The Experience of Aftercare After Surgery Abroad in the UK

- Aftercare After Surgery Abroad: UK-ready handover plan with documents, timelines, and clear escalation routes.
- Post-operative support from home via scheduled digital check-ins, photo reviews, and UK-accessible WhatsApp support.
- Know the red flags: fever, worsening redness, chest symptoms—when to contact your team or go to A&E.
- Flight-ready recovery support with HBOT and LLLT to reduce oedema, support scars, and shorten downtime.
AI-generated summary, fact-checked by our medical experts.
If you’re a British patient considering treatment overseas, the most important question isn’t always “How is the surgery?” — it’s aftercare after surgery abroad: what happens when you’re back in the UK, the swelling (oedema) has peaked, and you want a clinician-led plan rather than guesswork.
This article is written for the UK “expert patient” — someone who reads details, checks credentials, and wants a clear UK aftercare plan for surgery abroad before booking anything. We’ll cover what good post-operative aftercare UK should look like, what “normal” healing can feel like (and what isn’t normal), and how postoperative care after flying home can be structured so you’re not left feeling unsupported.
Importantly, this is not a replacement for medical advice. If you develop urgent symptoms (for example, chest pain or breathing difficulty), you should seek immediate help via A&E. However, when you’re not in an emergency, the goal is clarity — a programme built on communication, documentation, and evidence-informed practice from modern medical science and clinical standards.
Table of Contents

Why Aftercare Is the Real “Safety Test” After Surgery Abroad (From a UK Perspective)
Many UK patients can organise the flight and hotel. The real risk is the “handover” back to home life: you’re recovering, you may not want to burden your GP, and you’re unsure what the NHS can realistically provide for a privately chosen procedure overseas. That’s why aftercare after cosmetic surgery abroad is the true safety test — not the operating theatre day itself.
For many people, this feels even more acute when you’re flying to Turkey for facelift surgery: the procedure may be finished in a matter of hours, but your recovery unfolds over weeks back in the UK. A reliable aftercare pathway should spell out exactly who you contact, what photos or measurements to share, and how quickly you’ll get clinician-led guidance if something doesn’t look or feel right. In short, peace of mind comes from structure, not hope.
What UK patients fear most: “Who helps me once I’m home?”
British patients often worry about being left with unanswered questions once they return: “Is this bruising normal?”, “Should my incision look like this?”, “Do I need a dressing change?”, “Is my temperature too high?” The anxiety is understandable — your body is doing a lot of healing in the first 7–14 days, and uncertainty can make normal recovery feel alarming.
“Knowing I could message a UK number and still reach the medical team gave me real peace of mind once I was home.”
— Mehtap, UK patient
Continuity of care: why it matters more than the flight and hotel
Continuity means the people guiding your recovery understand exactly what was done, what devices were used (for example, compression garments or drains), and what your expected milestones are. Without a continuity plan, you may find yourself repeating your story to different providers — or worse, delaying help because you’re unsure who to contact. A strong UK aftercare plan for surgery abroad reduces this friction by making follow-up structured, predictable, and clinically useful.
The difference between normal healing and complications (in plain British terms)
After surgery, discomfort, bruising, tightness, and oedema can be normal — but “normal” should follow a pattern. Complications often worsen rather than gradually improve. The safest approach is to track symptoms and have clear escalation steps as part of your aftercare experience after medical travel.
| Common recovery experiences (often expected) | Red flags (contact your team urgently / consider A&E) |
|---|---|
| Bruising that slowly fades over days | Rapidly spreading redness, worsening heat, or foul-smelling discharge |
| Oedema that peaks then gradually reduces | Sudden one-sided leg swelling or calf pain (DVT concern) |
| Mild temperature changes | Fever of 38°C (100.4°F) or higher, especially with chills and worsening pain |
| Achiness managed with prescribed medication (often including paracetamol) | Severe pain that escalates despite medication or is accompanied by faintness |
| Low energy and sleep disruption early on | Shortness of breath, chest pain, or coughing blood (seek emergency care) |
What “Good Aftercare” Looks Like (A Practical, UK-Friendly Definition)
“Good aftercare” is not a vague promise of being “available 24/7”. It is a documented, clinician-led programme that tells you what will happen, when it will happen, and what to do if recovery deviates from the expected course. For UK patients, good postoperative care after international surgery also includes a plan for communication while you’re at home — so you’re not relying on guesswork or social media advice.
Clear timelines: day-by-day milestones vs vague reassurance
A reliable aftercare programme for cosmetic surgery abroad gives you a timeline in plain language. For example: what you should expect in the first 72 hours, what changes are typical in week one, and when swelling should start settling. This matters because a timeline turns anxiety into observation: you can compare your experience to realistic milestones rather than catastrophising.
Written instructions you can follow at home (medication, dressings, hygiene)
Aftercare should include written guidance that fits real UK home life: how to clean incisions, how to manage dressings and plasters, how much fluid to aim for (litres rather than ounces), and what activity level is appropriate. It should also clarify medication protocols and safety — including when to use paracetamol, how to take prescribed medication, and what interactions to avoid.
Escalation pathways: who to contact, when, and what information to share
The most reassuring part of a robust post-operative aftercare UK pathway is knowing exactly what happens if you’re worried. You should know:
- Who you message or call (ideally a UK-accessible contact route)
- When to escalate (for example, increasing pain, new redness, fever, unusual discharge)
- What to send (clear photos in good lighting, your temperature in °C, a brief symptom timeline, and your medication list)
| What to prepare before you fly home | Why it improves your UK aftercare experience |
|---|---|
| Procedure summary and operative notes | Makes it easier for any UK clinician to understand what was done |
| Medication list (names, doses, timing) | Reduces errors and helps safe prescribing decisions |
| Clear follow-up schedule (check-ins) | Creates structure for postoperative care after flying home |
| Escalation checklist (red flags + contact route) | Prevents delays if recovery deviates from expected milestones |
We utilise advanced Hyperbaric Oxygen Therapy (HBOT) to minimise downtime and enhance your healing process. Safety is our primary commitment.
The Reality of Aftercare in the UK After Surgery Abroad
Once you’re back home, the practical question becomes: who can help with post-operative aftercare UK needs such as dressing checks, reassurance about bruising, or advice on unexpected symptoms? The answer is rarely simple. That’s why aftercare after surgery abroad UK must be planned as carefully as the surgery itself — ideally with a written pathway and the right documents so you’re not starting from scratch if you need support.
For patients flying to Turkey for facelift surgery, this UK “handover” is where reassurance can quickly turn into uncertainty if there isn’t a clear plan. Even straightforward needs—such as a dressing query, a question about bruising patterns, or whether oedema is settling as expected—can feel stressful when you’re unsure who is best placed to advise. That’s why it helps to have a written aftercare pathway, key documents ready, and an agreed communication route before you travel, not after you return.
GP vs private clinics vs A&E: what each can and cannot do
In the UK, your GP is often your first point of contact for health concerns, but GPs may have limited capacity to provide routine post-op reviews for elective cosmetic surgery performed abroad. Some patients choose a private nurse/clinic for wound checks or dressing changes, especially in the first 1–2 weeks. A&E is appropriate for urgent symptoms (for example, chest pain, shortness of breath, sudden leg swelling, or heavy bleeding) — but it is not designed for reassurance-only check-ups.
| UK option | Most helpful for | Limitations to expect |
|---|---|---|
| GP / local NHS services | General health queries, signposting, medication advice | May not provide routine aftercare for elective overseas cosmetic surgery |
| Private wound care / nurse visit | Dressing changes, basic wound observation, compression garment checks | Cost varies; they may still need operative notes to advise confidently |
| A&E | Emergency symptoms (DVT/PE concern, severe infection signs, breathing issues) | Not a planned follow-up service; waiting times and triage priorities apply |
Common friction points (documentation, prescriptions, dressing changes)
Most aftercare stress isn’t “medical drama” — it’s admin friction. Patients can struggle with: (1) not having a concise procedure summary, (2) uncertainty about what is normal oedema vs something concerning, (3) confusion over dressings/plasters and showering rules, and (4) questions about medicines once they are home (including what is safe alongside paracetamol).
This is exactly why a structured aftercare experience after medical travel matters: it anticipates the practicalities and removes ambiguity before you board the plane.
What to prepare so UK clinicians can help you safely (summary letter, operative notes)
If you want UK-based support to be straightforward, you need to make it easy for any clinician to understand what was done. A “helpful pack” typically includes:
- Procedure summary (what surgery, when, key steps)
- Operative notes (important for context if anything deviates from the expected course)
- Medication list (names, doses, timing)
- Aftercare timeline (what to expect day 1–3, week 1, weeks 2–6)
- Red-flag checklist (when to contact the surgical team vs when to go to A&E)
Think of this as your “handover file” for postoperative care after international surgery. It reduces delays and helps UK clinicians give safer, faster guidance.
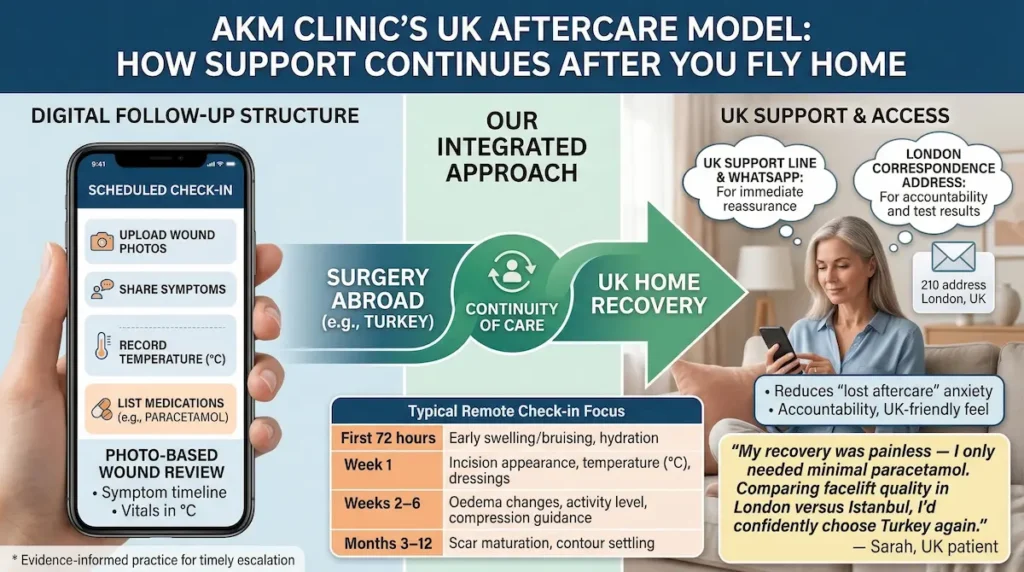
AKM Clinic’s Aftercare Model for British Patients (How Support Continues After You Fly Home)
A reliable UK aftercare plan for surgery abroad is built around continuity: the same team that understands your operating theatre details supports your recovery milestones once you’re back in the UK. In practical terms, that means scheduled check-ins, clear escalation rules, and a communication route that does not feel “overseas” when you need quick reassurance.
Digital follow-up structure: scheduled check-ins and photo-based wound review
Most recovery questions can be answered safely when your surgical team has the right information: good lighting photos, a short symptom timeline, your temperature in °C (and yes, 38°C (100.4°F) is a common threshold used in post-op guidance), and a list of what you’ve taken that day.
From the standpoint of medical science, structured monitoring improves decision-making because it turns vague worry into trackable observations. While every patient is different, evidence-informed practice and scientific research across peri-operative care consistently supports the value of early identification and timely escalation when recovery deviates from the expected pattern.
| Typical remote check-in focus | What you share | What the team assesses |
|---|---|---|
| First 72 hours | Photos, pain pattern, mobility, fluid intake (litres) | Early swelling/bruising pattern, hydration, comfort and safety |
| Week 1 | Incision photos, dressing questions, temperature (°C) | Wound appearance, infection risk signals, dressing plan |
| Weeks 2–6 | Oedema changes, scar care adherence, activity level | Expected progression, scar quality support, compression guidance |
| Months 3–12 | Longer-term healing photos and concerns | Scar maturation, contour settling, realistic outcome review |
UK support line & WhatsApp continuity (reducing “lost aftercare” anxiety)
One of the most common frustrations after medical travel is feeling you can’t reach anyone quickly once you’re home. A UK-accessible route (for example, a direct WhatsApp channel and a UK support line) removes that psychological barrier and makes postoperative care after flying home feel continuous rather than fragmented.
“My recovery was painless — I only needed minimal paracetamol. Comparing facelift quality in London versus Istanbul, I’d confidently choose Turkey again.”
— Sarah, UK patient
For Skeptical Sam, this is not a “nice extra”; it’s a safety feature. When you know exactly how to reach the medical team, you are less likely to delay asking a question that genuinely matters.
London correspondence address / UK contact point: why it changes trust and logistics
For many British patients, a UK-facing contact point (including a London correspondence address for patient documents) reduces uncertainty. It can help with practicalities — such as sending test results or paperwork — and it supports a feeling of accountability that UK patients often associate with Care Quality Commission-style expectations.
In other words: a well-designed aftercare programme for cosmetic surgery abroad should feel “UK-friendly” even when the procedure itself happened overseas.
From VIP airport transfers to 5-star hotel accommodation, we manage every detail. Enjoy a premier medical travel experience in Istanbul.
Planning Aftercare Before You Book (A Pre-Flight Checklist for Skeptical Sam)
If you want the strongest safety net, plan your aftercare before you commit. This is where the phrase aftercare after cosmetic surgery abroad stops being marketing and becomes a practical checklist. The goal is to know, in advance, what happens on day 1, day 7, week 6, and month 6 — and who is responsible at each step.
Questions to ask before surgery: dressings, drains, scar care, follow-ups
- Who changes dressings/plasters, and how often?
- Will I have drains? If yes, when are they removed and what should I watch for?
- What is the scar-care plan (and when does it start)?
- How often are remote check-ins scheduled once I return to the UK?
- What are the clear “red flags” that require urgent escalation?
What to pack for week 1–2 at home (practical and UK-relevant)
For smoother post-operative aftercare UK, pack items that make monitoring and hygiene easier at home:
- A digital thermometer (record readings in °C)
- Basic dressing supplies (as advised), gentle cleanser, and clean gauze
- Compression garment(s) as prescribed
- A note template for daily tracking (pain, mobility, fluid intake in litres)
- Comfortable, loose trousers
How to set up your “UK aftercare plan” at home (so you don’t panic)
Before you fly, create a simple home plan that supports postoperative care after flying home:
- Book 1–2 weeks of reduced commitments (work, childcare, heavy lifting).
- Arrange a trusted friend or family member to check in (especially days 1–5).
- Keep your aftercare documents in one place (digital + printed).
- Know your escalation rule: message the team early for concerns; go to A&E immediately for emergency symptoms.
Red Flags You Should Never Ignore Once You’re Back in the UK
After any procedure, most recovery changes are predictable — but a small number of symptoms should always be treated as time-sensitive. A safe UK aftercare plan for surgery abroad makes it crystal clear what counts as a red flag, what to do first, and when to skip messaging and go straight to A&E. This is the practical side of aftercare after surgery abroad UK: less panic, more decision-making.
For anyone flying to Turkey for facelift surgery, it’s especially important to know that red flags are about patterns, not perfection. A single odd sensation can be harmless, but symptoms that escalate—worsening pain, spreading redness, increasing swelling on one side, or feeling suddenly unwell—should prompt action rather than reassurance-seeking. The safest approach is to monitor consistently (photos, temperature in °C, symptom timeline) and follow your escalation pathway early, so small issues are addressed before they become bigger problems.
Fever, worsening redness, unusual discharge: what “urgent” looks like
A rising temperature, escalating redness, increasing warmth around the incision, or discharge that looks or smells unusual can indicate infection or irritation that needs timely assessment. Don’t “wait it out” if symptoms are worsening day by day — use your post-operative aftercare UK escalation route early (photos + temperature + symptom timeline).
Breathing/chest pain/leg swelling: DVT and emergency symptoms (when to go straight to A&E)
Some symptoms are emergencies, regardless of where you had surgery. If you develop chest pain, shortness of breath, fainting, coughing blood, or sudden one-sided leg swelling/calf pain, seek urgent assessment via A&E. This is not the moment for reassurance texts — it’s rapid medical evaluation.
Pain that is “not normal”: how to document symptoms for rapid triage
Most post-op discomfort follows a trend: it gradually improves, even if there are “up and down” days. Pain that suddenly escalates, becomes sharp, or is paired with new swelling, redness, fever, or dizziness is a reason to escalate. Documenting symptoms makes your team’s advice safer and faster:
- Timing: when it started and whether it’s worsening
- Location: exact area (and whether it spreads)
- Associated symptoms: temperature (in °C), nausea, dizziness, discharge, shortness of breath
- Medication log: what you took and when (including paracetamol)
- Photos: clear images in good lighting (same angle each day if possible)
| Symptom | What to do first | When to treat as emergency |
|---|---|---|
| Temperature at or above 38°C (100.4°F) | Message your surgical team with temperature readings, photos, and symptoms | If you also feel faint, confused, or severely unwell |
| Worsening redness / heat / increasing tenderness | Send photos + symptom timeline via your aftercare route | If rapidly spreading with fever or severe pain |
| Unusual discharge (especially foul-smelling) from incision | Contact your team promptly with photos | If heavy bleeding or you feel acutely unwell |
| Sudden one-sided leg swelling or calf pain | Do not delay: seek urgent assessment | Go straight to A&E |
| Chest pain, breathlessness, coughing blood | Call emergency services / attend A&E immediately | Always an emergency |
“The lifeline for me was the support after returning home — I used the direct UK WhatsApp number and the UK support line to stay in constant contact.”
— Mehtap, UK patient

Recovery Support That Helps You Get “Flight-Ready” (And Back to Normal Life Sooner)
Good recovery isn’t just about “resting” — it’s about reducing avoidable setbacks and supporting healing with a structured plan. For many patients, the aim of a well-designed aftercare programme for cosmetic surgery abroad is to reduce oedema, support scar quality, and help you feel confident returning to normal routines in the UK. This is where practical habits and targeted therapies can complement your standard care, in line with modern medical science.
For patients flying to Turkey for facelift surgery, “flight-ready” recovery is less about rushing and more about planning the right supports at the right time. Simple, evidence-informed steps—consistent compression (where advised), steady hydration in litres, gentle mobilisation, and disciplined scar care—often make the biggest difference to comfort and confidence once you’re back in the UK. Targeted therapies can then sit on top of those fundamentals, helping you progress through the early recovery window with fewer avoidable setbacks.
What slows healing: smoking, dehydration, poor compression, early activity
Most delays in postoperative care after flying home come from a handful of predictable issues:
- Dehydration: aim for steady fluids (commonly 2–3 litres daily unless your clinician advises otherwise)
- Smoking/vaping: reduces oxygen delivery and can worsen healing quality
- Poor compression adherence: can increase swelling and prolong discomfort
- Doing too much too soon: “feeling better” isn’t the same as being healed
- Inconsistent sleep and nutrition: common, but worth improving where possible
None of this is about perfection — it’s about giving your body the best conditions to do what it already knows how to do.
Faster recovery protocols: how HBOT can reduce bruising/oedema and support healing
At AKM Clinic, Hyperbaric Oxygen Therapy (HBOT) is used as a recovery strategy with the goal of reducing post-operative swelling (oedema), supporting lymphatic drainage, and shortening visible “social downtime”. HBOT is commonly described using pressure units such as ATA (a scientific way of expressing “pressure/depth”), which clinicians translate into patient-friendly language.
For UK patients, the value is practical: if your postoperative care after international surgery includes a recovery protocol designed to settle swelling earlier, you may feel more confident returning to work, social plans, and day-to-day responsibilities.
| Recovery focus | What UK patients usually notice | Why it matters after flying home |
|---|---|---|
| Reducing oedema | Less “tightness” and earlier comfort with movement | Supports confidence during the early UK recovery window |
| Reducing bruising visibility | Earlier return to normal social appearance | Shortens the period of feeling “stuck at home” |
| Structured monitoring | Clear check-ins and escalation rules | Improves your overall aftercare experience after medical travel |
Scar optimisation: how LLLT supports incision healing and scar quality
Scars are one of the most common concerns for British patients considering surgery abroad. Alongside good incision care, AKM Clinic uses Low-Level Laser Therapy (LLLT) as a scar-healing support. LLLT can be delivered via a soft laser (often described by its wavelength) with the goal of supporting skin quality and minimising visible scar lines during healing.
In plain terms: scar optimisation is a programme, not a product. It typically includes timing (when to start), consistency, sun protection, and realistic expectations about scar maturation over months.
“My recovery was painless, requiring minimal paracetamol. Comparing facelift quality in London versus Istanbul, I’d confidently choose Turkey over the UK.”
— Sarah, UK patient
Finally, recovery support only works when the fundamentals are in place: a safe operating theatre environment, clear written aftercare instructions, and a UK-friendly communication route (for example, a direct UK WhatsApp number and a support line) so your aftercare after cosmetic surgery abroad does not feel fragmented once you’re home.
Frequently Asked Questions (FAQ): Aftercare After Surgery Abroad
Below are the most common questions UK patients ask when planning aftercare after surgery abroad UK. The aim is to make post-operative aftercare UK feel practical, predictable, and clinically sensible — especially once you’ve flown home and real recovery begins.
Can my GP in the UK provide aftercare after cosmetic surgery abroad?
Your GP can help with general health advice, medication guidance, and signposting, but routine cosmetic aftercare (for example, planned wound checks or dressing changes for elective surgery performed overseas) may be limited. That’s why it’s best to arrange a clear UK aftercare plan for surgery abroad in advance, including who you contact for non-urgent concerns and what you do if something changes unexpectedly.
What documents should I bring back to the UK to make aftercare easier?
Bring a short procedure summary, operative notes (or a clinician summary letter), a medication list (names, doses, timings), and a written recovery timeline. These documents make postoperative care after international surgery safer and smoother because they help any UK clinician understand exactly what was done, what “normal” healing should look like, and what would be unusual.
When should I go to A&E instead of contacting my surgical team?
Go straight to A&E for emergency symptoms such as chest pain, shortness of breath, fainting, coughing blood, sudden one-sided leg swelling/calf pain, heavy bleeding, or feeling severely unwell. For non-emergency concerns (for example, questions about bruising patterns, mild temperature changes, or dressing guidance), contacting your aftercare route first is usually appropriate. A strong aftercare programme for cosmetic surgery abroad makes this decision clear, so you don’t waste time when minutes matter.
How long does swelling (oedema) usually last, and when should I worry?
Oedema is expected after many procedures and often peaks early before gradually settling, but timelines vary by operation, your individual biology, and how closely you follow compression and activity guidance. You should worry if swelling is rapidly worsening, becoming sharply painful, is paired with fever (for example, 38°C or higher), or comes with new redness/heat or unusual discharge. In postoperative care after flying home, tracking symptoms daily (photos, temperature in °C, pain pattern) makes it easier to spot changes that need timely advice.
Will I be able to get prescriptions in the UK after returning?
Some medicines may be managed in the UK, but prescribing decisions depend on clinical judgement, your medical history, and what documentation you have. For pain relief, many patients use paracetamol as advised, but you should follow your clinician’s instructions carefully and avoid self-medicating with multiple products that may overlap. Clear paperwork and a medication list are key parts of a safe aftercare after cosmetic surgery abroad plan.
What does remote follow-up actually involve (photos, calls, check-in schedule)?
Remote follow-up typically includes scheduled check-ins (especially in the first 1–2 weeks), photo-based wound reviews in good lighting, and short symptom updates (pain, mobility, temperature in °C, fluid intake in litres). This structure is designed to reduce uncertainty and improve decision-making — turning your aftercare experience after medical travel into a clear pathway rather than a series of anxious “Is this normal?” moments.
If I need a revision or an in-person review, what are my options as a UK patient?
Options depend on your situation. Some concerns can be managed remotely with a refined aftercare plan; others may require an in-person review (either with your original surgical team or a UK-based clinician). The safest approach is to plan for this possibility before booking surgery: ask what the revision policy is, what the escalation pathway looks like, and what support exists once you’re home. For Skeptical Sam, the most reassuring setup is one where the clinic’s aftercare after surgery abroad UK pathway includes clear next steps if recovery deviates from expectations.
If you’d like to explore related topics beyond aftercare, you can also read our Surgery Abroad Safety Checklist, guidance on choosing a Plastic Surgeon Turkey, and a practical Pre-Surgery Checklist to prepare for your trip. Travelling on your own? Our Travelling Solo for Surgery guide explains what support to expect at each step. We also address common concerns in Turkish Plastic Surgery Myths, and you can see what recovery can look like day-by-day in the Deep Plane Facelift Journey. For a real patient perspective, the Deep Plane Facelift Story shares a UK experience from consultation to long-term results.
Medical Disclaimer: This page is provided for general educational purposes only and does not replace a face-to-face medical consultation, diagnosis, or personalised treatment plan. All surgery carries risks and outcomes vary between individuals. Suitability for a plastic surgery, procedure selection, and anaesthesia choice can only be determined after a full clinical assessment by a qualified surgeon. Always follow your clinician’s instructions and seek urgent medical attention if you develop concerning symptoms during recovery.
Related Treatments
Ready to Begin Your Own Transformation Journey?
Join the 2,000+ patients who have trusted Dr Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, naturally restored you begins with a simple, no-obligation conversation. Contact us today from the UK for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. There are no hidden fees.
#2: Secure Your Date & VIP Booking
Once you are ready, our dedicated patient coordinators will help you secure your procedure date. We will handle all your bookings, including your 5-star hotel accommodation and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you will meet your specialist surgeon to finalise the details for your "natural, subtle, and restored" new look.


















