Awake Breast Lift in Turkey




- Awake breast lift under local anaesthesia with optional twilight sedation supports comfort and faster early recovery.
- Technique-led mastopexy planning addresses ptosis grades, parenchymal maldistribution, and options: lift alone, implants, or fat transfer.
- Safety-first monitoring and transparency covers risks, necrosis warning signs, and structured aftercare before and after returning to the UK.
- Premium value versus UK private clinics combines specialist standards with HBOT and LLLT to optimise healing and scars.
AI-generated summary, fact-checked by our medical experts.
Awake Breast Lift: Quick Facts
Duration of Surgery
Type of Anaesthesia
Initial Recovery Period
Hospital Accommodation
Return to Daily Activities
Awake Breast Lift Results: Before and After
An awake breast lift (mastopexy) is designed for women who want a refined uplift with a modern anaesthetic approach: local anaesthesia, often supported by twilight sedation, rather than a fully “asleep” general anaesthetic. This page is written for UK patients who prioritise surgical innovation, safety, and a well-structured recovery plan—and who want clinical clarity on how an awake technique differs from a standard breast lift pathway.
Table of Contents
Share your photos and medical history to receive a personalised assessment from our European Board-certified facial surgery team.
What is an Awake Breast Lift?
An awake breast lift is a form of mastopexy performed with the breast tissues fully numbed using local anaesthesia. Depending on your comfort level and the complexity of the plan, this may be paired with twilight sedation (a light, carefully monitored sedative state). The goal is the same as any high-quality lift: a more youthful breast position, improved nipple–areola placement, and a firmer, better-balanced breast shape—without relying on “being fully asleep” as the default.
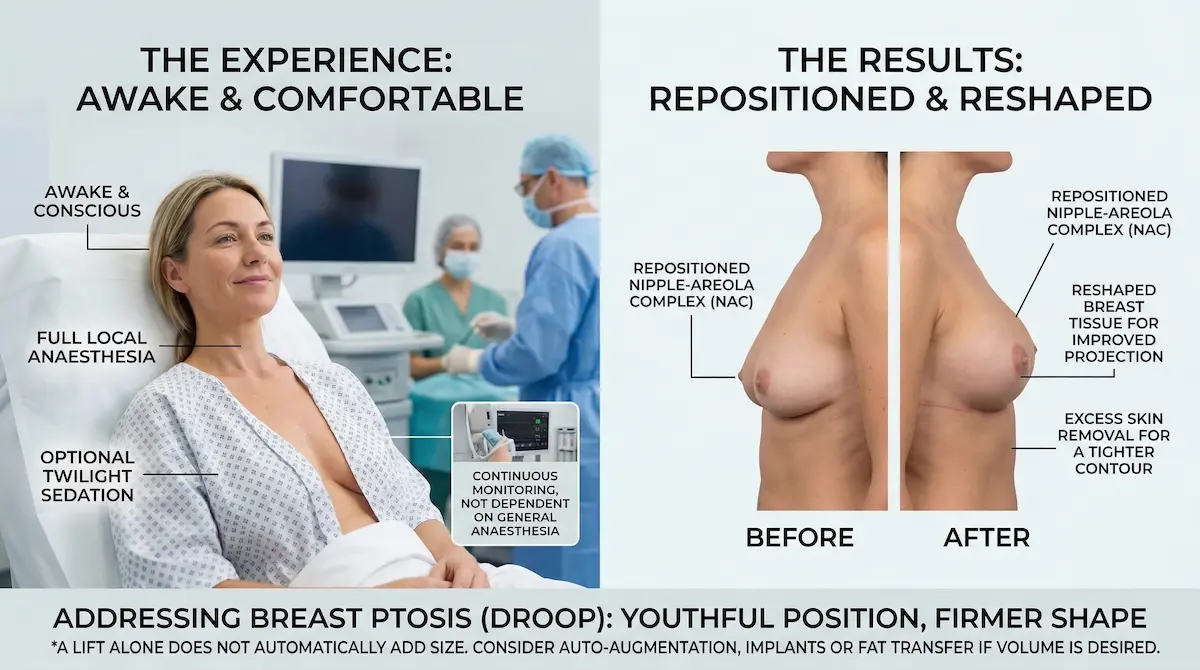
Mastopexy basics: what changes and what doesn’t
If you’ve ever searched “How is breast lift (mastopexy) surgery done?” the simplest answer is: a lift repositions and reshapes, it doesn’t automatically “add size”. In most cases, mastopexy involves:
- Repositioning the nipple–areola complex (NAC) to a higher, more proportionate point on the breast mound
- Reshaping breast tissue to improve projection and reduce long-term “bottoming out”
- Removing excess skin to tighten the skin envelope and refine the contour
A lift alone typically won’t create upper-pole fullness like an implant can. That’s why some patients explore options such as auto-augmentation breast lift (using your own tissue) or combining a lift with implants or fat transfer (covered later in this guide).
Breast ptosis and nipple–areola position (simple anatomy)
“Ptosis” is the clinical term for droop. It’s not just about where the nipple sits—it’s about the relationship between the nipple, the breast crease (inframammary fold), and how the breast tissue is distributed. Many patients also have a degree of parenchymal maldistribution in mastopexy, meaning the breast volume has migrated lower over time (often after pregnancy, breastfeeding, weight changes, or natural ageing).
Understanding your ptosis pattern matters because it influences:
- Which incision strategy is likely to be safest and most stable
- How much internal reshaping is needed (not just skin tightening)
- Whether a lift alone can meet your goals, or if an augmentation element is required
In practice, your surgical plan is built around your anatomy—your skin quality, tissue strength, and the degree of lift required.
What “awake” means: local anaesthesia and/or twilight sedation
“Awake” does not mean “no pain relief” or “white-knuckle surgery”. It means the operative area is numbed with local anaesthesia, and you may also receive twilight sedation to reduce anxiety and improve comfort. You remain under continuous monitoring, and the anaesthetic strategy is tailored to the procedure plan and your medical profile.
For many patients, an awake approach is appealing because it reframes the experience: you’re not relying on a full general anaesthetic as the only route to a high-standard awake mastopexy. That said, suitability is individual—and an awake pathway should be chosen for the right reasons, with the right clinical safeguards.
Our surgical dates fill up quickly due to high international demand. Secure your consultation today to arrange your preferred travel dates.
Why choose an awake approach for mastopexy
For the “expert patient”, the awake pathway is often about risk management and recovery quality, not “cutting corners”. The central idea is to reduce unnecessary physiological load while maintaining meticulous surgical standards—particularly when local anaesthesia and twilight sedation are appropriate for the case.
Awake breast lift vs general anaesthesia risks
General anaesthesia is widely used and can be very safe when correctly indicated. However, it does involve systemic effects and airway management that some patients wish to avoid when a suitable alternative exists. With an awake breast lift, the anaesthetic focus shifts toward:
- Targeted local numbing of the surgical area
- Optional light sedation rather than deep unconsciousness
- A recovery that may involve less nausea, grogginess, and “anaesthetic hangover” for certain patients
It’s also important to be balanced: local anaesthesia and sedation still require expertise, careful dosing, and monitoring. The key is not “awake is always better”, but awake is a modern option for the right patient and the right plan.
Less “anaesthetic hangover”, earlier mobilisation
One reason UK patients investigate awake mastopexy is the potential for a smoother early recovery phase. Many patients find they can:
- Mobilise sooner and feel more “clear-headed” in the hours after surgery
- Resume light activities earlier (within sensible surgical limits)
- Follow a structured aftercare plan without the lingering effects some associate with general anaesthesia
This doesn’t mean recovery is “instant”—a breast lift is still a significant procedure. Swelling, tightness, and activity restrictions are normal. But for appropriately selected cases, the anaesthetic approach can support a calmer first 24–72 hours.
Who usually benefits most from awake / twilight protocols
An awake breast lift may be particularly relevant if you:
- Prefer to avoid general anaesthesia where clinically appropriate
- Have had significant nausea or prolonged grogginess after general anaesthesia in the past
- Value an approach designed around controlled recovery and close monitoring
- Want a consultation that discusses technique, anatomy, and risk reduction in depth (not just “before-and-after” marketing)
Conversely, some patients are better served by general anaesthesia—such as those with very high anxiety, those requiring extensive reshaping, or when multiple procedures are planned together. The right approach is the one that fits your surgical plan, your safety profile, and your comfort needs.
Next step (UK patients): Review Your Surgical Plan with a European Board-Certified Specialist.
Understanding breast ptosis and parenchymal maldistribution
If you are researching mastopexy properly, you’ll notice that “droop” is rarely a single issue. It can be a mix of nipple position, skin laxity, and how the breast tissue has shifted over time. This matters because a lift that only tightens skin can look good early on, then lose definition. Our planning focuses on structural balance, so the result stays natural and stable.
In other words: we treat the shape, not just the surface. That is often what separates a generic uplift from a refined surgical plan.
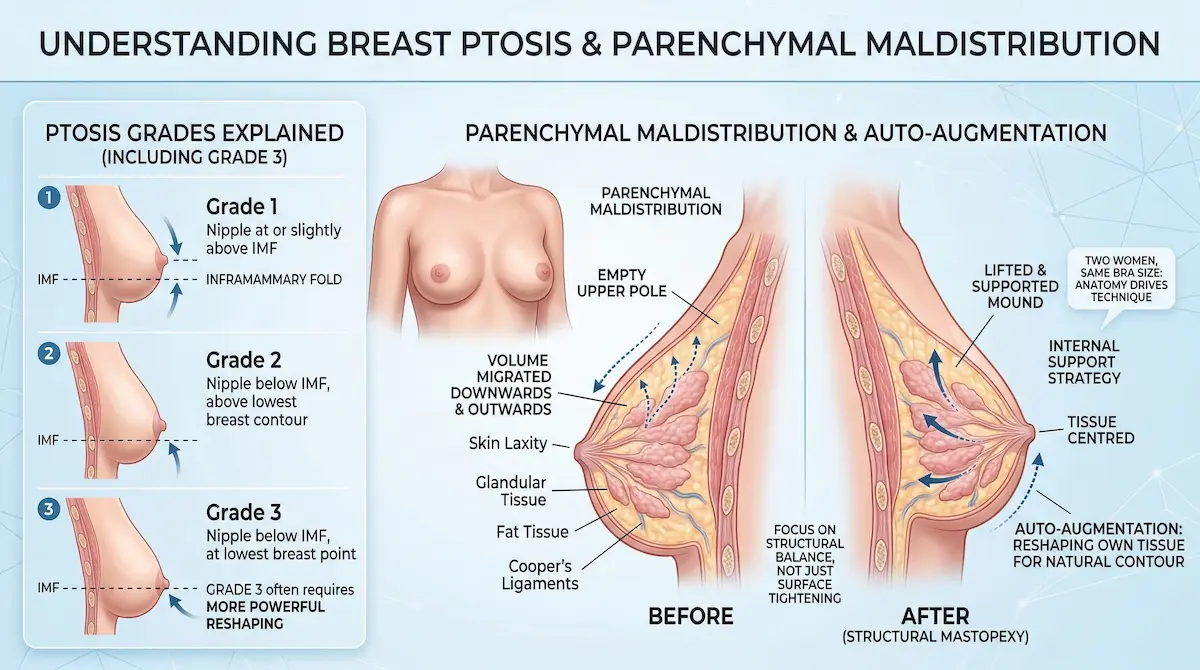
Ptosis grades explained (including Grade 3)
“Ptosis grade” is a clinical way of describing how far the nipple and breast tissue have descended relative to the inframammary fold. Patients often search for Grade 3 ptosis breast lift techniques because this is where a simple, minimal incision approach may be inadequate. With higher-grade ptosis, you typically need more powerful reshaping and a more supportive closure strategy.
- Lower grades may suit a more limited lift, depending on skin quality and tissue strength.
- Higher grades often require a technique that allows both lifting and internal reshaping, not just tightening.
- Asymmetry is common and should be built into the plan from the start.
What “parenchymal maldistribution” actually means
Many women don’t just have droop—they have parenchymal maldistribution in mastopexy, meaning breast volume has migrated downward and outward. That can create an “empty upper pole” look, even if your overall breast size hasn’t changed much. A good plan redistributes tissue to rebuild a centred, supported mound.
This is why two women with the same bra size can need very different operations. Anatomy drives the technique.
Internal support and auto-augmentation: building shape from your own tissue
When upper pole volume is a priority but you want to avoid implants, we may discuss an auto-augmentation breast lift. This uses your own tissue to create better projection and a more youthful contour. It is not “adding volume” from outside—it’s strategic reshaping.
- Auto-augmentation can improve fullness using existing tissue, where suitable.
- Some patients ask about an internal bra breast lift concept, which refers to extra internal support in selected cases.
- Online you may also see terms like “GalaFLEX mesh”; we treat these as tools, not promises, and only discuss them when clinically appropriate.
Our priority is subtle structural improvement—rejuvenation, not alteration.
Am I suitable for an awake breast lift?
Suitability is not just about “wanting local anaesthesia”. It’s about whether your anatomy and health profile match a plan that can be done safely with local anaesthetic and, if needed, twilight sedation. We take this seriously because the awake pathway should feel controlled and predictable. That means proper screening, clear limits, and a surgical plan that makes sense for your body.
If anything suggests you would be safer or more comfortable with a different anaesthetic approach, we will tell you directly.
Health screening and the basics we check
Before we confirm candidacy, we review your medical history, current medications, and any previous anaesthetic experiences. We also look for factors that can change healing or increase complication risk. For UK patients, we can coordinate around recent GP check-ups and existing test results where appropriate.
- General health conditions (including blood pressure and metabolic conditions)
- Medication review (especially blood thinners and certain supplements)
- Previous surgery and scar behaviour
Smoking, healing risk, and scar quality
Smoking and nicotine are major variables in wound healing. They affect circulation and oxygen delivery to tissues. If you are aiming for clean scars and reliable healing, this topic cannot be avoided.
- We will ask about cigarettes, vaping, and nicotine replacements.
- We provide a clear stop window based on your risk profile and plan.
- Scar quality is influenced by genetics, but nicotine is a controllable risk factor.
When an awake pathway may not be the right fit
Some cases are better served by general anaesthesia, particularly if the surgical plan is extensive or combined. Severe anxiety can also make an “awake” experience feel tense, even with sedation. The goal is not to force a technique—it’s to choose the safest route to a natural result.
- Complex multi-procedure plans that require longer operating time
- Medical factors that make sedation planning more difficult
- Patients who prefer to be fully asleep after discussing options
If you want a precise answer, the next step is simple: we review your anatomy, your ptosis grade, and your goals, then map a plan that fits.
Answer a few brief questions about your concerns, health, and goals to discover which treatment options may suit you best.
Breast lift techniques explained: Crescent vs Lollipop vs Anchor
Technique matters. A lot. A breast lift is not a single operation with one “right” scar; it is a set of methods chosen to match your ptosis grade, skin quality, and the amount of reshaping required. We plan the incision pattern to solve a specific problem, not to chase the smallest scar at any cost. When you read about breast lift techniques: Lollipop vs. Anchor vs. Crescent, you are really comparing how much access each method gives us to lift, reshape, and secure the breast mound. The awake pathway does not change the principles of technique selection; it changes the anaesthetic approach.
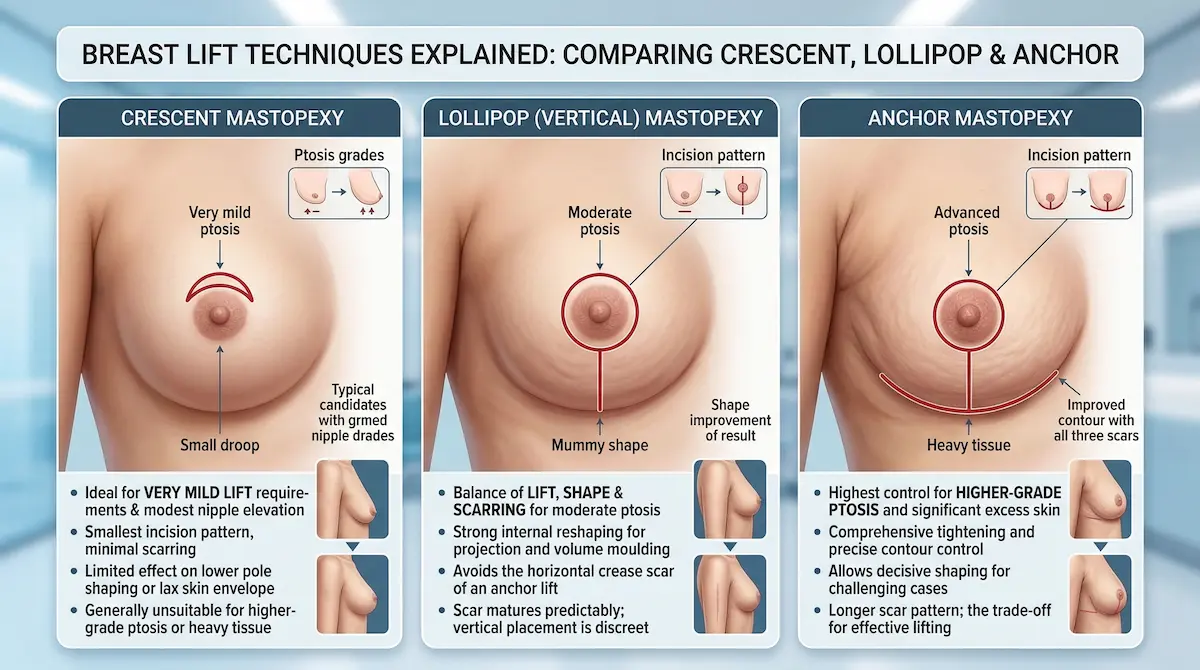
Crescent mastopexy: for very mild lift requirements
A crescent mastopexy uses a small, crescent-shaped excision at the upper areola border. It can offer a modest nipple elevation when the droop is minimal. It is not designed for significant reshaping. For many UK patients researching this option, the key question is simple: “Will this actually correct my shape?”
- Best suited to very mild ptosis and small adjustments.
- Limited ability to reshape the lower pole or tighten a lax skin envelope.
- Often not appropriate for Grade 2–3 ptosis or heavier tissue.
Lollipop (vertical) mastopexy: balance of lift, shape, and scarring
The lollipop approach is also called a vertical technique, because it typically involves an incision around the areola plus a vertical line down to the breast crease. Patients often search for Lollipop breast lift scar because they want to understand where it sits and how it matures over time. This method can offer strong reshaping without the longer horizontal scar of an anchor lift in selected cases.
- Often a good fit for moderate ptosis with a focus on reshaping and projection.
- You may see it described as vertical incision mastopexy when the emphasis is on the internal remodelling rather than skin-only tightening.
- Scar placement is predictable, but scar quality depends on healing factors such as skin type and nicotine exposure.
Anchor mastopexy: more access for higher-grade ptosis and excess skin
An anchor lift adds a horizontal scar along the breast crease in addition to the areolar and vertical incisions. It is usually discussed when there is significant skin excess, heavier tissue, or more advanced ptosis where a smaller pattern can leave residual laxity. This technique gives us more control when shaping has to be decisive. It is not “worse”. It is simply a different tool.
- Often considered for higher-grade ptosis and more extensive skin redundancy.
- Allows more comprehensive tightening and contour control.
- The trade-off is a longer scar pattern, which must be balanced against the benefit in shape.
| Technique | Typical best for | Scar pattern | What it does well | Main trade-off |
|---|---|---|---|---|
| Crescent | Very mild ptosis | Upper areola border | Small nipple lift | Limited reshaping power |
| Lollipop (Vertical) | Moderate ptosis | Around areola + vertical line | Good balance of lift and shape | Not ideal for significant skin excess |
| Anchor | Higher-grade ptosis / excess skin | Around areola + vertical + crease line | Maximum control for lift and tightening | Longer scar pattern |
We plan for a result that looks like you—just lifted, refreshed, and well-balanced. That is the point.
If you are also considering implants, fat transfer, or an internal support concept, technique selection becomes even more important. In those cases, we plan the “architecture” first, then decide the most sensible scar pattern to deliver it.
Lift alone vs lift with implants vs fat transfer: choosing the right combination
Many patients begin with one goal: “I want my breasts higher.” Then a second goal appears: “I also want them fuller.” These are not the same request. A lift repositions and reshapes; it does not automatically restore lost volume. This is where combination planning becomes relevant, especially when you’ve had pregnancy, weight changes, or long-term upper-pole deflation. We keep the plan practical: we match your anatomy to the option that delivers the most natural, stable outcome with the least unnecessary complexity.
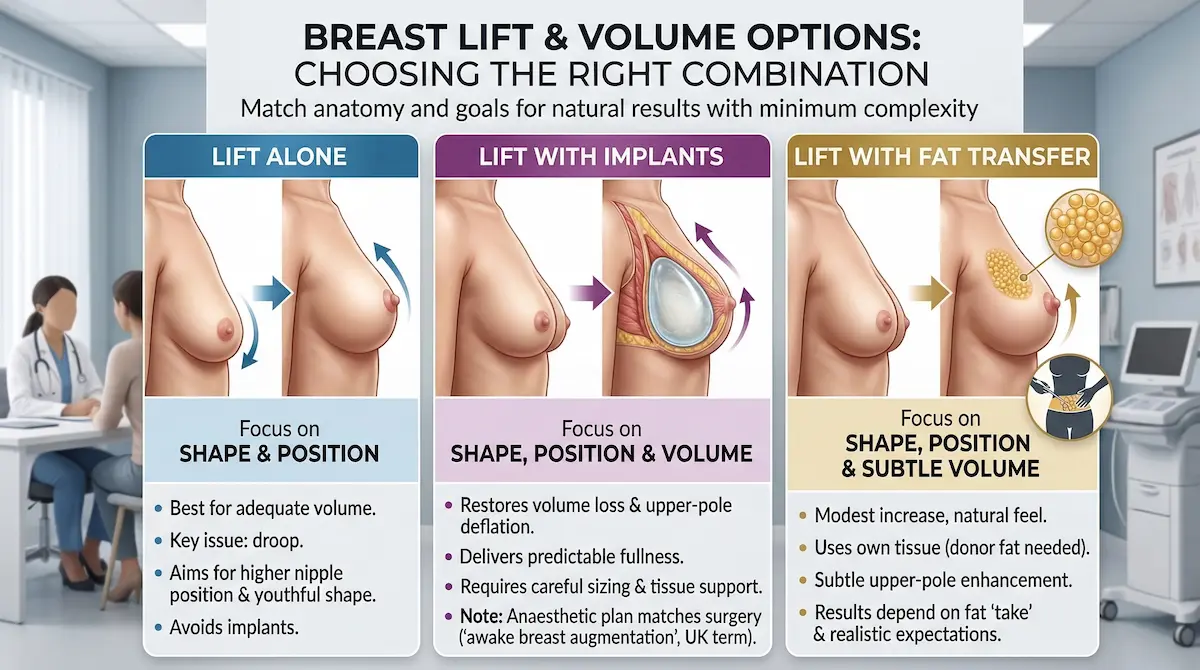
Breast lift alone: when shape and position are the priority
A lift-only plan can be ideal when your breast volume is still adequate and the main issue is droop. It is also the most straightforward route when you want to avoid implants and keep the intervention focused. For many patients, the “win” is a better breast footprint in clothing and a more youthful nipple position.
- Best for patients who like their current volume but want a higher, firmer shape.
- Often combined with internal reshaping to improve projection and reduce “bottoming out”.
- Usually involves fewer long-term variables than implant-based augmentation.
Breast lift with implants: when upper-pole fullness is non-negotiable
If your priority is visible upper-pole volume, implants can be the most predictable way to deliver it. The key is balance. Implant selection must match your tissue strength and your desired look, otherwise the breast can look top-heavy or feel over-stretched. When UK patients search “awake breast augmentation”, they are often trying to understand whether an augmentation element can be paired with local anaesthesia or twilight sedation in selected cases.
- Best for patients with volume loss and a clear preference for fuller upper poles.
- Requires careful implant sizing to respect skin quality and long-term support.
- May not be suitable for every awake pathway; the anaesthetic plan follows the surgical plan.
Fat transfer augmentation: subtle volume using your own tissue
Fat transfer can be a good choice when you want a modest increase and a soft feel, without an implant. The result is usually more subtle than implants. It also depends on how well the transferred fat “takes”. In some plans, fat transfer is used to smooth transitions and improve contour rather than to create a dramatic size change.
- Often suits patients who want natural-looking enhancement rather than a larger cup-size shift.
- Requires suitable donor fat and realistic expectations about retention.
- Can complement a lift by improving upper-pole contour in selected cases.
Our guiding principle is simple: rejuvenation, not alteration. We plan combinations to look refined, not “done”.
If you are researching related options, you may also want to read our pages on breast augmentation and breast reduction to understand how the goals differ. When you are ready, we can review your anatomy and outline what is realistic for your tissue, not just for a photo reference.
Next step (UK patients): Review Your Surgical Plan with a European Board-Certified Specialist.
From VIP airport transfers to 5-star hotel accommodation, we manage every detail. Enjoy a premier medical travel experience in Istanbul.
Anaesthesia: why we use local anaesthesia and twilight sedation
The awake approach is not a gimmick. It is an anaesthetic strategy designed to reduce unnecessary systemic load when the surgical plan allows it. For UK patients, the language matters: we’re usually talking about local anaesthesia with carefully monitored sedation, not “no anaesthetic”. In practice, the goal is simple—keep you comfortable, keep monitoring tight, and support a steadier early recovery.
We choose the anaesthetic plan after we’ve chosen the surgical plan. Not the other way round. That is why we talk you through options in plain terms, including what you may feel, what you won’t feel, and what would prompt us to recommend general anaesthesia. Safety comes first. Always.

Local anaesthesia for mastopexy: what it covers and what it doesn’t
With local anaesthesia, we numb the operative area thoroughly before we begin. You should not feel sharp pain. You may still notice pressure, movement, and the sense that work is happening. That is normal, and we plan for it.
- We aim for complete surgical numbness in the breast and incision zones.
- We set expectations clearly: numb does not always mean “you feel nothing at all”.
- We keep communication open throughout, so comfort can be adjusted in real time.
Twilight sedation in cosmetic surgery: comfort without being “fully asleep”
Many UK patients search for twilight anaesthesia cosmetic surgery because they want a middle ground. Twilight sedation (often described as conscious or semi-conscious sedation) is designed to ease anxiety and help you relax, while maintaining close monitoring. You are not “knocked out” in the same way as a full general anaesthetic.
- It can reduce awareness of time and lower procedural anxiety.
- It may support a calmer theatre experience for patients who don’t want full general anaesthesia.
- Suitability depends on your medical history and the complexity of the surgical plan.
When we recommend general anaesthesia instead
An awake pathway is a choice. It is not a rule. If your plan is extensive, if you are combining procedures, or if anxiety would make the experience stressful, general anaesthesia may be the more sensible option. We would rather choose the safest route than force an “awake” label.
- More complex reshaping or longer operating time can push a case towards general anaesthesia.
- Some medical factors affect sedation planning and monitoring choices.
- Your comfort matters. If you prefer to be fully asleep after discussing options, we respect that.
Rejuvenation, not alteration. The anaesthetic plan should feel as considered as the surgical plan.
If you have had a difficult anaesthetic experience before, tell us. Nausea, prolonged grogginess, panic, or airway concerns all matter. We build your plan around real details, not assumptions.
Our philosophy is “Restoration, Not Alteration.” Discover how our surgeons achieve subtle, naturally restored results that honour your unique beauty.
Step-by-step: what happens in theatre on surgery day?
A well-run surgery day feels structured. Predictable. Calm. From a UK patient’s perspective, it should also feel familiar: clear consent, careful marking, a monitored theatre environment, and a recovery plan you understand. We map the day in advance so you are not trying to process new information when you’re already nervous.
The exact flow depends on your technique (crescent, vertical/lollipop, or anchor) and whether you’re combining a lift with implants or fat transfer. The principles are consistent: confirm the plan, protect blood supply, reshape deliberately, and close carefully. Then we focus on recovery support.
Pre-op marking and final plan confirmation
Before theatre, we re-check your surgical plan and confirm your priorities. Then we perform pre-op markings in an upright position. This matters because breast position changes when you lie down. It is a practical step that improves symmetry and scar placement.
- We review your ptosis pattern and planned nipple–areola position.
- We confirm incision strategy and explain the scar map again.
- We answer last-minute questions directly, without rushing you.
Monitoring, comfort, and the “awake” experience
In theatre, monitoring is continuous. Your comfort is assessed throughout. With local anaesthesia, we numb the area thoroughly, and we can add sedation when appropriate. You are supported by an experienced clinical team from start to finish.
- Local anaesthetic is delivered in a controlled, staged way.
- We check numbness before the main surgical steps begin.
- We adjust comfort as needed rather than “pushing through”.
Reshaping, nipple positioning, and closure principles
The core of mastopexy is internal reshaping. Skin tightening alone is rarely enough for a stable, natural result. We reposition tissue, refine the breast mound, and place the nipple–areola complex where it looks proportionate to your frame. Closure is meticulous because it influences early healing and scar quality.
- We focus on balanced projection and a centred breast footprint.
- We protect blood supply to skin and nipple tissues throughout the procedure.
- We close in layers to support shape and reduce tension on the skin.
After surgery, we move you into recovery and keep instructions simple. You’ll know what “normal” looks like, and what would be a reason to contact us. That clarity is part of safety.
Recovery & aftercare: how long does healing take?
Recovery after a breast lift is usually straightforward, but it is not instant. The first goal is safe healing of the incisions and stable support of the new shape. The second goal is predictable scar maturation. We give you a clear, practical plan, because uncertainty is where anxiety grows.
If you are searching Breast lift recovery week-by-week, you are already thinking like an expert patient. That mindset helps. It keeps you realistic, consistent, and calm through normal healing changes.

Days 1–3: swelling, tightness, and a “keep it simple” routine
Expect tightness, pressure, and a bruised feeling rather than sharp pain. You will be in a supportive surgical bra, and we’ll keep early movement gentle. Most patients do best with short walks, good hydration, and reliable rest. You do not need to “push through” anything.
- Keep your upper body slightly elevated when resting.
- Take short, frequent walks to reduce stiffness.
- Aim for 2–3 litres (approx. 68–100 fl oz) of water daily, unless your clinician advises otherwise.
Week 1–2: returning to routine without stressing the tissues
This is the phase where you often feel better than you look. Swelling can fluctuate, and asymmetry is common early on. Your job is to protect healing, not to judge final shape. We plan check-ups and dressing guidance so you’re not guessing.
- Avoid heavy lifting, intense stretching, and raising arms repeatedly above shoulder height.
- Expect a “high and tight” look early; this usually softens as swelling settles.
- Most desk-based work is possible once you feel comfortable and your plan allows it.
Weeks 3–6: rebuilding strength, easing back into exercise
By this stage, day-to-day comfort is usually much improved, but tissues are still consolidating internally. That is why we reintroduce activity in steps. A structured return is safer than a sudden restart.
- Light lower-body exercise often returns first, then gradual upper-body activity.
- Continue supportive garments as advised to protect shape and reduce pull on scars.
- Scar care becomes more relevant as incisions close and sensitivity reduces.
When to contact us: practical red flags
We prefer early contact over late reassurance-seeking. If something feels “off”, say so. Do not wait it out if you have worsening symptoms. Safety is the priority.
- Fever of 38°C (100.4°F) or above.
- Sudden one-sided swelling, increasing redness, or a new discharge from an incision.
- Shortness of breath, chest pain, or calf swelling (urgent symptoms).
Recovery takes time. Our role is to make it predictable—so you can focus on healing, not worrying.
Next step (UK patients): Review Your Surgical Plan with a European Board-Certified Specialist.
We utilise advanced Hyperbaric Oxygen Therapy (HBOT) to minimise downtime and enhance your healing process. Safety is our primary commitment.
Our Rapid Recovery & Safety Protocol: HBOT + LLLT
For many UK patients, the deciding factor is not just the surgical technique—it’s the recovery system around it. We treat aftercare as a clinical phase, not an afterthought. That is why we integrate advanced recovery technologies into a structured pathway when they are appropriate for your case.
This is the “technology margin” expert patients look for: practical tools that support tissue health, reduce inflammatory load, and promote better-quality healing. It’s also where patients often notice the difference in how they feel during the first two weeks.
HBOT: oxygen support for early tissue recovery
Our HBOT for surgery recovery approach uses 100% oxygen in a pressurised environment to increase oxygen delivery to healing tissues. In simple terms, it’s like giving the body a more oxygen-rich setting to run repair work. Clinically, this can support tissue survival, reduce inflammation, and strengthen the early foundation for scar quality.
- We discuss HBOT pressure using ATA (Atmosphere Absolute), which is a way to describe “how pressurised” the environment is.
- We use it to support oxygenation, reduce swelling, and assist lymphatic drainage in selected patients.
- We also frame it as part of risk reduction, particularly where tissue vulnerability is a concern.
LLLT: cellular support for redness, swelling, and scar maturation
We also utilise LLLT therapy for scars as a gentle, non-heat “soft laser” approach designed to stimulate cellular activity. The aim is not drama. It’s biology—supporting the cells that drive repair and collagen remodelling. When used alongside HBOT, it becomes a practical, layered approach to recovery support.
- LLLT can support cellular energy (ATP) production, which fuels repair work.
- It can complement collagen-focused healing by stimulating fibroblast activity.
- Patients often like it because it is comfortable and fits into a structured aftercare plan.
How we integrate it for UK travel: “flight-ready” planning
Travelling home is a genuine concern, and we treat it that way. Our goal is to clear you properly, not to rush you. When appropriate, we build Flight-ready recovery protocols around check-ups, wound stability, and clear guidance for the journey back to the UK. If we recommend advanced recovery support, we position it as part of safety and predictability—not as a luxury add-on.
- We time check-ups around your travel schedule and wound stability.
- We give written guidance on garments, mobility, and what to watch for at home.
- We plan virtual follow-ups so you are not left alone once you are back in the UK.
“Rejuvenation, Not Alteration” is also a recovery philosophy. We build a plan that protects natural healing and avoids unnecessary stress on tissues.
If you are comparing options, ask one simple question: “What is the recovery system, and how is it delivered?” The answer tells you a lot about standards.
Next step (UK patients): Review Your Surgical Plan with a European Board-Certified Specialist.
Scars and Long-Term Awake Gynaecomastia Results
Scars are a normal part of mastopexy, and for most patients they fade into fine lines over time. What matters is not just the incision pattern, but how the tissues heal and mature over months. If you’re searching healed one year breast lift scars, you’re asking the right question: “What does this look like when it’s truly settled?” The answer depends on technique, skin biology, and how carefully you follow aftercare guidance.
Our approach is realistic and transparent. We plan scar placement thoughtfully, close in layers to reduce skin tension, and then support you with a clear aftercare routine. The aim is a natural result that looks like you—just lifted, refreshed, and proportionate.
Early scars vs mature scars: the timeline that matters
Breast lift scars usually go through predictable phases:
- Weeks 1–6: closed incisions, early redness, sensitivity, and firmness as tissues knit together.
- Months 2–6: scars often look more noticeable before they look better (a common “peak redness” phase).
- Months 6–12: gradual softening, lightening, and smoothing as collagen remodelling continues.
This is why early photos can be misleading. A breast lift should be evaluated on a long horizon, not week-to-week.
What “healed one year” commonly looks and feels like
By around 12 months, many patients notice that scars are softer, flatter, and less pink. You may still see a fine line in certain lighting, particularly around the areola and along the vertical incision (in a lollipop/vertical lift) or the crease line (in an anchor pattern). Genetics plays a role, but so does disciplined aftercare.
- Texture: typically smoother and less raised compared to early months.
- Colour: often fades from pink/red to a lighter tone, though timing varies.
- Sensation: numbness or sensitivity usually improves gradually, but can take longer in some patients.
Scar care habits that actually help
The basics work when done consistently. We tailor guidance to your skin and incision type, but common evidence-based habits include:
- Wearing supportive garments as advised to minimise pull on the scars.
- Keeping scars protected from sun exposure (especially in the first year).
- Using clinician-approved scar therapies (e.g., silicone-based options) once incisions are fully closed.
Scar care is not about chasing perfection. It’s about protecting good healing and giving your skin time to settle.
Our philosophy is “Restoration, Not Alteration.” Discover how our surgeons achieve subtle, naturally restored results that honour your unique beauty.
Safety and risks: what can go wrong and what to watch for
Every surgical procedure has risks, and a high-standard clinic should speak about them clearly. The “expert patient” does not want reassurance alone; they want a plan. Here we focus on practical risk awareness, early detection, and what we do to reduce complications through screening, technique, and structured aftercare.
The awake approach may reduce certain systemic burdens associated with general anaesthesia for selected patients, but it does not eliminate surgical risk. Safety is the result of good judgement, meticulous technique, and a robust recovery protocol.
Common risks after mastopexy
Most issues are minor and manageable when addressed early. Commonly discussed risks include:
- Bruising and swelling (expected to a degree)
- Bleeding or haematoma (rare, but can require urgent assessment)
- Infection (usually treatable when caught early)
- Delayed wound healing (more likely with nicotine use or poor circulation)
- Asymmetry and scar variation (often improves as swelling settles)
Signs of necrosis after breast lift: what it can look like
Patients often search signs of necrosis after breast lift because they want to understand the serious (but uncommon) complications without sugar-coating. “Necrosis” refers to tissue damage due to compromised blood supply. It is not something to self-diagnose online, but there are warning signs that require prompt clinical assessment.
- Worsening pain in a localised area rather than steady improvement
- Skin colour changes that look dusky, grey, very dark, or unusually pale in a patch
- Blistering, persistent weeping, or an area that appears to “break down”
- A foul-smelling discharge or a sudden change in wound appearance
If any of these occur, contact your clinic urgently. If you are back in the UK and symptoms are severe or rapidly worsening, seek emergency assessment.
How we reduce risk: planning, technique, and recovery structure
Risk reduction begins before surgery. We screen carefully, plan the lift pattern to respect blood supply, and close in layers to reduce tension. Then we support healing with a structured aftercare pathway and clear escalation guidance.
- Pre-op: health review, smoking/nicotine strategy, and realistic technique selection for your ptosis grade.
- Intra-op: tissue handling that prioritises perfusion, and closure that supports shape without over-tightening skin.
- Post-op: planned follow-ups, scar strategy, and (when appropriate) advanced recovery support such as HBOT and LLLT.
Transparency is safety. You should know what “normal” looks like—and what needs attention.
Receive a clear, day-by-day itinerary covering arrival, surgery, recovery, and fit-to-fly clearance tailored to your requirements.
Is it safe to have an awake breast lift in Turkey as a UK patient?
UK patients comparing options are not only comparing geography—they’re comparing standards, monitoring, and continuity of care. The question is reasonable. A safe pathway should feel clinically grounded, with clear documentation, clear follow-up, and a recovery plan that still works once you’re back home.
Our focus is to deliver a medical experience that feels closer to the UK private sector mindset—structured, monitored, and detail-driven—while offering the awake technique and advanced recovery technologies that many UK clinics do not routinely integrate.
What “British standards” should look like in practice
Rather than marketing language, look for practical indicators:
- Appropriate theatre environment and infection-control discipline
- Continuous monitoring during sedation and recovery
- Clear written aftercare, medication guidance, and escalation routes
- Real follow-up scheduling (not vague “message us if needed”)
Understanding credentials and specialist-level accountability
UK patients often search for a “GMC registered surgeon” because that is the reference point at home. When you look abroad, the equivalent mindset is to verify specialist training and recognised board-level credentials, then assess the clinic’s standards and outcomes transparency. You should be able to ask direct questions and get direct answers.
Aftercare that continues once you return to the UK
Post-operative care should not end when you get on a plane. We support UK patients with structured follow-ups and clear guidance for at-home recovery. If you need coordination with local care (for example, for dressings or routine checks), we can advise on what to request and when.
- Planned virtual follow-ups at key milestones (e.g., 1, 3, 6, 12 months)
- Clear photo guidance so assessments are consistent and clinically useful
- Direct communication routes for questions and concerns
From VIP airport transfers to 5-star hotel accommodation, we manage every detail. Enjoy a premier medical travel experience in Istanbul.
Awake Breast Lift Cost 2026 (GBP): Turkey vs UK private clinics
UK patients often research breast lift cost UK vs Turkey as part of a broader comparison—quality, safety, technique, and recovery support. We deliberately avoid “bargain” positioning. The awake pathway and advanced recovery technologies are not framed as extras; they are part of a premium, structured medical experience.
The most useful way to compare is to look at what drives cost: theatre time, anaesthetic approach, surgeon time, follow-up depth, and whether advanced recovery options (such as HBOT/LLLT) are integrated or simply unavailable.
What typically drives price differences (without the sales talk)
- Scope of surgery: crescent vs lollipop vs anchor, and whether internal reshaping is extensive.
- Combination plans: lift alone vs lift with implants or fat transfer.
- Aftercare structure: number of check-ups, wound support, and follow-up continuity.
- Recovery technology: whether HBOT/LLLT is included, optional, or not offered at all.
UK interception: London, Manchester, and the private sector comparison mindset
Searches like breast lift price London private clinics or breast lift cost Manchester usually reflect a patient who is already considering UK private care (including Harley Street-style environments). In that context, the meaningful comparison is not “cheapest option”, but “best risk-managed pathway and recovery experience for my anatomy”.
At-a-glance comparison: what UK patients usually compare
| Comparison point | UK private sector (typical pathway) | AKM Clinic (awake + recovery protocol focus) |
|---|---|---|
| Anaesthesia | Often general anaesthesia as default | Local anaesthesia with optional twilight sedation where suitable |
| Recovery support | Standard post-op care and routine follow-ups | Structured aftercare with optional HBOT + LLLT integration |
| Transparency | Varies by clinic and surgeon | Technique-led planning, scar education, and risk discussion |
| Patient experience | Local access, but technology and protocol depth vary | Planned journey with continuity from consultation to long-term follow-up |
| Cost framing | Often itemised with add-ons | Premium, plan-based pathway (GBP-focused for UK patients) |
Next step (UK patients): Review Your Surgical Plan with a European Board-Certified Specialist.
Receive a 100% transparent, all-inclusive quote tailored to your needs. No hidden fees—just world-class care at an accessible price.
Finding the best surgeon for an awake mastopexy
The awake technique is only as good as the judgement behind it. You are not just choosing a clinic—you are choosing a plan, a standard, and a team. For UK patients, it helps to approach this like a clinical audit: credentials, technique rationale, complication planning, and follow-up structure.
If a consultation feels rushed or sales-led, that is a signal. The right consultation should feel like problem-solving.
Questions that reveal surgical depth
- Which technique fits my ptosis grade—and why?
- How will you address parenchymal maldistribution, not just skin laxity?
- What is your plan to support long-term shape (not only early lift)?
Questions that reveal anaesthetic competence
- Am I suitable for local anaesthesia and/or twilight sedation for my plan?
- How will you manage comfort and monitoring during the procedure?
- What would make you recommend general anaesthesia instead?
Questions that reveal aftercare standards
- What is the follow-up schedule before I fly home?
- What support is available once I’m back in the UK?
- How do you handle wound concerns, scar issues, or unexpected symptoms?
The right surgeon won’t promise perfection. They will explain process, risks, and realistic outcomes with confidence and clarity.
Your UK-to-Istanbul medical journey: premium planning, not “medical tourism”
The experience should feel seamless and clinical—not like a package deal. For UK patients, that means structured communication, clear scheduling, and a pathway that respects your time and your safety. We plan your journey around clinical milestones, not around convenience alone.
This is where the “Medical Bridge” mindset matters: a private-care standard of planning and follow-up, paired with advanced technique and recovery support.
Remote consultation: what we review before you travel
- Your goals and anatomy (including ptosis grade and tissue distribution)
- Medical history, medications, and any relevant test results
- A clear plan: technique, anaesthesia route, and recovery structure
Travel timing and staying “flight-ready”
Travelling safely is part of the plan. We schedule check-ups to confirm wound stability and provide clear guidance for the journey back. If you have a desk-based role, we also help you plan a sensible return-to-work timeline based on your procedure scope.
Follow-up once you’re home in the UK
Recovery continues after you return. We maintain continuity with planned virtual follow-ups and clear guidance on what to send us (photos, symptoms, questions), so assessments are clinically meaningful and not guesswork.
Next step (UK patients): Review Your Surgical Plan with a European Board-Certified Specialist.
We utilise advanced Hyperbaric Oxygen Therapy (HBOT) to minimise downtime and enhance your healing process. Safety is our primary commitment.
Frequently Asked Questions: Awake Breast Lift
If you’re comparing an awake breast lift to a conventional mastopexy pathway, the questions tend to be specific: “Can this really be done under local anaesthesia?”, “How soon can I fly?”, “What should I look for in safety standards?”, and “How do I compare London private clinics to Istanbul without falling into ‘package deal’ thinking?” This FAQ is written to answer those practical points directly, in UK terms and with a risk-managed mindset.
Can a breast lift (mastopexy) be done under local anaesthesia?
Yes—an awake breast lift can be performed under local anaesthesia in selected cases, often with optional twilight sedation for comfort. Suitability depends on your anatomy, the technique required (crescent vs lollipop vs anchor), and whether you’re combining procedures (implants or fat transfer may change the anaesthetic plan). The safest approach is the one matched to your surgical plan.
Is twilight sedation safe for cosmetic surgery?
When properly planned and monitored, twilight anaesthesia is a well-established approach used across many procedures. The important variables are patient selection, medical history, appropriate monitoring, and an experienced clinical team. If you have anxiety, previous nausea, or any history of difficult sedation/anaesthesia, tell your clinician so the plan can be tailored.
What does “awake” actually feel like during surgery?
“Awake” does not mean you feel pain. Local anaesthesia is designed to prevent sharp pain, while twilight sedation can reduce anxiety and awareness of time. Some patients still notice pressure or movement. Your comfort is actively managed, and the team should explain in advance what sensations can be normal.
How soon can I fly after a breast lift?
Timing depends on the scope of surgery, wound stability, swelling, and your overall recovery progress. The safest approach is to plan travel around clinically sensible milestones, not a fixed number of days. We focus on “flight-ready” planning through scheduled check-ups and clear guidance for the journey, including mobility and what to watch for once you’re home.
How do I compare breast lift cost UK vs Turkey without chasing the cheapest option?
Think in terms of “clinical pathway value”, not headline price. Compare technique rationale, anaesthetic strategy (awake/twilight vs general), follow-up structure, and whether advanced recovery support is integrated. Searches like breast lift cost UK vs Turkey often miss the most meaningful difference: recovery depth and transparency.
What about UK finance options and “breast lift price UK finance” searches?
Many UK patients explore breast lift price UK finance while comparing London or Manchester private clinics. Financing can change monthly cost, but it doesn’t change surgical fundamentals: technique selection, anaesthetic planning, monitoring, and aftercare. If you are comparing options, keep the clinical pathway as your first filter, then decide what fits financially.
How do I compare Harley Street standards to Istanbul clinics?
Searches like breast lift Harley Street quality standards reflect a desire for predictable systems: sterile theatres, monitoring, clear consent, documented aftercare, and accessible follow-up. Use those operational indicators as your comparison tool. Location is not the standard—process is the standard.
Is there a meaningful “best breast lift surgeon London vs Istanbul” comparison?
A useful comparison is less about geography and more about fit: the surgeon’s specialist background, their ability to explain technique choice for your anatomy, and the clinic’s recovery infrastructure. If you’re searching best breast lift surgeon London vs Istanbul, translate that into questions: “Who can explain my ptosis grade and tissue distribution clearly, and who has a structured protocol for risk reduction and aftercare?”
I live outside London—does city matter (Manchester, Glasgow, etc.)?
City-specific searches such as breast lift cost Manchester or breast lift Glasgow are common because patients start local. The decision usually becomes: stay local for convenience, or travel for a more specialised pathway. If you’re considering travel, focus on anaesthetic options, recovery structure, transparency, and continuity once you are back in the UK.
What should I look for in “awake mastopexy safety reviews”?
When patients search awake mastopexy safety reviews, they’re often looking for two things: genuine patient experience and evidence of good systems. Look for consistency in how the clinic explains technique, anaesthetic planning, and follow-up. Be cautious of reviews that only mention hotels or transfers. The most valuable reviews describe clarity of consultation, post-op support, and how concerns were handled.
Do you have long-term follow-up for UK patients once I’m home?
A safe pathway should include structured follow-ups after you return to the UK. We plan virtual review points (commonly at 1, 3, 6, and 12 months), with clear guidance on what to send (photos and symptom notes) so assessments are consistent and clinically meaningful.
What does “Mastopexy Turkey before and after (1 year healed)” really tell me?
The most meaningful before-and-after sets include long-term healing, not only early photos. If you’re searching mastopexy Turkey before and after (1 year healed), you’re trying to see scar maturity and settled shape. That’s the right instinct. Ask about timelines, technique used, and whether results are shown after swelling has fully settled.
Next step: review your surgical plan (UK patients)
An awake breast lift is best approached like any premium medical decision: with a precise diagnosis (ptosis grade and tissue distribution), a technique-led plan (crescent vs lollipop vs anchor, and whether auto-augmentation or support concepts are relevant), and an anaesthetic strategy that matches the surgery—not marketing. If you want to move forward, the most useful next step is a structured plan review.
We avoid “get a quote” language on purpose. Instead, we focus on clinical planning: your anatomy, your priorities, and the safest pathway to a natural, refined uplift. If you’re comparing options—including breast lift Turkey prices (Premium All-Inclusive)—we’ll clarify what is included, what is not, and why, so you can make a decision with confidence.
Call to action: Review Your Surgical Plan with a European Board-Certified Specialist.
Awake Breast Lift: Patient Stories

Sarah


Lisa


Mrs. Giordano
Awake Breast Lift Surgeons
Awake Breast Lift Cost in Turkey
Starting from ~ £3400
* There are no hidden fees or unexpected charges.
- Your PersonalisedAwake Breast LiftProcedure
- All Specialist Surgeon & Anaesthesia Fees
- All Pre-Op Tests & Post-Op Check-ups
- 5-Star Hotel Accommodation (incl. breakfast)
- All Private VIP Airport & Clinic Transfers
- 24/7 Dedicated Patient Coordinator & Translation Services
Awake Breast Lift: A Cost Comparison
| City | Cost |
|---|---|
| London (Harley Street) | ~£10,000 |
| Manchester | ~£9,000 |
| Birmingham | ~£8,500 |
| Glasgow | ~£8,000 |
| Liverpool | ~£8,000 |
Awake Breast Lift: Patient Reviews
Jammal Canada
I have had face and neck lift with AKM Clinic they have been so good to me and my operation went so smoothly🥰 i would like to thank my doctor here and also to the team 💐

Ava Canada
Thank you AKM Clinic for giving me my confidence back! Had facelift + temporal lift 3 months ago and the outcome is already stunning. Special thanks to Hande!

Jakayla USA
Had a deep plane facelift and lower eyelid procedure at AKM Clinic 7 months ago. The results are fantastic - very subtle and natural. I didn’t expect the entire experience to be so comfortable. Hande managed everything and kept in contact even after I returned to USA. I’m beyond pleased with the outcome and the care I received. Would do it again in a heartbeat!

Barbara United Kingdom
It has been 4 months since my surgery. Everything is great, The most important thing is l love the way l look, l look exactly how l wanted. Meaning l look natural, just almost 40 years younger. I pulled Facebook - majority voted 37ys. I also had face, neck, chest, and hands CO2 laser. My skin is flawless.

Lisa Canada
I had a face, neck and arm lift at AKM. I’m just over 4 weeks post and couldn’t be happier with the results. The entire experience was wonderful! My coordinator, Khadija made me feel comfortable from beginning to end! I highly recommend AKM and will definitely go back for other procedures!

Julie USA
I am beyond grateful I went with AKM Clinic for my deep plane face and neck lift, upper eyelid, and co2 laser. Dr. Akif has magic hands and my results are truly incredible! I came from the US and assistant Emine was the best in assuring every detail was coordinated and communicated with me beyond my expectations every step of the way. 10 out of 10 to the entire team! I couldn’t be more pleased!

Ready to Begin Your Own Transformation Journey?
Join the 2,000+ patients who have trusted Dr Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, naturally restored you begins with a simple, no-obligation conversation. Contact us today from the UK for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. There are no hidden fees.
#2: Secure Your Date & VIP Booking
Once you are ready, our dedicated patient coordinators will help you secure your procedure date. We will handle all your bookings, including your 5-star hotel accommodation and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you will meet your specialist surgeon to finalise the details for your natural, subtle, and restored new look.




