Breast Reduction in Turkey




- Breast Reduction relieves heaviness and improves proportion through personalised reduction mammoplasty planning.
- Technique-led safety explains Wise/Vertical/Benelli options and pedicle choices to protect blood supply and healing.
- Clear recovery timeline covers week-by-week expectations, aftercare support, and red-flag guidance for peace of mind.
- Cost and value focus compares UK vs Turkey and clarifies all-inclusive inclusions for transparent decision-making.
AI-generated summary, fact-checked by our medical experts.
Breast Reduction: Quick Facts
Duration of Surgery
Type of Anaesthesia
Initial Recovery Period
Hospital Accommodation
Return to Daily Activities
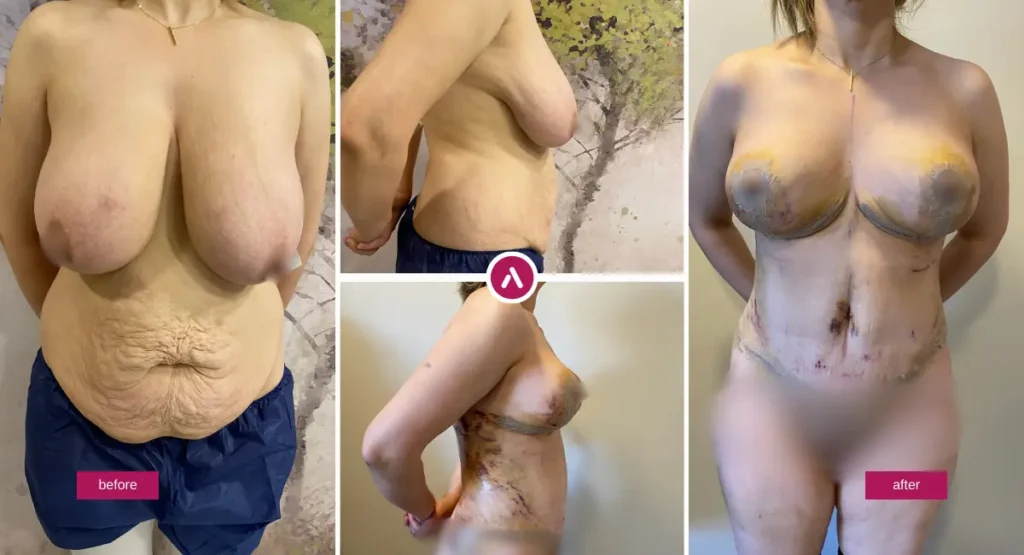
Breast Reduction Results: Before and After
Breast Reduction in Turkey is often chosen by UK patients who want a medically led solution for heavy, uncomfortable breasts without long waiting times. This procedure, also known as reduction mammoplasty, removes excess tissue and skin while reshaping and lifting the breast for a natural, proportional result. The aim is both functional relief and aesthetic balance—helping with comfort in daily life, sport, and clothing fit. Your outcome depends on personalised planning, safe technique selection, and structured aftercare.
This guide explains Breast Reduction with the detail an “expert patient” expects: incision options such as Wise pattern (anchor) and vertical (lollipop), pedicle choices that protect blood supply, and a realistic recovery timeline. You’ll also learn how to evaluate surgeon standards, facility safety, and follow-up support—especially important when travelling to Istanbul. If you’re comparing breast reduction cost UK vs Turkey, we focus on value and transparency: what’s included, how risk is managed, and how your care continues once you return to the UK.
Table of Contents
What is Breast Reduction?
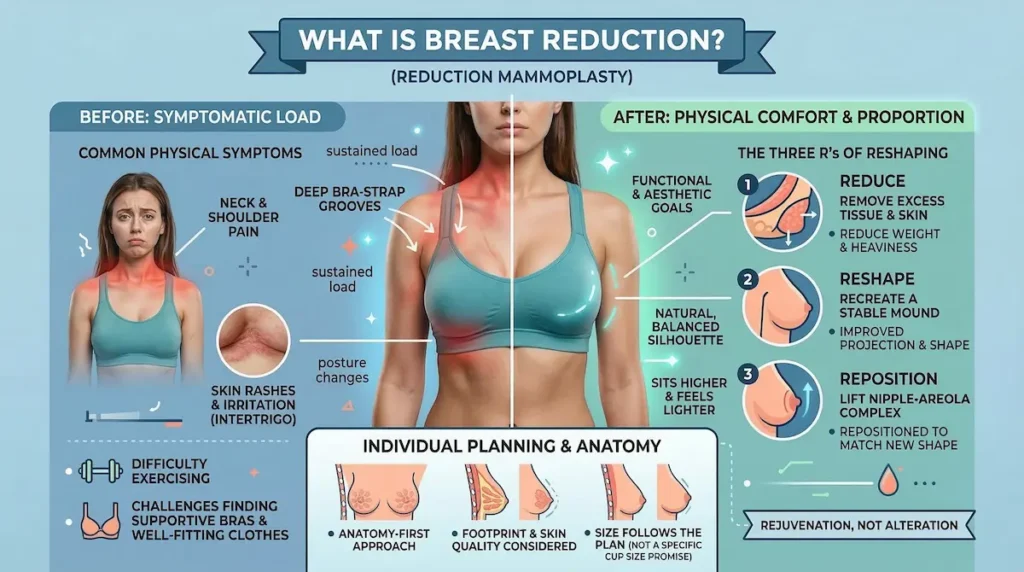
Breast Reduction is a surgical procedure that reduces breast volume while reshaping and lifting the breast for improved proportion. It removes a controlled amount of glandular tissue, fat, and excess skin. The aim is physical comfort as well as a balanced silhouette. Many patients also need the nipple–areola complex repositioned. Clinically, it is known as breast reduction surgery or reduction mammoplasty.
Definition: Reduction Mammoplasty (Bilateral Reduction Mammoplasty)
In surgical terms, reduction mammoplasty describes reducing breast size and weight, then rebuilding the breast shape so it sits higher and feels lighter. When both breasts are treated, it may be described as bilateral reduction mammoplasty. The procedure is not simply “making the breast smaller”. It is a structured reshaping operation.
- Reduce: remove tissue and skin to relieve heaviness.
- Reshape: recreate a stable breast mound with improved projection.
- Reposition: lift the nipple–areola complex to match the new breast shape (when appropriate).
Because every breast has a different footprint, density, and skin quality, we plan breast reduction around anatomy first. Size comes as a result of that plan, not as a promise of a particular cup size.
Why breasts become heavy and symptomatic
Large, heavy breasts can place sustained load on the neck, shoulders, and upper back. Skin-on-skin contact can also lead to irritation, especially in warm weather or during exercise. Some patients notice that their posture changes over time, simply to compensate for weight at the front of the chest. Others find that bras do most of the “lifting work”, which can become uncomfortable.
- Neck, shoulder, and upper back discomfort.
- Deep bra-strap grooves and pressure marks.
- Intertrigo (rash) and recurrent irritation under the breast fold.
- Difficulty exercising comfortably, especially running or high-impact activity.
- Challenges finding supportive bras and well-fitting clothing.
For the UK patient researching thoroughly, this symptom pattern often matters as much as the aesthetic outcome. It helps define whether surgery is being considered for comfort, proportion, or both.
Aesthetic goal vs functional goal (Rejuvenation, Not Alteration)
A well-planned breast reduction can be both functional and aesthetic. Functionally, the priority is reducing weight and improving day-to-day comfort. Aesthetically, the goal is proportion: a breast shape that sits naturally on the chest wall and aligns with your frame. The result should look like “you”, just better balanced.
Our approach is guided by a simple principle: “Rejuvenation, Not Alteration.”
In practice, that means we aim for a breast shape that is harmonious rather than “surgical-looking”. We also discuss scarring honestly from the start, because scar pattern is part of the technique selection and part of realistic planning.
Share your photos and medical history to receive a personalised assessment from our European Board-certified facial surgery team.
Benefits of Breast Reduction Surgery
The benefits of breast reduction are often immediate in daily life, but they are also long-term in how you move, dress, and exercise. Many patients describe a sense of lightness and improved ease with posture. Others value the change in proportion, especially when clothing fits more predictably. The key is matching the surgical plan to your anatomy and your goals. Done properly, the outcome should feel practical as well as aesthetic.
Physical relief and daily comfort
For patients seeking symptom relief, the most meaningful benefit is reducing mechanical load. Less weight can make simple tasks feel easier: walking briskly, taking the stairs, or sitting at a desk for long periods. The bra may feel like support rather than a necessity. Comfort can become more consistent across the day.
- Reduced pressure on the neck, shoulders, and upper back.
- Less pulling and bounce during movement.
- Improved comfort in bras, including wider choice in supportive styles.
Sport, posture, and skin health
Activity is often the deciding factor for surgery. When breast size limits exercise, overall fitness can suffer. Reducing volume can make high-impact activity more manageable, while also reducing friction under the breast fold. Better skin ventilation and less moisture trapping can support healthier skin in the long term.
- Easier participation in sports and gym routines.
- Less under-breast irritation and heat rash risk.
- More natural posture during standing and walking.
Clothing fit and proportion (natural-looking balance)
Breast reduction can help restore proportion between the chest, waist, and hips. Many patients find they can choose clothes for style rather than for “accommodating the bust”. That often includes improved fit in button-down shirts, dresses, and tailored jackets. The aim is not to create a generic shape, but a result that suits your frame and looks natural from the front and side profiles.
- Improved fit in everyday clothing and occasion wear.
- Greater confidence with swimwear and activewear.
- A more balanced silhouette that feels consistent with your body.
Answer a few brief questions about your concerns, health, and goals to discover which treatment options may suit you best.
Am I a Suitable Candidate?
Breast reduction is most suitable for patients who feel that breast size affects comfort, activity, clothing fit, or overall proportion. During consultation, we assess not only size, but also breast density, skin quality, symmetry, nipple position, and your goals. A good candidate is someone who wants a balanced, sustainable result and understands that the operation is a structured reshaping procedure, not just “removal”.
The “expert patient” checklist: symptoms, goals, and expectations
If you are researching breast reduction in depth, it helps to organise your decision around a few practical questions. These are the same questions we use to plan a safe, predictable operation:
- Symptoms: Do you have neck/shoulder discomfort, bra-strap grooves, skin irritation under the breast fold, or difficulty exercising comfortably?
- Proportion: Do you want your bust to feel more in harmony with your frame (rather than “as small as possible”)?
- Shape preferences: Do you prefer a more lifted, compact shape, or a softer natural contour?
- Scars: Are you prepared for scars as part of the trade-off for a lighter, reshaped breast?
- Long-term factors: Do you have future pregnancy plans or significant weight changes expected?
We also discuss what matters most to you: symptom relief, aesthetics, or a balanced combination of both. Clear priorities help us choose the most suitable technique.
Health factors that affect safety (smoking, BMI, comorbidities)
Safety is influenced by your overall health and by factors that affect circulation and wound healing. This matters in every country and every setting. In breast reduction, the quality of blood supply to the skin and the nipple–areola complex is a key consideration, so we evaluate risk factors carefully.
- Smoking/vaping/nicotine: Nicotine can compromise microcirculation and can increase wound-healing risks. A nicotine-free period is typically advised.
- BMI and metabolic health: Higher BMI can be associated with a higher risk profile in many operations. Assessment is individual and should be discussed clinically.
- Medical conditions: Diabetes, clotting disorders, uncontrolled hypertension, and certain autoimmune conditions may require additional planning or specialist input.
- Medications: Blood-thinning medication and some supplements can affect bleeding risk and should be reviewed prior to surgery.
None of these factors automatically exclude you, but they do shape how we plan surgery and aftercare. The goal is to reduce avoidable risk and support a smooth recovery.
UK pathway context: NHS breast reduction criteria / private options
In the UK, many patients begin their research after exploring NHS options. NHS breast reduction criteria can vary by region and are often strict, with thresholds that may include BMI considerations, symptom documentation, and evidence of conservative management. Even when criteria are met, waiting times can be a challenge. Others explore private breast reduction UK options and then compare value, access, and what is included in aftercare.
Wherever you are on that pathway, the most important step is a proper clinical assessment. A consultation should clarify candidacy, realistic outcomes, likely scar pattern, and a personalised recovery plan.
Breast Reduction Surgical Techniques Explained
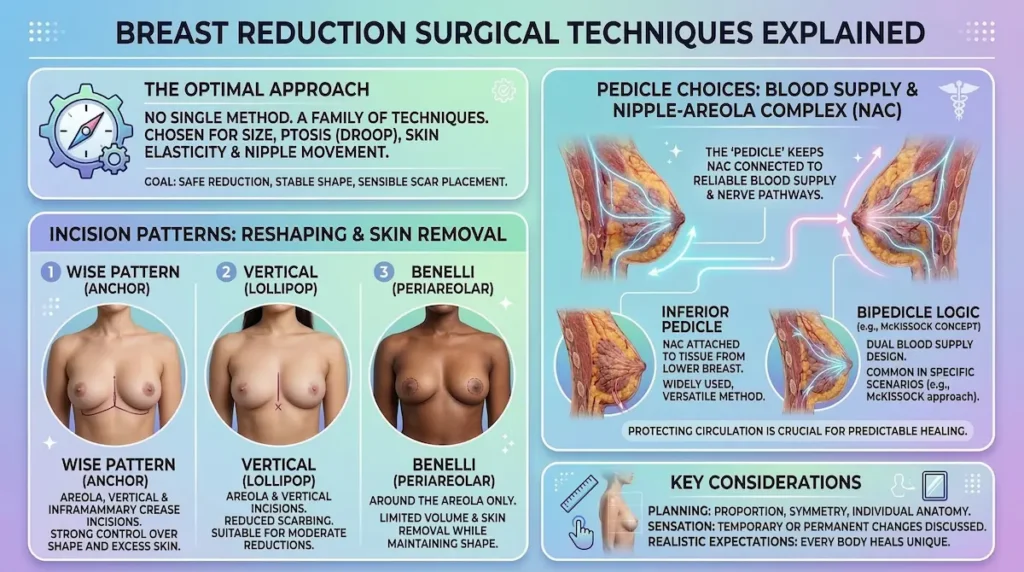
Breast reduction is not a single technique. It is a family of techniques chosen according to breast size, degree of ptosis (droop), skin elasticity, and how far the nipple–areola complex needs to move. The “best” method is the one that safely achieves your goals with stable shape and sensible scar placement.
Incision patterns: Wise Pattern (Anchor) vs Vertical (Lollipop) vs Benelli (Periareolar)
The incision pattern is a design choice that allows the surgeon to remove tissue and skin while reshaping the breast. The most commonly discussed patterns include:
- Wise pattern reduction mammoplasty (Anchor): Often used for larger reductions or significant reshaping. It typically includes an incision around the areola, a vertical line down to the breast crease, and a line within the crease. This pattern can provide strong control over shape and excess skin.
- Vertical reduction mammoplasty (Lollipop): Uses an incision around the areola plus a vertical line to the crease, usually avoiding the long crease incision. It may be suitable for moderate reductions and can reduce scar length in selected patients.
- Benelli reduction mammoplasty (Periareolar): Focuses around the areola. It can be appropriate for carefully selected cases, but it has limitations in how much volume and skin it can manage while maintaining shape.
These are not cosmetic “preferences” alone. They are engineering decisions: the incision pattern must match how much tissue needs to be removed and how much skin needs to be tightened to create a stable, natural-looking breast.
Pedicle choices: Inferior pedicle, McKissock, and blood supply logic
A “pedicle” is the segment of tissue that keeps the nipple–areola complex connected to a reliable blood supply and nerve pathways. This is one of the most important safety and quality considerations in breast reduction, especially when a significant lift is required.
- Inferior pedicle reduction mammoplasty: The nipple remains attached to tissue from the lower portion of the breast. It is a widely used approach and can be suitable in many breast sizes, depending on anatomy and goals.
- McKissock technique: Commonly described as a bipedicle approach, designed to support blood supply in certain scenarios. As with all techniques, suitability depends on individual anatomy.
Technique selection is not about using a fashionable method. It is about choosing the safest route to achieve the planned breast shape while protecting circulation and supporting predictable healing.
Nipple–areola complex positioning, sensation, and symmetry
Most breast reductions involve repositioning the nipple–areola complex to suit the new breast contour. Our planning focuses on proportion and symmetry, while being mindful that every body heals uniquely. Sensation can change temporarily during recovery, and in some cases changes can be longer-lasting. We discuss these possibilities clearly in consultation so expectations are realistic.
Finally, symmetry is a goal, not a guarantee. Natural breasts are rarely identical, and small differences in healing can influence final shape. Meticulous planning and careful technique reduce those differences, but honest pre-operative discussion is essential.

Planning Size, Shape, and Scars
Breast reduction planning is a balance of anatomy, proportion, and safety. The goal is a breast shape that looks natural on your frame, feels lighter in daily life, and remains stable over time. This is why pre-operative planning focuses on measurements, tissue quality, and how the breast sits on the chest wall, rather than on a single “before/after” image or a cup-size target.
How we plan proportion (not a ‘cup size promise’)
It is understandable to think in terms of cup sizes, but cup sizing varies between brands and styles, and it does not reliably reflect breast shape, density, or skin elasticity. Instead, we plan breast reduction using:
- Breast footprint and base width: how the breast attaches to the chest wall and what “natural proportion” means for your frame.
- Degree of ptosis (droop): how far the breast and nipple have descended, and how much lifting is required.
- Skin quality: elasticity and stretch marks can influence how the breast settles during healing.
- Tissue composition: glandular tissue and fatty tissue behave differently, which affects long-term shape stability.
- Symmetry planning: we plan for balance, while recognising that natural breasts are rarely identical.
From a patient perspective, the most useful way to define your goal is in outcomes that matter day-to-day: comfort during activity, improved fit in clothing, and a silhouette that feels consistent with your body. During consultation, we translate those goals into a surgical plan that prioritises safety and proportion.
Areola reduction and breast shape refinement
Many breast reductions also involve reshaping or resizing the areola. This is not always necessary, but it can be helpful when the areola has stretched over time due to breast weight and skin laxity. The objective is to create a result that looks harmonious with the new breast size and contour.
Shape refinement is equally important. Breast reduction is not simply “taking tissue away”. A high-quality outcome involves rebuilding the breast mound with good projection and a natural slope, then positioning the nipple–areola complex to match that contour. This is one reason technique selection (incision pattern and pedicle choice) is so central: it affects how well the breast holds its shape as swelling settles and tissues mature.
Scar strategy and management (including LLLT support)
Scarring is an unavoidable trade-off in breast reduction, and realistic planning is part of safe, ethical surgical care. The scar pattern depends on the technique required to achieve your planned reshaping (for example, Wise pattern/anchor scars versus vertical/lollipop scars in selected cases). What matters most is not only where scars sit, but how well they heal.
Scar healing is a process. Early scars can look red or firm while the body remodels collagen. Over time, scars usually soften and fade, but the timeline varies between individuals. Factors such as genetics, skin type, tension on the incision, nicotine exposure, and aftercare compliance all influence scar quality.
- Early phase: protecting the incisions, supporting the breast with the recommended garment, and avoiding unnecessary tension.
- Intermediate phase: structured scar care as advised (for example, silicone-based approaches where appropriate) and gradual return to activity.
- Long-term: consistent sun protection and patience while scars mature.
In selected cases, we may incorporate supportive technologies such as LLLT (low-level laser therapy) as part of a broader recovery and scar-management strategy. This is not a “magic fix” and it cannot guarantee a particular scar outcome, but it can be used as an adjunct within an evidence-informed aftercare plan. The most important driver of a good scar outcome remains good surgical technique, safe wound healing, and consistent aftercare.
Combined Procedures (Synergy) with Breast Reduction Surgery
Breast reduction is frequently considered alongside other procedures, especially when patients want overall balance rather than a change in one area alone. Combining procedures can be appropriate, but the plan must prioritise safety: operative time, recovery demands, and the total physiological “load” of surgery are all relevant. A responsible combined plan is always tailored to your anatomy, medical history, and recovery capacity.
Breast reduction with lift (mastopexy logic)
In practical terms, most breast reductions include an element of breast lift because removing tissue and tightening skin naturally reshapes and elevates the breast. However, the “lift component” can vary. Some patients benefit from a more pronounced repositioning and reshaping, particularly when there is significant ptosis or when the nipple–areola complex sits low on the breast. In these cases, the lift element is often discussed as mastopexy principles applied alongside reduction mammoplasty.
The key is alignment between goals and anatomy: a tighter, more lifted look may require more skin adjustment, which can influence scar pattern and tension. We plan for a result that looks natural, sits in a stable position, and matches your frame—rather than pursuing an overly tight aesthetic that may not age as well. When patients ask whether they “need a breast lift”, we explain how mastopexy strategy is integrated into the reduction plan to create proportion, comfort, and long-term balance.
Reduction + liposuction (axillary/bra fat) considerations
Some patients have fullness at the outer breast or underarm area (often described as “bra fat” or axillary fullness). In selected cases, liposuction can be used as an adjunct to refine the side contour and improve how clothing sits. This is not required for everyone, and it is not a substitute for structured breast reduction when tissue removal and reshaping are needed.
When considered, the discussion should be clear about what liposuction can and cannot do:
- Can help: smoothing outer contour and reducing localised fullness in selected anatomy.
- Cannot replace: reshaping the breast mound, lifting the nipple–areola complex, or addressing significant skin excess.
Mummy Makeover combinations (UK localisation)
Patients in the UK often research breast reduction alongside post-pregnancy body changes. A “Mummy Makeover” approach may involve breast surgery plus abdominal procedures (for example, a tummy tuck in suitable candidates). The principle is total balance, but the priority is always safety and a sensible recovery plan.
Not every patient is suited to combining multiple major procedures at once. The decision depends on your health profile, surgical time considerations, and how your recovery will be supported. In some cases, a staged plan is the safer, more predictable path—especially when it reduces operative time and allows focused healing. A high-quality plan is not defined by “how much can be done in one session”, but by achieving stable results with a risk profile you understand and accept.
Anaesthesia: Why We Prefer Awake/Twilight Sedation
Anaesthesia is not a “background detail” in breast reduction. It influences how you feel immediately after surgery, how smoothly you can mobilise, and how your care team manages comfort and safety. The right approach depends on your medical history, the scope of the reduction, and the clinical judgement of your surgeon and anaesthetist.
What “twilight anaesthesia” means (UK terminology)
“Twilight” commonly refers to intravenous (IV) sedation where you are very relaxed and drowsy, and you may not remember much of the procedure. It is typically paired with local anaesthetic to keep the surgical area comfortable. You are not “fully asleep” in the same way as general anaesthesia, but you are also not expected to be alert or engaged. Monitoring is continuous, and the anaesthetist’s role remains central throughout.
Depending on the case, anaesthesia options may include:
- General anaesthesia: you are fully asleep with airway support managed by the anaesthetist.
- IV sedation (“twilight”) with local anaesthetic: you are deeply relaxed and sleepy while the surgical area is numbed.
- Local anaesthetic with sedation (selected cases): a tailored combination depending on your needs and the planned procedure.
When twilight/awake sedation may be appropriate vs when general anaesthesia is better
There is no single “best” anaesthetic for every patient. The safest choice is the one that matches your risk profile and the technical demands of your surgery.
Twilight/IV sedation may be considered in selected patients when the surgical plan and your health profile are suitable. Some patients also prefer the idea of avoiding a full general anaesthetic. However, suitability is always determined clinically.
General anaesthesia may be recommended when:
- The reduction is extensive or the operative plan is complex.
- There are airway or medical factors that make deep sedation less suitable.
- Positioning, operative time, or comfort considerations favour a fully controlled anaesthetic.
Your consultation should include an honest discussion about what is appropriate for you. A responsible clinic will not “sell” a particular type of anaesthesia as a universal upgrade. It should be a medical decision made with your anaesthetist and surgeon.
Why anaesthesia choice affects recovery and risk management
Anaesthesia can influence early recovery in practical ways: nausea, grogginess, pain control, hydration, and the ease of mobilising. Some patients experience a smoother immediate recovery with lighter anaesthetic strategies, while others do best with a full general anaesthetic for optimal comfort and procedural control. In all cases, what matters most is that safety is prioritised through:
- Appropriate pre-operative assessment and optimisation (where possible).
- Continuous monitoring in theatre and during early recovery.
- A clear plan for pain relief, nausea control, and mobilisation.
- Risk-reduction measures tailored to the individual (for example, clot-risk assessment).
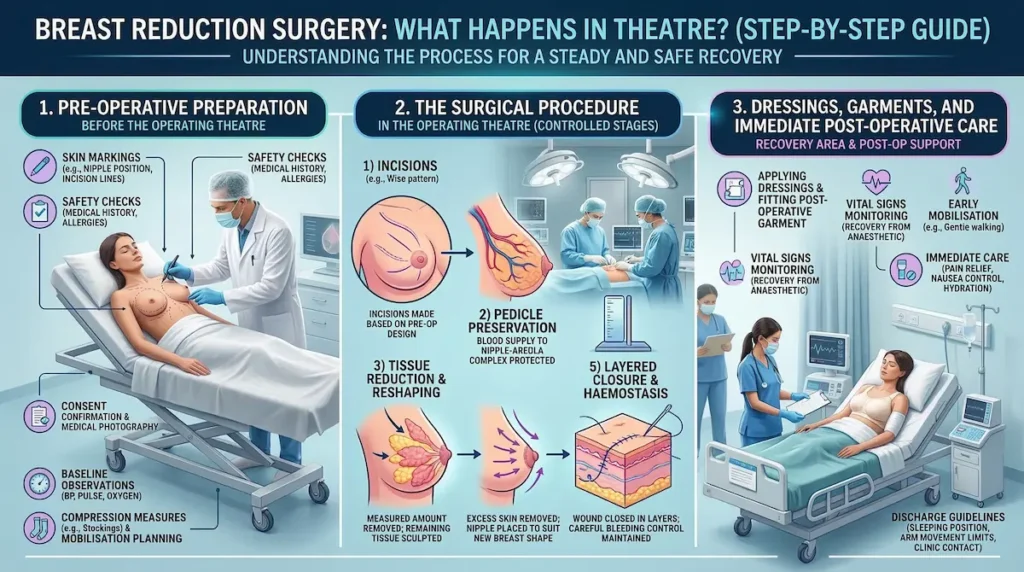
Breast Reduction Surgery Step-by-Step: What Happens in Theatre?
Understanding the process can reduce anxiety and help you plan realistically. While details vary by technique, most breast reductions follow a structured pathway from pre-operative markings to closure, dressings, and early monitoring. Below is an overview of what typically happens on the day of surgery.
Pre-op planning, markings, and safety checks
Before you go into the operating theatre, your surgeon will usually perform skin markings. These guide incision placement, nipple position planning, and symmetry goals. You will also go through standard safety steps, which may include:
- Review of your medical history, medication list, and allergies.
- Confirmation of the surgical plan and consent.
- Baseline observations (blood pressure, pulse, oxygen levels).
- Photography (where appropriate and agreed) for medical documentation.
- Compression measures and mobilisation planning based on clot-risk assessment.
This is also the moment to clarify practical questions: garments, showering, sleeping position, and the first follow-up timing.
Surgical steps (resection, reshaping, lift, closure)
Once anaesthesia is established and you are positioned safely, the operation proceeds in carefully controlled stages. While exact steps depend on whether an anchor (Wise pattern), vertical (lollipop), or other approach is chosen, the core principles are consistent:
- Incision and access: incisions are made according to the pre-operative design.
- Pedicle preservation: the nipple–areola complex is kept attached to a planned tissue “pedicle” to protect blood supply and support sensation where possible.
- Tissue reduction: a measured amount of glandular tissue and fat is removed to reduce weight and volume.
- Reshaping: the remaining tissue is sculpted to form a stable breast mound with natural contour and projection.
- Skin tailoring: excess skin is removed and the envelope is tightened to support the new shape.
- Repositioning: the nipple–areola complex is placed to suit the new breast shape and height.
- Haemostasis: careful control of bleeding is maintained throughout to support safer recovery.
- Layered closure: closure is performed in layers to support healing and reduce tension on the skin.
Throughout the procedure, the priority is balance: achieving the planned reduction while preserving circulation, shaping for a natural result, and closing in a way that supports predictable healing.
Dressings, garments, and immediate monitoring
At the end of surgery, dressings are applied and you are typically fitted into a supportive post-operative bra or garment. You will then move to a recovery area where your care team monitors you closely as the anaesthetic wears off.
Immediate post-operative care commonly focuses on:
- Comfort (pain relief and nausea control).
- Early mobilisation when safe, to support circulation.
- Hydration and gradual return to light food intake.
- Instruction on sleeping position, arm movement limits, and garment use.
- Clear guidance on what is normal vs what should trigger a call to the clinic.
Your discharge plan should be structured and easy to follow. The first days are about protecting the incisions, minimising tension, and allowing your body to settle. The “best” recovery is rarely the fastest—it is the one that is steady, safe, and well-supported.
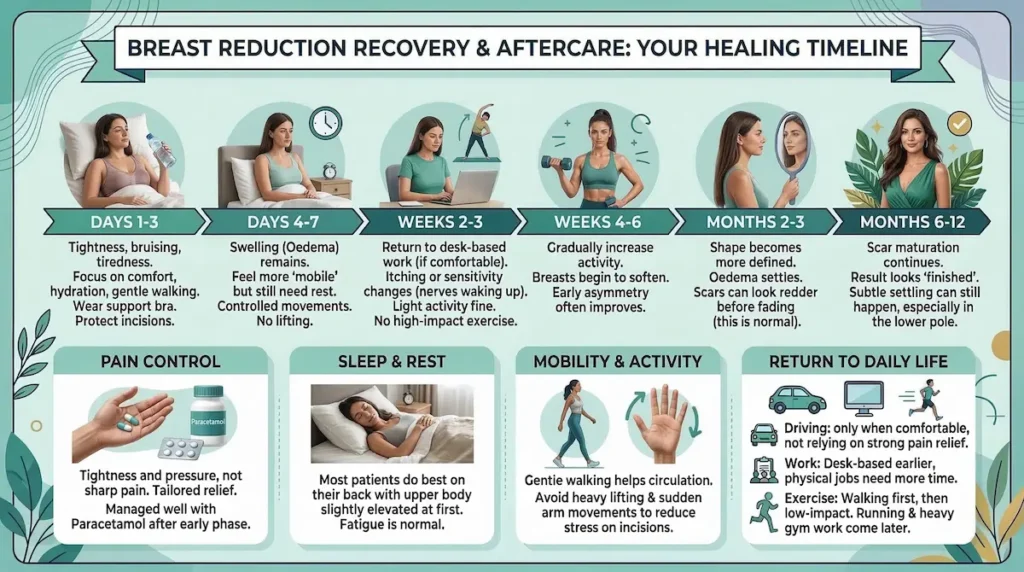
Breast Reduction Recovery & Aftercare: How Long Does Healing Take?
Recovery after Breast Reduction is a process, not a single milestone. You will feel better in stages. Swelling takes time to settle. We plan your aftercare around comfort, safety, and predictable healing.
Your timeline depends on the technique, the amount of reduction, your skin quality, and your lifestyle. A desk job and a physical job recover differently. So do smokers and non-smokers. We guide you through the phases with clear, practical steps.
Reduction mammoplasty recovery timeline (day-by-day to week-by-week)
Below is a realistic reduction mammoplasty recovery timeline. Use it to plan time off work, travel, and support at home. It is a framework, not a promise.
- Days 1–3: Expect tightness, bruising, and tiredness. We focus on comfort, hydration, gentle walking, and protecting the incisions. You will wear your support bra as instructed.
- Days 4–7: Swelling (oedema) is still present. Most patients feel more “mobile” but still need rest. Keep movements controlled and avoid lifting.
- Weeks 2–3: Many people return to desk-based work during this window, if comfort allows. You may feel itching or sensitivity changes as nerves begin to wake up. Light activity is usually fine. High-impact exercise is not.
- Weeks 4–6: You typically increase activity gradually, based on how your incisions look and how your body feels. Breasts begin to soften. Early asymmetry often improves.
- Months 2–3: Shape becomes more defined as swelling settles. Scars often look redder before they fade. This is normal.
- Months 6–12: Scar maturation continues and the result looks more “finished”. Subtle settling can still happen, especially in the lower pole.
Pain control, swelling (oedema), mobility, return to work
Most discomfort is pressure and tightness, rather than sharp pain. We tailor pain relief to you. For UK patients, we speak in familiar terms. Many people manage well with medication such as paracetamol once the early phase passes.
Swelling is normal. So is fatigue. Your body is diverting energy into healing. Gentle walking helps circulation, while heavy lifting and sudden arm movements can stress the incisions.
- Sleep: Most patients do best on their back with the upper body slightly elevated at first.
- Showering: We advise you when it is safe, based on dressings and incision status.
- Driving: Drive only when you can move comfortably and are not relying on strong pain relief.
- Work: Desk-based work is often possible earlier than active jobs. If your work is physical, plan more time.
- Exercise: Walking first. Then controlled, low-impact activity. Running and heavy gym work come later.
Our Rapid Recovery & Safety Protocol: HBOT + LLLT + structured follow-ups
After surgery, the priority is safe healing with minimal “social downtime”. We support that with a structured aftercare system, not guesswork. This is where our technology and follow-up model matters.
- HBOT (Hyperbaric Oxygen Therapy): We utilise HBOT as a strategic recovery intervention. It exposes you to 100% oxygen in a pressurised environment, supporting tissue oxygenation when post-surgical circulation is temporarily disrupted. The goal is stronger healing conditions and risk reduction.
- LLLT (Low-Level Laser Therapy): We use medical-grade low-level laser therapy to support cellular repair and collagen activity as part of scar and skin-healing care. It is an adjunct. It does not replace good surgery or good aftercare.
- High-touch monitoring: You are monitored closely in Istanbul during the early recovery phase. Your dedicated Patient Host is available 24/7 via WhatsApp for practical support.
- Long-term follow-up: We schedule structured virtual check-ins at 1, 3, 6, and 12 months to monitor healing and guide scar care over time.
That continuity is deliberate. Many international patients worry about being “on their own” once they fly home. We build aftercare to remove that fear.
Safety & Risks: Is Breast Reduction Dangerous?
Every operation carries risk. Breast reduction is generally safe in appropriate candidates, when planned carefully and supported by proper monitoring. Our job is to reduce avoidable risk through screening, sterile operating theatres, and vigilant post-op care. Your job is to follow the plan and speak up early if something feels wrong.
Normal early effects vs red flags
Not every symptom is a complication. Some changes are expected. The key is recognising patterns that require attention.
- Often normal early on: bruising, swelling (oedema), tightness, mild asymmetry, temporary numbness or hypersensitivity, low energy, mild itchiness as healing progresses.
- Red flags: rapidly increasing swelling on one side, sudden severe pain, active bleeding soaking dressings, fainting, chest pain, shortness of breath, or calf swelling.
If you experience red-flag symptoms, contact us immediately. If symptoms are severe or sudden, seek urgent medical attention.
Infection signs after breast reduction (what to watch for)
Most patients will not develop an infection, but you should know the warning signs. Early action makes management simpler.
- Increasing redness that spreads rather than settles.
- Warmth, worsening tenderness, or throbbing pain at the incision.
- Cloudy discharge, pus, or an unpleasant odour.
- Fever, chills, or feeling suddenly unwell.
- A wound that opens or becomes increasingly wet.
If you suspect infection, message us straight away. Do not “wait it out”. We will advise the safest next step based on your symptoms and timing.
Other risks: wound healing, fat necrosis, asymmetry, sensation changes
Breast reduction changes tissue structure and blood supply patterns. That is why technique choice and aftercare discipline matter. These are potential risks we discuss openly:
- Delayed wound healing: more likely with nicotine exposure, tension on incisions, or certain medical conditions.
- Wound separation: can happen at high-tension points, especially early if activity is too intense.
- Haematoma/seroma: bleeding or fluid collection that may require monitoring or intervention.
- Fat necrosis: small areas of fatty tissue can become firm as they heal. It may settle over time or need assessment.
- Changes in nipple sensation: often temporary, sometimes longer-lasting. Risk can increase with larger lifts.
- Scarring issues: thickened or raised scars can occur in genetically predisposed skin types.
- Asymmetry: we plan for balance, but natural anatomy and healing differences can influence the final result.
We do not minimise these topics. We manage them. A high-quality breast reduction is not only about the operating theatre. It is also about what happens after you leave it.
Breastfeeding and Future Pregnancy
One of the most common long-term questions is whether breast reduction affects breastfeeding and how pregnancy might change results. The honest answer is that breast reduction can influence breastfeeding potential, but the impact varies between individuals and depends on surgical technique, the amount of tissue removed, and how the ducts and nerves are preserved. Pregnancy and weight changes can also affect breast size and shape after surgery.
Breastfeeding after breast reduction (what can change, what can’t be promised)
Breastfeeding after breast reduction is possible for some patients, but it cannot be guaranteed. Breast milk production depends on the integrity of glandular tissue, milk ducts, and nerve signalling pathways. During breast reduction, tissue is removed and the nipple–areola complex may be repositioned. Even when a pedicle technique preserves blood supply and aims to protect nerve pathways, changes in anatomy can still reduce milk supply in some cases.
What we can do is plan responsibly and discuss your priorities clearly. If breastfeeding is a major future goal, tell your surgeon early. The operative plan can take this into account, but no ethical clinic should promise that breastfeeding will remain unchanged.
- Possible outcomes: normal breastfeeding, partial breastfeeding (supplementing), or difficulty producing sufficient milk.
- What helps: realistic expectations, technique selection based on anatomy, and good obstetric/lactation support when the time comes.
- What to avoid: assuming the outcome will be identical to pre-surgery function.
Pregnancy, weight change, and long-term breast shape
Breasts respond to hormonal changes, pregnancy, breastfeeding, and weight fluctuation. After reduction mammoplasty, you can still experience breast enlargement during pregnancy, and some stretching of the skin envelope can occur. This does not mean your surgery “failed”; it reflects normal biology. The degree of change varies and is influenced by genetics, skin elasticity, and the magnitude of weight or volume change.
In long-term planning, it helps to consider:
- Timing: If you plan pregnancy soon, you may choose to delay surgery, or proceed with a clear understanding that breast shape may change afterwards.
- Weight stability: Stable weight supports more stable results. Significant weight loss or gain can alter breast volume and skin quality.
- Ageing: Natural tissue laxity progresses over time. A well-planned reduction can age gracefully, but no breast remains “unchanged” forever.
Timing decisions: age, family plans, lifestyle
There is no perfect age for breast reduction. The right timing is personal: your symptoms, your lifestyle, your family plans, and your readiness for recovery all matter. If your current breast size is affecting daily comfort, activity, and quality of life, waiting indefinitely may not be realistic. Equally, if you have an imminent pregnancy plan, you may prefer to postpone or accept the possibility of future changes.
A good consultation will help you weigh these trade-offs calmly and make a decision you can stand behind long term.
Is Breast Reduction Safe in Turkey?
Safety is not determined by geography. It is determined by standards: surgeon expertise, facility protocols, anaesthesia management, sterile technique, and structured aftercare. For UK patients comparing options, the meaningful question is not “where is it?”, but “how is care delivered, monitored, and followed up?”
Facility standards, screening, and monitoring
Safe surgery starts before the operation itself. A proper pathway includes pre-operative assessment, clear instructions, and a plan for managing risk. In a well-run setting, you should expect:
- Pre-operative screening: a detailed medical history review, medication/supplement review, and appropriate investigations based on your profile.
- Anaesthesia oversight: an anaesthetist-led approach with continuous monitoring in theatre and recovery.
- Sterile operating theatre protocols: infection prevention is a system, not a slogan.
- Post-operative monitoring: observation after surgery, clear discharge criteria, and structured early follow-up.
International care should never feel “rushed”. You should have the time and clarity to understand your plan, your recovery, and who to contact if you need support.
Surgeon authority: European Board Certified expertise
For many patients, surgeon credentials are an essential trust signal—especially when travelling for care. When evaluating any clinic, look beyond marketing language and focus on demonstrable expertise, a consistent case portfolio, and a willingness to explain technique choice in plain terms. A high-quality surgeon can clearly justify why one incision pattern or pedicle is safer or more appropriate for your anatomy.
At AKM Clinic, breast procedures are led by surgeons described as European Board Certified, and consultations are designed to support the “expert patient” mindset: technique, risks, scars, and recovery are discussed with clarity, not glossed over.
The supported patient journey (VIP logistics + 24/7 host + clearance to fly)
Another safety factor for international patients is continuity of care. The concern is understandable: “What happens once I’m back in the UK?” A safe pathway includes clear planning in Istanbul and structured support after you return home.
- Travel and logistics support: coordinated transfers and accommodation planning can reduce stress and keep your early recovery practical.
- 24/7 communication: having a dedicated Patient Host available via WhatsApp can make it easier to raise concerns early rather than waiting.
- Clearance to fly: your return travel should be based on clinical assessment and your recovery status, not on a fixed calendar assumption.
- Remote follow-up: scheduled check-ins (for example at 1, 3, 6, and 12 months) help guide scar care, monitor symmetry settling, and address questions as healing progresses.
The goal is simple: your journey should feel medically supported from first consultation through to long-term healing, not like a one-off event. That is what turns international surgery from a “risk” into a planned, rational decision.
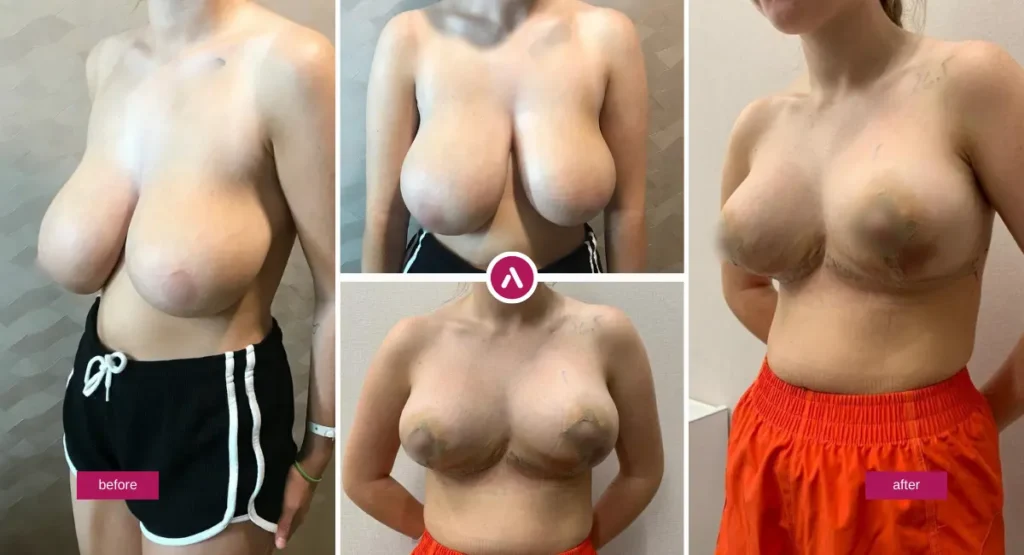
Breast Reduction Before and After: Realistic Expectations & Results
Breast reduction results are often life-changing in comfort, but the aesthetic result also evolves over time. Early on, swelling can mask shape, and scars can look more noticeable before they fade. The most reliable way to stay confident through recovery is to understand what “normal” looks like at each stage.
When results look “final” (settling timeline)
Most patients notice immediate relief from heaviness, but the visual outcome develops in phases:
- Immediately after surgery: The breasts look smaller and higher, but they may appear tight, swollen, and “set” higher on the chest.
- Weeks 2–6: Swelling gradually reduces. Bruising fades. Breasts begin to soften. Mild asymmetry is common and often improves.
- Months 2–3: Shape becomes more natural as tissues relax. The lower pole may “settle” slightly (this can be part of normal shaping).
- Months 6–12: Scar maturation continues and the breast contour looks more stable and finished.
It is normal to have days when you feel delighted and days when you feel uncertain—especially in the first 6–8 weeks. This is why structured follow-up and clear guidance matter.
Scar maturation and long-term maintenance
Scars are a predictable part of breast reduction. The goal is not “no scars”, but scars that heal cleanly and fade well over time. Scar appearance changes through stages:
- Early phase: Scars can look red, raised, or firm as collagen builds.
- Middle phase: Scars often soften but may still be pigmented or noticeable.
- Maturation phase: Many scars fade and flatten over 6–12 months (sometimes longer).
Long-term scar quality is influenced by genetics, skin type, nicotine exposure, and how much tension the incision experiences during early healing. Practical steps that commonly support better scar outcomes include:
- Wearing the recommended support bra/garment as advised.
- Protecting scars from sun exposure (UV can darken scars).
- Following a structured scar-care plan when appropriate (for example, silicone-based approaches).
- Avoiding early overexertion that places tension on incisions.
If you are prone to raised scars, tell your surgeon during consultation. It helps us plan both technique and aftercare strategies with more precision.
Natural, proportional outcome philosophy (“Rejuvenation, Not Alteration”)
A high-quality breast reduction should look like a natural version of you. That means:
- Proportion: Balance between bust, waist, and hips rather than a generic “target size”.
- Shape: A breast contour that sits naturally on the chest wall with realistic softness.
- Stability: A result that ages well, rather than an overly tight look that may not hold up as tissues settle.
We also discuss what breast reduction cannot do. It cannot stop the natural effects of ageing, pregnancy, or major weight fluctuation. The goal is improvement that feels rational and sustainable.
Receive a 100% transparent, all-inclusive quote tailored to your needs. No hidden fees—just world-class care at an accessible price.
Breast Reduction Surgery Cost 2026 Turkey vs UK: Value, and What’s Included
Cost is rarely the only deciding factor for Breast Reduction. UK patients usually want two things at once: clinical confidence and a rational cost. That is exactly how we frame it. Value is the full pathway—screening, surgery, anaesthesia, recovery support, and follow-up—not a headline figure.
Breast reduction cost UK vs Turkey: why the difference exists
When patients compare breast reduction cost UK vs Turkey, the gap often looks surprising. In practice, the difference is typically driven by macroeconomics and operational costs, not by “cutting corners”. Exchange rates, staffing costs, and facility overheads can shift the baseline cost of care between countries.
- UK private pricing is influenced by higher operational costs and the structure of the private hospital system.
- Turkey pricing can be more cost-effective due to different national operating costs and currency dynamics.
- What matters most is what is included, how you are monitored, and how aftercare is delivered once you return home.
A sensible comparison is not “cheapest vs most expensive”. It is “like-for-like”: surgeon credentials, accredited facility standards, anaesthesia oversight, and a defined aftercare plan.
All-inclusive breast reduction Turkey: what our VIP package covers
Many patients worry about hidden extras. We remove that uncertainty with a transparent, all-inclusive model. It keeps planning simple and protects you from the “surprise invoice” problem.
| What’s included | What’s not included |
|---|---|
| Your complete surgical procedure Anaesthesia & operating room fees All pre-operative tests 5-star hotel accommodation All VIP airport & clinic transfers Your 24/7 dedicated Patient Host All post-operative medications & garments First post-op meal Long-term virtual follow-up care | Your international flight tickets Personal travel insurance Personal expenses (e.g., meals, excluding the first post-op meal) Additional hotel nights (if you extend your stay) Visa fees (if applicable) |
If you are comparing providers, ask one simple question: “Is this an all-inclusive clinical pathway, or a base fee with layers of add-ons?” Clarity matters.
How to judge “value-for-money” without guessing
Cost comparisons work best when you anchor them to safety and predictability. Here are the questions we encourage patients to ask—of any clinic, anywhere:
- Who leads the surgery, and are they European Board Certified Surgeons or registered with recognised international boards?
- Where does the operation take place, and what standards are used for monitoring and infection prevention?
- What is the aftercare plan in the first 72 hours, and who answers messages outside office hours?
- Is there structured follow-up after you return to the UK?
When the answers are clear, the decision becomes logical. No drama. No sales pressure.

Finding the Best Breast Reduction Surgeon
“Best” is not a marketing label. For UK patients, the safest way to find the right Breast Reduction surgeon is to look for transparent decision-making, measurable standards, and a clearly structured aftercare pathway. A high-quality surgeon will not rush you into a date or promise a specific cup size. Instead, they will explain how your anatomy drives the plan: incision pattern, pedicle choice, scar strategy, and recovery milestones.
What to look for (beyond before-and-after photos)
- Credentials and accountability: Seek surgeons with recognised board-level training (for example, European Board Certified expertise), and clinics that can explain who will perform your operation and who supervises anaesthesia.
- Technique fluency: A reliable surgeon can explain Wise pattern (anchor) vs vertical (lollipop) options, and the logic of pedicle choices (such as inferior pedicle or McKissock) in plain language—matched to your breast size, skin quality, and nipple position.
- Realistic scar counselling: Expect an honest discussion about scars, scar maturation, and what influences healing (including nicotine exposure and tension points).
- Safety systems: Ask about pre-operative screening, sterile operating theatre protocols, and how red flags are handled (for example, infection signs or sudden swelling).
Questions to ask in your consultation
- Which technique is most suitable for my anatomy, and why?
- What are the key risks in my case, and how do you reduce them?
- What does my recovery timeline look like week by week?
- How will follow-up work once I return to the UK?
If the answers are clear, consistent, and pressure-free, you are likely in the right place.
From VIP airport transfers to 5-star hotel accommodation, we manage every detail. Enjoy a premier medical travel experience in Istanbul.
Your Medical Journey for Boob Reduction: Booking & Travel Planning
Once you decide to proceed with Breast Reduction, the next question is practical: “How does this work from the UK?” Our pathway is built to reduce friction. We keep the process structured, supported, and predictable from the first call to your long-term follow-up.
Free virtual consultation & planning your date
Your journey starts with a no-obligation virtual consultation. You share your goals and relevant information, and we review candidacy, technique options, and the recovery plan. If you choose to proceed, we secure your surgery date and begin the VIP planning.
Arrival, hotel, and VIP transfers
Travelling for surgery is easier when logistics are handled properly. Your Patient Host coordinates hotel and transfers so you can focus on preparation and rest. On arrival, you are met at the airport and transferred to your hotel in a private vehicle.
- 5-star partner hotel planning
- VIP airport and clinic transfers
- A single point of contact for scheduling and day-to-day coordination
Post-op support, clearance to fly, and long-term follow-up
After surgery, you are monitored closely by the medical team during your recovery in Istanbul. Your Patient Host remains available 24/7 via WhatsApp for support and practical guidance. Before you leave, you have a final in-person check-up to confirm you are recovering well and cleared to fly home.
Care continues after you return to the UK. We schedule virtual follow-ups at 1, 3, 6, and 12 months to monitor healing, guide scar care, and answer questions as your result settles.
Breast Reduction Surgery Frequently Asked Questions (FAQ):
Wise pattern vs vertical reduction: which leaves less scarring?
In general, a vertical (lollipop) approach can reduce scar length compared with a Wise pattern (anchor), but it is not suitable for every anatomy. Wise pattern techniques can offer stronger control for larger reductions or significant skin excess. The best choice is the one that safely achieves your planned shape and stability with well-managed tension on the incisions.
What is bilateral reduction mammoplasty?
Bilateral reduction mammoplasty simply means breast reduction is performed on both breasts. Most breast reductions are bilateral, with careful planning to improve balance and symmetry.
How long is the reduction mammoplasty recovery timeline?
Most patients can return to desk-based work within around 2–3 weeks if recovery is uncomplicated, while more physical jobs may need longer. Shape continues to settle over 2–3 months, and scars mature over 6–12 months (sometimes longer). Your personal timeline depends on technique, health factors, and activity level.
When can I sleep on my side after breast reduction?
Most patients are advised to sleep on their back initially to reduce pressure and protect healing incisions. Side-sleeping is usually introduced gradually once tenderness and swelling reduce and your surgeon confirms it is appropriate for your healing stage.
When can I shower after surgery?
Showering guidance depends on your dressings and incision status. We provide a clear plan after surgery, including when you can shower safely and how to protect incisions. Avoid soaking (baths, swimming pools, hot tubs) until you are medically cleared.
What are infection signs after breast reduction?
Warning signs can include spreading redness, increasing warmth, worsening tenderness or throbbing pain, cloudy discharge or unpleasant odour, fever/chills, or a wound that becomes increasingly wet or opens. If you suspect infection, contact the clinic promptly rather than waiting.
Will I lose nipple sensation?
Sensation changes can happen after breast reduction. Many patients experience temporary numbness or hypersensitivity while nerves recover. In some cases, sensation changes can be longer-lasting—risk can increase with larger lifts or more complex anatomy. We discuss this openly during consultation.
Can I breastfeed after breast reduction?
Breastfeeding after breast reduction can be possible, but it cannot be guaranteed. Outcomes vary depending on anatomy, technique, and how ducts and nerve pathways are affected. If breastfeeding is a priority, tell your surgeon early so this can be considered in the surgical plan.
Will breast reduction fix back pain?
Many patients report significant improvement in comfort, posture, and daily strain after surgery. However, back pain can have multiple causes (posture, spine issues, muscular imbalance). Breast reduction can reduce mechanical load, but no clinic should promise that it will “cure” all pain.
Does the NHS cover breast reduction? What are NHS breast reduction criteria?
NHS access varies by region and is often based on strict criteria that may include symptom documentation and health factors such as BMI. Many patients explore private options if they do not meet local criteria or do not want to wait. A consultation can clarify your candidacy and the safest pathway for you.
Breast reduction cost UK vs Turkey: why is it different?
Differences are often driven by operational costs and broader economic factors rather than quality. The meaningful comparison is “like-for-like”: surgeon expertise, facility standards, anaesthesia oversight, aftercare structure, and long-term follow-up—not a headline number.
What does an all-inclusive breast reduction Turkey package usually include?
All-inclusive packages typically bundle core medical costs (surgery, anaesthesia, tests) and may include accommodation and transfers. Always ask for a written breakdown of what is included and what is excluded (such as flights, insurance, extra hotel nights, or personal expenses) to avoid surprises.
How do I choose the best breast reduction surgeon in Turkey?
Focus on safety signals and transparency: clear explanation of technique selection (Wise/Vertical/Benelli and pedicle logic), realistic scar counselling, robust before/after planning, an anaesthetist-led approach, sterile facility protocols, and structured follow-up once you return to the UK.
When can I fly home after breast reduction in Istanbul?
Return travel should be based on clinical assessment and how you are healing, not an arbitrary date. We confirm clearance to fly through an in-person check-up and provide guidance for a safe journey and early aftercare once you are back in the UK.
Medical Disclaimer: This page is provided for general information only and does not constitute medical advice. A consultation with a qualified clinician is essential to determine whether breast reduction is appropriate for you, and to discuss risks, benefits, and alternatives based on your medical history. If you develop urgent symptoms (such as chest pain, shortness of breath, fainting, or rapidly increasing swelling), seek immediate emergency medical care.
Breast Reduction: Patient Stories

Lisa


Laura

Breast Reduction Surgeons
Breast Reduction Cost in Turkey
Starting from ~ £3000
* There are no hidden fees or unexpected charges.
- Your PersonalisedBreast ReductionProcedure
- All Specialist Surgeon & Anaesthesia Fees
- All Pre-Op Tests & Post-Op Check-ups
- 5-Star Hotel Accommodation (incl. breakfast)
- All Private VIP Airport & Clinic Transfers
- 24/7 Dedicated Patient Coordinator & Translation Services
Breast Reduction: A Cost Comparison
| City | Cost |
|---|---|
| London | ~ £11,000 GBP |
| Bristol | ~ £10,500 GBP |
| Edinburgh | ~ £10,000 GBP |
| Manchester | ~ £10,700 GBP |
| Belfast | ~ £10,000 GBP |
Breast Reduction: Patient Reviews
Jammal Canada
I have had face and neck lift with AKM Clinic they have been so good to me and my operation went so smoothly🥰 i would like to thank my doctor here and also to the team 💐

Ava Canada
Thank you AKM Clinic for giving me my confidence back! Had facelift + temporal lift 3 months ago and the outcome is already stunning. Special thanks to Hande!

Jakayla USA
Had a deep plane facelift and lower eyelid procedure at AKM Clinic 7 months ago. The results are fantastic - very subtle and natural. I didn’t expect the entire experience to be so comfortable. Hande managed everything and kept in contact even after I returned to USA. I’m beyond pleased with the outcome and the care I received. Would do it again in a heartbeat!

Barbara United Kingdom
It has been 4 months since my surgery. Everything is great, The most important thing is l love the way l look, l look exactly how l wanted. Meaning l look natural, just almost 40 years younger. I pulled Facebook - majority voted 37ys. I also had face, neck, chest, and hands CO2 laser. My skin is flawless.

Lisa Canada
I had a face, neck and arm lift at AKM. I’m just over 4 weeks post and couldn’t be happier with the results. The entire experience was wonderful! My coordinator, Khadija made me feel comfortable from beginning to end! I highly recommend AKM and will definitely go back for other procedures!

Julie USA
I am beyond grateful I went with AKM Clinic for my deep plane face and neck lift, upper eyelid, and co2 laser. Dr. Akif has magic hands and my results are truly incredible! I came from the US and assistant Emine was the best in assuring every detail was coordinated and communicated with me beyond my expectations every step of the way. 10 out of 10 to the entire team! I couldn’t be more pleased!

Ready to Begin Your Own Transformation Journey?
Join the 2,000+ patients who have trusted Dr Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, naturally restored you begins with a simple, no-obligation conversation. Contact us today from the UK for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. There are no hidden fees.
#2: Secure Your Date & VIP Booking
Once you are ready, our dedicated patient coordinators will help you secure your procedure date. We will handle all your bookings, including your 5-star hotel accommodation and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you will meet your specialist surgeon to finalise the details for your natural, subtle, and restored new look.













