BBL Implants vs Fat Transfer: Safety Comparison

- BBL implants vs fat transfer safety depends on anatomy, surgeon technique, and clinic protocols—not trends.
- Fat transfer risks include rare high-stakes embolism; implants carry infection, malposition, and revision considerations.
- Best candidate selection aligns donor fat, goals, and health factors to reduce complications and improve predictability.
- Recovery and aftercare drive outcomes: follow-ups, mobility, sitting guidance, and early warning sign awareness.
Summary generated by AI, fact-checked by our medical experts
If you’re researching bbl implants vs fat transfer, you’re probably not just chasing a “bigger” result—you’re trying to make the safest, most predictable decision for your body. That’s the right instinct. In medical science, “safer” is rarely a single yes/no label; it’s a risk profile shaped by your anatomy, surgical technique, anesthesia planning, and post-op care.
This guide breaks down what each option really involves, how their complications differ, and how to think like an “expert patient” when choosing a surgeon and clinic. You’ll also see the common search comparisons patients make—fat transfer vs bbl implants, bbl vs fat transfer, fat transfer vs bbl, bbl surgery vs fat transfer, and hip fat transfer vs bbl—translated into practical safety questions.
Key takeaway: “Safety” isn’t just what happens in the operating room. It’s what happens before surgery (candidate selection), during surgery (technique + monitoring), and after surgery (aftercare and early complication detection).
Table of Contents
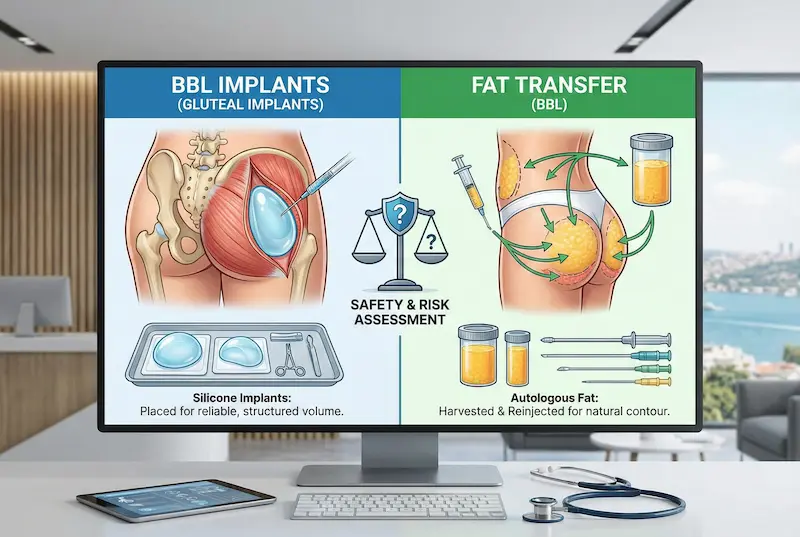
Quick Definitions: What Are BBL Implants and Fat Transfer (Brazilian Butt Lift)?
Before you compare safety, you need clarity on what’s actually being done to your body. Both approaches aim to improve projection and contour, but they do it in very different ways—one by placing a medical implant, the other by transferring your own fat. That difference drives most of the safety conversation.
BBL Implants (Gluteal Implants) in Simple Terms
BBL implants (gluteal implants) involve placing a silicone implant—designed for the buttock area—through an incision (commonly hidden in the crease). The implant is positioned in a specific tissue plane chosen by the surgeon. The goal is a reliable volume increase, especially in patients who don’t have enough donor fat for transfer.
Fat Transfer / Traditional BBL in Simple Terms
Fat transfer BBL uses liposuction to harvest fat (often from the abdomen, waist, back, or thighs), processes that fat, then reinjects it into the buttocks to create shape and projection. Many patients also ask about hip fat transfer vs bbl; clinically, “hip fat transfer” is usually part of a fat-transfer BBL plan—fat is placed not only in the central buttock, but also into hip dips/outer hips to improve silhouette.
Key Differences at a Glance (Material, Technique, Goals)
| Feature | Fat Transfer (BBL) | Gluteal Implants |
|---|---|---|
| What adds volume? | Your own fat | Medical-grade silicone implant |
| Who tends to be a candidate? | Patients with adequate donor fat | Patients with low body fat or very specific volume goals |
| Most discussed “headline” safety issue | Fat embolism risk (technique-dependent) | Implant-related infection/displacement/capsular issues |
| Result style | Softer, often more natural transitions | More structured projection; shape depends on pocket + implant |
| Predictability of volume | Some fat resorption is expected | More consistent “volume retained” |
The Safety Conversation: Why These Two Options Have Different Risk Profiles
When patients search “fat transfer vs bbl implants” or “bbl surgery vs fat transfer,” they often assume one is inherently safe and the other isn’t. The reality is more nuanced. Both can be performed responsibly, but the type of risk differs—because the body responds differently to injected fat than it does to an implanted device.
What “Safety” Actually Means in Body Contouring (Short vs Long-Term)
From a scientific research standpoint, it helps to separate safety into two buckets:
- Short-term safety: surgical and anesthesia risks, bleeding, infection, wound healing, blood clots, and technique-specific risks (like fat embolism in fat transfer).
- Long-term safety: the stability of results and the probability of future interventions (revision surgery), such as implant malposition or capsular contracture (implants), or contour irregularities/asymmetry after fat resorption (fat transfer).
Risk Drivers: Anatomy, Technique, and Patient Factors
Two patients can undergo the “same” procedure and have very different outcomes because risk is influenced by:
- Anatomy: tissue thickness, vascular anatomy, prior scars/surgeries, and skin quality.
- Technique: for fat transfer, safe injection planes and cannula strategy; for implants, pocket selection, sterile handling, and tension-free closure.
- Patient factors: smoking/vaping, diabetes, anemia, clotting history, BMI extremes, medication/supplement use, and ability to follow post-op instructions.
Why Surgeon Experience and Facility Standards Matter More Than Marketing
If you’re trying to decide between bbl vs fat transfer, the safer choice is often the one that matches your anatomy and is performed in a system built for safety: appropriate licensing, strict sterilization protocols, trained anesthesia monitoring, and a structured aftercare plan. “Discount” pricing should never replace documented standards.
Expert-patient mindset: Ask “What is your safety protocol for prevention, early detection, and rapid response to complications?” A credible team can answer clearly—without defensiveness.
Safety Comparison: Most Common Complications (Side-by-Side)
When people compare fat transfer vs bbl implants, they often want a simple verdict. A more useful approach is to compare what can go wrong, how often issues are mild vs serious, and which complications are most influenced by surgical technique. This is where “safety” becomes practical—not fear-based.
Fat Transfer Risks (e.g., Fat Embolism, Infection, Asymmetry, Fat Necrosis)
A fat-transfer BBL (often searched as bbl vs fat transfer or fat transfer vs bbl) has a unique risk profile because fat is injected into a region with important blood vessels and deep anatomy.
- Fat embolism (most serious, technique-dependent): The key safety principle is avoiding unsafe injection depth/planes and using careful technique. This complication is rare but high-stakes, which is why surgeon training and strict protocols matter.
- Infection: Any surgery carries infection risk. With fat transfer, infection may involve liposuction sites or injection sites.
- Fat necrosis / lumps: Some transferred fat may not survive. This can create firm areas, small nodules, or irregular texture.
- Asymmetry / uneven volume retention: A portion of fat resorption is expected, which can lead to side-to-side differences.
- Seroma / fluid collections: More commonly tied to liposuction areas.
Implant Risks (e.g., Capsular Contracture, Displacement, Infection, Revision Surgery)
Gluteal implants are a medical device placed into tissue. Device-based surgery tends to have more “mechanical” and long-term maintenance considerations—one reason some patients searching bbl surgery vs fat transfer are concerned about future revision.
- Infection (higher consequence when a device is involved): If an implant becomes infected, treatment can be more complex and may require removal.
- Capsular contracture: The body forms a capsule around implants; in some cases it can tighten, affecting comfort and shape.
- Displacement / malposition: The implant can shift if the pocket is not ideal, if tissue support is limited, or if post-op restrictions are not followed.
- Wound healing issues: Incisions in high-movement areas can be vulnerable if there is tension, moisture, or friction.
- Need for revision: Revisions may be needed for position, symmetry, discomfort, or aesthetic goals over time.
Which Complications Are Rare vs. Which Are More Likely?
From a medical science perspective, it helps to separate “headline risk” from “everyday risk.”
- Fat transfer: The “headline” risk is fat embolism (rare but severe), while more “everyday” issues are uneven retention, lumps/fat necrosis, and minor asymmetry.
- Implants: Severe complications are less often about injection-plane anatomy and more about infection management, implant malposition, wound healing, and longer-term revision probability.
| Risk Category | Fat Transfer BBL | BBL Implants |
|---|---|---|
| Highest-stakes “signature” risk | Fat embolism (technique-dependent) | Deep infection or major wound issues (device-related complexity) |
| Common “quality-of-result” issues | Resorption, asymmetry, fat necrosis/lumps | Malposition, visible edges in thin tissue, firmness |
| Long-term considerations | Stability depends on fat survival + lifestyle | Device maintenance mindset; revision sometimes needed |
Bottom line: If a clinic can’t clearly explain how they reduce technique-driven risks (fat transfer) or device-driven risks (implants), the “safety comparison” is already decided—look elsewhere.
Candidate Selection: Who Is a Better Fit for Each Option?
Most safety problems start with the wrong procedure for the wrong patient. A careful consultation should feel like a screening process—not a sales pitch. If you’re comparing bbl implants vs fat transfer, candidate selection is the real foundation of safety and natural-looking outcomes.

When Fat Transfer Is Typically Preferred
Fat transfer is commonly preferred when you have enough donor fat and want a softer, more natural transition. It also allows contour improvement in the areas where fat is harvested (abdomen/waist/back/thighs), which is why many patients like the “two-in-one” effect.
- Adequate donor fat: Without enough harvestable fat, results may be limited or require staged procedures.
- Preference for natural tissue: No implanted device; the goal is living tissue integration.
- Shape goals include hips: Many “hip fat transfer vs bbl” searches reflect a desire to address hip dips/outer hips for a smoother silhouette—fat transfer can be planned to target these zones.
When Implants Become a Consideration (Low Body Fat, Specific Shape Goals)
Implants may be considered when you are very lean or when the desired projection isn’t realistically achievable with fat transfer alone. In these cases, the safety discussion should include device-specific realities: implant pocket planning, infection prevention, and a clear revision strategy if needed.
- Low body fat / limited donor sites: If liposuction harvest would be too aggressive or unsafe, implants may offer volume.
- Highly structured projection goal: Some patients want a very defined projection that may be difficult with fat alone.
- Understanding the “device mindset”: Implants can be long-lasting, but they are not “set-and-forget.” You should be comfortable with the idea of long-term follow-up and potential revision.
Red Flags: Who Should Avoid Surgery or Delay It
Whether you’re leaning toward bbl vs fat transfer or bbl implants vs fat transfer, certain factors increase risk and may justify delaying surgery until optimized:
- Smoking/vaping: Strongly linked to wound-healing problems and infection risk.
- Uncontrolled diabetes or poor nutritional status: Raises infection and healing complications.
- History of blood clots or high clot risk: Requires specialist clearance and strict prevention planning.
- Unrealistic expectations or body-image distress: Safety includes psychological readiness.
- Inability to follow post-op restrictions: Sitting protocols, mobility guidance, and hygiene matter—especially for implants and for fat survival.
Expert-patient question: “If I’m not an ideal candidate today, what would you recommend I change before surgery—and why?” A trustworthy surgeon answers this clearly, even if it means postponing.
The Decision Tree: Find Your Perfect Match
Follow this simple step-by-step flow to see which procedure medical logic points you toward based on your unique body type.
Step 1: The “Pinch” Test (Donor Fat)
Do you have pinchable, excess fat on your abdomen, flanks (love handles), back, or thighs?
- 👉 Yes, I have stubborn fat I want gone: Proceed to Step 2.
- 👉 No, I am very lean / athletic (Low BMI): Your body likely cannot provide enough fat for a noticeable transfer. You are a strong candidate for Butt Implants.
Step 2: The Shape Goal
What kind of transformation are you looking for?
- 👉 I want a dramatic, highly projected, and structured curve: Implants provide guaranteed, firm projection regardless of your natural fat. Lean towards Butt Implants.
- 👉 I want a softer, natural curve and I want my waist/stomach snatched at the same time: Fat transfer allows the surgeon to sculpt your entire torso (Lipo 360) while enhancing your buttocks. Proceed to Step 3.
Step 3: The Maintenance Mindset
How do you feel about long-term maintenance?
- 👉 I want natural, living tissue. I understand I must maintain my weight for the fat to stay: You are the perfect candidate for a traditional Fat Transfer BBL.
- 👉 I want a permanent size that doesn’t fluctuate with my diet, and I am okay with having a medical device in my body: You align better with Butt Implants.
Results, Longevity, and Revision Rates: “Safer” Also Means “More Predictable”
For many expert patients, “safety” isn’t only about avoiding major complications—it’s also about avoiding avoidable revisions, prolonged recovery, or a result that doesn’t age well. That’s why comparisons like bbl implants vs fat transfer (and the variations fat transfer vs bbl implants / bbl vs fat transfer) should include predictability over time, not just what happens on surgery day.
Shape Outcomes: Natural Look vs. Structured Projection
Fat transfer tends to create softer transitions because the added volume is living tissue distributed in a sculpted pattern. This can be especially appealing if your goal includes contouring the outer hip area (often searched as hip fat transfer vs bbl) to smooth hip dips and improve overall silhouette.
Implants can deliver a more “engineered” projection—useful for very lean patients or those wanting a more defined shape. However, the final look depends heavily on pocket design, implant size/shape selection, and how well your tissue can camouflage the implant edges.
Longevity: Fat Retention vs. Implant Durability
- Fat transfer longevity: A portion of transferred fat typically does not survive. The fat that does survive can be long-lasting, but outcomes can still fluctuate with weight changes. Your post-op protocol (sitting strategy, activity timing, nutrition, and smoking avoidance) influences fat survival.
- Implant longevity: Implants are designed to be durable and can provide stable volume. But “durable” isn’t the same as “maintenance-free.” Over years, some patients may face implant-related issues (position changes, capsular concerns, discomfort) that lead to revision.
In practical terms, fat transfer vs bbl often comes down to this: fat transfer can be more “biologic,” while implants can be more “structural.” Neither is automatically “safer” without matching the method to the right candidate and surgical plan.
Common Reasons for Revision (Both Methods)
Revision isn’t always a failure—sometimes it’s a predictable tradeoff. But it’s important to know what drives it:
- Fat transfer revisions: uneven retention, under-correction, asymmetry, palpable fat necrosis, or the desire for more volume (sometimes a staged approach is safer than one aggressive session).
- Implant revisions: malposition/displacement, discomfort, capsular contracture concerns, visible implant edges in thin tissue, or infection-related management.
Expert-patient framing: Ask your surgeon, “What is the most common reason you see patients needing a revision for this exact method—and how do you reduce it from the beginning?”
Ready to Consult with an Expert?
Whether the decision tree pointed you toward the holistic sculpting of a Fat Transfer BBL or the structured projection of Gluteal Implants, the ultimate decision requires a surgeon’s anatomical assessment. Send us your photos for a free, confidential evaluation. Our board-certified body contouring experts at AKM Clinic will tell you exactly which option is safest and most effective for your unique frame.
Frequently Asked Questions (FAQ): BBL Implants vs Fat Transfer
Below are concise, safety-focused answers to the questions patients most commonly ask when comparing bbl implants vs fat transfer—including variations like fat transfer vs bbl implants, bbl vs fat transfer, fat transfer vs bbl, bbl surgery vs fat transfer, and hip fat transfer vs bbl.
Which is safer overall: BBL implants or fat transfer?
There isn’t a single “always safer” answer. Fat transfer has a rare but high-stakes, technique-dependent risk (fat embolism), while implants carry device-related risks such as infection complexity, malposition, and the potential for revision. The safer option is the one that matches your anatomy and is performed by an experienced team with clear safety protocols and structured follow-up.
Can a skinny patient get a BBL without implants?
Sometimes—if there is enough donor fat in selected areas (even modest amounts) and expectations are realistic. In very lean patients, pushing for aggressive liposuction harvest can be counterproductive or unsafe. A reputable surgeon may recommend a staged plan, modest fat transfer, or implants if donor fat is truly insufficient.
What is the biggest risk of fat transfer BBLs, and how is it reduced?
The most serious risk discussed in medical science is fat embolism, which is strongly influenced by injection technique and anatomical safety principles. Risk reduction relies on strict adherence to safe injection strategy, careful patient selection, and a clinic culture that prioritizes safety over “maximum volume in one session.”
Do gluteal implants feel natural?
Some patients find implants feel firm compared to natural tissue, especially in thin individuals where there is less soft-tissue coverage. Comfort and “natural feel” depend on implant selection, pocket planning, tissue thickness, and healing quality.
How long do results last for implants vs fat transfer?
Fat transfer results depend on fat survival and long-term weight stability; some resorption is expected early on, and the surviving fat can be long-lasting. Implants provide stable volume, but they are a medical device—long-term follow-up is important and some patients may need revision over time.
What is the typical recovery time for each option?
Both procedures typically require several weeks of activity modification. Fat transfer often involves strict sitting strategies to support fat survival, while implant recovery focuses heavily on incision/pocket protection and monitoring for wound issues. Many patients feel “more functional” within weeks, but shape stabilization can take a few months.
How do I reduce my risk of complications when traveling for surgery?
Choose the team, not the deal: prioritize documented standards, qualified anesthesia care, and a clear complication-response pathway.
Get a real pre-op workup: labs, medical history review, medication/supplement guidance, and clot-risk screening.
Follow aftercare exactly: sitting protocol, wound hygiene, mobility guidance, and scheduled follow-ups.
Know your red flags: fever, worsening redness/drainage, sudden one-sided swelling, calf pain/swelling, chest pain, or shortness of breath (urgent evaluation).
Medical Disclaimer: This page is provided for general educational purposes only and does not replace a face-to-face medical consultation, diagnosis, or personalised treatment plan. All surgery carries risks and outcomes vary between individuals. Suitability for a BBL brazilian butt lift, procedure selection, and anaesthesia choice can only be determined after a full clinical assessment by a qualified surgeon. Always follow your clinician’s instructions and seek urgent medical attention if you develop concerning symptoms during recovery.
Related Treatments
Ready to Start Your Own Transformation Journey?
Join the 2,000+ patients who trusted Dr. Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, revitalized you begins with a simple, no-obligation conversation. Contact us today from the USA for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. No hidden fees.
#2: Secure Your Date & VIP Booking
Once you're ready, our dedicated patient coordinators will help you secure your procedure date. We'll handle all your bookings, including your 5-star hotel and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you'll meet your specialist surgeon to finalise the details for your "natural, subtle, and revitalized" new look.



















