Otoplasty in Turkey




- Otoplasty tailored to your anatomy for natural ear pinning results and balanced facial harmony.
- Safety-first care in Istanbul with local or twilight anaesthesia options and structured UK follow-up.
- Clear recovery timeline: swelling days 1–3, work often 1–2 weeks, gradual activity from weeks 3–6+.
- High-value Otoplasty for UK patients with transparent inclusions, aftercare guidance, and fair comparison to UK private fees.
AI-generated summary, fact-checked by our medical experts.
Otoplasty: Quick Facts
Duration of Surgery
Type of Anaesthesia
Initial Recovery Period
Hospital Accommodation
Return to Daily Activities
Otoplasty Results: Before and After
Considering Otoplasty to correct prominent ears? Our Istanbul clinic offers ear pinning (pinnaplasty) designed for natural balance, not an over-tight look. We assess your anatomy, explain technique options, and plan anaesthesia around comfort, including local and twilight pathways when appropriate. Our focus is safety, symmetry, and results that look effortless in photos, profiles, and everyday life too.
You will find a clear recovery timeline, day-by-day aftercare guidance, and an honest discussion of risks, scarring, and permanence. For UK patients travelling to Turkey, we coordinate a calm journey and structured follow-up once you return home, so healing stays predictable and supported.
Table of Contents
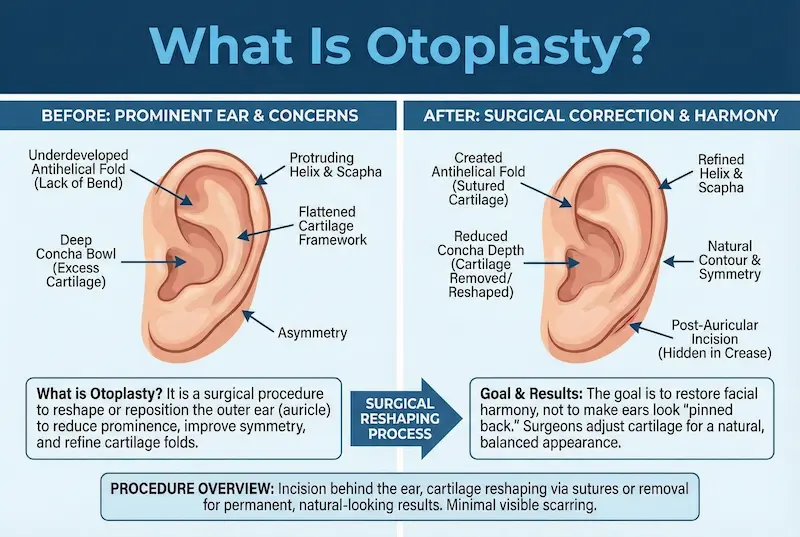
What is Otoplasty?
Otoplasty is a surgical procedure that reshapes and repositions the outer ear (pinna) so it sits in a more balanced, natural position. It is commonly used to correct prominent ears, asymmetry, or an underdefined fold. The goal is proportion, not perfection. Results are designed to be long-lasting.
Most people explore this surgery for one clear reason: their ears draw attention before their face does. Our approach is simple. We focus on anatomy, symmetry, and a natural contour that suits your features. We aim for a result that looks unremarkable in the best possible way.
Otoplasty, Ear Correction, Ear Pinning, and Pinnaplasty: UK terminology
In the UK, several terms are used for the same general goal: bringing prominent ears closer to the head and improving shape. “Otoplasty” is the medical umbrella term. “Ear correction” is a common UK phrase, while “ear pinning” and “pinnaplasty” are often used in clinic marketing and patient forums.
- Otoplasty: Broad term covering reshaping, repositioning, and selected structural adjustments.
- Pinnaplasty: Usually refers to pinning the ear back, often focusing on prominence.
- Ear correction: Patient-friendly UK term that may include symmetry and contour refinement.
- Ear pinning: Informal phrase describing the “set-back” effect.
Why ears look prominent: a simple anatomy explainer
Prominent ears are rarely caused by “too much ear”. More often, the shape of the cartilage creates an ear that projects. Two common contributors are a weak or absent antihelical fold (the inner ridge) and a deeper conchal bowl (the central cartilage cup).
- Underdefined antihelix can make the ear look flatter and more projected.
- Conchal prominence can push the whole ear outward.
- Asymmetry is normal, but a noticeable difference can become a daily distraction.
How does otoplasty work?
Otoplasty works by adjusting cartilage position and contour, then holding that new shape with precise internal sutures. The aim is to create a smooth, natural fold and reduce projection while keeping the ear’s normal landmarks. We plan every change with a “face-first” mindset, so the ears support your overall profile rather than becoming a feature of their own.
- Assessment: We map your ear shape, projection points, and symmetry on both sides.
- Reshaping: We refine folds and contours in the cartilage to reduce prominence.
- Stabilisation: We use internal sutures to maintain the new position as tissues heal.
- Finishing: We close carefully to keep scars discreet, typically hidden behind the ear.
Is otoplasty permanent?
For most patients, the result is long-lasting. Cartilage “memory” is real, which is why technique and stabilisation matter. In the early healing period, the tissues are still settling and the ear can feel firmer or slightly tight. Once healing is complete, the new contour typically remains stable.
- Early weeks: Swelling and stiffness can make the ears feel different to the touch.
- Settling phase: Subtle changes are expected as oedema resolves and tissues mature.
- Long term: A small risk of partial “spring back” exists, which is why follow-up and aftercare are part of the plan.
Share your photos and medical history to receive a personalised assessment from our European Board-certified facial surgery team.
Benefits of Otoplasty Surgery: what changes, realistically?
Patients often ask whether the change will be obvious. The honest answer: it depends on your starting point, your hairstyle, and how much prominence is corrected. The best outcomes look natural and proportionate, not “done”. We follow one consistent principle in every plan: create harmony, then stop.
Rejuvenation, Not Alteration.
A natural-looking contour, not an “operated” ear
Modern otoplasty is not about pinning the ear flat. The ear has depth and landmarks that need to stay intact. A well-planned correction keeps a gentle curve, avoids sharp edges, and respects the space between ear and scalp. The goal is to make the ears blend into your overall facial balance.
- A softer, more defined fold where it was previously absent
- Reduced projection, especially in photos and profile views
- Better balance without over-correction
Improved symmetry and proportion
Perfect symmetry is not realistic in human anatomy. What we target is “visual symmetry” at conversational distance and in typical lighting. That means reducing the most noticeable differences between sides and aligning projection points. For many UK patients, this is the benefit they notice most day to day.
- More even ear-to-head distance on both sides
- Improved alignment of the upper and mid-ear projection
- A calmer profile, especially when hair is short or tied back
Confidence in everyday situations
Many people adapt their behaviour around prominent ears without realising it. They choose specific haircuts, avoid windy days, or feel self-conscious in group photos. After healing, patients commonly report that their attention shifts away from their ears. That quiet change can matter.
- More freedom with hairstyles and sports headwear
- Less “ear awareness” in photos, video calls, and social settings
- A feeling of proportion that matches how you see yourself
What otoplasty does not do
Clear expectations protect results. Otoplasty does not change hearing, and it cannot guarantee identical ears. It also does not remove every minor irregularity in cartilage texture. What it can do is address prominence, improve contour, and bring the ears into better balance with your face.
Answer a few brief questions about your concerns, health, and goals to discover which treatment options may suit you best.
Am I A Good Candidate For Otoplasty?
Most UK patients who enquire about otoplasty have one of three concerns: prominent ears, noticeable asymmetry, or a contour they have never felt comfortable with. Suitability is not about chasing a “perfect” ear shape — it is about whether we can improve proportion safely, with a stable result that still looks natural.
Who tends to benefit most?
You may be a good candidate if prominent ears or shape irregularities affect your confidence, your hairstyle choices, or how you feel in photographs. Clinically, we look for a correctable anatomical reason for projection or imbalance, such as an underdefined fold, conchal prominence, or a combination of both.
- Prominent ears (often due to a weak antihelical fold and/or conchal prominence)
- Asymmetry where one ear sits further forward or has a different fold definition
- Post-traumatic changes in shape where contour can be safely improved
- Refinement goals where the aim is subtle balance rather than a dramatic “pin-back” look
Age considerations: children vs adults
Otoplasty can be considered in both younger patients and adults, but the approach and decision-making differ. In younger patients, the priority is emotional wellbeing, timing around school, and ensuring the child’s own comfort with the plan. In adults, the priority is stable anatomy, informed consent, and a recovery plan that fits work and daily life.
- Younger patients: timing is individual; we focus on readiness, support, and realistic expectations.
- Adults: cartilage is firmer and “memory” is stronger; technique and aftercare become even more important.
When we may advise waiting (or not proceeding)
Safety and predictability come first. There are scenarios where it is better to postpone treatment until conditions are optimal, or to explore alternatives. This is especially important for the UK “expert patient” who values long-term quality over short-term speed.
- Active skin or ear infection in or around the surgical area
- Uncontrolled medical conditions that increase surgical or healing risk
- Smoking or nicotine use (we typically advise stopping well in advance to support tissue healing)
- Unstable expectations (for example, aiming for perfectly identical ears)
- Complex scar history (including tendency to thickened scarring), where we must plan carefully and discuss risk transparently
Pre-operative assessment: our practical checklist
Before recommending a plan, we assess both anatomy and lifestyle factors that affect outcome. This is where careful planning prevents common frustrations later (for example, over-correction, visible edges, or recurrence).
- Anatomy mapping: projection points, fold definition, conchal depth, and side-to-side differences
- Skin and scar assessment: thickness, healing history, and any prior ear surgery
- Health review: medications, allergies, bleeding risk factors, and healing risks
- Recovery planning: work, exercise, sleep habits, glasses/headphones use, and travel schedule
- Expectation alignment: what “natural” means for your face and your goals
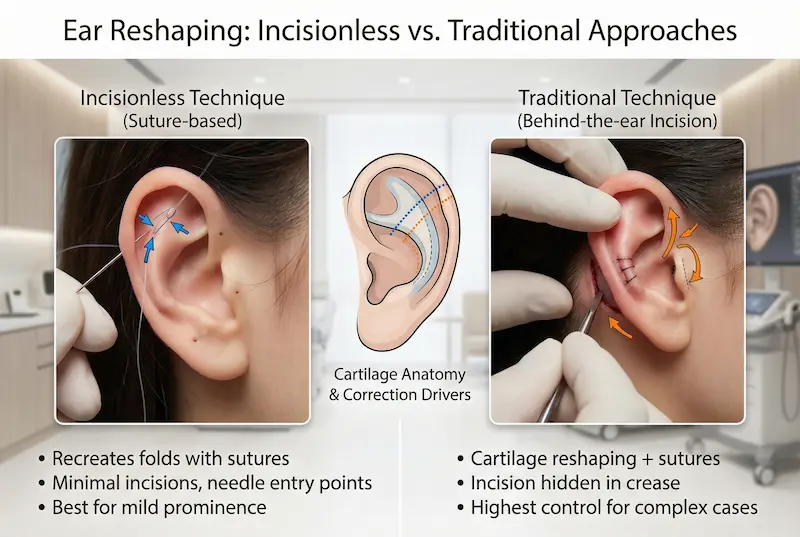
Surgical Techniques Explained: how we plan an Otoplasty
There is no single “best” technique for every ear. A strong result comes from matching the method to your anatomy and using a conservative, structured plan. In practice, we often combine techniques to create a natural contour, reduce projection, and support long-term stability.
Suture-based reshaping: creating a natural fold (Mustardé-style principles)
If the antihelical fold is weak or absent, the ear can look flatter and more prominent. Suture-based reshaping focuses on recreating a smooth fold using carefully placed internal stitches. The intent is refinement — avoiding sharp ridges or an overly tight appearance.
- Best suited to ears where fold definition is the main issue
- Designed to produce a soft, natural curve rather than a flat “pinned” look
- Often combined with other steps if conchal prominence is also present
Set-back positioning: addressing conchal prominence (Furnas-style principles)
When the conchal bowl pushes the ear outward, fold creation alone may not be enough. Set-back positioning uses internal fixation to bring the ear closer to the head in a controlled way, maintaining a natural ear-to-scalp distance and preserving normal landmarks.
- Best suited when the ear sits outward due to conchal depth
- Helps improve projection, particularly in the mid-ear region
- Requires precise planning to avoid an over-corrected, overly close appearance
Cartilage refinement: scoring and selective reduction
Some ears have thicker or stiffer cartilage, or a shape that benefits from additional refinement. In those cases, controlled cartilage modification may be considered to improve contour and reduce tension that can contribute to “spring back”. The guiding principle is always conservative change with stable support.
- Can help when cartilage is stiff or the shape is resistant to suturing alone
- May be used selectively for contour smoothing and long-term stability
- Planned carefully to maintain natural thickness and landmarks
Incisionless otoplasty: who it suits (and who it doesn’t)
Incisionless approaches may appeal to patients looking for minimal disruption, but they are not appropriate for every anatomy. They tend to suit mild prominence in selected cases, typically when the goal is modest fold enhancement rather than broader reshaping. If stronger structural correction is needed, a more formal approach is usually safer and more predictable.
- Potentially suitable for mild cases with specific anatomical patterns
- Not ideal where there is significant conchal prominence or complex asymmetry
- We prioritise predictability over “minimal” if the anatomy requires it
Revision otoplasty: correcting previous surgery
Revision otoplasty is more specialised than primary surgery. It may be needed if there is recurrence (partial return of prominence), an over-corrected appearance, sharp edges, visible irregularities, asymmetry, or concerns with scarring. Planning is more detailed because the tissues have changed and cartilage behaviour can be less predictable.
- Targets recurrence, over-correction, contour irregularities, and asymmetry
- Requires careful assessment of scar tissue and previous suture patterns
- Recovery can be slightly different; we plan aftercare to support tissue stability
Technique overview: how methods compare
| Method focus | Primary goal | Most suitable for | Key consideration |
|---|---|---|---|
| Suture-based fold creation | Improve antihelical fold definition | Prominence driven by weak/absent fold | Avoiding sharp edges and over-tightening |
| Set-back positioning | Reduce projection from conchal prominence | Ears pushed outward by conchal depth | Maintaining a natural ear-to-head distance |
| Cartilage refinement | Improve contour and reduce resistance | Stiff cartilage or resistant shapes | Conservative modification to preserve landmarks |
| Incisionless approaches | Modest correction with minimal disruption | Selected mild cases | Not appropriate for complex anatomy |
| Revision otoplasty | Correct previous outcome issues | Recurrence, irregularities, over-correction | More complex planning due to tissue changes |
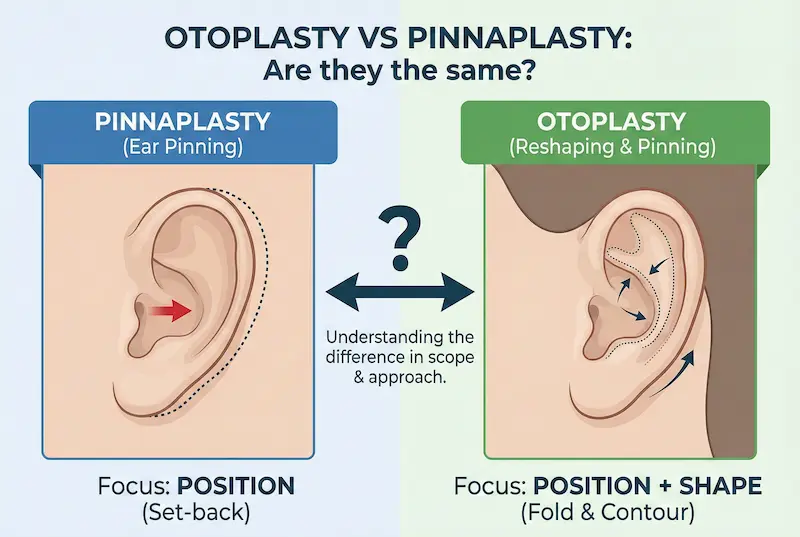
Otoplasty vs Pinnaplasty: are they the same?
This is one of the most common questions we hear from UK patients, and the confusion is completely understandable. In everyday UK usage, pinnaplasty is often used to mean “ear pinning” — bringing prominent ears closer to the head. Otoplasty, however, is the broader medical term that can include pinning, reshaping, contour refinement, and selected structural adjustments.
Why different clinics use different terms
In the UK, many clinics favour “pinnaplasty” because it sounds specific and patient-friendly. Others use “otoplasty” because it is the recognised surgical umbrella term. The challenge is that these words are sometimes used interchangeably on websites, even when the treatment plan is not identical.
- Pinnaplasty often emphasises position (set-back / reduced projection).
- Otoplasty covers position + shape (fold creation, contour refinement, and stabilisation).
- Ear correction is a broad phrase that may include symmetry, contour and prominence reduction.
The practical difference: “set-back only” vs “shape + set-back”
Many prominent ears are not just “sticking out” — they also have a fold that is underdefined. If a plan focuses only on pulling the ear back, the result can look tight or unnatural. A well-planned approach usually considers both contour and projection, with conservative changes that preserve normal landmarks.
- Set-back emphasis: may suit mild prominence driven mostly by position.
- Contour emphasis: important when the antihelical fold is weak or absent.
- Combined approach: commonly used when both fold and conchal prominence contribute.
How we describe it during consultation
We use whichever term makes the plan clear, but we never let terminology replace precision. During your assessment, we focus on what actually needs correcting:
- Where projection is most noticeable (upper ear, mid-ear, or both)
- Whether fold definition needs creating or refining
- How much correction looks natural for your face (not just “as close as possible”)
- How to reduce the risk of recurrence through technique and aftercare
Quick guide: which term matches your search intent?
- If you are searching “ear pinning” or “pinnaplasty”, you are usually thinking: “Will my ears sit closer to my head?”
- If you are searching “otoplasty” or “ear reshaping”, you are often thinking: “Will the shape look better and more natural?”
- If you are searching “ear correction surgery”, you are usually thinking: “Which option is safest and most reliable for my specific ears?”
Combined Procedures: when it makes sense (and when it doesn’t)
Some patients ask whether otoplasty can be combined with other procedures during the same trip. It can be possible in selected cases, but combining procedures should never be a default “bundle”. The deciding factors are safety, surgical time, recovery practicality, and whether combining genuinely improves the overall outcome.
Why UK patients consider combining procedures
UK patients travelling for treatment often want a structured plan that respects both time and recovery. When appropriate, combining can mean one travel period, one recovery window, and a single coordinated follow-up plan.
- One journey and accommodation period
- A single recovery “pause” from work and social commitments
- More efficient follow-up planning, especially for international patients
Common combinations we may discuss
Otoplasty is sometimes considered alongside other facial procedures, particularly when the goals are complementary and the total plan remains safe and realistic. Options vary by anatomy, health profile, and timeline.
- Rhinoplasty: for patients aiming for overall profile balance
- Eyelid surgery (blepharoplasty): for refreshed eye-area appearance where appropriate
- Facial fat transfer or other soft-tissue refinement: in carefully selected cases
- Facelift: for patients aiming for overall facial balance
We only recommend combination planning when it keeps the result natural and the recovery manageable. If combining would complicate healing or reduce predictability, we would stage procedures instead.
Our surgical dates fill up quickly due to high international demand. Secure your consultation today to arrange your preferred travel dates.
Safety considerations: what we evaluate before combining
Combining procedures can extend time in theatre and increase the complexity of post-operative care. Before recommending any combined plan, we evaluate your full medical profile and recovery constraints, not just the aesthetic goals.
- Total surgical time and whether the combined plan remains within a safe, predictable range
- Anaesthesia planning: the most appropriate approach for your comfort and safety
- Recovery practicality: sleep position, swelling management, activity restrictions, and travel schedule
- Aftercare compatibility: whether aftercare instructions for one procedure conflict with the other
When staging is usually the better choice
Staged treatment is often the more “expert patient” decision when a combined plan would compromise predictability or comfort. This is especially relevant if you have a demanding job, limited recovery time, or a complex anatomical goal that benefits from focused healing.
- If the plan would create competing aftercare needs (for example, different sleep or compression requirements)
- If the combined recovery would be too restrictive or stressful
- If a revision or complex correction is involved, where precision and tissue behaviour matter more
How we plan combined procedures for international patients
If a combined plan is appropriate, we structure it around clarity: a defined sequence, a realistic recovery map, and a follow-up schedule that works once you are back in the UK. Our priority is a plan you can actually follow — because compliance is part of the result.
- Clear day-by-day aftercare priorities
- Practical guidance for sleep, hygiene, work return, and activity
- Structured remote follow-up planning after you travel home
Anaesthesia For Otoplasty: what UK patients should know
For many UK patients, anaesthesia is the part of surgery that feels most uncertain — not because otoplasty is “major”, but because you want clarity and control. Our approach is to match the anaesthesia plan to your comfort, your anatomy, and the safest, most predictable pathway for your procedure.
Local anaesthesia: a controlled, awake approach
In selected cases, otoplasty can be performed under local anaesthesia. This means the ear area is fully numbed while you remain awake. Patients often prefer this option when they want a shorter recovery profile from anaesthesia and a straightforward day-plan.
- What you feel: pressure and movement, but not sharp pain
- What you don’t feel: cutting sensations in the treated area
- Why it can work well: the surgical field is localised and the procedure can be carefully controlled
Twilight sedation: comfort without deep anaesthesia
Some patients prefer to be more relaxed during the procedure. In those cases, we may discuss twilight sedation alongside local anaesthesia. This is designed to reduce anxiety and awareness without the depth of a full general anaesthetic.
- Often preferred by patients who feel uneasy about being fully awake in theatre
- Can support a calmer experience while keeping recovery practical
- Planned carefully to balance comfort and safety
General anaesthesia: when it may be considered
General anaesthesia is sometimes appropriate depending on clinical factors, patient preference, or the complexity of the plan (for example, certain revision scenarios). If general anaesthesia is recommended, we explain exactly why — and what that means for your day-of-surgery schedule and recovery.
- May be considered for more complex correction plans
- May suit patients who strongly prefer to be fully asleep
- Requires standard pre-operative preparation and post-anaesthetic monitoring
How we choose the safest option
We do not treat anaesthesia as a “tick-box”. We assess what is medically appropriate and what is realistically comfortable for you. The goal is a plan you can follow calmly — because a smooth experience supports a smooth recovery.
- Medical profile: overall health, medications, allergies, and any prior anaesthetic history
- Procedure complexity: primary vs revision otoplasty and the steps required
- Anxiety level: how you respond to clinical environments and theatre settings
- Recovery practicalities: travel timing, rest needs, and support in the first 24–48 hours
What to do before anaesthesia (practical UK-style guidance)
Before surgery, we provide clear instructions that help reduce avoidable risks. The details vary by your anaesthesia plan, but preparation generally focuses on safety, comfort, and predictable healing.
- Follow fasting and hydration instructions exactly if sedation or general anaesthesia is planned
- Disclose all medications and supplements (including aspirin-like products and herbal supplements)
- Avoid alcohol immediately before surgery, and plan a calm night’s sleep if possible
- Arrange practical support for the first night, especially if sedation is used

Step-By-Step: what happens in the operating theatre?
UK patients often want to know exactly what will happen, in order, with no vague reassurance. Below is a clear overview of the typical otoplasty journey on the day of surgery. Exact steps can vary depending on your anatomy and whether the plan is primary correction or revision.
1) Pre-operative review and final planning
Before you enter theatre, we confirm the plan in a structured way. This includes checking your medical information, answering final questions, and ensuring the goals are aligned with what is anatomically achievable.
- Review of your intended correction: projection points, fold definition, and symmetry aims
- Confirmation of anaesthesia plan and comfort priorities
- Final photographs and surgical markings where appropriate
2) Preparation in theatre
In theatre, we focus on sterility and precision. The surgical area is prepared carefully, and we confirm positioning so the ears can be assessed accurately. If you are having local anaesthesia (with or without twilight sedation), we make sure the area is fully numb before proceeding.
- Sterile preparation and draping
- Local anaesthetic administration (if planned)
- Comfort check before any surgical step begins
You are never alone. Our dedicated 24/7 Patient Hosts and English-speaking team will be by your side from the moment you arrive until your departure. Your comfort and safety are our constant priority.
3) Access and reshaping: the core of otoplasty
Most otoplasty techniques use discreet access behind the ear, so scars are typically hidden in the natural crease. From there, we reshape and stabilise the cartilage based on your individual anatomy — creating or refining a natural fold, reducing projection, and balancing both sides.
- Fold creation/refinement: improving the antihelical contour for a natural curve
- Projection control: addressing conchal prominence when needed
- Stabilisation: internal sutures to hold the new shape as tissues heal
4) Symmetry checks (done properly)
Symmetry is not a single moment — it is checked throughout. We assess both ears repeatedly during the procedure to ensure the correction looks balanced from typical viewing angles. The goal is a result that sits naturally on your face, not a result that looks “engineered”.
- Side-to-side projection checks at key stages
- Contour checks to avoid sharp edges or over-correction
- Final positioning before closure
5) Closure and dressing
Closure is performed carefully to support healing and keep scars discreet. A dressing is then applied to protect the ears in the early phase and reduce the risk of accidental bending or pressure while tissues settle.
- Meticulous closure behind the ear
- Protective dressing and, where indicated, head support
- Immediate post-op comfort and safety monitoring
6) After theatre: recovery room and discharge planning
After the procedure, you are monitored while the effects of anaesthesia settle. We confirm that you are comfortable, stable, and clear on aftercare instructions before discharge. We also explain what is normal (swelling, tightness, sensitivity) and what would be a reason to contact us promptly.
- Monitoring for comfort and stability
- Clear aftercare instructions: dressing/headband, hygiene, and activity restrictions
- Follow-up plan and contact guidance for any concerns

Otoplasty Recovery & Aftercare: How Long Does Healing Take?
Recovery after otoplasty is usually straightforward, but it is still surgery — and the first few weeks matter. Most patients feel “socially presentable” sooner than the ears feel fully normal. Swelling (oedema), tightness, and sensitivity are common early on, and the ears can feel firm while the cartilage and soft tissues settle.
Otoplasty recovery time: a realistic timeline
Every patient heals at a different pace, but a practical guide looks like this:
- Days 1–3: noticeable tightness and swelling; mild discomfort is typical. You may feel pressure from dressings or a head support band.
- Days 4–7: swelling begins to settle; bruising (if present) often starts to fade. Many patients feel comfortable doing light, calm activities at home.
- Week 2: daily life becomes easier; sensitivity may persist, especially to touch or cold air. Most patients can return to desk-based work depending on comfort and dressing schedule.
- Weeks 3–6: ongoing refinement as oedema continues to resolve. The ears usually feel more “yours”, but can still feel slightly firm.
- After 6–12 weeks: tissues mature further; minor changes in contour can continue. This is when many patients feel the result looks fully settled in normal lighting and photos.
We utilise advanced Hyperbaric Oxygen Therapy (HBOT) to minimise downtime and enhance your healing process. Safety is our primary commitment.
Day-by-day recovery: what is normal?
UK patients often want to know what is “normal” versus what should worry them. Typical early experiences include:
- Swelling (oedema): expected, usually most noticeable in the first week.
- Bruising: variable; some patients have very little, others have mild bruising that fades over 7–14 days.
- Changing sensation: temporary numbness, tingling, or hypersensitivity can happen as nerves settle.
- Unevenness: one side can appear more swollen than the other early on; this often resolves as healing progresses.
What we aim for is a recovery you can manage calmly, with clear instructions and predictable milestones.
How to sleep after otoplasty
Sleep is one of the most important practical factors in early healing, because accidental pressure can affect comfort and, in rare cases, stability. We usually recommend protecting the ears from bending and avoiding side-sleeping at the start.
- Best position: on your back, with your head slightly elevated (extra pillows can help).
- Avoid: sleeping on either side until we advise it is safe, and avoid tight headphones or anything that presses on the ear.
- If you roll in sleep: a travel pillow or pillow “barrier” can help prevent turning onto the ear.
Dressings and headband: how long will I need them?
Dressings and head support are used to protect the ears during the early phase. The exact schedule varies by technique and anatomy, but the principle is consistent: protection first, then gradual normalisation.
- Early protection: your initial dressing supports the ears while tissues begin to heal.
- Headband phase: a supportive band is commonly recommended to reduce accidental bending, especially at night.
- Practical care: we advise how to keep the area clean and when to resume hair washing safely.
Work, exercise, and daily routine
Most patients can return to calm, non-physical routines relatively quickly, but impact and pressure are the risks to avoid. We plan your timeline around your job and lifestyle so you are not guessing.
- Desk-based work: commonly within 1–2 weeks, depending on comfort and dressing schedule.
- Gym and vigorous exercise: usually delayed until swelling is settling and the ears are protected from contact.
- Contact sports: typically avoided for longer, because accidental trauma can compromise the result.
- Glasses: we guide you on how to wear them comfortably without pressure on healing tissues.
Recovery support: comfort and tissue healing
For suitable patients, supportive recovery measures may be discussed to help comfort and tissue recovery. These are not a substitute for technique or aftercare — they are an additional layer of support when clinically appropriate.
- Hyperbaric oxygen support: may be considered to support tissue oxygenation in selected cases.
- Low-level light support: may be discussed as part of a comfort-and-recovery approach.
We only recommend supportive options when they fit your medical profile and your recovery plan.
Safety & Risks: Is Otoplasty Dangerous?
Otoplasty is generally considered a safe procedure when performed with appropriate patient selection, careful technique, and structured aftercare. That said, no surgery is “risk-free”. The role of an expert plan is to reduce avoidable risks and to identify early warning signs if something is not progressing as expected.
Is otoplasty safe?
For most healthy patients, safety is high and recovery is predictable. The key is not simply “where it’s done”, but how it’s planned and how closely aftercare is followed. We focus on conservative correction, natural contour, and stability — rather than forcing the ears into an overly tight position.
Common, expected side effects (not complications)
These effects are common during normal healing and usually improve steadily:
- Swelling (oedema) and firmness in the early weeks
- Bruising around the ear or behind the ear
- Temporary numbness or sensitivity changes
- Mild asymmetry early on due to uneven swelling
- Itchiness as the skin heals (particularly as dressings change)
Possible complications (what we monitor for)
Complications are uncommon, but the “expert patient” approach is to understand them clearly and respond early if needed.
- Infection: increasing redness, heat, swelling, or discharge.
- Haematoma (blood collection): rapid swelling, significant pain, or pressure that worsens rather than improves.
- Wound healing issues: delayed healing or irritation around the incision line.
- Scarring concerns: thickened scarring can occur in predisposed patients and should be discussed honestly in advance.
- Recurrence: partial return of prominence in a small number of cases (cartilage “memory” can contribute).
- Contour irregularities: visible edges or unnatural lines if correction is too aggressive (why conservative planning matters).
How we reduce risk: practical, controllable factors
Many risks are reduced by doing simple things consistently — before and after surgery. We provide clear instructions and a follow-up pathway that is realistic for UK patients travelling internationally.
- Medical screening: full review of medications, allergies, and healing risks.
- Technique choice: matching method to anatomy to avoid over-correction and instability.
- Aftercare structure: dressings/headband use, hygiene, and activity restrictions explained clearly.
- Behaviour factors: avoiding nicotine, protecting the ears from bending/trauma, and prioritising sleep in early healing.
When to contact us urgently (and when to seek emergency care)
We prefer you to contact us early if something feels “off”. It is always easier to address concerns at the earliest stage. Seek urgent medical attention if symptoms are severe or rapidly worsening.
- Contact us promptly if you notice increasing redness, heat, discharge, worsening swelling, or unusual asymmetry that develops suddenly.
- Seek urgent medical care if you have severe pain not relieved by prescribed measures, rapid swelling/pressure, fever, or signs of an allergic reaction.
- If you are back in the UK, we support you with guidance and coordination while you access appropriate local services when needed.
Our surgical dates fill up quickly due to high international demand. Secure your consultation today to arrange your preferred travel dates.
Is Otoplasty Safe In Turkey? A UK patient’s guide to making a confident choice
It’s normal to question safety when you’re considering treatment outside the UK. The right way to think about it is this: safety is not determined by geography alone — it’s determined by clinical standards, patient selection, sterile practice, anaesthesia planning, and structured follow-up. If those fundamentals are strong, international treatment can be both safe and predictable.
What “safety” actually means for otoplasty
For otoplasty, safety is mostly about reducing avoidable risks and responding early if anything deviates from normal healing. That includes:
- Appropriate patient selection: confirming you are medically suitable and timing surgery sensibly.
- Controlled technique: conservative correction with stable support (avoiding over-correction).
- Sterile standards: proper preparation, theatre discipline, and post-op wound care guidance.
- Clear escalation pathways: knowing exactly what to do if you have concerns after you return to the UK.
What to look for as a UK “expert patient”
If you’re comparing options in the UK and Turkey, focus on signals of quality and accountability. The best clinics make information easy to verify and do not rely on vague reassurance.
- Transparent consultation: a detailed plan based on your anatomy, not a one-size approach.
- Clear discussion of risks: including recurrence, contour irregularities, infection/haematoma signs, and scarring considerations.
- Defined aftercare: written guidance, follow-up schedule, and direct routes to clinical support.
- Revision capability: evidence that the team understands complex ear anatomy and can manage suboptimal outcomes.
Our approach in Istanbul: structure, not hype
In our clinic, safety is designed into the pathway. We plan your procedure around anatomy, comfort, and predictability, using an approach that prioritises natural contour and long-term stability. We do not aim for “as close as possible” ears — we aim for balance that looks normal in real life.
- Planning-first workflow: assessment of projection points, fold definition, and symmetry goals before technique selection.
- Conservative correction: avoiding sharp edges and avoiding an overly tight, operated appearance.
- Aftercare clarity: practical rules for sleep, head support, hygiene, work return, and activity restrictions.
Continuity of care when you return to the UK
International patients need more than a successful day in theatre — they need a follow-up plan that continues once they’re home. We structure remote follow-up so you are not left guessing during the key settling phase.
- Scheduled check-ins: structured follow-up points (for example, at 1, 3, 6, and 12 months) depending on your plan and progress.
- Clear photo guidance: how to take consistent photos so we can assess contour and symmetry accurately.
- Escalation guidance: what is normal, what is not, and what to do if you need in-person assessment in the UK.
Travel practicality: choosing a sensible timeline
UK patients often ask about timing around flights, work, and social commitments. The goal is not simply “fast travel” — it is a timeline that respects early healing, protects the ears, and reduces stress.
- Plan for a calm first week: protecting the ears is easier when your schedule is not demanding.
- Avoid rushing back into contact risks: crowded environments, heavy exercise, and anything that pressures the ears too early.
- Choose travel dates that allow you to follow aftercare properly (especially sleep position and head support).
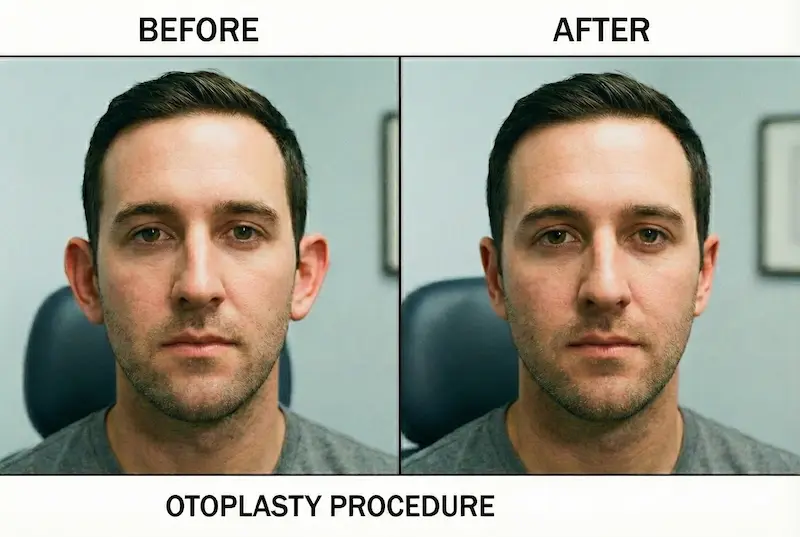
Realistic Expectations & Results: what good otoplasty looks like
Otoplasty results are best judged by one standard: does it look natural on your face? A strong outcome is rarely dramatic to other people — it simply removes the “ear-first” impression and restores balance. The “expert patient” mindset is helpful here: you want a plan that prioritises proportion, stability, and predictable healing.
What you can realistically expect to change
Most patients notice improvement in two areas: projection and contour. The biggest visible difference is often in photos, video calls, and side profiles.
- Reduced prominence with a natural ear-to-head distance (not pinned flat).
- Improved fold definition where it was weak or absent.
- Better visual symmetry when one ear has been more prominent than the other.
What you should not expect
Clear boundaries prevent disappointment. There are things otoplasty does not promise — and a trustworthy plan is honest about that.
- Perfect mirror-image ears: natural anatomy is never identical side to side.
- Instant final results: early swelling and stiffness can temporarily change how the ears look and feel.
- “Invisible” healing sensations: temporary numbness or sensitivity can be part of normal recovery.
Achieve the same high-standard, clinical excellence you expect in the UK or US, but without the premium price tag. Quality meets exceptional value at AKM Clinic.
When do results look “settled”?
Most patients see a meaningful change immediately, but the result continues to refine as oedema resolves and tissues mature. That is why early photos can be misleading, especially in harsh lighting.
- First 1–2 weeks: swelling and dressing effects can make ears look slightly different day to day.
- Weeks 3–6: contour becomes more natural as tissues soften and swelling reduces.
- After 6–12 weeks: many patients feel the result looks stable in typical photos and everyday life.
Scars: where they sit and how they usually heal
Otoplasty scars are typically placed behind the ear in the natural crease, so they are usually well concealed. Scar quality depends on skin type, healing behaviour, and aftercare. We discuss scar risk honestly, especially if you have a personal or family tendency toward thickened scarring.
- Typical location: behind the ear, within a natural fold.
- Early appearance: redness and firmness can be normal while scars mature.
- Long-term: scars usually fade and soften over time, but scar behaviour varies between individuals.
Is the result permanent? And what about revision?
For most patients, results are long-lasting. However, cartilage has “memory”, and a small risk of partial recurrence exists. That is exactly why technique choice, stabilisation, and protecting the ears during early healing matter.
- Long-term stability is the goal, supported by internal fixation and conservative contour design.
- Recurrence risk is uncommon but possible; we plan to reduce it and we explain how aftercare helps.
- Revision otoplasty may be considered if there is recurrence, asymmetry that does not settle, or contour concerns once healing is complete.
Receive a 100% transparent, all-inclusive quote tailored to your needs. No hidden fees—just world-class care at an accessible price.
Cost Analysis: Otoplasty Cost 2026 (UK vs Turkey)
UK patients often start with one practical question: “How much will this actually cost me?” The more useful question is slightly different: what am I paying for, and what does the fee include? With otoplasty, the headline price alone can be misleading. Technique, aftercare structure, anaesthesia planning, and revision capability all influence both the fee and the overall value.
What determines the cost of otoplasty?
Fees vary because the procedure is not identical for every ear. Even within the same patient, each side may require a slightly different plan to achieve balanced results. Factors that typically influence pricing include:
- Complexity of the anatomy: mild prominence vs combined fold and conchal correction
- Primary vs revision otoplasty: revision work is usually more complex due to scar tissue and cartilage behaviour
- Anaesthesia plan: local anaesthesia, twilight sedation, or general anaesthesia (where appropriate)
- Aftercare intensity: dressing schedule, follow-up structure, and recovery support
- Time in theatre: longer plans require more resources and monitoring
UK private fees vs Turkey: why the difference exists
Many UK patients notice that fees in Turkey can be more cost-effective compared to UK private care. This is often driven by broader operational costs (such as staffing and overheads) rather than a meaningful difference in the surgical goal. The important point is to judge any option by clinical standards and aftercare structure, not by price alone.
- UK private care: often reflects higher overheads and facility costs, especially in major cities
- Turkey: can offer a more cost-effective pathway while still focusing on quality and safety fundamentals
- Value focus: the strongest choice is the one with predictable planning, clear aftercare, and accountability
Understanding “all-inclusive” planning (what it should mean)
For international patients, the most helpful pricing model is transparent and structured. An all-inclusive approach should reduce guesswork and make it easy to compare options fairly. In our pathway, we aim to keep the process clear and practical for UK patients travelling to Istanbul.
Depending on your plan, an all-inclusive structure may cover:
- Consultation and planning: assessment, treatment plan, and pre-op guidance
- Clinical care: theatre, surgical team, monitoring, and standard consumables
- Aftercare: dressings/headband guidance and structured follow-up
- Travel logistics support: coordinated scheduling that helps you plan accommodation and transfers smoothly
We explain exactly what is included for your specific plan, and what is not, so you can compare like-for-like.
A simple comparison framework (so you can judge value, not just price)
If you are comparing the UK and Turkey, use a framework that protects you from “false comparisons”. Below is a practical way to evaluate the total proposition:
| What to compare | Why it matters | What to look for |
|---|---|---|
| Technique plan | Predictability and natural contour | Clear explanation of fold creation, projection control, and stabilisation |
| Anaesthesia pathway | Comfort and safety | Option explained and matched to your case (not a default) |
| Aftercare structure | Protects the result | Written guidance, headband plan, and clear check-in schedule |
| Revision capability | Accountability | Evidence of experience with complex outcomes and honest risk discussion |
| Total costs | True budget clarity | What’s included vs excluded (tests, medications, logistics, follow-up) |
Financial planning: making the decision rational
If you are planning treatment from the UK, we encourage you to think in terms of total predictability: the plan, the recovery, and the support once you return home. We are happy to outline the expected structure clearly so you can decide with confidence.
Finding The Best Otoplasty Surgeon: a UK “expert patient” checklist
Searching for the “best” otoplasty surgeon can quickly become noisy. A more reliable approach is to assess competence, planning quality, and accountability. Otoplasty is a detail-driven procedure: small technical choices can affect natural contour, long-term stability, and whether the result looks quietly normal.
Questions to ask in your consultation
A good consultation should feel specific to your ears, not generic. These questions help you understand whether the plan is truly individualised:
- What is causing the prominence in my ears: fold, concha, or both?
- Which techniques will you use, and why are they appropriate for my anatomy?
- How do you avoid over-correction and sharp contour edges?
- What is the realistic symmetry goal, and what limitations should I understand?
- What does aftercare look like week by week, and what are the rules that protect the result?
What genuine expertise looks like (without relying on marketing)
Expertise shows up in structure: precise explanations, measured promises, and a plan that prioritises natural contour. Look for:
- Anatomy-led planning: clear discussion of fold definition, projection points, and stabilisation strategy
- Balanced aesthetic judgement: aiming for proportion rather than “maximum pin-back”
- Risk literacy: open discussion of recurrence risk, scarring considerations, and how complications are managed
- Revision competence: comfort discussing revision scenarios and how they differ from primary surgery
Undergo your procedure with total confidence. Meet our European Board-certified surgeons, who have performed over 2,000 successful facial procedures.
How to read reviews and before/after photos intelligently
Reviews and images can be helpful, but they should not be the only decision driver. Use them to confirm consistency, not to chase a single “perfect” example.
- Look for consistency: similar natural contour across multiple outcomes, not just one standout image
- Check angles and lighting: harsh light can exaggerate swelling or contour edges early on
- Focus on profile and three-quarter views: these show projection changes most clearly
- Read for process, not praise: reviews that mention clarity, aftercare, and follow-up are more meaningful
Red flags that should make you pause
When safety and long-term predictability matter, certain signals should prompt caution:
- Overpromising (“perfect symmetry”, “no swelling”, “instant final results”)
- Vague or dismissive risk discussion
- No clear aftercare pathway or follow-up schedule
- Pressure-selling behaviour or rushed decision timelines
Why follow-up matters more than most patients expect
Otoplasty is not just a day in theatre. Early healing is when the result is most vulnerable to bending, pressure, and avoidable disruption. A structured follow-up plan helps you stay calm and consistent, especially when you return to the UK.
- Clear milestones for what is normal at each stage
- Direct guidance if swelling, redness, or discomfort changes unexpectedly
- Longer-term check-ins to assess settling and stability
From VIP airport transfers to 5-star hotel accommodation, we manage every detail. Enjoy a premier medical travel experience in Istanbul.
Your Medical Journey: From The UK To Istanbul With Us
Travelling for surgery should feel structured, not stressful. We organise the process so you know what happens, when it happens, and what you need to do at each stage. Our aim is simple: a calm experience, a clear plan, and a recovery pathway you can follow confidently once you are back in the UK.
Step 1: Online consultation and anatomy-led planning
We begin with a remote consultation focused on your ears, your goals, and your medical profile. This is not a generic “yes/no” call. We map your anatomy, discuss the likely technique approach, and explain what a natural result looks like for your face.
- Review of ear prominence pattern (fold, concha, or both)
- Discussion of realistic symmetry goals and natural contour priorities
- Medical screening questions and preparation guidance
- Clear outline of recovery rules that protect the result
Step 2: Travel coordination and a practical timeline
Once you decide to proceed, we help you plan dates around recovery practicality. The goal is not to rush — it is to choose a timeline that protects early healing and gives you breathing space for rest.
- Scheduling that avoids unnecessary pressure in the first week
- Guidance on what to bring (headband comfort items, loose clothing, pillow support)
- Clear expectations for activity, sleep position, and daily routines while travelling
Step 3: Arrival, pre-op review, and surgery day
In person, we confirm the plan and make sure nothing has changed medically since your remote assessment. We then proceed with the agreed pathway, keeping communication clear and measured throughout.
- In-person review of anatomy and final plan confirmation
- Anaesthesia plan review (local, twilight sedation, or general anaesthesia where appropriate)
- Post-operative instructions explained in plain English before you leave
Step 4: Post-op checks in Istanbul and “ready-to-travel” guidance
Before you travel home, we check progress and ensure you understand the next phase of aftercare. You will know what is normal, what is not, and what to do if something changes once you are back in the UK.
- Dressing/head support plan and hygiene instructions
- Comfort management guidance and normal healing milestones
- Clear red flags and escalation steps (what to message us about immediately)
Step 5: Follow-up once you are back in the UK
Healing continues after you travel. We support you with structured remote follow-up so you are not left guessing during the settling phase.
- Planned check-ins based on your case and progress
- Photo guidance for consistent, clinically useful updates
- Supportive advice if you need local assessment in the UK
If you would like a clear otoplasty plan based on your anatomy, you can request an online consultation.
Ear Correction Surgery Frequently Asked Questions (FAQ):
What is otoplasty?
Otoplasty is a surgical procedure that reshapes and repositions the outer ear (pinna) to reduce prominence and improve contour. It can involve fold creation, projection reduction, or a combined approach depending on anatomy.
Otoplasty vs pinnaplasty: which term should I use?
In the UK, “pinnaplasty” often refers to ear pinning (reducing projection). “Otoplasty” is the broader medical term and can include both repositioning and reshaping. What matters is the technique plan, not the label.
Is otoplasty permanent?
Results are typically long-lasting. Cartilage has “memory”, so stabilisation technique and early aftercare (protecting the ears from bending and pressure) are important to reduce the risk of partial recurrence.
Is otoplasty safe?
Otoplasty is generally considered safe in suitable patients when performed with appropriate planning, sterile standards, and structured aftercare. As with any surgery, risks exist and should be discussed clearly.
What are the risks of otoplasty?
Possible risks include infection, haematoma, wound healing issues, scarring concerns, contour irregularities, asymmetry, and (uncommonly) partial recurrence. We explain what to watch for and when to contact us.
What is the recovery time for otoplasty?
Many patients return to desk-based work within around 1–2 weeks depending on comfort and dressing schedule. The ears continue to settle over several weeks as swelling (oedema) resolves and tissues mature.
What does otoplasty recovery look like day by day?
Expect the most swelling and tightness in the first few days, with steady improvement across the first two weeks. Minor day-to-day variation is normal early on, especially between sides.
How do I sleep after otoplasty?
Sleeping on your back with slight head elevation is typically recommended at the start. Avoid side-sleeping until advised, and protect the ears from bending or pressure during early healing.
Will otoplasty affect my hearing?
No. Otoplasty changes the outer ear’s shape and position and does not alter the inner ear or hearing function.
Will there be visible scars?
Scars are typically placed behind the ear in the natural crease and are usually well concealed. Scar behaviour varies by individual, and we discuss this transparently if you have a tendency to thickened scarring.
When can I exercise again?
Light activity may be possible relatively early, but vigorous exercise and contact risk should be avoided until tissues are stable. We give practical guidance based on your procedure plan and healing progress.
When will I see my final result?
You will see a change immediately, but the result continues to refine as swelling settles and tissues soften. Many patients feel the outcome looks fully “settled” over 6–12 weeks, with continued subtle maturation beyond that.
Do I need revision otoplasty?
Most patients do not. Revision may be considered if there is partial recurrence, persistent asymmetry that does not settle, or contour concerns once healing is complete. We focus on planning that reduces avoidable revision risk.
How much does otoplasty cost?
Fees vary based on anatomy, technique, anaesthesia plan, and whether the procedure is primary or revision. We explain what is included in your plan so you can compare options fairly and rationally.
Medical Disclaimer
This information is provided for general educational purposes and does not replace a medical consultation. Surgical suitability, technique choice, risks, recovery time, and outcomes vary by individual anatomy and health factors. A formal assessment by a qualified clinician is required to determine the appropriate plan for you. If you have urgent symptoms (such as rapidly worsening pain, significant swelling/pressure, fever, or signs of an allergic reaction), seek immediate medical care.
Otoplasty: Patient Stories

Sarah

Otoplasty Surgeons
Otoplasty Cost in Turkey
Starting from ~ £2400
* There are no hidden fees or unexpected charges.
- Your PersonalisedOtoplastyProcedure
- All Specialist Surgeon & Anaesthesia Fees
- All Pre-Op Tests & Post-Op Check-ups
- 5-Star Hotel Accommodation (incl. breakfast)
- All Private VIP Airport & Clinic Transfers
- 24/7 Dedicated Patient Coordinator & Translation Services
Otoplasty: A Cost Comparison
| City | Cost |
|---|---|
| London | ~ £7,500 GBP |
| Manchester | ~ £7,000 GBP |
| Bristol | ~ £6,500 GBP |
| Cardiff | ~ £6,700 GBP |
| Edinburgh | ~ £6,200 GBP |
Otoplasty: Patient Reviews
Jammal Canada
I have had face and neck lift with AKM Clinic they have been so good to me and my operation went so smoothly🥰 i would like to thank my doctor here and also to the team 💐

Ava Canada
Thank you AKM Clinic for giving me my confidence back! Had facelift + temporal lift 3 months ago and the outcome is already stunning. Special thanks to Hande!

Jakayla USA
Had a deep plane facelift and lower eyelid procedure at AKM Clinic 7 months ago. The results are fantastic - very subtle and natural. I didn’t expect the entire experience to be so comfortable. Hande managed everything and kept in contact even after I returned to USA. I’m beyond pleased with the outcome and the care I received. Would do it again in a heartbeat!

Barbara United Kingdom
It has been 4 months since my surgery. Everything is great, The most important thing is l love the way l look, l look exactly how l wanted. Meaning l look natural, just almost 40 years younger. I pulled Facebook - majority voted 37ys. I also had face, neck, chest, and hands CO2 laser. My skin is flawless.

Lisa Canada
I had a face, neck and arm lift at AKM. I’m just over 4 weeks post and couldn’t be happier with the results. The entire experience was wonderful! My coordinator, Khadija made me feel comfortable from beginning to end! I highly recommend AKM and will definitely go back for other procedures!

Julie USA
I am beyond grateful I went with AKM Clinic for my deep plane face and neck lift, upper eyelid, and co2 laser. Dr. Akif has magic hands and my results are truly incredible! I came from the US and assistant Emine was the best in assuring every detail was coordinated and communicated with me beyond my expectations every step of the way. 10 out of 10 to the entire team! I couldn’t be more pleased!

Ready to Begin Your Own Transformation Journey?
Join the 2,000+ patients who have trusted Dr Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, naturally restored you begins with a simple, no-obligation conversation. Contact us today from the UK for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. There are no hidden fees.
#2: Secure Your Date & VIP Booking
Once you are ready, our dedicated patient coordinators will help you secure your procedure date. We will handle all your bookings, including your 5-star hotel accommodation and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you will meet your specialist surgeon to finalise the details for your natural, subtle, and restored new look.







