using on each side. We also review your medication list and any bleeding-risk supplements.
- Vital signs and screening: we confirm baseline safety before entering theatre.
- Marking: we plan the contour in standing position, not lying down.
- Consent: we discuss risks, scarring, symmetry limits, and realistic goals.
Comfort plan: local infiltration, timing, and what you can feel
Once you are in the operating theatre, we create the numb surgical field first. We infiltrate local anaesthetic in stages, then allow adequate time for it to take full effect. We test the area before we begin the main surgical work.
- What you may feel: pressure, movement, mild vibration from liposuction.
- What you should not feel: sharp pain or “burning” during the core steps.
- How we respond: if you feel pain, we pause and re-numb. No rushing.
The surgical steps: liposuction, excision, haemostasis, closure
Technique is selected based on your anatomy. If liposuction is planned, we contour first to define the chest shape. If gland excision is needed, we remove the firm gland carefully and preserve a natural transition under the areola. We then secure haemostasis, close, and apply dressings.
- Contour creation: smooth transitions matter as much as volume reduction.
- Gland removal: targeted excision to reduce puffiness and restore a flatter profile.
- Closure: precise layers and dressings designed to protect the shape.
Immediate aftercare: monitoring, discharge criteria, and the first 24 hours
After surgery, we monitor you for stability, comfort, and early swelling patterns. You receive clear written aftercare instructions and a direct contact route for questions. Because you are not recovering from a full general anaesthetic, discharge can be smoother for suitable patients.
- Monitoring: we assess comfort, bleeding risk, and vital signs before discharge.
- Medications: we explain what to take, when to take it, and what to avoid.
- Clear boundaries: we tell you what is normal, and what is not.
Surgeon’s Insight: A calm theatre experience is engineered. We build it with planning, measured technique, and continuous feedback from you.
From VIP airport transfers to 5-star hotel accommodation, we manage every detail. Enjoy a premier medical travel experience in Istanbul.
Awake Gynaecomastia Recovery & Aftercare: How Long Does Healing Take?
Recovery is where trust is either reinforced or lost. We keep it structured and honest. Your chest will look “improved” early, but it will not look “final” early. Swelling, firmness, and contour settling take time, and that timeline varies by your grade, tissue type, and how faithfully you follow garment protocols.
Our job is to give you a realistic roadmap. Your job is to stick to it, even when you feel fine. That discipline is what protects your final contour and scar quality.
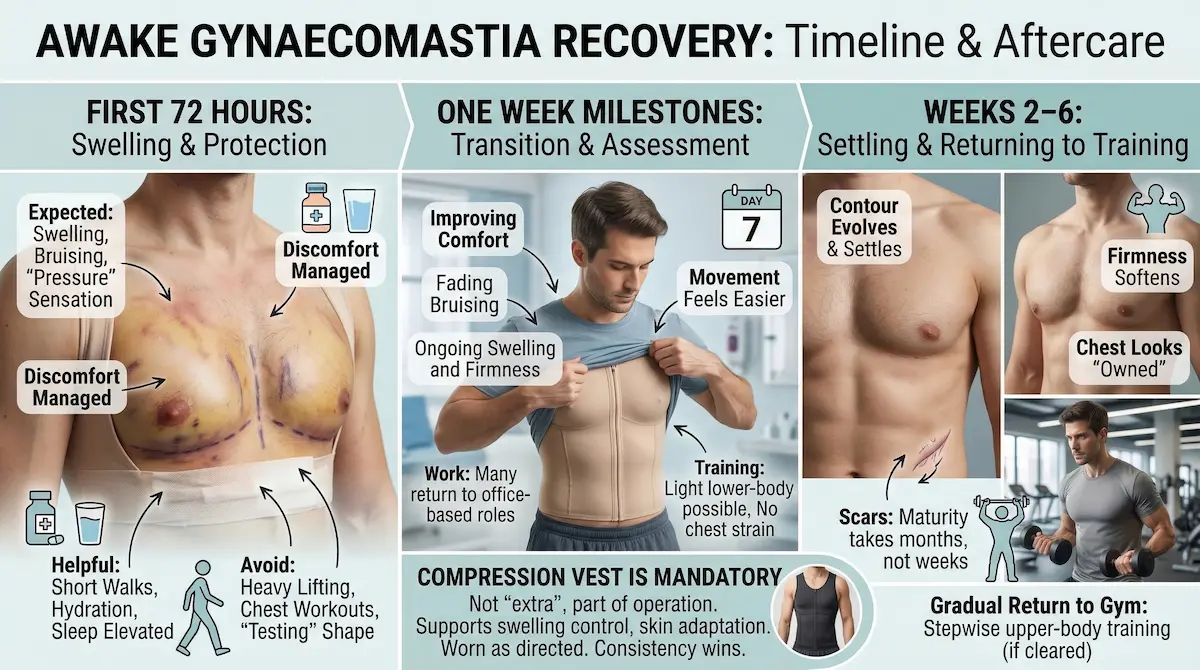
The first 72 hours: swelling control and protecting the contour
The first three days are about stabilising. Expect swelling, bruising, and a tight “pressure” sensation across the chest. Many patients manage discomfort with simple medication such as paracetamol, but your plan is individual.
- Normal: swelling, bruising, mild firmness, sensitivity around the areola.
- Helpful: short walks, hydration, sleeping slightly elevated.
- Avoid: heavy lifting, chest workouts, and “testing” the new shape by poking.
One week milestones: what changes by day 7
Most UK patients ask about the gynaecomastia surgery recovery time (1 week post-op) because they are planning travel, work, and social downtime. At one week, bruising is often fading and movement feels easier, but swelling is still present. The chest may look uneven day-to-day; that is common. We judge progress by trend, not by a single morning in the mirror.
- Common at day 7: improving comfort, ongoing swelling, firmness under the areola.
- Work: many office-based patients can return earlier than gym-based patients.
- Training: light lower-body movement may be possible, chest strain is not.
Compression garments: why the vest is not optional
Wearing a compression vest is not “extra”. It is part of the operation. The compression vest after gynaecomastia surgery supports swelling control, reduces fluid build-up risk, and helps the skin adapt to the new contour. We tell you exactly how long to wear it and how to fit it properly.
- Fit matters: firm support, not painful restriction or breathing difficulty.
- Consistency wins: irregular use is a common reason for prolonged swelling.
- Skin care: we advise simple strategies to reduce irritation under the vest.
Weeks 2–6: settling, scar maturity, and returning to training
Weeks two to six are where the shape becomes more predictable. Swelling gradually reduces, firmness softens, and the chest starts to look “owned” rather than “operated”. Training returns in phases, based on your healing and the extent of excision. We give you a stepwise plan so you do not sabotage a good result by doing too much too soon.
- Week 2–3: more daily normality, but contour still evolving.
- Week 4–6: gradual return to upper-body training if cleared and comfortable.
- Scars: early redness is normal; maturity takes months, not weeks.
We utilise advanced Hyperbaric Oxygen Therapy (HBOT) to minimise downtime and enhance your healing process. Safety is our primary commitment.
Practical Questions UK Patients Ask: Driving, Eating, and Flying
Most men don’t just want a better chest. They want control over the week that follows surgery. That’s why practical queries matter as much as technique. A good plan answers the everyday questions before you need to ask them at 2am. We give clear boundaries, not vague reassurance.
Because we perform surgery under local anaesthesia (with optional calm, light support where appropriate), your post-op experience can feel more “functional” than a full general anaesthetic pathway. Still, it’s surgery. Your judgement, comfort, and safety come first. We build your guidance around that.
Can I drive after local anaesthesia?
The phrase can i drive after local anaesthesia? usually means: “Will I be alert enough, and is it safe?” Our default advice is conservative. Even if you feel fine, driving too soon is not worth the risk. Pain, stress, fatigue, and any calming medication can all change reaction time.
- Our approach: we advise you to arrange transport on the day of surgery.
- Why: you may be tired, tender, and less mobile than you expect.
- When you can consider driving again: once you feel fully clear-headed, can manoeuvre comfortably, and are not taking medication that affects concentration.
We will give you a personalised recommendation based on what was done, what medication you received, and how you feel before discharge.
Can I eat before local anaesthesia?
Another common search is can i eat before local anaesthesia? This question often comes from people who associate surgery with strict “nil by mouth” rules. Local anaesthesia can allow a more flexible plan than general anaesthesia. Even so, we don’t treat food as casual. We plan it.
- What we typically prefer: a light meal and good hydration, timed sensibly.
- What we avoid: heavy, greasy meals that can trigger nausea or reflux.
- What changes the rule: if you will receive calming medication, we may adjust the timing to keep you comfortable and safe.
We give you exact instructions in writing as part of your pre-op plan, so there is no guesswork.
Flying home: timing, swelling, and comfort planning
Flying is not a “yes or no” topic. It’s a risk-managed decision. Swelling can increase with travel, and long sitting can make you feel stiff and tight in the vest. The solution is not to panic. It’s to plan properly.
We organise your schedule around sensible milestones: early checks in Istanbul, a final review before you leave, and clear guidance on what to watch for at home. For UK patients, this is also where aftercare confidence matters. We keep the line open after you fly back.
- Comfort tactics: gentle walking, hydration, and vest fit checks.
- Swelling reality: mild fluctuation is common after travel.
- Red flags: sudden worsening pain, significant one-sided swelling, or symptoms that feel “not normal” for you.
Some men explicitly look for flight-ready recovery protocols. Our view is simple: “flight-ready” is not a slogan. It is a structured plan, backed by monitoring and clear instructions.
Our Premium Recovery Protocol: HBOT and LLLT
Recovery is where most clinics become passive. We don’t. We treat the post-op phase as a clinical workflow, not an afterthought. That is why we built a technology-supported protocol to reduce swelling, support tissue repair, and protect scar quality. The goal is not drama. It’s predictability.
We also know what UK patients are trying to avoid. They want downtime that is shorter, calmer, and easier to manage. They want to feel “like themselves” sooner. Our protocol is designed for that kind of patient.
HBOT: oxygen support for tissue recovery
HBOT for surgical recovery refers to Hyperbaric Oxygen Therapy. The concept is straightforward: controlled oxygen delivery can support tissue healing and help the body handle inflammation. We use it as part of a structured post-op programme, not as a stand-alone “add-on”.
- Why we use it: to support healing physiology in the early recovery window.
- What patients usually care about: swelling control and a smoother return to routine.
- How we frame it: a supportive tool within a wider aftercare plan (compression, monitoring, sensible activity).
LLLT: scar biology, not “scar cream marketing”
LLLT (Low-Level Laser Therapy) for surgical recovery is used to support scar behaviour and tissue calm. UK patients often worry about visible scars more than pain. That’s reasonable. Scar quality matters in a male chest, especially around the areola edge.
- How we use it: as part of aftercare, alongside correct wound care and compression.
- What it targets: tissue irritation, early scar behaviour, and recovery comfort.
- How it fits your goal: a chest that looks natural, not “treated”.
You may also see search phrases like “LLLT scar healing therapy Turkey”. The country is not the point. The protocol is.
Why recovery tech supports the “awake” strategy
Awake surgery is about reducing perioperative load and keeping recovery more functional. Recovery technology complements that logic. It gives your body support in the exact window when swelling and bruising are most active. Used properly, it can make the early phase calmer.
We still keep expectations realistic. No protocol deletes biology. Healing takes time. Our job is to reduce friction, keep you safe, and guide you with the same clarity you’d expect from a UK-standard consultation.
Surgeon’s Insight: We don’t chase extremes. We build a predictable recovery so your result settles naturally. That is “Rejuvenation, Not Alteration.”
Safety & Risks: Is Awake Gynaecomastia Surgery Dangerous?
Every honest surgical guide must include risk. Not to alarm you, but to keep you informed. Awake gynaecomastia surgery changes the anaesthetic profile, but it does not remove the fact that this is still a surgical procedure involving tissue removal, healing biology, and individual variability.
Our approach is risk-first: identify preventable problems early, use measured technique in theatre, and give you a recovery plan that reduces avoidable complications. “Safe” is not a feeling; it is a system.
Common risks (and what they actually look like)
Most complications are manageable when identified early. That is why we focus on predictable patterns and clear communication, especially for UK patients travelling home soon after surgery.
- Haematoma: a collection of blood that can create sudden swelling and increased pressure.
- Seroma: a fluid pocket that may feel like a soft, shifting swelling.
- Infection: uncommon with proper technique, but requires early attention if suspected.
- Contour irregularity: minor unevenness can happen during early swelling; true issues are assessed after settling.
Nipple sensation, scarring, and asymmetry (the “real world” outcomes)
Most men tolerate the scar extremely well when it is planned correctly, but you should understand what “normal” can include. Temporary nipple sensitivity changes are common. Long-term changes are possible. Asymmetry is also common in nature, and surgery improves symmetry but does not guarantee mirror perfection.
- Sensation changes: often temporary; sometimes longer-lasting.
- Scarring: early redness is typical; maturity is measured in months.
- Asymmetry: planned for at the start, not “fixed later”.
Risk mitigation: screening, sterile theatres, and follow-up cadence
Reducing risk is mostly about discipline. We screen properly, track local anaesthetic dosing, maintain sterile technique, and give you a defined follow-up pathway. When you travel, structured aftercare matters even more.
- Pre-op: medical history, medication review, and risk factor correction (smoking, supplements).
- In theatre: controlled infiltration, haemostasis, and careful contour strategy.
- Post-op: compression, scheduled check-ins, and rapid access if something feels off.
From VIP airport transfers to 5-star hotel accommodation, we manage every detail. Enjoy a premier medical travel experience in Istanbul.
Is Gynaecomastia Surgery Safe in Turkey? A UK-Standard Checklist
UK patients often arrive at this question after reading generic “cheap Turkey surgery” narratives. That framing is unhelpful. Safety is not a nationality. It is governance: surgeon training, facility standards, protocols, and continuity of care. If you evaluate those elements objectively, the conversation becomes clear.
Our aim is to give you a checklist that mirrors UK expectations: transparent credentials, documented workflows, and follow-up you can rely on after you return home.
What “safe” means in practice (not in marketing)
When you compare gynaecomastia surgery London vs. Istanbul, the meaningful differences are not slogans. They are process and standards. A premium centre should feel clinically organised and audited, not sales-driven.
- Facilities: sterile theatre standards, monitoring, and recovery observation.
- Team: clear role allocation, not a “one person does everything” setup.
- Protocols: written pathways for complications, pain control, and follow-up.
Continuity of care after you return to the UK
Travelling for surgery is only sensible when aftercare is real. We structure remote follow-ups, keep your documentation organised, and maintain direct access for clinical questions. For the expert patient, this matters as much as the operation itself.
- Scheduled check-ins: planned touchpoints, not “message us if you need”.
- Documentation: clear operative notes and aftercare instructions.
- Responsiveness: fast access if symptoms change.
Neutralising “Turkey bias” through transparency
Many UK clinics reduce information to keep things “simple”. We do the opposite. We explain technique selection, anaesthetic logic, and recovery protocols in clinical language. That depth is not intimidation; it is respect.
If you are comparing against the UK private sector (Harley Street, Nuffield, regional providers), your decision should be based on evidence: surgeon credentials, grade-matched results, complication management, and communication quality.
Share your photos and medical history to receive a personalised assessment from our European Board-certified facial surgery team.
Awake Gynaecomastia Surgery 2026 Cost Analysis (UK vs Istanbul)
Cost is a legitimate question, but it is often asked in the wrong way. The right question is: “What does this price include clinically, and what risks does it reduce?” Premium care is not just a nicer room. It is surgeon time, planning depth, monitoring, and structured aftercare.
UK patients commonly compare private quotes against Istanbul and try to map “value” onto cost alone. We prefer a clearer framework: price anchored to clinical scope, facility standards, and recovery support.
London vs Istanbul: clinical scope and economic reality
Search intent like gynaecomastia surgery London vs. Istanbul usually reflects two drivers: UK pricing and UK waiting constraints. London can offer excellent care, but it is often priced at a level that pushes many patients into “delay mode”. Istanbul can be a rational choice when delivered at premium standards with transparent governance.
Benchmarking against UK providers (Nuffield, Signature Clinic, and regional hubs)
Patients frequently search comparisons such as Nuffield Health gynaecomastia cost vs. Istanbul Premium or private gynaecomastia surgery cost UK vs. Signature Clinic. These queries are not “bargain hunting”; they are benchmarking exercises. If you are also looking at regional pricing (for example, Manchester/Edinburgh/Leeds surgery cost), the same logic applies: compare like-for-like clinical scope.
Istanbul premium pricing: what “premium” should include
When you see terms like Istanbul gynaecomastia cost (Premium Tier), the word “premium” should translate into defined deliverables: surgeon-led planning, monitored care, and aftercare infrastructure. We discuss your plan transparently during consultation, including what is included and what is optional.
| Comparison point | UK private pathway (typical) | Istanbul premium pathway (what to expect) | What it means for you |
|---|---|---|---|
| Pricing context | Often higher, especially in London | Competitive vs UK, but not “budget” in premium tier | Value depends on clinical scope, not just headline price |
| Anaesthetic model | Frequently GA-based | Awake/local-focused options for suitable candidates | Different recovery profile and different risk trade-offs |
| Aftercare structure | In-person follow-ups within the UK | On-site checks + remote follow-up after return | Continuity must be planned, not improvised |
| Recovery support | Varies by provider | May include advanced recovery protocols (HBOT/LLLT) | Can reduce early recovery friction for some patients |
Receive a 100% transparent, all-inclusive quote tailored to your needs. No hidden fees—just world-class care at an accessible price.
Finding the Best Awake Gynaecomastia Surgeon: Credentials, Technique, and Evidence
If you only take one thing from this guide, take this: your outcome is largely surgeon-dependent. Facilities matter, but the surgeon’s decision-making matters more. For UK patients, trust is built through credentials, clarity, and a consistent body of evidence—not through flashy branding.
That is why search modifiers like board certified gynaecomastia surgeon are so common. They signal the right instinct: verify training and expertise before you verify price.
What “board certified” should mean in real terms
Certification language varies between countries. The correct approach is not to chase acronyms blindly, but to confirm what they represent: training pathway, specialty focus, and professional accountability. Ask direct questions about who operates, how often they perform gynaecomastia correction, and how they handle revisions.
How to read reviews and avoid being misled
Men often search Harley Street gynaecomastia clinic reviews as a proxy for quality. Reviews can be helpful, but they are not evidence of technique. Use reviews to assess service reliability and communication, not to diagnose surgical skill.
- Look for specifics: mention of recovery support, responsiveness, and realistic counselling.
- Avoid extremes: “perfect, pain-free, instant” language is not clinical.
- Ask for grade-matched cases: compare your anatomy to similar starting points.
Evidence that matters: grade-matched results and revision policy
Serious providers show you results for patients who resemble your Simon grade, tissue type, and skin quality. They also discuss limitations and revision policy transparently. If a clinic avoids these conversations, take that as a signal.
Undergo your procedure with total confidence. Meet our European Board-certified surgeons, who have performed over 2,000 successful facial procedures.
Booking-Level Queries: What “Premium” Means in Istanbul
At high intent, UK patients start using destination keywords. This is normal. But to stay in the premium tier, the key is specificity: technique, surgeon credentials, and clinic standards. A “cheap deal” mindset creates the wrong incentives. A premium mindset is about process quality.
Below, we address the common transactional searches in a clinically grounded way, without pretending there is a single “best” answer for everyone.
Premium gynaecomastia clinic Istanbul: the standards you should demand
If you search premium gynaecomastia clinic Istanbul, you are implicitly asking for a centre that behaves like a specialist unit, not a tourism package. Your checklist should include surgeon-led planning, documented protocols, and robust follow-up.
Awake gland excision surgery Istanbul: who it suits and why it matters
Searches like awake gland excision surgery Istanbul typically come from men who understand that gland is the core problem. The key is selecting the correct technique for your anatomy and delivering it within a controlled local anaesthetic protocol, including dosing discipline and monitoring.
“Best gynaecomastia surgeon in Turkey”: how to evaluate without guesswork
“Best” is not a title; it’s a method. When you search best gynaecomastia surgeon in Turkey, translate it into measurable criteria: experience with your Simon grade, consistency of outcomes, willingness to explain risks, and a transparent revision approach.
Surgeon’s Insight: The best surgeon for you is the one who can explain your plan with clinical precision—and can show consistent results in cases like yours.
Achieve the same high-standard, clinical excellence you expect in the UK or US, but without the premium price tag. Quality meets exceptional value at AKM Clinic.
Your Medical Journey: From Virtual Consultation to Returning Home to the UK
A well-run cross-border pathway is structured and predictable. The aim is to minimise friction while keeping clinical control. For UK patients, that means clear documentation, defined appointment timing in Istanbul, and remote follow-up that continues after you land back in the UK.
We treat your journey as part of the medical plan, not a separate “travel” plan. That’s how you avoid last-minute uncertainty.
Pre-op: photos, medical history, and a plan you can audit
We start with a focused consultation: your concerns, your tissue type, your Simon grade estimate, and your anaesthetic suitability. You receive clear guidance on preparation, including medication adjustments and lifestyle factors that affect healing.
In Istanbul: assessment, surgery, and early checks
Once you arrive, we confirm the plan in person, complete any final checks, and proceed with surgery. After the procedure, we monitor you, fit compression, and provide written instructions. You are not left to “figure it out”.
Back in the UK: remote follow-up and support
After you return, we maintain scheduled check-ins and remain available for clinically relevant questions. The goal is continuity: predictable recovery, early identification of issues, and calm decision-making.
From VIP airport transfers to 5-star hotel accommodation, we manage every detail. Enjoy a premier medical travel experience in Istanbul.
Frequently Asked Questions: Awake Gynaecomastia Surgery
These questions come directly from UK search behaviour—usually from men who are risk-auditing and trying to plan their week. We answer them plainly, without overpromising. Your personalised advice will always depend on your medical history and the exact plan used.
Does local anaesthesia make you loopy?
Local anaesthetic is designed to numb tissue, not alter your mind. Feeling “loopy” is more commonly related to calming medication (if used), pain medicines, dehydration, poor sleep, or anxiety. We keep sedation appropriate and discuss medication effects openly.
Is local anaesthesia painful / how is it given?
You may feel brief stinging or pressure during injection. A proper infiltration technique, slow delivery, and correct tissue-plane placement reduce discomfort significantly. During the procedure, you should feel pressure and movement rather than sharp pain. If you feel pain, we pause and re-numb.
Why can’t the NHS just do this?
Many men search NHS gynaecomastia surgery criteria because access can be restrictive and waiting times can be long. If you are not eligible or do not want to wait, private care becomes the alternative. The decision should still be clinical: correct diagnosis, stable weight, and a realistic plan.
How do I compare Signature Clinic and Istanbul fairly?
Queries like Signature Clinic gynaecomastia vs. Istanbul are best answered by comparing like-for-like: surgeon involvement, technique offered (excision + contouring), anaesthetic model, facility standards, and aftercare structure. Avoid comparing only headline price.
Medical Disclaimer: This page is for general information and does not replace a medical consultation. Suitability for awake gynaecomastia surgery, anaesthetic planning, dosing decisions, and recovery timelines must be assessed individually by a qualified clinician based on your health status, medications, and examination findings. If you develop concerning symptoms after surgery (for example, sudden swelling, increasing pain, fever, or symptoms that feel abnormal for you), seek urgent medical advice.
Awake Gynaecomastia Surgery: Patient Stories
Awake Gynaecomastia Surgery Surgeons
Awake Gynaecomastia Surgery Cost in Turkey
Starting from ~ £2800
* There are no hidden fees or unexpected charges.
- Your PersonalisedAwake Gynaecomastia SurgeryProcedure
- All Specialist Surgeon & Anaesthesia Fees
- All Pre-Op Tests & Post-Op Check-ups
- 5-Star Hotel Accommodation (incl. breakfast)
- All Private VIP Airport & Clinic Transfers
- 24/7 Dedicated Patient Coordinator & Translation Services
Awake Gynaecomastia Surgery: A Cost Comparison
| City | Cost |
|---|---|
| London (Harley Street) | ~£6,500 |
| Manchester | ~£5,500 |
| Birmingham | ~£5,000 |
| Glasgow | ~£4,800 |
| Liverpool | ~£4,500 |
Awake Gynaecomastia Surgery: Patient Reviews
Jammal Canada
I have had face and neck lift with AKM Clinic they have been so good to me and my operation went so smoothly🥰 i would like to thank my doctor here and also to the team 💐

Ava Canada
Thank you AKM Clinic for giving me my confidence back! Had facelift + temporal lift 3 months ago and the outcome is already stunning. Special thanks to Hande!

Jakayla USA
Had a deep plane facelift and lower eyelid procedure at AKM Clinic 7 months ago. The results are fantastic - very subtle and natural. I didn’t expect the entire experience to be so comfortable. Hande managed everything and kept in contact even after I returned to USA. I’m beyond pleased with the outcome and the care I received. Would do it again in a heartbeat!

Barbara United Kingdom
It has been 4 months since my surgery. Everything is great, The most important thing is l love the way l look, l look exactly how l wanted. Meaning l look natural, just almost 40 years younger. I pulled Facebook - majority voted 37ys. I also had face, neck, chest, and hands CO2 laser. My skin is flawless.

Lisa Canada
I had a face, neck and arm lift at AKM. I’m just over 4 weeks post and couldn’t be happier with the results. The entire experience was wonderful! My coordinator, Khadija made me feel comfortable from beginning to end! I highly recommend AKM and will definitely go back for other procedures!

Julie USA
I am beyond grateful I went with AKM Clinic for my deep plane face and neck lift, upper eyelid, and co2 laser. Dr. Akif has magic hands and my results are truly incredible! I came from the US and assistant Emine was the best in assuring every detail was coordinated and communicated with me beyond my expectations every step of the way. 10 out of 10 to the entire team! I couldn’t be more pleased!

Ready to Begin Your Own Transformation Journey?
Join the 2,000+ patients who have trusted Dr Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, naturally restored you begins with a simple, no-obligation conversation. Contact us today from the UK for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. There are no hidden fees.
#2: Secure Your Date & VIP Booking
Once you are ready, our dedicated patient coordinators will help you secure your procedure date. We will handle all your bookings, including your 5-star hotel accommodation and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you will meet your specialist surgeon to finalise the details for your natural, subtle, and restored new look.













