Is BBL Safe? A Surgeon-Led Guide to Ultrasound-Guided BBL Safety

- Is BBL safe depends on technique, not geography — modern ultrasound-guided injection and subcutaneous-only placement dramatically reduce fat embolism risk.
- Common BBL myths about Turkey (cheap = low quality, non-board-certified surgeons, poor hygiene) are debunked by EBOPRAS certification and JCI-accredited hospital standards.
- Safe BBL surgery requires verifiable patient selection, anesthesia-team accountability, conservative volume goals, and first-24-hour post-op monitoring — not marketing claims.
- Recovery safeguards include structured mobility, hydration, DVT prevention, HBOT/LLLT support, and a clear "fit-to-fly" clearance before flying home to the US.
Summary generated by AI, fact-checked by our medical experts
If you’re researching “is BBL safe,” you’re not being paranoid—you’re doing the right thing. A Brazilian Butt Lift can deliver natural-looking contour when done correctly, but the margin for error is smaller than many patients realize. The procedure became known as a higher-risk cosmetic operation for reasons we’ll unpack honestly here.
For the procedure itself—steps, anatomy, recovery, what’s included—our BBL surgical reference covers the full overview. This article focuses specifically on the safety question.
People searching phrases like “is a BBL safe,” “is BBL surgery safe,” “how safe is BBL surgery,” or “is getting a BBL safe” are usually trying to answer one question: What has actually changed in modern BBL safety—and how can I verify it?
Two important notes before we begin:
- This article is about Brazilian Butt Lift surgery (fat transfer to the buttocks). Some patients also use “BBL” to mean broadband light skin treatments; that’s a different topic and has different pregnancy considerations.
- No technique can make BBL “risk-free.” What modern standards can do is reduce avoidable risk through better planning, better intraoperative control (including ultrasound), safer technique, and stricter aftercare. If you want a full overview of the procedure itself — techniques, recovery timeline, and what’s included — see our detailed Brazilian Butt Lift in Turkey guide.
Key takeaway: The biggest safety question isn’t “Which country?” It’s which standards and which technique are used—consistently, verifiably, and with the right safety infrastructure.
Table of Contents
Is BBL Safe? Understanding Why the Procedure Became “High-Risk”
To understand what “safe BBL surgery” really means, you have to understand what made BBL risky in the first place. The procedure combines two operations in one: liposuction (harvesting fat) and fat grafting (re-injecting purified fat). Each step can be done safely—but the danger historically centered on how and where fat is injected. For a step-by-step walkthrough of how modern BBL surgery in Turkey combines these two steps with safety protocols, see our full procedure guide.
The real danger: fat embolism (explained in plain English)
The most feared complication discussed in BBL safety is fat embolism. In simple terms, it’s when fat enters the bloodstream and travels to the lungs, where it can block blood flow. This is rare, but it can be life-threatening. The risk is closely tied to anatomy and injection depth—which is why modern “safe BBL technique” focuses so heavily on controlling the plane of injection.
Intramuscular vs. subcutaneous fat placement—why the “plane” matters
The buttock area has multiple tissue layers. From a safety standpoint, the critical issue is avoiding unsafe depth. Many modern safety approaches emphasize placing fat in the subcutaneous layer (the layer beneath the skin and above the muscle) rather than deep within muscle. This is one of the reasons ultrasound guidance became a major conversation: it helps reduce “guesswork” about where the cannula tip is at the moment of injection.
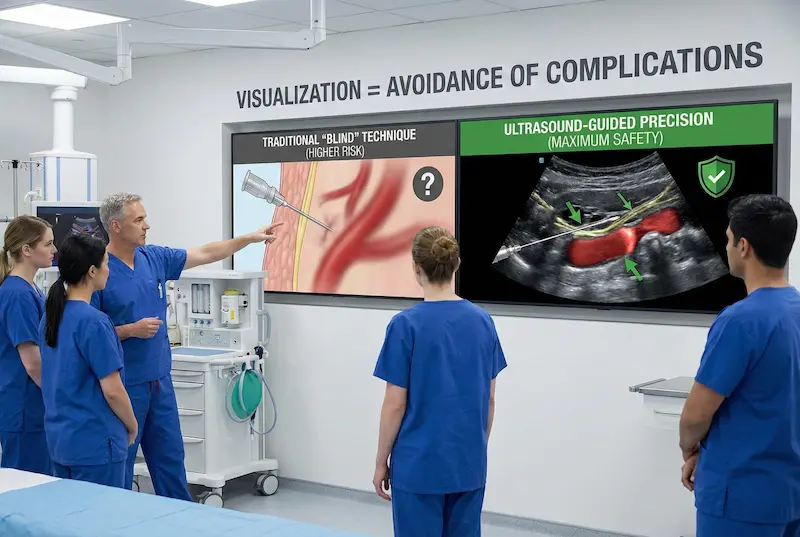
Technique and pressure: how mistakes happen
Even with a skilled surgeon, BBL can become risky when technique becomes aggressive or uncontrolled—especially if the injection is effectively “blind.” Risk can increase with:
- Poor tip awareness (not knowing exactly where the cannula is in real time)
- Uncontrolled depth changes during repositioning or difficult anatomy
- Excessive force/pressure while injecting
- High-volume goals that push beyond what the patient’s tissues can safely accommodate
This is why modern safety is not just about “experience.” It’s about standardized, repeatable controls—and why ultrasound-guided approaches gained momentum.
Risk multipliers: when a “normal” case becomes a higher-risk case
Patients searching “is it safe to get a BBL” often don’t realize that risk isn’t identical for everyone. A case can become higher-risk when multiple factors stack together, such as:
- Very high BMI or significant medical comorbidities
- Smoking/nicotine use (impairs healing and increases complication risk)
- Very large volume transfer goals (“as big as possible” plans)
- Combining multiple major surgeries in one session without appropriate safeguards
- Inadequate post-op monitoring—especially relevant for medical tourism patients
| Safety Driver | Why It Matters | What a “Safer Standard” Looks Like |
|---|---|---|
| Injection depth control | Depth is directly linked to the most serious BBL risks | Clear plane strategy + methods that reduce “blind” injection (often including ultrasound) |
| Volume goals | Chasing extreme size can push tissues beyond safe limits | Realistic planning based on anatomy, skin quality, and fat availability |
| Team + facility readiness | Safety depends on monitoring, protocols, and emergency capability | Hospital-grade standards, anesthesia safety, and a documented complication pathway |
| Aftercare + observation | Many complications are time-sensitive—early detection matters | Structured follow-up, mobility guidance, and clear escalation rules |
In the next section, we’ll get very specific about what ultrasound-guided BBL means, what it can realistically improve, and what questions you should ask to verify whether a clinic truly follows modern safety standards—whether you’re looking for safe BBL Turkey options or evaluating any provider globally.
What Is an Ultrasound-Guided BBL?
When patients ask “is BBL surgery safe” or “how safe is BBL surgery”, they’re often really asking whether the procedure is still being performed “by feel” (blind) or with modern safeguards that reduce avoidable risk. One of the biggest shifts in the last decade has been the rise of the ultrasound-guided BBL.
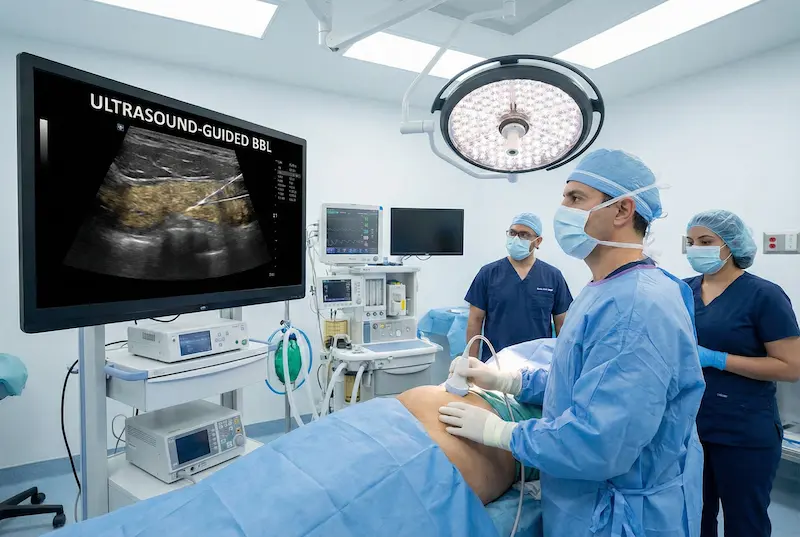
An ultrasound guided BBL uses real-time imaging during the fat-transfer step to help the surgeon verify where the cannula tip is positioned at the moment fat is injected. The goal is not to “add a gadget.” The goal is to make the most safety-critical part of the operation less dependent on estimation—a principle strongly supported by medical science.
Think of it like headlights in fog: ultrasound doesn’t guarantee a perfect drive, but it can reduce the risk of “driving blind” in the most dangerous moments.
How intraoperative ultrasound works (what it can and can’t show)
Ultrasound is an imaging method that allows a trained operator to see tissue layers in real time. During fat grafting, the ultrasound probe is placed on the skin while the surgeon advances the cannula underneath. On the screen, the team can observe:
- Tissue layers (helping distinguish superficial fat layers from deeper structures)
- Cannula position and movement (to confirm where the tip is as the injection is performed)
- Consistency of the injection plane across different zones of the buttocks
What it cannot do is make an unsafe plan safe. Ultrasound is most valuable when paired with an already sound approach: proper patient selection, conservative volume goals, correct cannula choice, controlled technique, and a facility equipped for surgical safety.
What the surgeon is verifying in real time
If you’ve ever wondered “is getting a BBL safe”, here’s what “real-time verification” is trying to accomplish during the critical minutes of fat transfer:
- Confirming the injection depth matches the planned safe BBL technique (staying in the intended layer consistently)
- Reducing unintentional depth changes that can happen with repositioning or challenging anatomy
- Improving team standardization so safety is not dependent on a single person’s “feel” on a single day
This is why modern conversations about safe BBL surgery increasingly include ultrasound—not as marketing, but as a tool that supports safer execution of a safer plan.
Does ultrasound guidance add time/cost—and why that tradeoff matters
In many practices, ultrasound-guided fat transfer can add steps and time to the procedure because it requires:
- Equipment availability and proper maintenance
- A trained operator (often the surgeon and/or a dedicated team member)
- Deliberate, methodical injection rather than “rushed volume”
From a patient perspective, the right question isn’t “Is it faster?” The right question is: Does the clinic prioritize a safety-first workflow even if it’s slower? That’s one of the practical differences between a clinic that sells a “safe BBL package” and a clinic that actually follows safety standards as a non-negotiable baseline.
“Ultrasound-assisted” vs. “ultrasound-guided”: terminology patients should clarify
If you’re looking into safe BBL Turkey options (or any location), the words on a website can be vague. These terms are not always used consistently:
- Ultrasound-guided bbl typically implies ultrasound is used during fat injection to visualize the cannula tip and confirm the plane while injecting.
- Ultrasound-assisted bbl may mean ultrasound is used for other steps (for example, pre-op assessment) or only in selected moments—not necessarily throughout fat transfer.
What to ask (and what a confident clinic should answer clearly):
- Do you use ultrasound guidance for every BBL fat injection or only in “some cases”?
- Who performs the injection, and who is responsible for the ultrasound visualization?
- What layer do you target, and how do you confirm you remain there throughout?
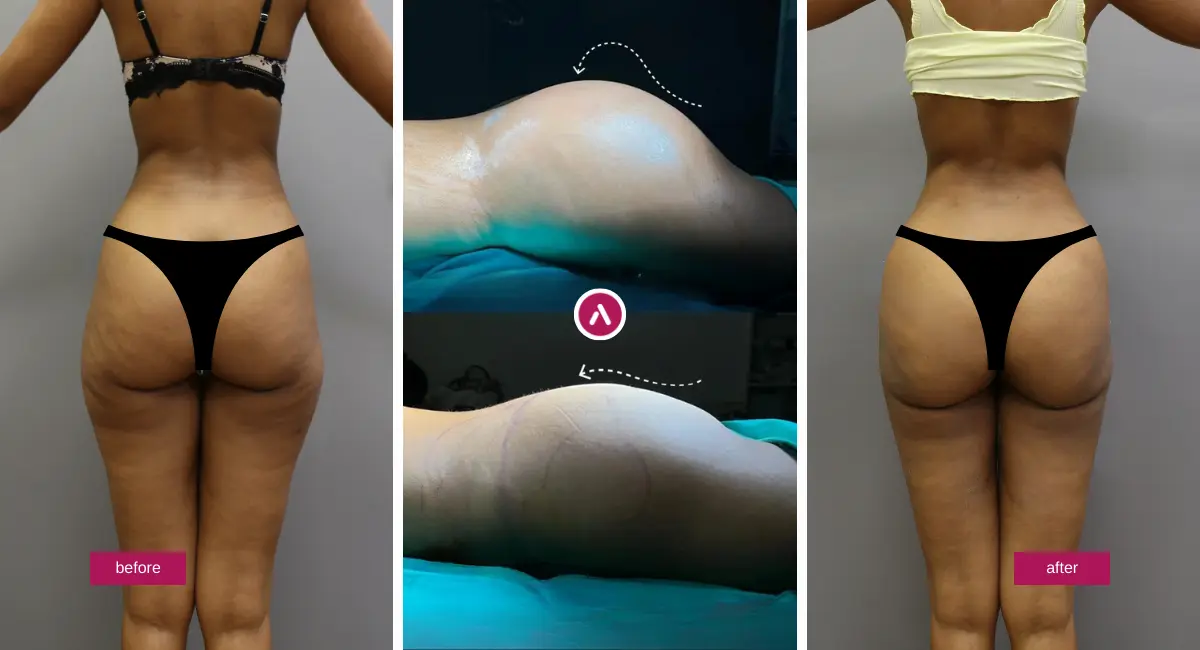
These three cases are a fraction of what natural BBL results look like across different ages, BMIs, and donor profiles. If you want broader context — multiple body types, varied projection goals, post-op timeline progression — our full BBL before-and-after gallery shows the range.
A quick note on “Awake BBL”: is awake BBL safe?
Some patients search “is awake BBL safe” or “awake BBL surgery”. This usually refers to BBL performed without full general anesthesia—often with local anesthesia and sedation protocols. “Awake” can mean different things, and it’s not automatically safer or riskier by itself.
Safety depends on:
- Patient selection (medical history, anxiety tolerance, procedure complexity)
- Anesthesia team and monitoring (airway safety, vital sign monitoring, emergency readiness)
- Surgical plan and duration (long, complex combined procedures can increase overall risk regardless of anesthesia type)
So if your core question is “is it safe to get a BBL”, don’t treat “awake” as a shortcut to safety. Treat it as a clinical decision that must be individualized.
The “awake” question gets emotional fast — patients either treat it as a safety guarantee or dismiss it entirely. Neither view is right. What matters is whether the awake protocol is paired with the right candidate, the right monitoring, and realistic volume goals. Done well, it can offer different recovery dynamics; done poorly, it carries the same risks as any BBL.
Real awake BBL outcomes—what natural projection actually looks like and which clinic factors drive results—are documented in our awake BBL outcomes guide.
Here’s a practical comparison of how the two approaches differ from a safety perspective:
| Feature | General Anesthesia BBL | Awake BBL (Local + Sedation) |
|---|---|---|
| Muscle relaxation | Muscles fully relaxed | Muscle tone preserved (acts as barrier) |
| Patient feedback | None (patient unconscious) | Patient can feel and react to deep probing |
| Systemic stress | Higher (respiratory/cardiac load) | Minimal (bypasses full systemic anesthesia) |
| Post-op nausea | Common | Rare |
| Early mobility | Slower (grogginess, nausea) | Faster (walk out shortly after) |
| Selection suitability | Broader (including complex/combined cases) | Requires careful candidate screening |
This comparison doesn’t mean one approach is “always safer” than the other — it means the right choice depends on your medical profile, procedure scope, and the clinic’s monitoring capabilities. A safety-first clinic will recommend the method that fits you, not the one that fits their default workflow.
How Ultrasound Has Changed the Modern Safety Standards
If you’re asking “is BBL safe” in 2026, the most important shift to understand is this: modern safety is moving away from “trust my hands” and toward verifiable intraoperative control. Ultrasound didn’t change the goal of a Brazilian Butt Lift (BBL)—it changed the standard of proof that the fat is being placed where the plan says it should be placed.
In other words, the question “how safe is BBL surgery” increasingly depends on whether a clinic can demonstrate a safe BBL technique that is consistent, repeatable, and documented—not just promised.
Here’s where the recent evidence becomes hard to ignore. A 2025 systematic review and meta-analysis published in the Aesthetic Surgery Journal — the official journal of the American Society for Aesthetic Plastic Surgery — pooled data from 6,235 patients undergoing ultrasound-guided gluteal fat grafting. The conclusion: ultrasound guidance demonstrated reduced risk of fat embolism and death, alongside lower minor complication rates including seroma, fat necrosis, and surgical-site infections.
The full ultrasound BBL meta-analysis is the strongest current evidence — but the authors are also clear that ultrasound only works inside a disciplined surgical system. Equipment doesn’t replace judgment.
Safety principle: A “safe BBL surgery” plan is only as safe as the team’s ability to execute it reliably—every pass, every zone, every time.
Real-time cannula tip visualization to reduce “blind” injection
Historically, one of the biggest problems in BBL safety was that fat injection could be performed with limited real-time visibility—meaning the surgeon relied on tactile feedback and experience to estimate depth. Ultrasound changes that by allowing the team to visualize the cannula tip during the critical moments.
That matters because the most serious BBL risks are linked to where the cannula tip is at the moment fat is delivered. Seeing the tip helps reduce the chance of an unintentional depth change—especially during:
- Repositioning of the patient
- Transitioning between different buttock zones
- Cases with complex anatomy or prior surgery
- Moments when swelling or tissue resistance makes “feel” less reliable
When patients ask “is it safe to get a BBL”, this is one of the most meaningful differences between older-era approaches and modern practice: safety is increasingly designed to be system-based, not personality-based.
Confirming the correct fat-grafting layer throughout the procedure
Many patients researching “is a BBL safe” assume the injection layer is a single decision made once. In reality, the injection plane can drift unintentionally as the procedure progresses. Ultrasound can be used to repeatedly confirm that the team is staying in the intended layer.
From a patient standpoint, this is important because it reframes safety from “Did the surgeon say they inject safely?” to “How does the surgeon verify they’re injecting safely throughout?” That’s the mindset behind the modern expectation for safe BBL technique—especially when clinics advertise safe BBL Turkey options to international patients who must rely on structure and documentation, not familiarity.
Standardizing technique across the team (not just “surgeon skill”)
One reason the phrase “safe BBL surgery” can be confusing online is that patients are often told to “find the best hands.” Skill matters—but safety at a high level is not just a talent issue, it’s a system issue.
Ultrasound guidance can support standardization by making the procedure more teachable and more auditable:
- Shared visual reference: the team can see the same anatomy and cannula position, reducing miscommunication.
- Consistency checks: the surgeon can confirm technique remains aligned with the plan across multiple zones.
- Reduced variability: safer workflows are less dependent on “how it feels today.”
This is one reason many “expert patients” who ask “is getting a BBL safe” also ask a second question: “What happens if something doesn’t look right mid-procedure?” A standardized environment is more likely to catch and correct small deviations early.
Documentation and accountability: what should be recorded
Here’s a practical point most blog posts skip: if ultrasound is truly part of a clinic’s safety standard, there should be a culture of documentation. Not because patients want paperwork—but because documentation reflects a clinic’s seriousness about reproducible safety.
Examples of what a safety-forward clinic may be able to discuss transparently (without oversharing sensitive data):
- Whether ultrasound is used continuously during injection or only in “spot checks”
- How the team confirms the intended injection layer in different zones
- Who is responsible for ultrasound visualization while the surgeon injects
- What the clinic’s complication pathway is (recognition, escalation, hospital transfer)
| What Patients Often Hear | What Matters More | What to Ask to Verify |
|---|---|---|
| “We do safe BBL surgery.” | Is the injection plane controlled and verified? | “How do you confirm the cannula tip position during injection?” |
| “We offer a safe BBL package.” | Are safety protocols built into workflow, not add-ons? | “What are your monitoring and escalation protocols post-op?” |
| “We use ultrasound.” | Is it truly ultrasound-guided during fat transfer? | “Is ultrasound used for every injection pass, every case?” |
| “Awake BBL is safer.” | Safety depends on selection + monitoring + procedure scope | “Who manages anesthesia/sedation and what monitoring is used?” |
So, is BBL surgery safe today? The honest answer is: it can be significantly safer when modern standards are used—especially when clinics reduce “blind” variables and commit to a disciplined technique. But ultrasound is only one piece of the puzzle.
Our surgery dates fill up quickly due to high international demand. Secure your consultation today to plan your ideal travel dates.
BBL Meaning, Ultrasound Guidance, and What “Safer” Really Means
Many patients begin with one urgent question: is BBL safe? Before you can judge safety claims, you need clarity on terms. The bbl meaning in cosmetic surgery is “Brazilian Butt Lift,” a procedure combining liposuction (fat harvesting) and fat transfer (fat grafting) to reshape the buttocks. Online, “BBL” can also refer to BroadBand Light skin treatments, which creates confusion—especially in searches about “BBL laser” and pregnancy.
What safety depends on (beyond marketing)
Modern standards focus on controlled technique, correct injection layer, conservative volume goals, qualified anesthesia monitoring, and structured post-op observation. Technology is not a shortcut, but it can support safer execution when used consistently within a disciplined surgical system.
Why ultrasound changes the safety conversation
The key upgrade with bbl ultrasound is real-time visualization during fat injection. Instead of relying only on tactile feel, the team can confirm cannula position and the intended plane throughout different zones. This helps reduce “blind” variability and encourages repeatable, auditable technique—especially important for patients traveling for surgery.
How to verify a clinic’s ultrasound claim
- Ask if ultrasound is used during every injection pass, not only “selected cases.”
- Confirm who operates and interprets imaging while the surgeon injects.
- Request a clear explanation of the target layer and how it’s maintained throughout.
- Review the first-24-hour plan: monitoring, mobility guidance, and escalation pathway.
If a clinic offers bbl with ultrasound, it should be able to explain the workflow calmly, transparently, and without absolutes—because “safer” comes from standards you can verify, not promises.
Safety Standards That Matter More Than Marketing Claims
If you’re comparing clinics and searching “safe BBL surgery” or “safe BBL Turkey”, here’s the uncomfortable truth: marketing language is cheap, and the word “safe” is unregulated. What protects you is a clinic’s standards—the ones that show up in credentials, facility readiness, anesthesia protocols, and post-op monitoring.
Ultrasound guidance can be a meaningful upgrade, but it’s not a “magic shield.” A truly safe BBL technique lives inside a safety system.
Expert-patient mindset: Don’t ask “Do you do safe BBL?” Ask, “What do you do when everything doesn’t go perfectly?”
Surgeon credentials: what to verify (and what vague titles don’t prove)
Patients who ask “is a BBL safe” are usually trying to filter out two risks: lack of surgical training and lack of judgment. Credentials can’t guarantee outcomes, but they can reduce avoidable risk by confirming a minimum training standard.
- Confirm the operating surgeon’s full legal name (not just a brand name) and verify licensing on official registries where possible.
- Ask who performs each step: liposuction harvesting, fat processing, and fat injection (the most safety-critical part).
- Ask about safety philosophy: Will the surgeon say “no” to unsafe volume goals? A surgeon who never refuses requests is not a safety signal.
- Ask about experience with your profile: prior surgery, scar tissue, higher BMI, or complex body contouring plans.
When patients search “how safe is BBL surgery”, the best answers come from transparency: a surgeon who explains risk plainly and can describe a structured safety approach is typically safer than one who dismisses risk or overpromises.
The hardest filter in surgeon evaluation isn’t credentials—it’s philosophy. A surgeon who never says “no” to a volume request is not a safety signal. A surgeon who explains exactly why a 1200cc transfer is unsafe for your anatomy, even when you’re disappointed, is doing the job correctly.
The full credential-verification framework, including how to read fellowship pedigrees and what specific questions surface unsafe philosophy, is detailed in our surgeon evaluation guide.
Facility standards: “clinic” vs. surgical readiness
Many complications are time-sensitive. That’s why the facility matters as much as the surgeon. If you’re evaluating a safe BBL package (in Turkey or anywhere), the key question is whether the package includes real surgical infrastructure, not just hotel transfers.
- Operating room standards: sterile protocols, controlled environment, and consistent infection-prevention workflows.
- Monitoring capability: proper intraoperative monitoring and trained staff present throughout.
- Emergency readiness: clear escalation pathway and the ability to transfer to a higher-level hospital setting if needed.
- Regulatory licensing: confirm the facility is officially licensed/authorized to provide surgical services (don’t rely only on social media claims).
“Clinic” is one of the most abused words in cosmetic marketing. A spa-grade aesthetic suite and a JCI-accredited surgical hospital both call themselves “clinic” online. The difference shows up in the first 30 minutes of an emergency — and you don’t get to find out which one you booked until it’s too late.
The accreditation criteria, OR-grade infrastructure benchmarks, and emergency-pathway questions that separate genuine surgical facilities from marketing-grade ones are in our facility evaluation guide.
Practical takeaway: A clinic can advertise “safe BBL surgery,” but if it can’t clearly explain its emergency plan and monitoring standards, you’re being asked to take a leap of faith.
Anesthesia safety: who administers it, what monitoring is used, and why it matters
Patients asking “is BBL surgery safe” often focus on the fat transfer—but anesthesia safety is a major pillar of overall risk management. Your questions should be specific:
- Who is responsible for anesthesia/sedation? (Credentials, role, and accountability.)
- What monitoring is used throughout? (Vital signs, oxygenation, and continuous observation.)
- What is the rescue capability? (If something changes rapidly, what is the response plan?)
This matters even more when patients search “is awake BBL safe” or “awake BBL surgery”. “Awake” doesn’t automatically equal safer—what matters is patient selection + monitoring + procedure scope. A “lighter” anesthesia approach can be appropriate in selected cases, but it still requires rigorous safety standards and a team trained for escalation.
Post-op observation protocols: the first 24 hours are not a formality
One of the most overlooked parts of safe BBL surgery—especially for medical tourists—is what happens immediately after surgery. Early complications can be subtle at first, and the difference between “fine” and “serious” can depend on monitoring and response time.
- Observation: is there structured monitoring right after surgery (not just “go back to the hotel”)?
- Mobility guidance: early movement plans to reduce clotting risk, with clear rules for your specific case.
- Communication: who do you contact after hours, and what symptoms require urgent evaluation?
- Follow-up schedule: real check-ins, not just a single quick discharge.
| Marketing Claim | What It Should Mean | What You Should Ask For |
|---|---|---|
| “Safe BBL technique” | Clear plan for injection plane + controlled execution | “How do you verify the injection layer during the procedure?” |
| “Ultrasound BBL” | Used during fat injection (not just mentioned) | “Is ultrasound guidance used throughout injection in every case?” |
| “Safe BBL package” | Safety infrastructure + aftercare, not just logistics | “What monitoring happens in the first 24 hours post-op?” |
| “Awake BBL is safer” | Depends on selection + monitoring + scope | “Who manages sedation and what continuous monitoring is used?” |
Common BBL Myths Debunked: Separating Fact from Tabloid Fiction
If the medical protocols are so advanced, why does the stigma persist? The narrative around is BBL safe in Turkey is often clouded by misconceptions that conflate “affordability” with “danger.” For US patients comparing options, separating headline fear from clinical reality is critical. Below are the three biggest myths preventing patients from making objective decisions about safe BBL surgery.

Myth-busting mindset: The right question isn’t “Is Turkey safe?” — it’s “Which standards is this specific clinic following, and can I verify them?”
Myth #1: “Turkey is cheap because the medical quality is low”
This is the most pervasive economic fallacy in medical tourism. The 60–70% cost difference between a BBL in Turkey and the USA is not a reflection of cut corners — it’s a reflection of macroeconomics. The lower costs are primarily driven by:
- The favorable exchange rate between the US Dollar and the Turkish Lira
- Significantly lower national operational costs (facility rents, staff salaries, overhead)
- Government support for accredited medical tourism facilities, which helps clinics maintain hospital-grade standards at lower prices

You are not paying for “cheap surgery” — you are paying for high-quality surgery performed in a lower-cost economy. Price and safety are separate variables, and the real question is always what safety standards are built into the specific clinic you’re evaluating. To see exactly what’s included in a surgeon-led BBL surgery in Turkey — from pre-op testing to post-op monitoring — review the complete procedure breakdown.
The “Turkey is cheap therefore unsafe” argument oversimplifies on both ends. It conflates exchange-rate economics with quality of care, and it ignores the fact that JCI-accredited Istanbul hospitals operate under the same international standards as their counterparts in Houston or London. The honest answer to “is plastic surgery in Turkey safe” requires separating market structure from medical structure.
The full picture — regulatory framework, accreditation reality, complication statistics, and what actually drives the price differential — is unpacked in our Turkey safety standards primer.
Myth #2: “Turkish surgeons aren’t board-certified”
Skeptical patients often assume that “board certified” is a title unique to American doctors. This is false. Top Turkish surgeons undergo rigorous training and certification processes that rival US standards. Many hold the European Board of Plastic, Reconstructive and Aesthetic Surgery (EBOPRAS) certification, which is widely considered the direct equivalent of US board certification.
What matters more than geography is whether a clinic is surgeon-led — meaning medical ethics and clinical judgment dictate the patient journey, not sales targets. A surgeon-led environment is far more likely to:
- Refuse unsafe volume goals
- Conduct thorough pre-op screening and medical clearance
- Maintain consistent technique and safety protocols across every case
Before booking, always verify the operating surgeon’s credentials on official registries — not just on the clinic’s website. You can see how a surgeon-led patient journey should be structured from virtual consultation to aftercare in the AKM Clinic process.
Myth #3: “Hygiene standards are lower than in the USA”
There is a misconception that clinics abroad operate in less-than-sterile environments. The reality is often the opposite. Turkey serves as a major hub for international healthcare, and the government imposes strict regulations to protect this industry’s reputation.
Leading clinics operate in hospitals accredited by the Joint Commission International (JCI) — the gold standard in global healthcare accreditation. These facilities adhere to multi-stage sterilization protocols that align with standards mandated by the CDC and WHO. When you choose a reputable JCI-accredited provider, the clinical environment is statistically as safe as — if not safer than — many private outpatient surgical centers in the US.
The real safety filter is not the country. It’s the specific facility, the named surgeon, and whether the workflow you can audit matches the safety claims you were sold.
One myth most BBL safety articles skip: the surgeon you consulted may not be the surgeon who operates. “Ghost surgery” — when an unannounced surgeon performs the procedure while the consulting surgeon is named on paperwork — is a real medical-tourism red flag, not a tabloid invention. It’s also one of the few risks that ultrasound technology cannot fix, because it’s a contractual and accountability issue, not a technique issue.
The contractual clauses, identity-verification steps, and consultation questions that protect against this are in our ghost surgery red-flag walkthrough.
Patient Selection—Who Is (and Isn’t) a Good Candidate for a Safer BBL
When people ask “is getting a BBL safe” or “is it safe to get a BBL”, they often assume safety is mainly about the operating room. In reality, a major part of safe BBL surgery happens before surgery even starts: patient selection and realistic planning. To understand how candidacy is evaluated during a surgeon-led consultation, see the full BBL consultation and candidacy process at AKM Clinic.
A clinic can use ultrasound guidance and still create avoidable risk if the plan is wrong for the patient’s anatomy, health profile, or goals. A truly safe BBL technique includes the discipline to say “not now” (or “not at all”) when risk is too high.
Here’s a candor moment: not everyone asking about BBL safety is actually a good candidate for fat transfer. Low BMI, limited donor area, or aggressive volume goals can shift the math toward implants—not because BBL is “less safe,” but because the right procedure for your anatomy isn’t always the one you walked in asking for.
The candidacy filter—BMI, donor area, projection goals, recovery tolerance—is mapped step by step in our BBL decision-tree breakdown.
For patients whose anatomy or goals don’t fit fat transfer logic, the conversation shifts entirely. Implants follow a different risk profile, recovery curve, and longevity timeline than fat grafting. They’re not a “consolation prize” — they solve a different problem.
The technique mechanics, candidacy criteria, and revision considerations specific to gluteal implants are covered in our implant-based augmentation overview.
Safety truth: The “best” BBL result is the one that is achieved without pushing your body past safe limits.
BMI, fat availability, and why “more fat transfer” isn’t always better
Many patients interpret “more fat transferred” as “better.” That’s not how safety works.
- Very low body fat: If there isn’t enough donor fat, clinics may be tempted to “stretch” the plan or promise unrealistic volume. Safer options may involve modest transfer or alternative contour strategies.
- Higher BMI: More donor fat doesn’t automatically make the case safer. Higher BMI can correlate with increased anesthesia risk, higher clotting risk, and more complex recovery needs.
- Skin quality: Loose or poor-quality skin can limit how much volume looks natural and how evenly it settles.
If your key question is “how safe is BBL surgery” for your body type, the answer depends on how conservatively the surgeon plans volume relative to your tissue capacity—not on marketing promises.
Smoking, clotting risk, and medical history red flags
“Safe” isn’t just about the buttocks. It’s about your whole body’s ability to tolerate surgery and heal.
- Nicotine/smoking can increase complication risk by impairing circulation and healing.
- History of clotting issues, certain medications, hormone therapy, or limited mobility can raise DVT/PE risk and requires careful planning.
- Uncontrolled medical conditions (for example, poorly controlled hypertension or diabetes) can shift the risk profile significantly.
A clinic offering safe BBL Turkey options should be able to explain how they screen and stratify risk—without minimizing your medical history.
Answer a few quick questions about your concerns, health, and goals to learn which treatment options may suit you best.
Prior surgeries and scar tissue: how they change planning
If you’ve had prior liposuction, tummy tuck, C-section, or other abdominal/flank procedures, your anatomy may include scar tissue that changes how liposuction and fat harvesting behave. That doesn’t automatically disqualify you, but it should change the plan:
- Donor area strategy: where fat can be harvested safely and evenly
- Symmetry planning: scar tissue can influence contour and swelling patterns
- Procedure duration: complex cases can run longer, which can affect overall risk
For patients asking “is BBL surgery safe” after previous body surgery, the safest clinic is typically the one that plans more carefully and promises less—not more.
Setting realistic goals to avoid unsafe overcorrection
Unrealistic expectations are a hidden safety risk. Why? Because chasing extreme volume can pressure the plan in unsafe ways—more aggressive liposuction, longer operative time, and more transfer than tissues can predictably support.
Here’s a simple way to evaluate whether a surgeon is aligned with safe BBL surgery standards:
- Do they discuss a range of outcomes rather than a guaranteed size?
- Do they explain fat survival variability and why “bigger is not always better”?
- Will they set a firm boundary if you request an unsafe amount of fat transfer?
| Candidate Factor | What It Can Affect | What a Safety-First Clinic Typically Does |
|---|---|---|
| Nicotine use | Healing quality, complication risk | Requires cessation protocol and may delay/decline surgery if not followed |
| High BMI or complex medical history | Anesthesia + clotting risk, recovery complexity | Risk stratification, clear medical clearance steps, and conservative planning |
| Very low donor fat | Feasibility of desired volume | Discusses realistic volume, staged planning, or alternative approaches |
| “Extreme” size goals | Overcorrection pressure, tissue stress, longer surgery | Sets boundaries, prioritizes safe proportions and tissue capacity |
So, is a BBL safe for you? The safest answer is individualized. Your risk profile isn’t determined by one variable—it’s the sum of your health status, your goals, and the clinic’s willingness to design a plan that fits both.
Share your photos and medical history to receive a personalized assessment from our European board-certified facial surgery team.
Pre-Op Planning That Reduces Complications
For anyone typing “is BBL safe” or “is it safe to get a BBL”, here’s a useful way to think about risk: the operation doesn’t begin in the operating room—it begins with pre-op planning. The clinics that consistently deliver safe BBL surgery tend to be the ones that treat preparation as a safety protocol, not a formality.
Whether you’re considering safe BBL Turkey options or staying local, your best protection is a clinic that can show you a structured system that covers: medical screening, anesthesia planning, a clear surgical map, and a realistic recovery plan.
Pre-op labs, medication review, and risk stratification
A proper pre-op process for brazilian butt lifting should include more than a quick questionnaire. Ask what is actually reviewed and when. Key areas usually include:
- Baseline health screening: medical history, prior surgeries, allergies, and conditions that change surgical risk.
- Medication and supplement review: blood thinners, certain hormones, and even “natural” supplements can affect bleeding and clotting risk.
- Clot-risk evaluation: your mobility, travel plans, personal/family history, and procedure scope should inform DVT prevention planning.
- Nicotine policy: a serious clinic will have clear rules on nicotine cessation because it can meaningfully impact healing and complication risk.
If your clinic can’t clearly explain how it screens for risk, it’s hard to call the process safe BBL technique—even if they advertise “ultrasound-guided.”
Surgical plan: lipo areas, transfer strategy, and symmetry planning
Patients asking “how safe is BBL surgery” often focus on the fat injection, but safety also depends on how the overall procedure is designed. A well-planned BBL typically includes:
- Donor site strategy: where fat will be harvested (abdomen, flanks, back, thighs) and how to avoid over-aggressive liposuction.
- Volume planning: a realistic range based on your tissue capacity, skin quality, and goals—without pushing for extreme outcomes.
- Symmetry mapping: photos, measurements, and a zone-by-zone plan to reduce unevenness.
- Technique alignment: if the clinic claims “safe BBL surgery,” they should be able to explain the intended injection layer and how they confirm it throughout.
The fat harvest step is rarely talked about as a safety variable, but it should be. Donor-site liposuction technique, anesthesia depth, and patient awareness during harvest all affect total surgical load — especially in awake protocols where the lipo phase is performed without general anesthesia.
The awake high-def liposuction workflow—what stays comfortable, what’s monitored, what’s traded off—is detailed in our awake liposuction primer.
This is also where an ultrasound guided bbl approach can add value: it supports consistent execution of a plan that prioritizes controlled depth and repeatable technique.
Travel planning for international patients (timing, logistics, support person)
If you’re researching safe BBL Turkey, travel safety becomes part of medical safety. A clinic’s “package” only matters if it supports safe timing and follow-up—not just convenience. Consider these planning elements:
- Arrival timing: you should have enough time for in-person evaluation before surgery (not “land and operate” rushed schedules).
- Post-op observation: ask where you’ll be monitored right after surgery and what the first-night plan is.
- Follow-ups while still in-country: safe medical tourism includes structured check-ins before you fly home.
- Support person: ideally, have someone with you—especially in the first 48 hours—to help with mobility, hydration, meals, and symptom monitoring.
- Flight timing: your surgeon should give individualized guidance based on your risk profile and procedure scope.
What a “safe BBL package” should include (and what it should never replace)
Many people search for a safe BBL package expecting it to mean “everything is covered.” The right way to use that idea is as a checklist. A safety-forward package typically includes:
- Documented pre-op screening (not just a sales consult)
- Clearly defined anesthesia and monitoring responsibilities
- Structured post-op observation and clear after-hours support
- Planned follow-ups before departure for medical tourists
But no package should replace the essentials: surgeon judgment, facility readiness, and transparent risk discussion. If you feel pressure to “book fast,” that’s a safety red flag—especially when your core question is “is BBL surgery safe”.
| Pre-Op Safety Step | Why It Matters | What to Listen For |
|---|---|---|
| Risk screening + medication review | Prevents avoidable bleeding/clotting complications | Specific instructions, not vague reassurance |
| Procedure scope planning | Overly aggressive plans increase risk | Conservative, anatomy-based volume goals |
| Travel + observation plan | Early detection of issues is time-sensitive | Clear first-night monitoring and follow-up schedule |
Recovery and Aftercare—Where Safety Is Won or Lost
If you’re still asking “is BBL safe” after reading about ultrasound, credentials, and planning, this next section is where many “expert patients” shift from theory to reality. A safe BBL surgery isn’t just the technique in the OR—it’s what happens in the first hours, days, and weeks after surgery.
Even the best safe BBL technique can be undermined by poor monitoring, rushed discharge, dehydration, immobility, or unclear instructions—especially for medical tourists evaluating safe BBL Turkey options.
BBL has unique post-op flight constraints that other procedures don’t. Sitting restrictions in the first weeks, donut cushion logistics in airline seats, DVT risk on long-haul flights, and cabin pressure effects on swelling — all of these compound when the patient is flying transatlantic from Istanbul to a US destination. “When can I fly?” is not a single answer; it’s a multi-variable clearance.
The procedure-specific timing window for BBL, plus the airline-seating logistics that medical tourism patients should plan for, are in our post-op flight clearance reference.

Recovery mindset: Your goal is not “toughing it out.” Your goal is early detection, safe mobility, and controlled healing.
Early mobility + DVT prevention strategies
One of the most important safety topics after any major body surgery is clot prevention (DVT/PE risk management). The safest clinics build this into your plan—not as generic advice, but as an individualized protocol based on your history, procedure scope, and travel timing.
- Early, gentle movement: short, assisted walks as advised—starting as soon as your care team clears you.
- Hydration and nutrition: dehydration increases risk; follow a structured hydration plan.
- Leg circulation habits: ankle pumps, calf activation, and avoiding long, immobile periods.
- Medication guidance: only if prescribed—never self-start blood thinners or supplements without surgeon clearance.
When to escalate urgently: shortness of breath, chest pain, fainting, severe calf swelling/pain, or sudden worsening symptoms are not “normal recovery.” They require immediate medical evaluation.
Sitting restrictions, garments, and swelling management—what’s practical (and what’s not)
Patients searching “is it safe to get a BBL” often overlook how much recovery affects outcomes and comfort. After a brazilian butt lifting, your surgeon may advise strategies to reduce direct pressure on the grafted area and protect fat survival.
- Pressure management: many protocols recommend avoiding direct sitting pressure early on and using a purpose-made support pillow when necessary.
- Sleeping position: often stomach/side positioning is recommended early (your surgeon’s instructions win).
- Compression garments: typically aimed at liposuction donor areas to help swelling and contour control—fit matters.
- Swelling expectations: swelling is normal; sudden asymmetry, severe pain, or rapidly increasing swelling is not.
Be cautious with “one-size-fits-all” rules found online. The safest path is a plan tailored to your procedure details and anatomy.
| Aftercare Item | What It’s For | Common Mistake to Avoid |
|---|---|---|
| Mobility plan | Reduce clot risk + support circulation | Staying in bed too long “to protect results” |
| Compression garment (donor areas) | Swelling control + contour support | Over-tight compression or improper fit |
| Pressure management (BBL pillow, positioning) | Reduce direct pressure on grafted area | Ignoring instructions because you “feel fine” |
| Hydration + nutrition | Support healing + reduce avoidable complications | Under-eating/under-drinking due to low appetite |
Follow-up schedule and what “good monitoring” looks like for medical tourists
If you’re evaluating safe BBL Turkey options, follow-up isn’t just a convenience—it’s a safety feature. A strong follow-up plan should include:
- Early post-op checks while you are still in-country (not just a quick discharge)
- Clear after-hours contact for urgent concerns
- Written instructions for mobility, garments, showering, wound care, and warning signs
- Departure readiness: guidance on when flying is appropriate for your risk profile
As one AKM Clinic patient described the support experience: “the nurses, the doctors, the medications, everything is included.”
A “safe BBL package” should mean the clinic has built a care pathway that covers both medical safety and recovery logistics—without replacing the essentials (surgical standards, monitoring, and a real escalation plan).
Advanced recovery support: HBOT & LLLT as part of a complication-prevention mindset
Technology can’t replace surgical safety—but it can support recovery when used appropriately. AKM Clinic highlights two post-operative recovery technologies as part of its broader patient care standards:
- Hyperbaric Oxygen Therapy (HBOT): used to support healing by increasing oxygen delivery in tissues, with aims such as helping tissue recovery, reducing swelling/downtime, supporting scar healing, and assisting infection-risk mitigation as part of a structured protocol.
- Low-Level Laser Therapy (LLLT): a non-invasive light-based therapy described for supporting cellular repair, collagen support, and inflammation reduction—often positioned as complementary to HBOT in recovery protocols.
Important: neither HBOT nor LLLT makes an unsafe injection safe. They are best understood as adjuncts that may help recovery quality and comfort when integrated into a well-designed surgical and aftercare system.
Questions to Ask Any Clinic Claiming “Ultrasound BBL Safety”
If you’re comparing providers and typing things like “safe BBL surgery,” “safe BBL technique,” or “safe BBL Turkey”, the smartest move is to stop reading claims and start asking verification questions. Ultrasound guidance can be a meaningful safety upgrade—but only if it’s used properly, consistently, and by a proficient team.
Rule of thumb: A clinic that truly prioritizes safety will welcome detailed questions. A clinic that dodges details is telling you something—without saying it.
1) “Do you use ultrasound guidance during fat injection—every case, every pass?”
Don’t accept vague answers like “Yes, we have ultrasound.” What you want to clarify is whether the procedure is truly ultrasound-guided during the fat transfer step (not just pre-op scanning or occasional spot checks).
- Good sign: “We use ultrasound guidance throughout injection to confirm the cannula tip and the target layer.”
- Red flag: “We only use it sometimes,” or “We use it if needed,” with no clear criteria.
2) “Who is responsible for ultrasound visualization while the surgeon injects?”
Ultrasound guided bbl technique is a skill. Ask who holds the probe, who interprets the image, and how the team coordinates during injection.
- Good sign: Clear workflow + evidence that the team is trained and consistent.
- Red flag: Confusion about roles, or “our assistant does it” with no mention of training/proficiency.
3) “What layer do you inject into, and how do you confirm you stay there?”
When patients ask “is a BBL safe” or “how safe is BBL surgery”, this is the most safety-critical technical question. You’re looking for a clinic that can describe a safe BBL technique in plain language—without defensiveness, and without oversimplifying.
- Good sign: A consistent, layer-specific plan and a method for verification (often ultrasound guided bbl visualization).
- Red flag: “We do it our way,” “We’ve never had a problem,” or refusal to discuss injection plane.
4) “How many BBLs does the surgeon perform in a day?”
Patients rarely ask this—but it matters. Safety tends to improve when clinics avoid assembly-line scheduling. If a surgeon is doing a very high number of BBLs daily, that can raise concerns about fatigue, rushed technique, and reduced attention to detail.
- Good sign: A reasonable daily case limit and a calm, methodical workflow.
- Red flag: “We do as many as we can,” or an unusually high daily volume.
5) “Who manages anesthesia/sedation, and what continuous monitoring is used?”
This matters for all BBLs—and even more if you’re searching “is awake BBL safe” or “awake BBL surgery”. “Awake” can mean different sedation levels; safety depends on patient selection, monitoring, and rescue capability.
- Ask: Who is responsible for anesthesia or sedation? What monitoring is continuous? What is the emergency response plan?
- Red flag: No clear anesthesia lead, vague monitoring details, or “You’ll be fine” reassurances without specifics.
6) “What happens if there is a complication—what is your escalation pathway?”
Any clinic offering safe BBL surgery should be able to describe, calmly and clearly:
- How urgent symptoms are recognized (by staff, not just the patient)
- How rapidly care escalates (who decides, what steps happen)
- Where you are transferred if higher-level care is needed
Red flag: No concrete plan, or a clinic that treats emergency readiness as an “unlikely scenario” rather than a required safety standard.
7) “What does the first 24 hours look like—monitoring, mobility, and after-hours contact?”
If you’re choosing a safe BBL package, the package should include real aftercare structure—not just transport and a hotel. Ask about:
- Immediate observation: where you are monitored and for how long
- Mobility plan: how and when you begin safe movement (clot-risk prevention)
- After-hours support: who answers, how fast, and what triggers an urgent evaluation
8) “Will you refuse unsafe volume goals?”
This sounds blunt—but it’s one of the best predictors of safety culture. A clinic aligned with safe BBL technique will set boundaries when a requested size would require aggressive lipo, excessive transfer, or an overly long procedure.
| Question to Ask | Why It Matters | What a Safety-First Answer Sounds Like | Red Flag |
|---|---|---|---|
| “Is ultrasound used during injection for every case?” | Verifies technique vs. marketing | Clear “yes,” explained workflow | Vague or inconsistent answer |
| “Who operates/interprets ultrasound?” | Proficiency reduces error | Defined roles + training culture | Unclear responsibility |
| “What layer do you inject into, and how do you confirm?” | Most critical safety variable | Layer-specific plan + verification method | Refuses to discuss plane |
| “How many BBLs per day?” | Fatigue/rushing risk | Reasonable limits, not assembly-line | Very high daily volume |
| “What is your complication pathway?” | Time-sensitive emergencies | Clear escalation + transfer plan | “We’ve never needed it” attitude |
Final thought: If your core question is “is BBL surgery safe”, judge a provider by what they can explain and verify: modern technique (often including ultrasound), conservative planning, proper facility standards, and structured aftercare—not by marketing promises or “package” wording.
Is BBL Safe Frequently Asked Questions (FAQ):
Is BBL safe—or is an ultrasound-guided BBL simply safer?
The most honest answer is: a Brazilian Butt Lift (BBL) can be performed with modern safety standards, but it is not “risk-free.” Ultrasound guidance is best understood as a tool that can make a safer plan easier to execute consistently—especially by reducing “blind” variables during the most safety-critical step (fat injection).
So if you’re asking “is BBL safe”, the practical upgrade is not a guarantee—it’s a shift toward verifiable technique and stricter protocols.
Does ultrasound guidance eliminate the risk of fat embolism?
No. If you’re searching “is a BBL safe” or “how safe is BBL surgery”, it’s important to avoid absolute claims. Ultrasound can help confirm cannula position and intended injection plane, which may reduce avoidable risk, but it cannot eliminate risk entirely. Safety still depends on surgeon judgment, patient selection, conservative planning, controlled technique, and post-op monitoring.
How can I verify ultrasound was actually used during my BBL?
If a clinic advertises safe BBL surgery with ultrasound, ask for specifics—not slogans:
Workflow: “Is ultrasound used during injection in every case, every zone, every pass?”
Roles: “Who operates and interprets the ultrasound while the surgeon injects?”
Documentation: “Do you record ultrasound use in the operative notes?”
Transparency: “Can you walk me through how you confirm the injection layer throughout?”
A clinic that truly follows a safe BBL technique should be comfortable answering these clearly.
Is awake BBL safe? (Awake BBL surgery explained)
Patients often search “is awake BBL safe” because they want to reduce anesthesia risk. “Awake BBL surgery” usually means local anesthesia with sedation (rather than full general anesthesia), but the term can be used loosely.
Safety depends on:
Selection: your medical history, anxiety tolerance, and procedure complexity
Monitoring: continuous monitoring and an experienced anesthesia/sedation lead
Scope: avoiding overly long, aggressive combined operations
So, is getting a BBL safe because it’s “awake”? Not automatically. It can be appropriate in selected cases—but it must be individualized.
Is a BBL safer than butt implants?
This is not a one-size-fits-all answer. Butt implants and brazilian butt lifting have different risk profiles. BBL involves liposuction + fat transfer (and the safety discussion focuses heavily on injection technique and anatomy). Implants introduce device-related risks (like infection, displacement, capsular contracture, or long-term revision needs). The safer option depends on your anatomy, goals, and what your surgeon believes is appropriate for your risk profile.
How soon can I fly after a BBL?
If you’re researching safe BBL Turkey, this question matters even more. Flying too soon can add risk, especially related to swelling, comfort, and clot prevention. The correct answer is individualized—based on your medical history, procedure scope, mobility, and recovery progress.
Ask your surgeon for a written travel plan that includes: movement guidance, hydration rules, warning signs, and when to seek urgent evaluation.
Is BBL safe during pregnancy?
This search phrase is commonly misunderstood because “BBL” can mean two different things:
BBL surgery = Brazilian Butt Lift (fat transfer surgery). This is not a pregnancy-time procedure.
BBL laser / BBL light = BroadBand Light (an IPL-type skin treatment). Many clinics list pregnancy as a contraindication or advise against it during pregnancy due to limited safety data and higher pigmentation sensitivity.
If you meant BBL surgery, the answer is no—pregnancy is not the time for elective body-contouring surgery. If you meant BBL (BroadBand Light), defer treatment and get individualized medical guidance from your OB-GYN and a qualified clinician.
How safe is ultrasound guided fat transfer?
Ultrasound-guided fat transfer can be safer than “blind” injection because it helps the team confirm cannula position and the intended injection plane in real time. It does not make the procedure risk-free—overall safety still depends on patient selection, conservative planning, qualified anesthesia monitoring, and structured post-op observation.
Does ultrasound-guided BBL change the final results or just safety?
Primarily, it supports safer, more controlled technique by reducing uncertainty during injection. Some patients also value the consistency it brings to execution—helping the team follow the planned layer and distribution more reliably, which can support more predictable contouring.
What should I ask to confirm a clinic truly uses ultrasound during BBL?
Ask specific, verifiable questions: Is ultrasound used during every injection pass? Who holds and interprets the probe while the surgeon injects? What layer is targeted, and how do you confirm you stay there throughout? A safety-focused clinic will explain the workflow clearly and document it in operative notes.
How do I plan my bbl budget without compromising safety?
Start by prioritizing non-negotiables: surgeon-led care, proper facility standards, anesthesia monitoring, ultrasound guidance during injection (if offered), and structured aftercare. Treat unusually low pricing or “fast-book” pressure as a red flag, and allocate funds for recovery support and adequate follow-up time before flying.
What is the current mortality rate for BBL when performed correctly?
While past statistics were alarming (as high as 1 in 3,000), recent data shows that when the "subcutaneous only" technique combined with ultrasound guidance is strictly followed, the safety profile of BBL surgery improves dramatically — becoming comparable to that of a tummy tuck. The risk drops significantly when intramuscular injection is completely avoided through disciplined technique and verifiable intraoperative control.
Is it safe to fly back to the USA after a BBL in Turkey?
Yes, but not immediately. Most surgeons require you to stay in Istanbul for 4 to 5 days after surgery. This allows initial swelling to subside and ensures no immediate complications arise. You'll receive a "fit-to-fly" clearance from your surgeon before departure. During the flight itself, walk frequently, stay hydrated, and wear compression garments as advised to maintain healthy circulation and reduce DVT risk. For the full in-country stay timeline and what's included in each day, review the BBL recovery and travel plan.
Do I really need to stop smoking before BBL surgery?
Yes, absolutely. Nicotine constricts blood vessels, which can cause newly transferred fat cells to die (fat necrosis) and significantly delays wound healing. For successful recovery and to ensure the survival of your BBL results, you must stop all nicotine products — including vaping and nicotine patches — for at least 4 weeks before and 4 weeks after surgery. A safety-first clinic will not operate on active nicotine users and may require a cotinine test to verify cessation.
Medical Disclaimer: This page is provided for general educational purposes only and does not replace a face-to-face medical consultation, diagnosis, or personalised treatment plan. All surgery carries risks and outcomes vary between individuals. Suitability for an ultrasound guided bbl, procedure selection, and anesthesia choice can only be determined after a full clinical assessment by a qualified surgeon. Always follow your clinician’s instructions and seek urgent medical attention if you develop concerning symptoms during recovery.
Related Treatments
Ready to Start Your Own Transformation Journey?
Join the 2,000+ patients who trusted Dr. Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, revitalized you begins with a simple, no-obligation conversation. Contact us today from the USA for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. No hidden fees.
#2: Secure Your Date & VIP Booking
Once you're ready, our dedicated patient coordinators will help you secure your procedure date. We'll handle all your bookings, including your 5-star hotel and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you'll meet your specialist surgeon to finalise the details for your "natural, subtle, and revitalized" new look.














