Upper Back Lift in Turkey




- Upper Back Lift smooths bra-line rolls by removing excess skin for a natural upper-back contour.
- Safety-first planning includes suitability screening, scar strategy, and structured follow-up for UK patients.
- Recovery support features clear timelines and optional HBOT + LLLT to aid healing where appropriate.
- Transparent value compares UK vs Turkey upper back lift costs with all-inclusive care, logistics, and aftercare clarity.
AI-generated summary, fact-checked by our medical experts.
Upper Back Lift: Quick Facts
Duration of Surgery
Type of Anaesthesia
Initial Recovery Period
Hospital Accommodation
Return to Daily Activities
Upper Back Lift Results: Before and After
Considering an Upper Back Lift to smooth bra-line rolls? Our Istanbul team explains techniques, scar placement and whether awake/twilight anaesthesia is suitable, with clear expectations for UK patients seeking natural contour refinement after weight loss or ageing done safely abroad.
You’ll learn who is a candidate, how recovery typically progresses, and how we support healing with structured aftercare, including HBOT and LLLT where appropriate. Explore costs, risks, and follow-up from consultation to flight-ready recovery, step by step for UK patients.
Table of Contents
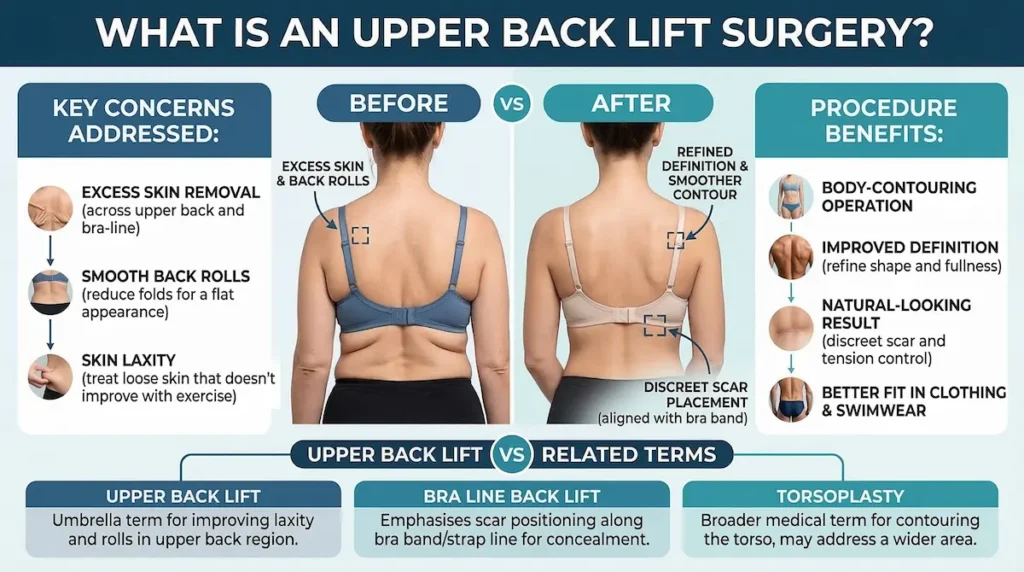
What is an Upper Back Lift Surgery?
An Upper Back Lift is a body-contouring procedure that removes excess upper-back skin—often concentrated along the bra line—to smooth back rolls and refine definition. It focuses on lift direction, tension control, and discreet scar placement for a natural-looking result in clothing and swimwear.
Definition (quick answer)
An Upper Back Lift is a body-contouring operation designed to remove excess skin and refine fullness across the upper back—often around the bra-line area—creating a smoother, more defined contour. It is commonly chosen after significant weight loss or when skin laxity forms persistent rolls that do not respond to exercise.
What area does it treat: upper back vs bra-line zone
In real-life anatomy, the “upper back” concern is often concentrated around the bra-line—the band area where skin and soft tissue can fold or gather. Over time (or after weight changes), the skin may lose elasticity and “hang” in a way that creates a visible ridge under fitted clothing, swimwear, or bras.
An Upper Back Lift focuses on:
- Excess skin removal across the upper back and bra-line region.
- Contour refinement by re-draping the skin to reduce rolls and improve definition.
- Scar placement planning to keep the final scar as discreet as possible—often aligned with where a bra strap or band naturally sits (depending on your anatomy and surgical plan).
Because this region moves with the shoulders and upper torso, the plan must balance a meaningful lift with tension control. That is why an Upper Back Lift is not simply “skin trimming”; it’s a structured contouring procedure with a deliberate strategy for lift direction, tissue handling, and closure.
Upper Back Lift vs Bra Line Back Lift vs Torsoplasty
You may see several terms used online, and they can overlap:
- Upper Back Lift is the patient-friendly umbrella term for improving laxity and rolls in the upper back region.
- Bra Line Back Lift typically emphasises scar positioning so the incision line can be concealed by a bra band/strap line (where appropriate).
- Torsoplasty is a broader medical term describing contouring procedures of the torso. Some torsoplasty techniques address a wider area than the upper back alone and may be discussed when there is more extensive laxity.
During consultation, the key is not the label but the pattern of laxity (where the excess sits) and the best lift vector (the direction the tissue needs to be repositioned). A precise plan is what creates a natural result and a scar that sits where you can live with it.
Our surgical dates fill up quickly due to high international demand. Secure your consultation today to arrange your preferred travel dates.
Why Does Upper-Back Skin Loosen In The First Place?
Upper-back skin laxity commonly follows significant weight loss, ageing, and reduced skin elasticity. The bra-line area is a frequent “hotspot” because it creases under compression and movement. When true redundant skin is present, exercise can improve tone but cannot reliably tighten excess skin.
Weight loss, ageing, and the “elasticity gap”
Skin is designed to stretch and recoil, but it does not always return to its original shape—especially after substantial, repeated, or rapid changes in body size. Following significant weight loss, the underlying volume reduces faster than the skin can contract, leaving an “elasticity gap” that becomes most noticeable in areas that naturally crease, such as the bra-line and upper back.
Ageing can amplify this effect. Over time, skin support structures naturally change, and the upper back may show laxity sooner than expected—particularly when the tissue has been stretched previously or the skin quality is compromised.
Genetics, skin quality, and why the bra-line is a common hotspot
Two people can have the same lifestyle and weight history yet develop very different patterns of laxity. That’s because genetics and skin quality matter: baseline elasticity, collagen density, and how your skin responds to stretching all influence whether the upper back tightens on its own.
The bra-line area is a common “hotspot” because it is:
- A natural compression point (bra band/strap pressure can accentuate folding in this region).
- A high-movement zone (shoulder and torso motion can encourage creasing).
- Structurally complex (skin, fat distribution, and fascial support vary person to person).
This is also why non-surgical measures—while helpful for general fitness and skin care—cannot reliably eliminate true excess skin. Exercise strengthens muscle, but it cannot “shrink” redundant skin beyond what your skin biology allows.
It’s not always “just skin”: tissue distribution and contour dynamics
Upper back concerns often involve a combination of skin laxity and soft-tissue distribution. Some patients have a distinct “back bra bulge” created by where the body stores fat and how the skin drapes over it. Others have minimal fat but significant skin redundancy, especially after weight loss.
That distinction matters because it influences the surgical approach and whether a combined strategy is appropriate. In many cases, the best plan is not simply removing skin—it is repositioning and re-draping tissue in a way that looks smooth in real life (not only when standing still) and that respects scar placement and tension.
The most reliable way to determine the cause of your upper-back contour is a personalised assessment, including a review of skin quality, laxity pattern, and how the tissue behaves with movement. From there, the procedure plan can be tailored to your anatomy and priorities.

Symptoms & Functional Complaints: when it feels more than cosmetic
Many patients describe irritation, rubbing, and discomfort from bra-line folds, plus frustration with clothing fit. However, pain when lifting arms or clicking sensations often relate to shoulder or musculoskeletal causes. An Upper Back Lift targets contour and excess skin—not a substitute for medical assessment.
“Upper back hurts when I lift my arms” — what it may mean (and what it usually doesn’t)
Some people searching for an Upper Back Lift describe discomfort when raising their arms or reaching overhead. It’s understandable to wonder whether upper-back skin laxity or bra-line folds are “pulling” or contributing to an uncomfortable sensation—particularly if the tissue feels heavy, rubs under clothing, or becomes irritated with movement.
However, pain with arm lifting is far more commonly linked to the shoulder, neck, spine, or muscular structures than to excess skin alone. Aesthetic surgery is designed to improve contour; it is not a primary treatment for musculoskeletal pain. If your main concern is pain (rather than skin redundancy), the safest route is to speak with your GP or a qualified clinician for an appropriate assessment before considering surgery.
“Back pain, can’t lift arms” — red flags and when to seek medical advice
If you experience back pain alongside a reduced ability to lift your arms, it’s important to treat this as a health concern first. In many cases, the cause is benign (for example, muscle strain or posture-related issues), but there are situations where you should seek prompt clinical advice.
Please contact a healthcare professional urgently if you have:
- Sudden or severe pain that does not improve.
- Numbness, tingling, or weakness in the arms or hands.
- Loss of coordination or difficulty walking.
- Fever, unexplained weight loss, or pain that wakes you at night.
- Recent trauma (fall, impact injury) followed by persistent symptoms.
Where an Upper Back Lift can be relevant is when your “functional” complaint is primarily about comfort in clothing, persistent skin irritation, friction, or feeling restricted by the way excess tissue folds and moves. In those cases, surgery may address the contour issue—while still keeping expectations realistic about pain outcomes.
“Clicking/clunking” sensations — why a cosmetic consultation should be careful here
Searches such as “Why does my back click/clunk when I lift my leg?” often reflect concerns that are orthopaedic or biomechanical rather than cosmetic. Clicking can be related to joints, tendons, spinal mechanics, or muscular imbalance. It is not a typical symptom caused by upper-back skin laxity.
If you notice clicking accompanied by pain, weakness, or restricted movement, a targeted medical evaluation is recommended. From an aesthetic perspective, the key role of an Upper Back Lift consultation is to:
- Clarify whether the primary issue is skin redundancy and contour.
- Identify when symptoms suggest a non-cosmetic diagnosis that should be assessed first.
- Ensure your plan prioritises safety, suitability, and realistic outcomes.
In short: if your concerns are mainly about how your upper back looks and feels in daily life (clothing fit, rubbing, visible rolls), an Upper Back Lift may be appropriate. If your concerns are mainly pain or mechanical symptoms, treat those as a medical issue first.
Share your photos and medical history to receive a personalised assessment from our European Board-certified facial surgery team.
Benefits: What Changes After An Upper Back Lift?
The main benefit of an Upper Back Lift is a smoother bra-line contour with reduced back rolls, improving how bras, sportswear, and fitted tops sit. Many patients also feel more comfortable due to less folding and friction. Results are designed for natural proportion, not an “overdone” look.
A smoother bra-line contour (especially in fitted clothing)
The most noticeable change after an Upper Back Lift is typically a cleaner, smoother upper-back profile. Patients often report that the bra-line area looks less “bunched” and that upper-back rolls are reduced, particularly in:
- Bras and sportswear that previously highlighted folds.
- Fitted tops and dresses where the upper back is visible.
- Swimwear where bra-line bulges can be more apparent.
Because the procedure is designed around the anatomy of the bra-line region, the goal is a result that looks natural in real life—standing, sitting, and moving—not just in one posed position.
Improved comfort for day-to-day wear
While an Upper Back Lift is a cosmetic procedure, some people find they feel more comfortable afterwards because there is less excess tissue to rub, fold, or irritate the skin. Potential comfort-related improvements may include:
- Less friction and chafing where skin folds meet.
- Better bra fit with less “spillage” at the back band line.
- Greater ease choosing clothing without needing to “dress around” the upper back.
It’s important to frame this correctly: the procedure aims to refine contour and reduce redundant skin. If you have pain, numbness, or significant functional limitation, these should be evaluated medically rather than assumed to be solved by aesthetic surgery.
Confidence and proportion (rejuvenation, not alteration)
For many patients—especially after weight loss—upper-back laxity can feel like the “last reminder” that the body hasn’t caught up with their progress. By removing redundant skin and refining the contour, an Upper Back Lift can help you feel that your shape better matches your efforts.
Our philosophy is rejuvenation, not alteration: the aim is not to create an artificial look, but to restore smoother lines and proportion, with scar planning that is transparent and realistic.
What it won’t do (setting realistic expectations)
Clear expectations are a major part of achieving a satisfying outcome. An Upper Back Lift generally will not:
- Replace a medical work-up for shoulder/neck/back pain.
- Eliminate all skin texture changes (for example, stretch marks may improve in the excised area but won’t disappear everywhere).
- Guarantee a “scar-free” result—there will be a scar, and the plan focuses on placing it as discreetly as possible and supporting good scar maturation.
When the procedure is chosen for the right reasons—excess skin, bra-line rolls, and contour concerns—the benefits can be highly meaningful and long-lasting.
Answer a few brief questions about your concerns, health, and goals to discover which treatment options may suit you best.
Am I a Suitable Candidate for Upper Back Lift?
You may be suitable if you have persistent upper-back or bra-line skin excess despite stable weight and good overall health. Ideal candidates are non-smokers (or able to stop nicotine), with realistic scar expectations and a clear contour goal. Suitability depends on laxity pattern, skin quality, and safety screening.
Who tends to benefit most from an Upper Back Lift
You may be a good candidate for an Upper Back Lift if you have noticeable excess skin (often forming rolls at the bra-line) that persists despite stable weight, exercise, and general skin care. This procedure is most commonly considered by people who:
- Have experienced significant weight loss (including post-bariatric patients).
- Have upper-back laxity related to ageing and reduced skin elasticity.
- Feel self-conscious about visible back rolls in clothing, lingerie, or swimwear.
- Experience friction or irritation where skin folds rub—particularly in warmer weather or during exercise.
In consultation, we focus on the pattern of laxity (where the excess sits), the quality of the skin, and how your tissue behaves with movement. These details determine whether an Upper Back Lift alone is appropriate, or whether a broader torso contouring plan (such as torsoplasty) makes more sense.
Key suitability factors we assess (and why they matter)
Because scar placement and tension control are critical in the upper back, suitability is not just about “how much skin” you have. We typically assess:
- Weight stability: results are usually most predictable when your weight has been stable for several months.
- Skin quality: thin, fragile, or very stretched skin may influence scar behaviour and technique choice.
- Health status: conditions affecting healing (such as poorly controlled diabetes) can increase risk.
- Smoking/vaping: nicotine can impair circulation and wound healing; stopping well in advance is often advised.
- Medication and clot risk: some medicines and medical histories require careful planning and peri-operative risk reduction.
We also discuss what “success” looks like for you: scar concealment priorities, clothing goals, how you wear bras/swimwear, and whether you are open to combining procedures (if clinically appropriate).
Who should postpone or avoid surgery
An Upper Back Lift may not be appropriate right now if you are:
- Currently losing weight rapidly, or planning major weight changes (including pregnancy).
- Unable to stop nicotine use (smoking, vaping, nicotine replacement) for the recommended period.
- Managing a medical condition that is not well controlled (for example, blood sugar issues), or you have an active infection.
- Looking primarily for pain relief for shoulder/neck/back symptoms without a clear contour concern.
- Expecting a “scar-free” outcome (there will be a scar; the plan is to place and manage it responsibly).
Suitability is always individual. A proper assessment is essential to align your goals with the safest plan and the most realistic outcome.
Your consultation checklist (to get the most accurate plan)
To build a precise surgical plan, it helps to come prepared with:
- Photos (front/back/side) or a short video showing the area in motion, if your consultation begins online.
- Your weight history (including major changes), and any previous surgery details.
- A full list of medications and supplements, plus relevant medical history.
- Your priorities: scar concealment, clothing goals, and whether you would consider combining procedures.
The aim is a plan tailored to your anatomy—not a one-size-fits-all approach.
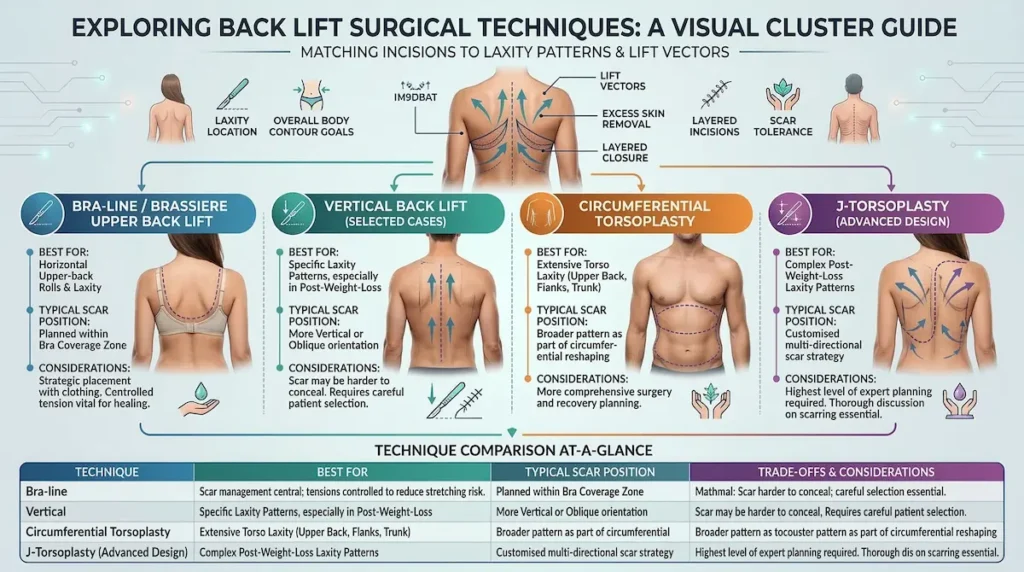
Back Lift Surgical Techniques Explained (Technique Cluster)
Technique selection depends on where laxity sits and how it moves. A bra-line approach can place scars within typical coverage zones, while vertical or more extensive torsoplasty options may suit broader post-weight-loss laxity. The goal is controlled lift vectors, layered closure, and predictable healing with a tailored scar strategy.
Bra-line (brassiere) approach: why scar placement is planned, not guessed
When patients search for a “bra-line back lift”, they are usually focused on one thing: where the scar will sit. A bra-line (or “brassiere”) approach is designed so the incision can often align with the natural coverage zone of a bra band or strap line—depending on your anatomy, how you wear bras, and the amount of lift required.
This approach can be particularly useful when the laxity concentrates across the upper back in a horizontal pattern. The surgical goal is to remove redundant skin and re-drape tissue so the contour looks smoother in everyday clothing, while keeping scar planning transparent and realistic.
Vertical Back Lift Surgery vs circumferential torsoplasty: the lift vector matters
Different incision orientations create different “lift vectors” (the direction tissue is tightened and repositioned). In simplified terms:
- Horizontal (bra-line) patterns often target rolls across the upper back and aim to smooth the bra-line contour.
- Vertical approaches may be discussed when laxity extends in a way that benefits from tightening along a different axis, particularly in selected post-weight-loss patterns.
- Circumferential torsoplasty is broader and may be considered when contour concerns extend beyond the upper back into a more comprehensive torso reshaping plan.
There is no single “best” technique for everyone. The right approach depends on where the excess sits, how much skin needs to be removed, your scar tolerance, and whether the goal is isolated upper-back refinement or wider torso contouring.
Our surgical dates fill up quickly due to high international demand. Secure your consultation today to arrange your preferred travel dates.
Circumferential torsoplasty and J-torsoplasty: when more advanced reshaping is considered
Torsoplasty is a broader medical term that can include different methods of torso contouring. In some cases—particularly after significant weight loss—upper-back laxity is part of a larger pattern involving the flanks and trunk. When that happens, a more comprehensive plan may be discussed.
J-torsoplasty is a term used for specific incision designs intended to address complex laxity patterns. These are typically considered when a straightforward bra-line approach would not deliver an adequate or balanced result. The benefit of advanced patterns is the potential for more comprehensive contouring; the trade-off is that scar design can be more involved and must be carefully planned.
Technique comparison table (at-a-glance)
| Technique | Best for | Typical scar position | Trade-offs to consider | Common combinations (when appropriate) |
|---|---|---|---|---|
| Bra-line / Brassiere Upper Back Lift | Upper-back rolls concentrated around the bra-line; horizontal laxity pattern | Across upper back, often aligned with bra coverage zone (anatomy dependent) | Scar management is central; tension must be controlled to reduce stretching risk | Selected liposuction for contour refinement; sometimes paired with arm contouring planning |
| Vertical Back Lift (selected cases) | Specific laxity patterns where a vertical tightening vector offers better correction | More vertical or oblique scar orientation (case dependent) | Scar can be harder to conceal in some clothing; careful selection is essential | May be part of broader post-weight-loss contouring strategy |
| Circumferential Torsoplasty | More extensive torso laxity (not limited to upper back) | Broader pattern as part of circumferential reshaping | More comprehensive surgery; recovery planning and aftercare become more involved | Often planned alongside other body contouring procedures, depending on needs |
| J-torsoplasty (advanced incision design) | Complex post-weight-loss laxity patterns needing tailored excision and lift | More customised scar design (may extend beyond a simple line) | Highest need for expert planning; scar strategy must be discussed in detail | Used within advanced torso contouring plans when clinically indicated |
How we decide the “right” technique for you
Choosing the technique is a balance of anatomy, goals, and risk management. In consultation we look at:
- Laxity map: where the skin is truly redundant, and where it is simply compressing or folding.
- Movement dynamics: how the tissue behaves when you sit, reach, and twist.
- Scar tolerance: what concealment means for your lifestyle (bra styles, swimwear, sportswear).
- Safety profile: health factors that influence wound healing and recovery planning.
The end goal is a result that is aesthetically refined, practical for real-life clothing, and planned around scar quality and long-term healing.
Receive a clear, day-by-day itinerary covering arrival, surgery, recovery, and fit-to-fly clearance tailored to your requirements.
Scar Strategy: Bra-Line Scars, Concealment, and Tattoo Questions
A scar is unavoidable, so we prioritise planning: placement, tension control, and aftercare. Bra-line scars can often be positioned for concealment, then supported with structured scar care as healing matures over months. If you’re considering a tattoo cover-up, it’s usually safest after full scar maturation.
Where the scar typically sits (and why bra-line planning matters)
An Upper Back Lift involves an incision, which means a scar is unavoidable. The key is scar planning: placing the incision where it is most likely to be concealed by your typical clothing—often along a bra-line coverage zone—while still achieving the lift you need.
During consultation, scar placement is discussed in practical terms, including:
- How you wear bras day-to-day (band height, strap position, sports bras vs underwired styles).
- Whether you prioritise concealment in swimwear or open-back clothing.
- The amount of skin that needs to be removed (more lift can mean a longer or differently positioned scar).
Because the upper back moves with shoulder and torso motion, we also plan the closure to manage tension—this can influence how the scar matures over time.
What “normal” scar healing looks like: a realistic timeline
Scars evolve. Early scars often look more noticeable before they improve. While every patient heals differently, a realistic pattern is:
- Weeks 0–6: the scar can look pink/red and feel firm or slightly raised as healing begins.
- Months 2–4: gradual softening; colour often starts to settle, though activity and tension can still affect the line.
- Months 6–12 (and beyond): continued maturation; many scars become flatter and less pigmented with time.
Scar quality is influenced by skin type, genetics, tension, aftercare consistency, and lifestyle factors (including nicotine use and sun exposure).
Scar minimisation: what we typically recommend (and what to avoid)
Good scar outcomes are a partnership between surgical planning and aftercare. Your clinician may recommend a scar-care plan tailored to you, which can include:
- Wound care and dressings in the early phase to protect the incision and reduce irritation.
- Silicone-based scar therapy (gel or sheets) once the incision is fully closed, if appropriate.
- Compression/support garments when advised, to help manage swelling and reduce stress on the closure.
- Sun protection for the scar area, as UV exposure can worsen pigmentation.
What to avoid: pulling or over-stretching the area early, returning to intense upper-body training too soon, and nicotine exposure (smoking/vaping) which can impair healing and increase complication risk.
“Can I cover it with a tattoo?” — practical guidance and timing
It’s common to see searches like “bra-line back lift tattoo” because patients want reassurance that scar concealment is possible. Tattooing over a surgical scar may be an option for some people, but timing and scar maturity matter.
As a general guide, most reputable tattoo artists and clinicians advise waiting until the scar is fully mature—often around 12 months—and sometimes longer depending on how the scar is healing. Tattooing too early can increase irritation, affect pigment uptake, and interfere with scar maturation.
If a tattoo is part of your long-term plan, mention it at consultation. Scar placement and aftercare can be discussed with that goal in mind, while keeping the priority on safe healing and a well-planned surgical result.
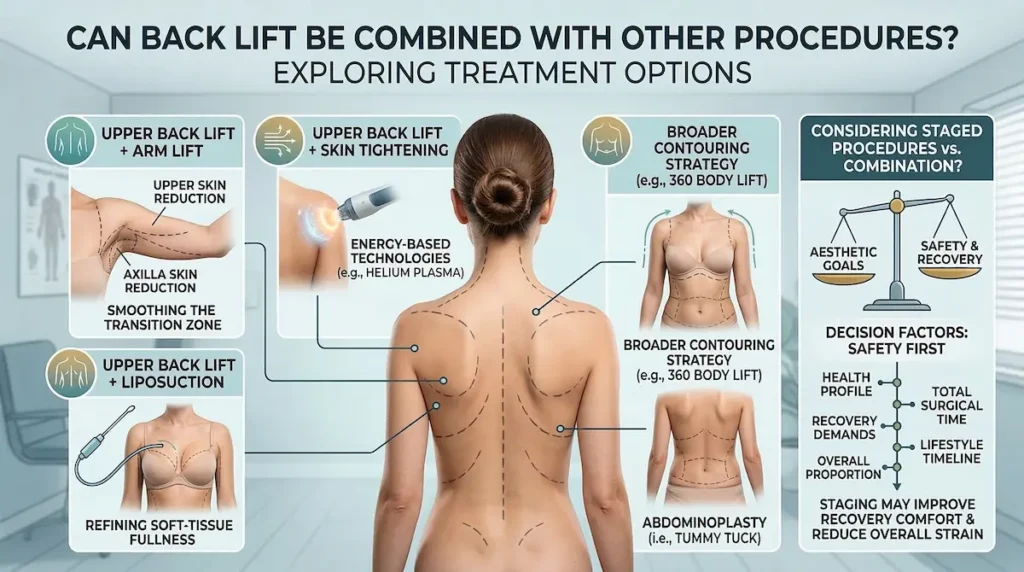
Can Back Lift Be Combined With Other Procedures?
Yes—an Upper Back Lift can be combined with procedures like an Arm Lift or selected liposuction when clinically appropriate, especially after weight loss. Combining can improve overall proportion across the upper torso, but it must be balanced against operating time and recovery demands. Sometimes staging procedures is safer.
Upper Back Lift + Arm Lift: smoothing the upper-torso “transition zone”
For some patients—particularly after weight loss—the concern is not isolated to the upper back. The area where the upper back meets the outer arm and underarm can create a visible “transition zone” that may benefit from a combined plan.
When clinically appropriate, combining an Upper Back Lift with an Arm Lift can help create a more harmonious contour across the upper torso. The decision depends on:
- Where the excess skin is most pronounced.
- How many incision lines you are comfortable with.
- Your overall health profile and ability to recover safely from a longer procedure.
Upper Back Lift + liposuction / skin tightening: when refinement is the goal
In selected cases, liposuction may be considered to refine soft-tissue fullness around the upper back or bra-line region. This is not a substitute for removing excess skin, but it can be helpful where there is a combined pattern of skin laxity + localised fullness.
Energy-based skin tightening (for example, helium plasma technologies often referred to as “J-Plasma”) may be discussed in specific situations, but it is not a guaranteed alternative to excision when true redundant skin is present. The safest plan is always based on what your tissue can realistically do.
Upper Back Lift within a larger body contouring plan (torsoplasty / 360 approach)
If your laxity extends beyond the upper back—into the flanks, mid-back, or lower torso—an Upper Back Lift may be one part of a broader contouring strategy. In post-weight-loss patients, this can sometimes involve a torsoplasty concept or a staged approach that may include procedures such as:
- 360 body lift (circumferential contouring, when indicated)
- Tummy tuck (abdominoplasty) for the abdominal component
- Additional areas (such as thighs or arms) depending on your priorities
Whether to combine procedures or stage them is an individual decision based on safety, operating time, recovery capacity, and your goals. In some cases, staging improves recovery comfort and allows each area to heal with less overall strain.
How we decide whether combining is right for you
The decision to combine procedures is never purely aesthetic—it is primarily a safety and recovery question. We consider:
- Your health profile, medical history, and anaesthetic suitability.
- The total surgical time and expected recovery demands.
- Your lifestyle timeline (return to work, travel planning, support at home).
- Whether a combined plan improves overall proportion—or simply adds unnecessary complexity.
A well-designed plan prioritises a stable, predictable result with a recovery you can realistically manage.
Anaesthesia: Why We Often Prefer Awake / Twilight Sedation
For many UK patients, the biggest worry is not the scar or the flight home. It’s the anaesthesia. We take that seriously, and we build your plan around both comfort and safety. When it’s clinically suitable, we often favour an “awake” approach with sedation rather than a full general anaesthetic.
What “awake” really means (and what it doesn’t)
“Awake” does not mean you are fully alert and anxious throughout surgery. It usually means we use local anaesthesia to numb the surgical area, alongside carefully managed sedation to keep you calm and comfortable. You can still be drowsy and relaxed, and many patients remember very little. Our priority is that you feel safe, stable, and well-supported from start to finish.
Twilight vs general anaesthesia: the practical differences
In UK search terms you may see “twilight” used for sedation-based surgery (conscious sedation). Twilight anaesthesia commonly refers to a level of sedation where you are sleepy and comfortable, without the same depth of unconsciousness as general anaesthesia. General anaesthesia can be the right choice in some cases, particularly for longer or more complex plans. We decide based on your medical history, procedure scope, and what is safest for you.
Why UK patients ask for conscious sedation (control, comfort, and recovery feel)
Some patients prefer sedation because they dislike the idea of being “fully put under”. Others have had a difficult experience previously and want a different approach this time. When sedation is appropriate, patients often describe a gentler overall experience, with less “grogginess” in the immediate recovery phase. We never oversell this; individual responses vary, and your safety always comes first.
Who may not be suitable for awake / twilight sedation
Not everyone is a candidate for sedation-based surgery. We may recommend general anaesthesia if the operative plan is extensive, if your airway or medical history suggests it is safer, or if anxiety is likely to make an awake approach uncomfortable. We also factor in previous reactions to anaesthetic medicines and any relevant GP or specialist input. The goal is a plan you can tolerate well, not a “one-size” protocol.
How we keep it safe: our anaesthesia decision process
We keep the decision structured and evidence-led. We review your medical history, medications, and any clot-risk factors, and we align the anaesthesia plan with the expected operating time. If you are travelling from the UK, we also plan around a sensible recovery window before you fly. Clear, conservative planning is the point.
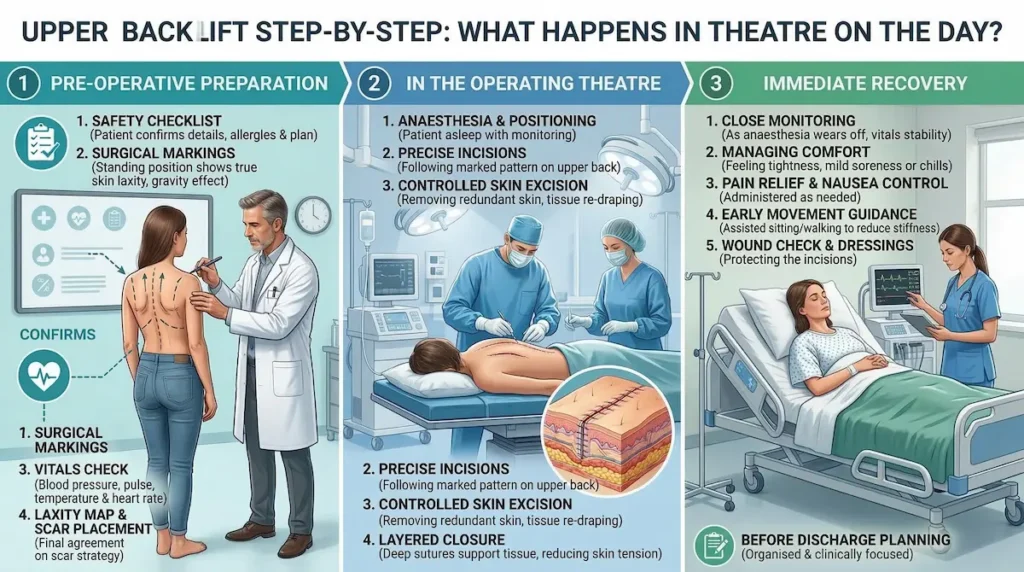
Upper Back Lift Step-By-Step: What Happens In Theatre On The Day?
Most people feel calmer when they know what the day will look like. We keep the process organised, predictable, and clinically focused. Your experience starts with final checks and markings, then moves into a sterile operating theatre environment. Throughout, we prioritise comfort, privacy, and clear communication.
Pre-op checks and surgical markings
On the day, we begin with a safety-first checklist. We confirm your medical details, allergies, and the agreed surgical plan. Your surgeon then performs precise markings while you are standing, because gravity shows the true pattern of laxity. This is also the moment to confirm scar placement preferences as realistically as your anatomy allows.
- Vitals check and final consent confirmation
- Skin assessment and “laxity map” review
- Markings designed for lift direction and scar strategy
In the operating theatre: a high-level walkthrough
Once you are comfortable, we prepare the area in a sterile manner and begin the planned anaesthesia. The operation itself focuses on removing redundant skin and re-draping tissue to achieve a smoother contour across the upper back. We close in layers to support the tissues and reduce tension on the skin line. Dressings are applied to protect the incision and support early healing.
- Positioning and sterile preparation in theatre
- Planned incision and controlled skin excision
- Layered closure and protective dressings
Achieve the same high-standard, clinical excellence you expect in the UK or US, but without the premium price tag. Quality meets exceptional value at AKM Clinic.
Immediate recovery: what you may feel and what we monitor
After surgery, we monitor you closely as the anaesthesia or sedation wears off. It is normal to feel tightness, mild soreness, and fatigue. Some patients feel a little chilled or shaky early on, which often settles quickly. We focus on comfort, stable observations, and safe mobilisation before discharge planning.
- Pain relief plan and nausea control if needed
- Early movement guidance to reduce stiffness
- Wound check and dressing instructions
Discharge planning and your first evening
Many patients return to their accommodation the same day, although some cases may require an overnight stay depending on the surgical plan and your individual response. We explain how to rest, how to position your upper body, and what is “normal” in the first 24 hours. You will also receive clear guidance on medications and when to contact us. We prefer simple instructions you can actually follow.
What to bring and how to prepare (small things that make a difference)
Comfort matters. We advise loose, easy-to-put-on clothing and a plan that avoids heavy lifting or overhead reaching right after surgery. If you are travelling alone, arranging practical support for the first day can make the experience noticeably easier. These details don’t sound medical, but they reduce stress and protect your result.
- Front-opening top or zip hoodie for easy changing
- Soft bra options (if you wear one) that won’t rub the incision line
- A simple plan for meals, rest, and short walks

Upper Back Lift Recovery & Aftercare: how long does healing take?
Recovery after an Upper Back Lift is very individual. Your comfort, swelling, and scar maturation will depend on your anatomy, the amount of skin removed, whether you combined procedures, and how consistently you follow aftercare. The aim is to support predictable healing with a plan that is realistic for UK patients travelling home.
The first 72 hours: what you may feel and what matters most
In the first few days, it’s normal to experience:
- Tightness across the upper back (especially when reaching or changing position).
- Soreness and fatigue, particularly on day 1–2.
- Swelling (oedema) and bruising, which can look worse before it improves.
Your priority during this phase is simple: rest, gentle mobility, and protecting the incision line from tension. Avoid overhead reaching, pushing/pulling, and sudden twisting. We also advise sleeping in a position that reduces strain on the upper back (often slightly elevated and supported).
Week 1–2: swelling, movement, and returning to basic routine
During the first two weeks, most patients notice a gradual improvement in day-to-day comfort, but the area can still feel firm and “pulled”. Light walking is encouraged as advised, but strenuous activity is not. If you wear a support garment (when recommended), it helps manage swelling and reduces stress on the closure.
Common practical guidance in this window includes:
- Keep movements controlled (especially shoulder extension and overhead reach).
- Follow wound care instructions precisely (do not improvise dressings).
- Prioritise hydration, protein intake, and sleep to support tissue repair.
If you are travelling back to the UK, flight timing should be planned around your clinical progress and your surgeon’s advice. The goal is to travel when your pain is controlled, mobility is safe, and your wound care is stable.
We utilise advanced Hyperbaric Oxygen Therapy (HBOT) to minimise downtime and enhance your healing process. Safety is our primary commitment.
Weeks 3–6: easing back into normal life (and what “too soon” looks like)
Many patients feel significantly more “normal” between weeks 3 and 6, but internal healing is still ongoing. This is often the phase where people feel well enough to do more—yet the scar line can still be vulnerable to stretching if you return to upper-body exercise too early.
Typically, your plan may include:
- Gradual increase in activity (guided by your clinical review).
- Scar care once the incision is fully closed (for example, silicone therapy if appropriate).
- Continuing to avoid heavy lifting and intense upper-body training until cleared.
“Too soon” often looks like increased swelling, increased soreness, or a scar that becomes more inflamed after activity. If that happens, it’s a signal to step back and follow your aftercare guidance more conservatively.
Long-term healing: scars, contour settling, and final results
Your contour may look improved early, but the final “settled” outcome takes time. Swelling can fluctuate for weeks, and scars continue to mature for many months. A realistic expectation is:
- Contour refinement: often noticeable early, with continued softening over several months.
- Scar maturation: ongoing up to 12 months (and sometimes longer), with gradual fading and flattening.
Consistency matters. Patients who follow scar care advice, avoid nicotine, and protect the area from excessive tension tend to have the most predictable healing experience.
Our Rapid Recovery & Safety Protocol: HBOT + LLLT
Many patients travelling from the UK want two things at the same time: high-quality results and a recovery plan that feels supported. Alongside surgical technique, we place strong emphasis on structured aftercare and recovery support. Where clinically appropriate, we use technology-led protocols designed to support tissue healing and comfort—most notably HBOT (Hyperbaric Oxygen Therapy) and LLLT (Low-Level Laser Therapy).
HBOT (Hyperbaric Oxygen Therapy): supporting tissue oxygenation and recovery
HBOT involves breathing oxygen in a controlled, pressurised environment. The aim in a post-operative setting is to support tissue oxygenation—which matters because healing tissues benefit from an adequate oxygen supply. When used appropriately, HBOT is often discussed in relation to:
- Supporting the body’s natural repair processes
- Helping with inflammation management
- Supporting overall wound healing conditions
HBOT is not a “magic shortcut”, and it is not a substitute for good surgery and good aftercare. It is best viewed as a supportive tool within a wider recovery strategy.
LLLT (Low-Level Laser Therapy): a gentle approach to healing support
LLLT (sometimes described as “cold laser”) uses low-energy light intended to support cellular activity in the treated area. In post-operative care, it is commonly positioned as a non-invasive method to support:
- Comfort and local tissue recovery
- Inflammation modulation
- Early-stage scar support as part of a broader scar-care plan
LLLT does not replace scar care basics (silicone therapy when appropriate, sun protection, tension control), but it can complement them when used as part of a structured protocol.
Why we combine them: a “systems approach” rather than a single intervention
Upper Back Lift outcomes depend on more than the operation itself—particularly because the upper back is a mobile area where tension and movement can influence healing. Our approach is to combine:
- Technique and closure planning (to control tension and support scar quality)
- Clear aftercare structure (to protect the area during early healing)
- Selective technology support (HBOT + LLLT where appropriate)
The goal is to reduce uncertainty for the patient: better comfort, clearer guidance, and a recovery pathway that is designed—rather than left to chance.
Who is (and isn’t) suitable for these protocols
These therapies are not “automatic add-ons” for everyone. Suitability depends on your medical history and clinical assessment. We will explain what is appropriate for you, what the realistic benefits are, and what the plan will look like in your specific case.
Safety & Risks: Is An Upper Back Lift Dangerous?
Any operation carries risk, and an Upper Back Lift is no exception. The safest way to approach this procedure is to understand the risks clearly, choose an appropriate surgical plan for your anatomy, and follow a structured aftercare pathway. “Dangerous” is not a useful label on its own; what matters is risk awareness and risk reduction.
General surgical risks (and why transparency matters)
The most common categories of risk after body-contouring surgery include:
- Bleeding and bruising (usually mild, occasionally more significant).
- Infection (typically managed with hygiene protocols and, where appropriate, antibiotics).
- Seroma (fluid collection under the skin), which may require monitoring or drainage.
- Delayed wound healing or wound separation, particularly if the closure is under high tension.
- Unfavourable scarring (widening, thickening, pigmentation changes), influenced by genetics, tension, and aftercare.
- Blood clots (a rare but serious risk in surgery in general), where individual risk factors must be assessed carefully.
These risks are not unique to an Upper Back Lift, but the upper back has its own considerations because it is a high-movement area and scar tension must be managed thoughtfully.
Upper-back specific considerations (tension, movement, and scar behaviour)
The upper back moves every time you reach, twist, or change posture. That movement matters because it can affect:
- Scar tension: higher tension can increase the chance of scar widening or delayed healing.
- Swelling patterns: oedema can fluctuate with activity and posture in the first few weeks.
- Comfort: tightness can feel more pronounced because the area is constantly engaged.
For this reason, technique choice, layered closure, and realistic restrictions during early recovery are not “minor details”—they are central to achieving a safe and predictable outcome.
How we reduce risk: selection, planning, and aftercare structure
Risk reduction starts before you enter theatre. Key pillars include:
- Patient selection: stable health, controlled conditions, and realistic expectations.
- Pre-operative screening: understanding medical history, medications, and clot-risk profile.
- Technique and tension control: designing the lift vector and closure to protect the scar line.
- Clear recovery rules: restricting overhead reaching/heavy lifting early to protect healing.
- Supportive recovery protocol: structured follow-up and, where clinically appropriate, recovery-support technologies such as HBOT and LLLT.
Finally, we encourage patients to speak up early if anything feels “off”. Timely review can prevent small concerns becoming bigger problems.
When to contact a clinician urgently (post-op warning signs)
After any surgery, you should seek prompt medical advice if you develop:
- Fever, increasing redness, or worsening pain that feels out of proportion.
- Sudden swelling on one side, significant fluid leakage, or a foul odour from the wound.
- Shortness of breath, chest pain, or calf swelling (urgent assessment required).
Good outcomes are supported by early communication, not “waiting it out”.
Is It Safe To Have An Upper Back Lift in Turkey?
For UK patients, the safety question usually has two layers: clinical safety (the operation itself) and process safety (how reliably care is organised before, during, and after surgery). The country is not the safety factor by itself; the deciding factors are the surgical team, clinical standards, and the structure of your care pathway.
What “safe” looks like in practice: standards, systems, and theatre discipline
A safe Upper Back Lift pathway should include:
- Proper pre-operative assessment (medical history, medications, suitability, and realistic goal setting).
- Sterile theatre protocols and disciplined surgical processes.
- Appropriate anaesthesia planning based on your health profile and procedure scope.
- Structured monitoring immediately after surgery and clear discharge criteria.
- Written aftercare and an accessible clinical contact route if you have concerns.
These are non-negotiable elements. When they are in place, travelling for surgery can be approached responsibly and safely.
Continuity of care for UK patients: follow-up that doesn’t end at the airport
One of the most important safety questions is, “What happens after I leave?” A well-run international pathway should offer continuity through planned check-ins and clear escalation routes. A typical follow-up structure may include staged reviews (for example, early checks in the first weeks, then later assessments as scars mature) alongside remote support where appropriate.
When follow-up is organised properly, patients feel supported and clinical issues can be addressed early—this is a key part of safe medical travel.
How to judge a clinic: practical questions to ask before booking
If you’re comparing options, ask questions that reveal the clinic’s safety culture:
- Who will be responsible for my care in theatre and in recovery?
- What screening do you require before surgery?
- What is your plan for pain control, wound care, and scar management?
- How do you handle complications or unexpected findings?
- What does follow-up look like once I return to the UK?
High-quality providers are comfortable answering these questions clearly. If a provider is vague, rushes you, or minimises risk, treat that as a warning sign.
“London-level quality in Istanbul”: what that should mean
Patients often want reassurance that standards can match what they expect from private care at home. In practical terms, this should mean a structured, professional pathway: disciplined theatre processes, careful selection and planning, and a genuine commitment to aftercare and follow-up. Safety is not a slogan—it is the sum of these systems.

Cost / Fees: Back Lift Surgery Cost 2026 Turkey vs UK
When UK patients compare fees, they are rarely asking for the “cheapest” option. They want clarity. They want to know what is included, what could be added later, and whether the standard of care matches what they would expect from private clinics at home. We approach this conversation with numbers second and structure first.
Why UK private fees often feel fragmented
In the UK, it is common for private surgery costs to be split across multiple line items. That can make comparisons difficult, even when two providers appear to offer the same procedure. It also makes “headline prices” less useful without a full breakdown.
- Surgeon’s fee
- Anaesthetist fee
- Hospital / theatre fees
- Pre-op tests, garments, medications, follow-up visits
It is not a problem. It is just a different billing culture.
How our all-inclusive model reduces uncertainty
Our approach is built around a transparent package model designed for international patients. It is meant to remove “surprise costs” and make planning simpler, especially if you are travelling from the UK. You receive a personalised quote after your virtual consultation and medical review.
- Your complete surgical procedure
- Anaesthesia and operating room fees
- All pre-operative tests
- 5-star hotel accommodation (as planned)
- VIP airport and clinic transfers
- Post-operative medications and garments
- A dedicated Patient Host with 24/7 WhatsApp support
- Long-term virtual follow-up care
What is usually not included (so you can budget accurately)
Even in an all-inclusive model, some items sit outside medical care and remain personal travel decisions. We prefer to state these upfront. It keeps the relationship straightforward.
- International flights
- Personal travel insurance
- Personal expenses (meals beyond what is provided, shopping, etc.)
- Additional hotel nights if you extend your stay
- Visa fees (if applicable)
Comparison table: what you are really comparing
| Category | UK private clinics (typical model) | Our Istanbul package (typical model) | What to double-check |
|---|---|---|---|
| Billing structure | Often itemised (multiple separate fees) | All-inclusive quote after review | Ask for a written breakdown either way |
| Theatre & anaesthesia | Commonly billed separately | Included within the package | Confirm anaesthesia plan (sedation vs general) |
| Tests, garments, medications | May be add-ons depending on provider | Included as part of the pathway | Check what is provided post-op and for how long |
| Travel logistics | Usually self-managed | Hotel + VIP transfers included (flights excluded) | Confirm number of hotel nights and transfer scope |
| Follow-up care | In-person local follow-ups | In-person checks in Istanbul + virtual follow-ups | Confirm follow-up schedule and contact route |
“The most successful aesthetic surgery is one that goes unnoticed.”
If you want an accurate comparison, we can provide a clear, written quote after a no-obligation virtual consultation. No pressure. Just a plan you can audit line by line.
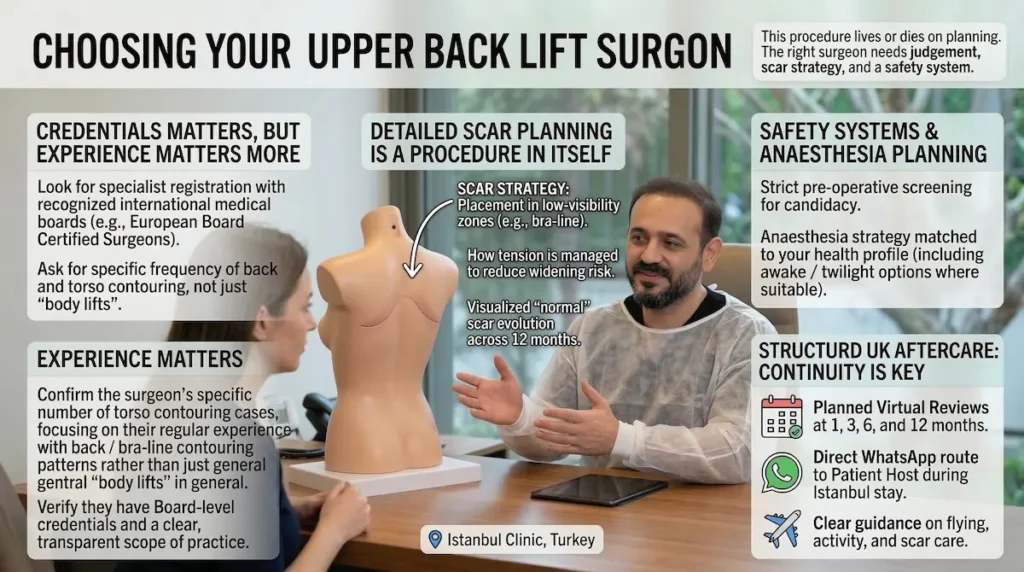
Choosing The Best Upper Back Lift Surgeon
This procedure lives or dies on planning. The upper back is mobile, scars sit in a high-tension zone, and your result must look natural in real life, not only in a single pose. The right surgeon is not simply “good at lifting skin”. They need judgement, scar strategy, and a safety system that holds up when you fly home.
Credentials matter, but experience matters more
Start with credentials. We recommend looking for European Board Certified Surgeons or specialists registered with recognised international medical boards. Then go a step further and ask how often they perform back and torso contouring procedures, not just “body lifts” in general.
- Board-level credentials and transparent scope of practice
- Regular experience with back / bra-line contouring patterns
- A clear, written consent process that includes risks and trade-offs
Ask about scar planning like it is its own procedure
A well-placed scar can be the difference between confidence and daily frustration. In consultation, we show you where the scar is expected to sit and why. We also explain what can change that plan, because anatomy sets limits.
- Where the scar sits in relation to your bra-line coverage
- How tension is managed in closure to reduce widening risk
- What “normal” scar evolution looks like across 12 months
Undergo your procedure with total confidence. Meet our European Board-certified surgeons, who have performed over 2,000 successful facial procedures.
Safety is a system: screening, anaesthesia planning, and monitoring
Great outcomes are built before surgery begins. We use strict pre-operative screening to confirm candidacy, then match the anaesthesia plan to your health profile and the scope of surgery. In recovery, we monitor you closely and give you rules that are simple enough to follow.
- Pre-op screening and medical history review
- Anaesthesia strategy (including awake / twilight options where suitable)
- Clear escalation pathway if you have concerns post-op
Follow-up for UK patients: the part many clinics underbuild
International surgery needs continuity. We maintain support after you return home, with scheduled virtual follow-ups and a direct WhatsApp route to your Patient Host. That structure reduces anxiety and helps us catch small issues early.
- Planned virtual reviews at 1, 3, 6, and 12 months
- 24/7 WhatsApp support during your Istanbul stay
- Clear guidance on flying, activity, and scar care
From VIP airport transfers to 5-star hotel accommodation, we manage every detail. Enjoy a premier medical travel experience in Istanbul.
Your Medical Journey (UK → Istanbul): what to expect
Travelling for surgery should feel structured, not stressful. Our pathway is designed so you know what happens next at each step—clinically and logistically—while keeping safety and follow-up at the centre of the experience.
Step 1: Virtual consultation and surgical planning
Your journey usually begins with an online consultation. We review your goals, your laxity pattern (especially the bra-line zone), relevant medical history, and the most suitable technique options. If you are considering combinations (such as an Arm Lift), we discuss whether that adds genuine value or unnecessary complexity.
- Review of photos/video and a personalised “laxity map”
- Discussion of scar strategy and likely scar placement
- Procedure scope, recovery expectations, and travel timing guidance
- A clear quote and what’s included (with transparent exclusions)
Step 2: Arrival in Istanbul and settling in comfortably
Once your dates are confirmed, the logistics become simple. We provide VIP airport transfers and hotel accommodation as part of the pathway, so you can focus on the medical process rather than managing multiple moving parts. A dedicated Patient Host supports you throughout the experience, including 24/7 WhatsApp access while you are in Istanbul.
- VIP airport pick-up and transfers between hotel and clinic
- Accommodation arranged as part of the package
- Dedicated Patient Host and 24/7 WhatsApp support during your stay
Step 3: Pre-op assessment in clinic
Before surgery, we complete your pre-operative checks and confirm the surgical plan in person. This is where we finalise markings and make sure scar placement expectations are aligned with your anatomy and the degree of lift required.
- Pre-op tests and safety screening
- Final consultation and consent confirmation
- Markings designed for lift direction and scar strategy
Step 4: Surgery, immediate recovery, and aftercare in Istanbul
On the day, we follow a structured theatre process with a focus on comfort, sterile discipline, and predictable recovery. After surgery, we monitor you, guide early mobilisation, and provide practical rules that protect your incision line—particularly important in the upper back, where movement and tension can influence healing.
- Clear pain-control plan and wound-care instructions
- Support garments and post-op medications as planned
- In-person checks before discharge planning
Step 5: Flying home and long-term follow-up
International care should not end at the airport. We provide long-term virtual follow-up so you remain supported once you return to the UK. Follow-up is typically structured at key milestones (for example, 1, 3, 6, and 12 months), focusing on scar maturation, contour settling, and safe return to full activity.
- Virtual follow-ups at planned milestones (e.g., 1/3/6/12 months)
- Clear guidance on flying, activity progression, and scar care
- Escalation route if you have concerns after returning to the UK
Our aim is simple: London-level quality in Istanbul, with the kind of structure and follow-up that expert patients expect.
Upper Back Lift Frequently Asked Questions (FAQ):
How long until I can fly home?
Flying should be planned around your individual recovery and your surgeon’s advice. In general, you should be comfortable, mobile, and stable with wound care before travelling. We plan a sensible recovery window in Istanbul and provide guidance tailored to your procedure scope and health profile.
Will my bra-line scar be visible in a swimsuit?
Scar visibility depends on your anatomy, the required lift, and the cut of your swimwear. Many patients choose an approach where the scar can often sit within a bra-line coverage zone, but swimwear varies widely. We discuss concealment realistically in consultation and show you the expected scar position before surgery.
Can I combine an Upper Back Lift with an Arm Lift?
In selected cases, yes. Combining procedures can improve overall proportion across the upper torso, especially after weight loss. Whether combining is appropriate depends on safety, total operating time, and your recovery capacity. Sometimes staging procedures is the safer and more comfortable choice.
Is awake / twilight anaesthesia suitable for me?
It can be, but suitability depends on your medical history, the length and complexity of your plan, and your comfort with the concept. We decide the anaesthesia approach based on safety first, then comfort. If general anaesthesia is safer for your situation, we will recommend it.
When can I return to work and exercise after Back lift surgery?
Return-to-work timing depends on your job demands and whether you’ve combined procedures. Desk-based work is often possible earlier than physically demanding roles, but you should avoid overhead reaching and heavy lifting in the early phase. Exercise is typically reintroduced gradually, with upper-body training delayed until you are clinically cleared.
What if I’m worried about scars—can you help minimise them?
Yes, scar strategy is built into the plan. We focus on scar placement, tension control, and structured scar-care guidance. Healing varies person to person, but consistent aftercare and avoiding nicotine exposure are two of the biggest controllable factors for scar quality.
How long does Upper Back Lift surgery take?
The length of an Upper Back Lift depends on how much skin needs removing, the technique used (including bra-line scar planning), and whether you combine procedures. A straightforward upper back-only plan is usually shorter than a broader torsoplasty-style plan. Your surgeon will confirm an estimated operating time after reviewing your anatomy and goals.
Will I need drains after a bra-line back lift?
Drains may be used after a bra-line back lift in some cases to reduce fluid build-up (seroma) during early healing, but not every patient needs them. If drains are used, we explain how to care for them and when removal is expected based on your progress. The decision is made for safety and is tailored to your surgical plan.
How painful is an Upper Back Lift recovery?
Most patients describe the first phase as tightness and soreness rather than severe pain—especially when moving the shoulders or reaching. We provide a structured pain-control plan and practical movement guidance to protect the incision line. If your pain is escalating rather than improving, it should be reviewed promptly.
When can I shower after Upper Back Lift surgery?
Showering depends on your dressings, incision status, and your surgeon’s instructions. In the early phase, we often advise keeping the area dry and avoiding soaking (baths, pools, sea) until the incision is adequately healed. We give clear, written aftercare guidance so you know exactly what’s safe and when.
How long do Upper Back Lift results last?
Upper Back Lift results are typically long-lasting, especially if your weight remains stable and you follow scar-care and activity guidance during healing. Ageing continues, and future weight changes can affect skin laxity over time, but removing true excess skin generally creates a durable improvement. Maintaining stable weight and healthy habits helps protect your contour.
Upper Back Lift vs liposuction: which is better for bra-line back rolls?
It depends on whether the issue is mainly excess skin, excess fat, or a combination. Liposuction can reduce fullness, but it cannot reliably remove redundant skin—so if you have true skin laxity at the bra-line, an Upper Back Lift is often the definitive solution. In selected patients, combining approaches can refine contour, but the plan should be based on a personalised assessment.
Medical Disclaimer: This page is for general information only and does not replace a medical consultation, diagnosis, or treatment advice. Suitability for an Upper Back Lift depends on your individual health status, anatomy, and clinical assessment. Always seek advice from a qualified healthcare professional for symptoms such as pain, weakness, numbness, or restricted movement, and follow the guidance of your treating clinician for surgical decisions and aftercare.
Upper Back Lift: Patient Stories

Laura

Upper Back Lift Surgeons
Upper Back Lift Cost in Turkey
Starting from ~ £3000
* There are no hidden fees or unexpected charges.
- Your PersonalisedUpper Back LiftProcedure
- All Specialist Surgeon & Anaesthesia Fees
- All Pre-Op Tests & Post-Op Check-ups
- 5-Star Hotel Accommodation (incl. breakfast)
- All Private VIP Airport & Clinic Transfers
- 24/7 Dedicated Patient Coordinator & Translation Services
Upper Back Lift: A Cost Comparison
| City | Cost |
|---|---|
| London | ~ £10,000 GBP |
| Bristol | ~ £9,800 GBP |
| Bristol | ~ £9,700 GBP |
| Edinburgh | ~ £10,200 GBP |
| Manchester | ~ £10,500 GBP |
Upper Back Lift: Patient Reviews
Jammal Canada
I have had face and neck lift with AKM Clinic they have been so good to me and my operation went so smoothly🥰 i would like to thank my doctor here and also to the team 💐

Ava Canada
Thank you AKM Clinic for giving me my confidence back! Had facelift + temporal lift 3 months ago and the outcome is already stunning. Special thanks to Hande!

Jakayla USA
Had a deep plane facelift and lower eyelid procedure at AKM Clinic 7 months ago. The results are fantastic - very subtle and natural. I didn’t expect the entire experience to be so comfortable. Hande managed everything and kept in contact even after I returned to USA. I’m beyond pleased with the outcome and the care I received. Would do it again in a heartbeat!

Barbara United Kingdom
It has been 4 months since my surgery. Everything is great, The most important thing is l love the way l look, l look exactly how l wanted. Meaning l look natural, just almost 40 years younger. I pulled Facebook - majority voted 37ys. I also had face, neck, chest, and hands CO2 laser. My skin is flawless.

Lisa Canada
I had a face, neck and arm lift at AKM. I’m just over 4 weeks post and couldn’t be happier with the results. The entire experience was wonderful! My coordinator, Khadija made me feel comfortable from beginning to end! I highly recommend AKM and will definitely go back for other procedures!

Julie USA
I am beyond grateful I went with AKM Clinic for my deep plane face and neck lift, upper eyelid, and co2 laser. Dr. Akif has magic hands and my results are truly incredible! I came from the US and assistant Emine was the best in assuring every detail was coordinated and communicated with me beyond my expectations every step of the way. 10 out of 10 to the entire team! I couldn’t be more pleased!

Ready to Begin Your Own Transformation Journey?
Join the 2,000+ patients who have trusted Dr Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, naturally restored you begins with a simple, no-obligation conversation. Contact us today from the UK for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. There are no hidden fees.
#2: Secure Your Date & VIP Booking
Once you are ready, our dedicated patient coordinators will help you secure your procedure date. We will handle all your bookings, including your 5-star hotel accommodation and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you will meet your specialist surgeon to finalise the details for your natural, subtle, and restored new look.













