Tube Tummy Tuck: The Drainless Abdominoplasty

- Tube tummy tuck explains drainless abdominoplasty using internal fixation to reduce fluid buildup and drain reliance.
- Recovery-focused guidance for parents covers mobility, lifting limits, red flags, and realistic healing milestones.
- Safety-first, science-informed expectations clarify seroma risk, follow-up importance, and who qualifies for drainless techniques.
- Scar planning within the bikini line highlights incision strategy and avoiding extra tummy tuck drain tube scars.
Summary generated by AI, fact-checked by our medical experts
If you’re researching tube tummy tuck, you’re likely trying to solve a very specific problem: how to get a flatter abdomen without the discomfort and hassle of traditional drains. In online forums and surgeon consults, the same questions repeat—“Will I need a tummy tuck drain?”, “What is the drain tube after tummy tuck like?”, “How painful is drain tube removal after tummy tuck?” This guide breaks down the concept of a “Tube Tummy Tuck” (often used to describe no drain tummy tuck or drain free tummy tuck approaches), how it works, who it fits best, and what outcomes are realistic—through the lens of medical science and responsible surgical principles.
Important note: “Tube tummy tuck” isn’t always a standardized textbook term. Patients often use it to describe a technique that minimizes or avoids external drainage by reducing “dead space” and managing fluid more intelligently. In a consultation, you should ask exactly which method your surgeon uses and why.
Key takeaway: A “drainless” abdominoplasty aims to reduce fluid collection risk by closing internal spaces and supporting tissues—rather than relying on a drainage tube after tummy tuck. It can improve comfort and simplify recovery, but it does not mean “zero risk” of swelling or seroma.
| Topic | Traditional Tummy Tuck (with drains) | “Tube/Drainless” Approach (no external drains) |
|---|---|---|
| Fluid management | Relies on a tummy tuck drain to remove fluid during early healing | Relies on internal fixation + space reduction; may still require monitoring for fluid |
| Daily care | Drain emptying, measuring output, hygiene around tubing | No external tubing care; compression and follow-up remain essential |
| Common patient concern | Drain tube removal after tummy tuck and accidental tugging | “If there’s no drain, what happens if fluid builds up?” |
| Scarring | May include a small tummy tuck drain tube scar at drain exit site | No drain exit scar; incision scar still depends on technique + healing |
Exploring all your abdominoplasty options? This guide focuses strictly on the drainless (tube) technique and fluid management. For a complete overview of the surgery, including our all-inclusive VIP packages, muscle repair, and total costs, please visit our main Tummy Tuck Surgery in Turkey guide.
Table of Contents
Understanding the “Tube” (Drainless) Technique
When patients say tube tummy tuck surgery, they’re often referring to a drainless strategy that reduces the need for a drain tube after tummy tuck. Traditional abdominoplasty creates a space under the lifted abdominal skin; during early healing, fluid can collect there. Historically, a tummy tuck drain was used to evacuate that fluid. Drainless methods aim to reduce the internal space where fluid collects and stabilize tissues as they heal—so an external drain tube tummy tuck setup is often unnecessary. The best way to evaluate claims is to ask for the surgeon’s exact technique and their management plan if fluid does occur.
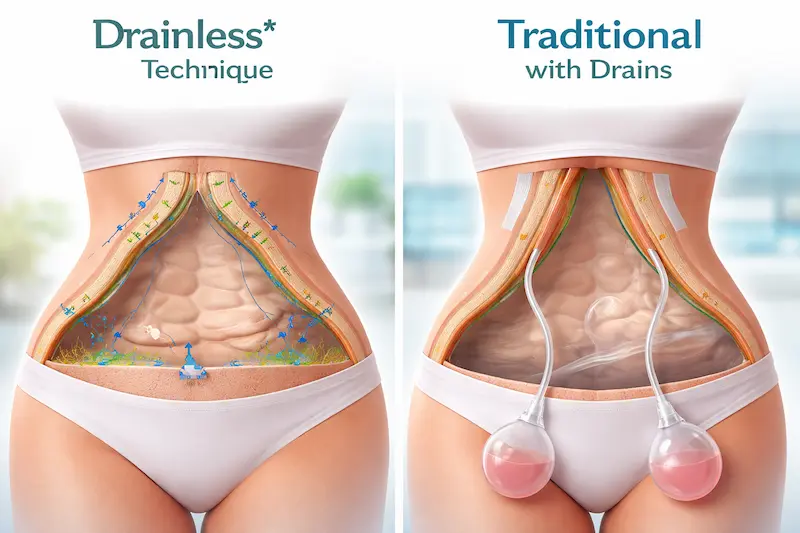
What “Tube Tummy Tuck” Means (Concept, Not a Marketing Term)
In patient language, “tube tummy tuck” may describe either (1) a drainless tummy tuck (no external drain tubes), or (2) the opposite—concerns about “the tube” people saw in photos after surgery. Because the phrase is inconsistent, your consultation should clarify terminology: Are they offering a no drain tummy tuck (drainless technique), or are they describing a standard approach where a tummy tuck tube is used temporarily for drainage?
One layer this section doesn’t address: drainless techniques can stack with awake protocols for selected candidates—producing a meaningfully different perioperative experience. “Drainless plus awake” reduces both the at-home drain logistics AND general anesthesia exposure. The candidate filter is stricter (cardiac sensitivities, anxiety profile, BMI, surgical extent), but for the right patient, the combination compresses the disruption window significantly.
The full awake-protocol mechanics, candidacy filter, and how it interacts with drainless planning are detailed in our awake-procedure overview.
Preserving Lymphatic Vessels to Reduce Fluid Buildup
One reason fluid accumulates after abdominoplasty is temporary disruption of lymphatic channels. Some surgeons modify dissection planes and tissue handling to reduce unnecessary trauma, which may support smoother recovery. This is where scientific research and evolving surgical technique matters: better respect for anatomy and gentler handling can reduce swelling and may reduce the chance that a drainage tube after tummy tuck is needed.
Progressive Tension / Internal Fixation: How Surgeons Minimize “Dead Space”
A major principle behind drainless surgery is minimizing “dead space”—the potential pocket where fluid can collect. Many surgeons accomplish this using internal fixation methods (often called progressive tension sutures). By anchoring tissues in a controlled way, the body has less room to create a fluid pocket, and external drainage becomes less necessary. In practical terms: this is the engineering behind drain free tummy tuck approaches.
“Engineering behind drain free tummy tuck” needs the actual numbers behind it. A 2025 systematic review and meta-analysis published in the Aesthetic Surgery Journal—Oxford University Press, ASAPS official—pooled data from 24 studies and 750 patients (including 2 randomized controlled trials) using PRISMA, AMSTAR 2, and GRADE methodology. The pooled finding: progressive tension suturing significantly reduced postoperative seroma rates compared to drainage alone (relative risk 0.34, P=0.001), with no significant differences in hematoma, infection, or wound dehiscence rates.
The full tension-suturing meta-analysis is the strongest current evidence synthesis for the drainless mechanism—worth knowing the actual numbers when a surgeon describes their technique, rather than relying on terminology alone.
Does “Drainless” Mean “Zero Fluid Risk”? (Seroma Reality & Monitoring)
No. Even with excellent technique, fluid can still accumulate. A responsible plan includes careful follow-up, compression strategy, and a clear protocol if a seroma forms (for example, office aspiration when appropriate). So while the goal is to avoid the discomfort of a drain tube after tummy tuck, you should still ask: “If fluid builds up, what is your management plan—and how quickly do you typically see patients after surgery?”
Who Is an Ideal Candidate—and Who Isn’t? (BMI, skin quality, revision cases, smoking)
Drainless approaches can be especially appealing for patients who are anxious about tummy tuck drain care and want a simpler early recovery. However, candidacy depends on factors like skin quality, amount of tissue to be removed, history of prior abdominal surgery, body mass index, and smoking status. Complex revisions or high-risk cases may require a different fluid-management strategy—occasionally including a temporary drain tube tummy tuck approach if the surgeon believes it improves safety.
One candidate filter this list misses for international patients: flight timing back home. Drainless techniques can shift the safe-fly-home window earlier than traditional drain-based protocols—not because the surgery is “less”—but because there’s no drain emptying, no exit-site care during long-haul travel, and fewer mid-flight equipment concerns. For US/UK/Canada patients planning the Istanbul trip, this changes the realistic time-off-work calculation.
The procedure-by-procedure safe-fly-home windows—including DVT/PE risk timing and how drainless versus drain-based protocols compare—are mapped in our post-op flight timing reference.
Drainless candidacy doesn’t sit alone in the candidacy conversation. It usually rides alongside another decision: how much surgery is being done in the first place. Mini-scope cases produce less dead space, less tissue mobilization, and less fluid risk—so they’re often easier to plan as drainless. Full-scope cases involve broader undermining, more potential dead space, and a different complication risk profile—so the drainless calculation shifts. The two questions—”how much surgery” and “drains or no drains”—are actually one decision, not two.
The full mini-versus-full candidacy framework, including how it intersects with drainless planning, is detailed in our tummy tuck scope decision.
Keyword clarity (so you can ask smarter questions): If you see phrases like drain tube after tummy tuck, drainage tube after tummy tuck, or drain tube removal after tummy tuck, you’re reading about a traditional drain-based recovery. If you see no drain tummy tuck or drain free tummy tuck, you’re reading about techniques designed to avoid those external tubes.
Our surgery dates fill up quickly due to high international demand. Secure your consultation today to plan your ideal travel dates.
Benefits Over Traditional Tummy Tuck
For many patients, the biggest “benefit” of a no drain tummy tuck is simply not having to manage a tummy tuck drain at home. But comfort isn’t the only consideration. From a medical science perspective, the potential upsides are tied to how well the technique reduces dead space, stabilizes tissues, and supports predictable early healing. The key is to separate real advantages from oversimplified claims, and to understand what may still happen during recovery—even without a drain tube after tummy tuck.
Why Patients Walk Upright Sooner
Walking posture after abdominoplasty depends on multiple factors: tension across the lower incision, muscle repair (if performed), swelling, and pain control. Some patients report earlier confidence in movement when they are not worried about tugging a drain tube after tummy tuck. That said, walking upright is still gradual, and your surgeon’s protocol (including compression and activity guidance) matters more than the drain/no-drain label.
Reduced Risk of Seroma and Complications
Drainless methods are designed to reduce seroma risk by limiting the space where fluid can collect. In scientific research on abdominoplasty techniques, approaches that reduce dead space (including internal fixation strategies) are often discussed as ways to reduce seroma rates. However, outcomes vary by patient factors (BMI, smoking, tissue quality), surgical extent, and adherence to aftercare. A responsible surgeon will explain both: what the method aims to improve, and the realistic residual risk.
Three case examples make a point. Thirty across body types, ages, and surgical scopes make a pattern. The cases above show outcomes from individual patients—useful for orientation. The procedure-specific gallery sits one layer above that: a curated archive of tummy tuck and abdominoplasty cases across postpartum, post-weight-loss, mini-scope, full-scope, and combined-procedure presentations. The signal you’re looking for isn’t “the most dramatic after”—it’s “consistency across diverse starting points.”
The full tummy-tuck-only case archive, organized for cross-comparison rather than highlight-reel browsing, is in our abdominoplasty case gallery.
Comfort & Practicality: No Drain Care, Easier Sleep and Mobility
With traditional approaches, patients manage a drain tube tummy tuck setup: emptying bulbs, measuring output, keeping the exit site clean, and avoiding accidental pulling. Eliminating external drains can make day-to-day life simpler in the first week, especially for patients who feel anxious about tubing. This is also why people search phrases like drain tube removal after tummy tuck—they want to know what that moment will feel like and when it happens.
Recovery Experience Differences (Pain, Movement Confidence, Daily Hygiene)
Not having a drain tube after tummy tuck can improve perceived comfort—less “hardware” to protect, fewer dressing changes around exit sites, and often easier shower planning. But it does not eliminate the normal discomfort of abdominoplasty: incision soreness, swelling, tightness, and fatigue. In other words, drainless can simplify the logistics, but it doesn’t turn recovery into “nothing happened.”
“Daily hygiene” is one phrase. International home recovery is a different chapter entirely. Once you’re back in your home country—New York, London, Toronto—the day-to-day adapts to your local network: who handles compression garment changes, when to seek US/UK/Canada-side check-ups for swelling, what your home pharmacy actually stocks for scar care, and how to bridge the geographic gap to your Istanbul surgical team. Drainless simplifies the equipment side; the continuity-of-care side still needs an explicit plan.
The fly-home continuity framework—including pharmacy logistics, local-doctor coordination, and the surgical-team check-in cadence that catches early issues—is in our fly-home aftercare protocol.
Evidence-Based View: What Outcomes Actually Improve—and What Doesn’t Change
Here’s the practical, evidence-aligned way to think about it:
- May improve: drain-related inconvenience, drain-site care, and avoidance of a tummy tuck tube exit wound.
- May reduce: likelihood of requiring a drain tube after tummy tuck in appropriately selected patients with good technique.
- Does not automatically improve: scar quality, long-term contour, or the need for compression and follow-up.
- Still requires: a clear plan for swelling/seroma monitoring—because “drainless” does not mean “fluid can’t happen.”
Surgeon-level question to ask: “If I develop fluid anyway, how do you detect it early, and what is your step-by-step management plan?” A high-quality answer matters more than marketing terms like drain free tummy tuck.
| Patient Question | Traditional (with drains) | Drainless / “Tube” approach |
|---|---|---|
| “Will I have a tummy tuck drain?” | Usually yes, temporarily | Often no (depends on surgeon, case complexity) |
| “What about drain tube removal after tummy tuck?” | A planned step in recovery | Usually not applicable |
| “Will I have a tummy tuck drain tube scar?” | Possible small drain exit scar | Usually avoided (no drain exit site) |
Scar Placement: Hiding It Within the Bikini Line
Scar planning is one of the most “expert patient” concerns because it’s visible, long-term, and emotionally loaded. Whether you choose a traditional technique with a tummy tuck drain or a no drain tummy tuck, you will still have a primary lower abdominal incision scar. What can differ is whether you also have a small secondary mark from a drain exit site (a tummy tuck drain tube scar). The goal is not “no scar”—it’s a scar that is strategically placed, symmetrical, and supported with excellent aftercare.
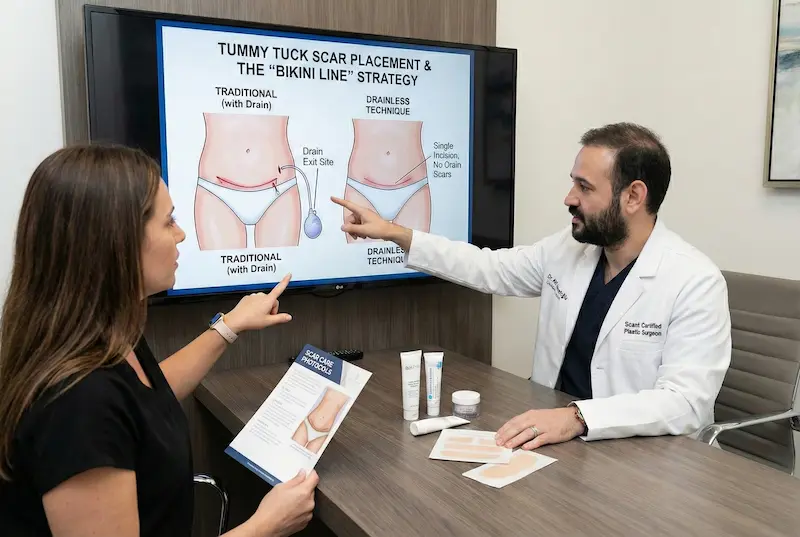
Incision Planning: Anatomy, Clothing Lines, and Symmetry
Incision placement is customized based on your torso length, skin redundancy, and existing scars (including C-section scars). A skilled surgeon plans the incision to sit low enough to be hidden by underwear or a bikini line while maintaining balanced tension across the closure. This is where surgical judgment matters: overly aggressive tightening can pull scars upward; overly conservative tightening may leave laxity. The best approach is individualized, not one-size-fits-all.
Scar Quality Drivers: Tension, Genetics, Aftercare, and Sun Exposure
From a medical science standpoint, scar outcomes are influenced by mechanical tension, inflammation control, and your biology (including genetic tendency toward hypertrophic scarring). Even the best incision placement can be undermined by early strain, smoking, or poor aftercare. This is also why surgeons emphasize compression garments, activity restriction, and structured follow-up—not just the surgical technique.
Scar Maturation Timeline: What to Expect at 6 Weeks, 3 Months, 12 Months
Scar maturation is a process, not a moment. Early scars are often firm and pink; later they soften and fade. Many patients worry too early—before the scar has had time to remodel. A typical progression is:
- 0–6 weeks: incision healing, swelling, sensitivity; scar may look more noticeable.
- 6 weeks–3 months: firmness and color changes; itching can occur as nerves recover.
- 3–12 months: gradual fading/softening; this is when the “final” look becomes clearer.
Scar Care Protocol (Silicone, Massage Guidance, Clinic Follow-Up)
Scar care should be guided by your surgeon because timing matters. Common evidence-informed strategies include silicone-based products, sun protection, and—when appropriate—gentle massage once the incision is fully closed and approved. If you previously had drains, care might also include attention to any drain exit site marks. In a drainless approach, you typically avoid that additional drain-site scar, which is one reason patients seek drain free tummy tuck options.
“Silicone-based products” gets a polite mention in most discharge handouts—and very little explanation behind it. What changes the actual scar appearance is the timing layer: when silicone goes on, when massage starts, when LLLT or HBOT layer in, what’s pointless before week 6, what’s wasted after month 12. The drainless advantage of avoiding a drain-site scar is real, but the primary bikini-line scar still does the heavy lifting on the final aesthetic.
The phase-by-phase scar intervention timeline, the evidence base for each modality, and what’s marketing-driven versus genuinely effective are in our scar healing reference.
What If I Previously Had Drains? (Addressing Drain Exit Marks)
If you’ve had a prior tummy tuck or abdominal procedure with a drainage tube after tummy tuck, you may have small marks where the tubing exited. These are usually minor, but if they bother you, a surgeon can assess whether they can be improved through scar management strategies or revision planning. The best first step is documentation (photos, measurements) and a clear discussion of realistic improvement—because scar “erasure” is not medically realistic.
Recovery Timeline: Returning to Motherhood Duties
Recovery is where most “expert patients” want specifics—especially if you’re caring for children and trying to plan travel, help at home, and a safe return to normal life. Whether your surgery is described as tube tummy tuck surgery, no drain tummy tuck, or drain free tummy tuck, your recovery still involves swelling control, incision protection, mobility, and careful activity limits. The difference is that a drainless strategy often removes the added task of managing a tummy tuck drain and the anxiety surrounding the drain tube after tummy tuck.
Most patients reading “tube tummy tuck” are postpartum—and most postpartum tummy tuck conversations don’t stay isolated for long. Breast volume changes, abdominal skin laxity, and the “everything happened at once” pattern usually mean the question shifts from “drainless tummy tuck” to “which combination of procedures, sequenced how, and is drainless feasible across the combination?” That’s a different planning conversation.
The full combined-procedure logic—how breast and abdominal procedures coordinate, drainless feasibility across multiple sites, and recovery sequencing for postpartum patients—is in our mommy makeover roadmap.

Below is a realistic, science-informed timeline. Keep in mind: your exact schedule depends on the extent of surgery (skin removal, liposuction, muscle repair), your overall health, and your surgeon’s protocol.
“Muscle repair” sounds like a single technical step. In practice it’s the variable that shifts everything else. How much diastasis is being repaired, whether there’s an associated hernia, how the abdominal wall is reapproximated—each one changes recovery restrictions, lifting limits, and even drainless candidacy. The “extent of surgery” sentence above hides a much bigger decision than most patients realize at consultation.
The full diastasis assessment framework and how muscle-repair scope affects the rest of the surgical plan are in our muscle repair context guide.
| Timeframe | What You’ll Likely Feel | What You Should Do | What to Avoid |
|---|---|---|---|
| Day 0–3 | Tightness, fatigue, swelling; walking slightly bent is common | Short, frequent walks; hydration; medications as prescribed; start compression as directed | Heavy lifting, twisting, long periods in bed without walking |
| Week 1 | Swelling and bruising; soreness at incision; “pulling” sensation with movement | Prioritize rest + gentle mobility; keep incision clean/dry; attend scheduled check-ups | Lifting children, intense chores, driving if on narcotics |
| Week 2 | Improving comfort; still swollen; energy is variable | Increase walking; continue compression; begin scar-care only if approved | Gym workouts; core exercises; lifting beyond restrictions |
| Weeks 3–6 | More upright posture; swelling persists but gradually improves | Return to light work; gentle daily activity; follow garment guidance | Heavy lifting, aggressive stretching, high-impact exercise |
| Weeks 6–12 | Noticeable refinement; scar begins to mature; tightness eases | Progress activity gradually; resume exercise only as cleared | Rushing to “full workouts” too early |
Week 1–2: Posture, Showering, and “Drain vs Drainless” Realities
This is the phase where people with drains are actively managing a tummy tuck drain—emptying it, measuring output, and protecting the tubing. That’s why searches like drain tube after tummy tuck and drain tube removal after tummy tuck spike around this time. With a drainless approach, you typically avoid those tasks, but you still need structured follow-ups to ensure fluid isn’t accumulating quietly. Compression and routine check-ins are not optional, even in drain free tummy tuck recovery.
- If drains are used: ask how to care for the tubing, how output is measured, and when drain tube removal after tummy tuck is typically considered.
- If drainless: ask how the clinic checks for early seroma and what symptoms should prompt a same-day assessment.
“Lifting children” sounds like one constraint. It’s actually a chain of small constraints stacked across the day. Bath time, school drop-off, getting in and out of the car with a toddler, the unplanned moment when a child runs at you for a hug—each one needs an actual plan, not a generic “avoid lifting” rule. Drainless reduces the equipment-management layer; it doesn’t reduce the child-care layer.
The day-by-day household logistics—who does what, how partner/family support windows are sequenced, and what the actual practical plan looks like across the recovery weeks—are mapped in our recovery-with-children playbook.
Red Flags & When to Contact the Surgeon (Fever, Fluid, Asymmetric Swelling)
Whether you had a drain tube tummy tuck setup or a drainless technique, you should contact your surgical team urgently if you notice:
- Fever, chills, or increasing redness/warmth around the incision
- Sudden increase in swelling, especially if one-sided (possible fluid collection)
- Persistent fluid-like “sloshing” sensation (could suggest seroma)
- Worsening pain rather than gradual improvement
- Shortness of breath, chest pain, or calf pain/swelling (emergency evaluation needed)
Safety-first mindset: A drainless technique is not a reason to reduce follow-up. In fact, good outcomes depend on early detection and management of swelling or fluid—an approach aligned with responsible medical science.
“Drain Questions” Patients Ask Most (and How to Translate Them)
Even if your plan is drainless, it’s helpful to understand common drain-related questions so you can interpret what you read online:
- “tummy tuck drain” = the external device used to evacuate fluid in traditional recovery.
- “drain tube after tummy tuck” / “drainage tube after tummy tuck” = the tubing exiting the skin connected to a bulb or reservoir.
- “drain tube removal after tummy tuck” = the clinic visit where drains are removed once output drops.
- “drain tube scar” = the small mark where the drain exited.
- “no drain tummy tuck” / “drain free tummy tuck” = methods designed to avoid external drains by managing internal space and fixation.
Recovery Support Technologies: What They’re Intended to Improve
Some clinics support recovery with technologies aimed at swelling control and tissue healing. When evaluating these, look for clarity and restraint: what is the intended benefit, what is realistic, and what is not guaranteed? In an evidence-driven practice, these tools complement—not replace—sound surgical technique, compression, mobility, and structured follow-up.
Explore the Full Tummy Tuck Journey
Drainless is one decision in a longer chain. Recovery framework, package logistics, surgeon-led pre-op clearance, and the international-patient continuity plan are the rest. Most patients who research drainless techniques alone end up booking with incomplete planning—then discover the gaps once they’re already in Istanbul. Reversing that order produces fewer surprises.
The full pre-op preparation, day-by-day recovery, all-inclusive Istanbul packages, and aftercare logistics for international patients are mapped in our complete abdominoplasty guide.
Drainless versus drain-based isn’t typically a pricing variable—but the surgery scope around it is. Mini versus full, with or without muscle repair, lipo addition, mommy-makeover combination—each scope decision moves the cost line. The “drainless premium” you might worry about is mostly a myth; the scope premium is the real driver, and it deserves transparent breakdown rather than a single bundled number.
The procedure-by-procedure pricing breakdown—including what’s bundled, what’s add-on, and how scope decisions actually move the total—is in our tummy tuck pricing transparency.
Frequently Asked Questions (FAQ): Tube Tummy Tuck
This FAQ is designed for the “expert patient” who wants clear, safety-first answers—especially around drains, fluid management, and what “drainless” truly means in practice. These answers use patient language (including common search terms like tummy tuck drain and drain tube after tummy tuck) while staying grounded in responsible medical science.
Is Tube Tummy Tuck truly “drainless,” and can a drain ever be needed?
In most cases, “tube tummy tuck” is used to describe a no drain tummy tuck strategy—meaning the surgeon plans to avoid external drains by reducing internal dead space and stabilizing tissues. However, in higher-risk or complex cases, a surgeon may still decide a temporary tummy tuck drain is safer. The best question is: “In what situations would you switch from drainless to drains, and why?”
What’s the difference between Tube Tummy Tuck and progressive tension sutures?
Many “drainless” techniques rely on internal fixation—often referred to as progressive tension sutures—to reduce the space where fluid collects. So in practical terms, a drain free tummy tuck is frequently built on that concept. Because “tube tummy tuck” isn’t always a standardized medical term, ask your surgeon which internal fixation method they use and how it affects seroma risk.
What are the most common risks (seroma, infection, delayed healing) and how are they handled?
Common risks include seroma (fluid collection), infection, delayed wound healing, and scar concerns. A quality plan includes scheduled follow-ups, compression guidance, and clear steps if fluid occurs (often evaluation and possible aspiration). The presence or absence of a drainage tube after tummy tuck changes logistics, not the need for monitoring.
Who is NOT a good candidate for a drainless approach?
Patients with significant risk factors—such as active smoking, uncontrolled diabetes, very high BMI, extensive revision surgery, or complex tissue conditions—may not be ideal candidates for a strict no drain tummy tuck approach. In some cases, the surgeon may recommend a traditional plan using a drain tube after tummy tuck to reduce complication risk.
What happens if fluid builds up anyway—what is the management plan?
Even with no drain tummy tuck techniques, fluid can occur. A responsible plan includes early assessment and, when appropriate, aspiration in clinic, continued compression, and close follow-up. This is why you should ask for a written or clearly explained protocol—because real safety is a process, not a marketing phrase.
Final takeaway: A tube tummy tuck approach can simplify the early recovery experience by avoiding external drains for many patients. But the best results come from surgeon technique, careful candidate selection, and structured follow-up—principles grounded in medical science and patient safety.
Medical Disclaimer: This page is provided for general educational purposes only and does not replace a face-to-face medical consultation, diagnosis, or personalised treatment plan. All surgery carries risks and outcomes vary between individuals. Suitability for a tube tummy tuck, procedure selection, and anaesthesia choice can only be determined after a full clinical assessment by a qualified surgeon. Always follow your clinician’s instructions and seek urgent medical attention if you develop concerning symptoms during recovery.
Related Treatments
Ready to Start Your Own Transformation Journey?
Join the 2,000+ patients who trusted Dr. Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, revitalized you begins with a simple, no-obligation conversation. Contact us today from the USA for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. No hidden fees.
#2: Secure Your Date & VIP Booking
Once you're ready, our dedicated patient coordinators will help you secure your procedure date. We'll handle all your bookings, including your 5-star hotel and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you'll meet your specialist surgeon to finalise the details for your "natural, subtle, and revitalized" new look.













