Thick Skin Rhinoplasty: Swelling Timeline, Recovery & Tip Definition

- Thick skin rhinoplasty needs patience—tip definition appears later as swelling resolves gradually.
- Swelling duration is longer with thick skin; milestone photos (6–12+ months) guide realistic expectations.
- Structural support improves definition by helping thicker tissue re-drape smoothly over time.
- Choose a surgeon-led plan with clear follow-up, safe swelling management, and revision timing guidance.
Summary generated by AI, fact-checked by our medical experts
If you’ve been told you have “thick skin,” it can feel like a warning label — especially when you’re researching nasal surgery and hoping for a refined, defined tip. The truth is more nuanced: thick skin doesn’t mean “bad results,” but it does change how surgeons plan the operation and how your nose heals (especially swelling and when definition becomes visible). The complete primary rhinoplasty technique foundation — including open versus closed approach selection, dorsal hump management, septal cartilage preservation, and how technique choice adapts to skin envelope thickness — is documented on our primary rhinoplasty technique hub.
This guide breaks down what thick nasal skin really means, what medical science says about swelling behavior in thicker tissue, and how to set realistic expectations for the results of thick skin rhinoplasty—including how to interpret thick skin rhinoplasty before and after photos fairly.
- What thick skin is (and what it isn’t)
- Why swelling lasts longer and when definition appears
- How surgeons create support so thick skin can drape cleanly
- What you can do during recovery to support a better outcome
Table of Contents
What “Thick Skin” Really Means in Rhinoplasty
In rhinoplasty, “skin thickness” usually refers to the thickness of the soft-tissue envelope that covers the nasal framework (skin + subcutaneous tissue). This matters because the skin isn’t just a “cover”—it’s an active biological layer that influences swelling, scar behavior, and how crisply the underlying structure can show through. In thick skin rhinoplasty, the goal is often to build a stable, well-supported framework that can still look natural and refined under a heavier soft-tissue envelope.
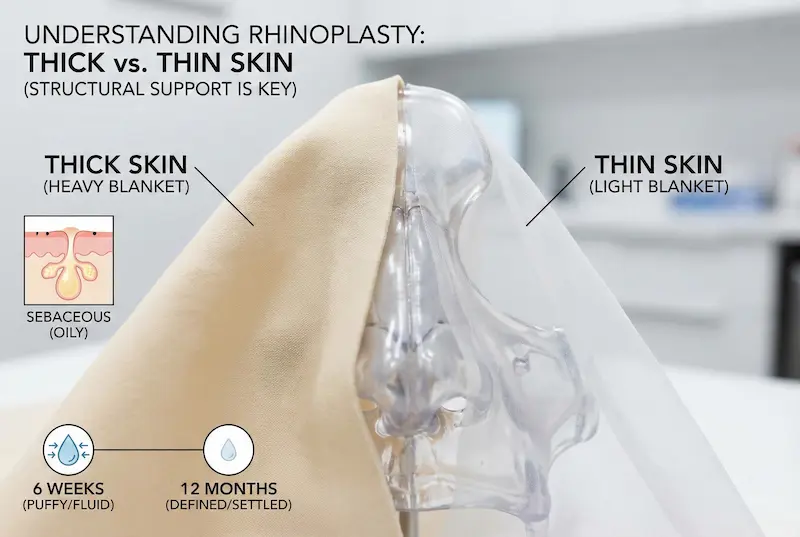
Skin thickness vs. sebaceous (oily) skin: why it matters
Many patients hear “thick skin” when what they actually have is sebaceous skin (more oil glands, more visible pores) or a combination of both. These traits often travel together, but they’re not identical:
- Thicker soft tissue can hold fluid longer after surgery and may blur early definition.
- Sebaceous skin may look shinier and can make pores more noticeable, especially on the tip.
- Both can make early “after” photos look less sharp than the final outcome.
Why this matters: thick tissue is more forgiving of tiny irregularities, but it can also delay visible definition — particularly at the tip. A peer-reviewed September 2025 nasal skin thickness classification study from the British Association of Plastic, Reconstructive and Aesthetic Surgeons evaluated 166 open rhinoplasty patients using the Nasal Skin Thickness Scale (NSTS) and demonstrated that pre-operative skin grading directly informs perioperative care decisions including surgical technique adaptation, edema management protocol, and revision risk stratification — providing the evidence base for why thick-skin cases require individualized planning rather than a single generic approach.
How thick skin affects tip definition and refinement
Think of the nasal tip like a sculpture under a blanket. With thin skin, the blanket is light—fine details show quickly. With thick skin, the blanket is heavier—detail can still show, but it may take longer and the surgeon often needs stronger “support beams” underneath.
This is why thick skin rhinoplasty planning often emphasizes:
- Structural support (so the tip doesn’t soften or droop as swelling resolves)
- Controlled shaping (prioritizing a smooth, natural contour over “razor sharp” definition)
- Patience with healing (definition can be a slow reveal, not an overnight change)
When you evaluate thick skin rhinoplasty before and after images, it’s crucial to note the time stamp. A 6-week photo may look “puffy,” while a 9–12 month photo may show a much cleaner tip.
Can thick skin be “thinned”? (What’s possible vs. marketing myths)
Some marketing implies surgeons can simply “thin thick skin.” In reality, ethical surgeons treat this carefully. In most cases, the safest and most predictable approach is not aggressive skin thinning, but rather:
- Optimizing the framework so the skin can redrape smoothly
- Reducing dead space where fluid can collect
- Using recovery protocols to support swelling control and scar modulation
In select cases, surgeons may address excess soft tissue in a conservative, technique-dependent way—but it must be individualized. From a scientific research perspective, the guiding principle is tissue safety: over-aggressive manipulation increases risks that can compromise healing and long-term appearance.
Share your photos and medical history to receive a personalized assessment from our European board-certified facial surgery team.
Why Swelling Lasts Longer With Thick Skin
One of the most common frustrations in thick skin rhinoplasty recovery is that the nose can look “bigger” or less defined for longer—especially at the tip. This isn’t a sign that something went wrong; it’s often a predictable healing pattern. In simple terms, thicker soft tissue can hold postoperative fluid longer, and the skin envelope may take more time to re-drape tightly over the new framework. That’s why thick skin rhinoplasty swelling duration is typically longer than in patients with very thin skin.
The biology of edema in thicker soft tissue
After rhinoplasty, your body responds with inflammation—this is normal healing. From a medical science standpoint, swelling (edema) is influenced by how much soft tissue is present, how it holds fluid, and how quickly lymphatic drainage normalizes. With thicker skin/soft tissue:
- There’s more tissue volume to swell and more space for fluid to linger.
- Redraping is slower because the skin envelope is heavier and may take longer to “shrink-wrap” to the refined structure.
- Tip swelling is stubborn because the nasal tip has delicate soft-tissue dynamics and is often the last area to decongest.
This is a key reason early photos can look less “snatched” than expected, even when the underlying work is excellent.
The “slow reveal”: why results can look boxy early on
Many patients with thick skin experience a phase where the bridge looks improved, but the tip seems rounded or “boxy.” This is often the slow-reveal phase—swelling masks definition, and the skin hasn’t fully settled onto the newly supported framework.
Key takeaway: In thick skin cases, it’s common for the bridge to “declare” earlier than the tip. Tip definition often improves gradually over months, not weeks.
When you evaluate thick skin rhinoplasty before and after images, try to compare photos taken at similar milestones (e.g., 3 months vs. 3 months, 12 months vs. 12 months). Otherwise, you may underestimate the real results of thick skin rhinoplasty.
What swelling is normal vs. warning signs
Normal swelling varies from person to person, but there are broad patterns surgeons expect. “Normal” often means the swelling fluctuates (some days look better, some worse), gradually trends down, and is not accompanied by escalating pain or systemic symptoms.
However, you should contact your surgeon promptly if you experience any of the following:
- Sudden, rapidly increasing swelling (especially on one side)
- Worsening pain that doesn’t match the expected recovery course
- Fever or concerning drainage/odor
- Skin color changes (marked blanching, dusky or dark areas) or any symptom your surgeon flags as urgent
| Milestone | What Patients Often Notice | Why It Matters for Thick Skin |
|---|---|---|
| Weeks 1–2 | General swelling, bruising, “puffy” appearance | Early swelling can obscure tip refinement more than expected |
| Months 1–3 | Bridge looks better; tip still feels firm/swollen | Tip definition commonly lags; patience is part of the plan |
| Months 6–12+ | Gradual sharpening and better contour balance | Many thick-skin cases show their best definition later in the first year |
Our surgery dates fill up quickly due to high international demand. Secure your consultation today to plan your ideal travel dates.
Surgical Strategies That Improve Definition in Thick Skin
In thick skin rhinoplasty, the most reliable way to achieve refinement is not “over-reducing” the nose, but building a stable internal structure that can support the heavier skin envelope as it heals. This is one reason thick-skin cases are often approached with a more structural mindset: the surgeon focuses on support, long-term contour stability, and a plan that anticipates a longer thick skin rhinoplasty recovery window—especially for tip definition.
Structural rhinoplasty: building support for the skin envelope
Thicker skin tends to soften or blur subtle changes, so surgeons often prioritize a framework that remains stable as swelling resolves. While the exact plan is individualized, “structural” thinking commonly includes:
- Reinforcing tip support so the tip doesn’t look amorphous early on or lose definition later.
- Maintaining airway stability (function matters—especially when adding structure).
- Balancing reduction with support to avoid an over-reduced look that thick skin can still mask (and that can increase revision risk).
From a scientific perspective, stable support helps the soft tissue re-drape more predictably over time, which is directly related to the long-term results of thick skin rhinoplasty.
Tip shaping techniques and graft choices (conceptual overview)
The nasal tip is usually the last area to “declare,” and thick skin can prolong that timeline. For that reason, tip strategy is often the centerpiece of the surgical plan. Depending on anatomy and goals, surgeons may use techniques designed to:
- Create a clearer tip shape that can still be appreciated under thicker tissue.
- Improve projection and definition without creating an artificial or pinched appearance.
- Enhance symmetry and reduce the chance of contour irregularities showing through later.
When you’re comparing thick skin rhinoplasty before and after photos, the most meaningful “definition” is often seen in the 9–12 month range (or later), once the tip has had time to settle and the skin envelope has adapted.
Beyond tip-specific techniques, the broader rhinoplasty toolkit also influences how thick skin redrapes — particularly the bone-shaping component. Piezoelectric (ultrasonic) rhinoplasty, which uses high-frequency vibrations to sculpt bone with minimal soft-tissue trauma, is sometimes selected in thick-skin cases to reduce the dead-space irregularities that can develop when traditional rasping disturbs the soft-tissue envelope more aggressively. The complete piezoelectric technique foundation — including ultrasonic instrument vectors, soft-tissue trauma comparison, and the specific candidate profile that benefits most from piezo over conventional osteotomy — is detailed in our piezo rhinoplasty technique guide.
Managing dead space and minimizing prolonged edema
One under-discussed factor in thick skin rhinoplasty swelling duration is “dead space”—areas where soft tissue isn’t closely supported by the underlying framework after surgical changes. When there’s more potential space, fluid can linger longer.
Surgeons reduce prolonged swelling risk by planning for:
- Precise soft-tissue handling to limit unnecessary inflammation.
- Thoughtful support and contouring so the skin envelope has a stable surface to re-drape over.
- Post-op guidance (e.g., taping protocols in selected patients) to encourage controlled redraping.
Surgeon-led mindset: In thick skin, the goal is often “stable refinement”—a nose that looks natural and balanced once the tissue fully settles, rather than chasing early sharpness that may not be biologically realistic.
This strategy is also important for patients worried about revision rhinoplasty for thick skin. Many revisions happen not because the primary plan was wrong, but because patients judge results too early—before swelling resolves and definition emerges. A careful structural plan plus realistic recovery expectations can reduce that risk.
A Realistic Recovery Timeline (Week-by-Week / Month-by-Month)
The most important mindset shift in thick skin rhinoplasty recovery is accepting that “looking finished” takes longer—especially at the tip. Thick skin tends to hold swelling and can delay visible definition, so a realistic timeline protects you from unnecessary anxiety (and premature “I need a revision” thoughts). While every patient is different, the outline below reflects common healing patterns and why thick skin rhinoplasty swelling duration can feel extended compared with thinner-skin cases.
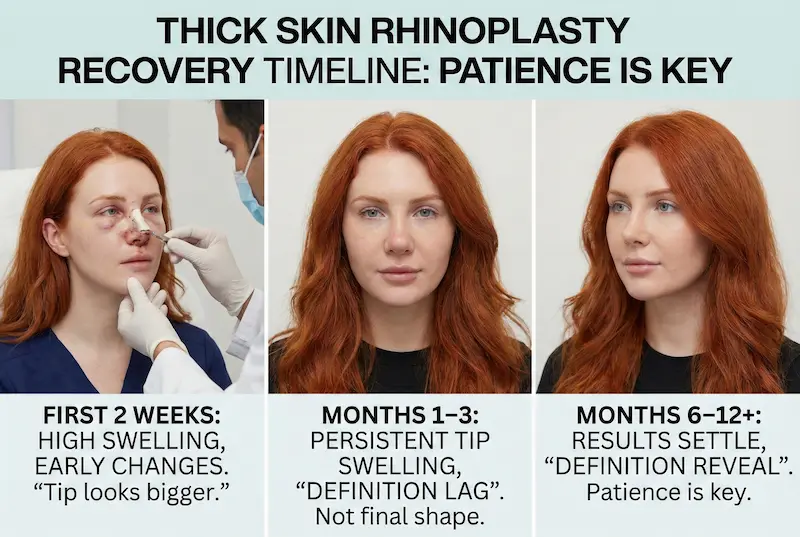
First 2 weeks: cast removal, bruising, early contour changes
During the first two weeks, swelling is high in almost everyone. For thick skin, the tip can look disproportionately swollen, and it’s normal to feel firmness when you touch the nose. This is not a reliable time to evaluate thick skin rhinoplasty before and after comparisons because the “after” is still dominated by postoperative edema and tissue stiffness.
- Common experience: “My bridge looks better, but the tip looks bigger.”
- Why it happens: The tip holds swelling longer; thick tissue can keep fluid and stay firm.
- Helpful mindset: Think “early healing,” not “final shape.”
| Time Point | What You May See/Feel | What It Usually Means (Thick Skin Context) |
|---|---|---|
| Days 1–7 | Congestion, facial puffiness, stiffness; the nose feels “tight” | Early inflammation is expected; thick tissue can feel firmer and more swollen |
| Week 1–2 | Cast removal; swelling still obvious, tip looks rounder | Definition is often masked—don’t judge results of thick skin rhinoplasty this early |
| Weeks 3–6 | Bridge begins to look more “refined,” tip remains puffy | Classic “slow reveal” phase; tip swelling commonly lingers |
| Months 2–3 | Better balance from the front; tip still not sharp | Normal for thick skin; swelling fluctuations (good days/bad days) are common |
| Months 4–6 | More stable shape; subtle improvements month-to-month | Many patients start noticing definition “arriving” gradually |
| Months 9–12+ | Cleaner contour; tip looks more defined, less firm | This is when many thick-skin noses show their most meaningful refinement |
Months 1–3: persistent tip swelling and “definition lag”
This is the phase when many patients start searching intensely for thick skin rhinoplasty recovery stories—because they expected sharper definition by now. In thick skin rhinoplasty, it’s common for the nose to look improved but not “fully refined.” The tip often remains rounded, and the skin envelope may still be adapting to the new structure underneath.
Reality check: A 6–8 week photo is rarely a fair representation of the final outcome in thick skin cases. The timeline is different, not the potential.
If you’re looking at thick skin rhinoplasty before and after galleries, try to prioritize results that show at least 6–12 months post-op—those images are more representative of actual definition and balance.
Months 6–12+ (and sometimes longer): when thick-skin results settle
By months 6–12+, swelling has typically decreased enough that the framework can be appreciated more clearly. For thick skin, this is often where the real “definition reveal” happens. The tip may continue to refine gradually, and subtle improvements can still occur beyond the one-year mark.
This longer settling window is also why reputable surgeons are cautious about labeling something as a “problem” too early. In many cases, what looks like “too round” at 3 months is simply ongoing swelling—part of the expected thick skin rhinoplasty swelling duration.
Important note on revision timing: Because thick skin can blur definition early, discussions about revision rhinoplasty for thick skin are often more appropriate later—once swelling has stabilized and the true baseline is visible.
How to Manage Swelling and Support Better Definition
Because thick skin rhinoplasty swelling duration can be longer, “doing the basics well” matters. Swelling control isn’t about hacks—it’s about supporting lymphatic drainage, minimizing inflammation triggers, and following a surgeon-specific plan that matches your anatomy and technique. The goal during thick skin rhinoplasty recovery is steady improvement month by month, not day-to-day perfection.
Evidence-based basics: elevation, cold/heat timing, activity limits
These fundamentals are simple, but they consistently make the biggest difference in early recovery:
- Head elevation: Sleep with your head elevated (especially in the first 1–2 weeks) to support fluid drainage.
- Cold compress timing: If your surgeon allows it, cold compresses can be helpful early for comfort and bruising—usually around the cheeks/eye area (not pressing on the nose).
- Heat timing: Heat is generally not an “early swelling fix.” Many surgeons prefer avoiding heat until bruising and acute inflammation have calmed—follow your surgeon’s timeline.
- Activity limits: Avoid heavy lifting, intense cardio, bending over, and anything that spikes blood pressure early on. These can worsen swelling fluctuations.
- Alcohol and high-salt meals: Both can increase fluid retention and make swelling look worse the next day.
| Swelling Trigger | Why It Matters | Practical Alternative |
|---|---|---|
| Hard workouts too early | Raises blood pressure; can increase swelling | Short walks as cleared by your surgeon |
| High sodium meals | Fluid retention can exaggerate puffiness | Lower-salt meals, good hydration |
| Smoking / nicotine | Impairs microcirculation and healing | Nicotine-free plan before and after surgery |
| Alcohol in early recovery | Can worsen inflammation and swelling fluctuations | Delay alcohol until cleared by your surgeon |
Taping, massage, and garments: who benefits and who shouldn’t
For thick skin patients, taping is sometimes used to guide swelling reduction and help the skin envelope redrape more smoothly—particularly around the tip. However, it’s not “one-size-fits-all.” In medical science, external compression can help in selected scenarios, but improper pressure or incorrect technique can irritate skin or create uneven swelling patterns.
- Taping: Can be helpful for some thick skin noses, usually when prescribed and demonstrated by your surgeon/team.
- Massage: Not automatically beneficial. Some surgeons recommend gentle techniques at a specific stage; others prefer avoiding manipulation early. Always follow your surgeon’s protocol.
- “More is better” is a myth: Over-taping or aggressive massage can inflame tissue and backfire, prolonging thick skin rhinoplasty recovery.
Rule of thumb: If your surgeon didn’t prescribe it (and show you how), don’t DIY it—especially in thick skin cases where swelling patterns can be more complex.
Clinic-based recovery support options (e.g., surgeon-guided protocols)
Some clinics support recovery with adjunct therapies alongside standard post-op care. At AKM Clinic, two post-operative technologies are highlighted for recovery support:
- Hyperbaric Oxygen Therapy (HBOT) is positioned at AKM Clinic as a structured recovery support modality. The patient breathes 100% oxygen in a pressurized chamber, with documented benefits including reduced inflammation/swelling, tissue regeneration support, improved scar healing, and infection-risk mitigation. For thick-skin rhinoplasty patients specifically, HBOT can support faster resolution of the prolonged tip swelling phase that is anatomically expected in thicker tissue envelopes — though the timeline still respects biological reality (HBOT shortens the curve, it doesn’t eliminate it). The complete oxygenation protocol — including session timing, pressurization parameters, and how it integrates with rhinoplasty-specific edema patterns — is detailed in our HBOT swelling reduction protocol.
- Low-Level Laser Therapy (LLLT) — using a 650nm low-level laser system — supports post-surgical skin healing mechanisms such as cellular repair (ATP-related pathways), enhanced collagen synthesis, and reduced inflammation. For thick-skin rhinoplasty, LLLT serves a dual role: it supports edema resolution at the nasal envelope and modulates collagen behavior in healing tissue, which is especially relevant when the soft-tissue layer is heavier and slower to redrape. The complete photobiomodulation protocol — including session frequency, fluence parameters, and how it pairs with rhinoplasty-specific scar and edema patterns — is detailed in our LLLT scar minimization guide.
These modalities shouldn’t replace the fundamentals (rest, elevation, activity restrictions, surgeon follow-up), but they may be used as part of a structured recovery plan—especially for patients who worry about prolonged swelling and delayed definition.
Importantly, even with strong recovery support, thick skin remains thick skin—so the timeline still matters. If you’re tracking progress, compare photos at the same milestones (e.g., month 1 vs. month 1; month 6 vs. month 6) to fairly judge the results of thick skin rhinoplasty.
Our philosophy is “Rejuvenation, Not Alteration.” Discover how our surgeons achieve subtle, revitalized results that honor your unique beauty.
What Results Are Realistic With Thick Skin
The most reassuring thing to know is this: results of thick skin rhinoplasty can be excellent—natural, balanced, and clearly improved—when the plan respects thick-skin biology and the surgeon builds the right support underneath. The main difference is rarely “can you get a good result?” but rather how long it takes for that result to visibly declare, and what level of tip sharpness is realistic for your specific skin/soft tissue.
“Refined but natural”: setting the right expectation
Thick skin can soften very sharp edges, which is why ethical surgeons usually aim for a refined, harmonious result rather than an ultra-sculpted, highly angular tip that may not read naturally (or may not be achievable without compromising tissues). In other words, the ideal thick-skin outcome is often:
- Cleaner overall contour (front and profile balance)
- Improved tip shape that becomes more visible over time
- Natural proportions that fit your face, not a “template nose”
This expectation aligns with how medical science and real-world healing behave: thick tissue needs time to settle and redrape, and definition is a gradual reveal.

Before/after interpretation: angles, lighting, and timeline traps
Many people feel discouraged when comparing thick skin rhinoplasty before and after photos—often because they compare a mature “after” (12+ months) with their own early “after” (6–8 weeks). For thick skin rhinoplasty, this is one of the biggest psychological traps.
To evaluate before-and-after images fairly, match time points (3 months to 3 months, 12 months to 12 months), check angles, beware lighting traps, and look for balance rather than just sharpness. The most reliable visual research happens not on Instagram or Reddit galleries but on standardized clinic libraries that document multiple time points, multiple angles, and multiple skin types. The complete documented outcome library — including time-stamped rhinoplasty cases with 6-month, 12-month, and 18-month visual progressions across thin-skin, medium-skin, and thick-skin profiles — is available on our documented outcome gallery hub.
| Common “Concern” in Early Photos | What It Often Is | What to Do |
|---|---|---|
| Tip looks round/boxy | Normal thick-skin swelling + firm tissue | Track monthly photos; follow surgeon protocol |
| Definition seems uneven | Swelling is rarely perfectly symmetric | Wait for stabilization before judging symmetry |
| Nose looks “bigger” than expected | Early edema; thick tissue holds fluid longer | Focus on timeline, not day-to-day changes |
Revision risk: when it’s considered and why waiting matters
It’s normal to research revision rhinoplasty for thick skin—especially if you’re anxious about definition. But thick skin makes “early revision thinking” particularly risky because swelling can mimic problems that aren’t actually structural issues.
In many cases, surgeons prefer to wait until healing stabilizes before labeling something as a true indication for revision. The reason is simple: thick-skin healing can continue evolving for a long time, and operating too early can introduce new scar behavior that further blurs definition.
Practical guidance: If your main concern is definition and your surgeon says healing is on track, give your nose time—because thick skin often shows its best refinement later in the first year (and sometimes beyond).
That said, if there are functional issues (breathing), major asymmetries that persist after the swelling window, or structural concerns confirmed on follow-up, a carefully planned revision rhinoplasty for thick skin may be appropriate. The key is surgeon-led assessment at the right time—not self-diagnosis based on early photos.

Choosing the Best Rhinoplasty Surgeon for Thick Skin
With thick skin, surgeon selection matters because the “win condition” is different: you’re not just chasing immediate sharpness — you’re investing in a stable structure, careful soft-tissue handling, and a long-term follow-up plan that respects biology. The credentials checklist also looks different: beyond the headline board certification, look for a surgeon whose case portfolio includes specifically thick-skinned patients with time-stamped 12-month and 18-month results, not just thin-skin “wow” cases. The complete credential verification framework — including TPCD/EBOPRAS/ISAPS public registries, fellowship pedigree, and the specific markers that distinguish a thick-skin-experienced rhinoplasty specialist from a generalist — is detailed in our surgeon evaluation guide.
What to ask in consultation (technique, grafting, follow-up plan)
Use your consultation to evaluate thinking, not just photos — but credentials still matter as the foundational filter. Beyond surgeon-led planning and structured follow-up, verify that the surgeon holds active board certification from a recognized rhinoplasty-relevant body (EBOPRAS, ABFPRS, ABPS, or country-specific equivalents) and that the credential is current rather than lapsed. Public registry verification takes minutes and is the single highest-leverage step in pre-booking due diligence. The complete board certification verification protocol — including registry lookup steps, credential expiration patterns, and the specific differences between facial-plastic-surgery boards and general plastic surgery boards — is detailed in our board certification verification guide.
- “How does my skin thickness change your surgical plan?” (Listen for structural support, not vague promises.)
- “How do you build tip definition in thick skin?” (They should discuss support and realistic outcomes.)
- “What is your expected thick skin rhinoplasty swelling duration for a case like mine?” (They should normalize a longer timeline.)
- “Do you use grafting or structural support in thick-skin noses, and why?” (Expect individualized reasoning.)
- “What is your follow-up schedule, and how do you manage prolonged swelling?” (A plan for monitoring matters.)
- “When do you consider revision rhinoplasty for thick skin, and what criteria do you use?” (Look for patience and clear milestones.)
Beyond credentials, the consultation itself reveals more than any photo gallery — but only if you arrive with the right questions. The depth of a surgeon’s answer to “how does my skin thickness change your surgical plan?” or “what is your expected swelling duration for a case like mine?” tells you more about thinking quality than any aesthetic outcome can. The complete pre-consultation question framework — including 25 vetted questions organized by topic (technique, recovery, revision policy, complication management) — is detailed in our consultation questions checklist.
Perform your surgery with confidence. Meet our European Board Certified surgeons with over 2,000 successful facial surgeries.
What a good thick-skin plan includes (pre-op + post-op roadmap)
A strong thick-skin plan usually feels “structured” from start to finish. It doesn’t promise instant definition; it explains how definition is built and when it’s expected to appear.
| Phase | What a High-Quality Plan Typically Includes | Why It Matters for Thick Skin |
|---|---|---|
| Pre-op | Clear goal-setting, realistic expectations, photo analysis at multiple angles | Prevents “template nose” goals that thick skin won’t display naturally |
| Surgery | Framework support strategy + careful soft-tissue handling | Supports better long-term results of thick skin rhinoplasty |
| Early recovery | Swelling management basics + surgeon-specific instructions | Reduces unnecessary inflammation that can prolong thick skin rhinoplasty swelling duration |
| Mid/late recovery | Milestone-based assessment (months, not weeks) + photo tracking guidance | Protects you from misreading early “puffiness” as a final result |
| Revision policy | Clear criteria + timing guidance for revision rhinoplasty for thick skin | Prevents premature revision decisions before healing stabilizes |
Also ask how the clinic supports your longer recovery window—especially if you’re traveling for care. Thick-skin cases often benefit from consistent follow-up and a plan for swelling fluctuations.
Red flags in clinics/claims (too-fast promises, one-size-fits-all)
Because thick skin can delay visible definition, it’s a common target for unrealistic promises. Be cautious of clinics that advertise “instant final definition,” “easy skin thinning,” or pressure toward early revision before the swelling timeline has stabilized — these red flags are particularly common in clinic marketing aimed at thick-skin patients precisely because the longer healing window creates an opening for impatience-based upsells. The complete clinic-evaluation framework — including JCI accreditation criteria, OR class verification, and the specific safety infrastructure markers that separate boutique medical-tourism setups from full-spectrum hospital environments — is detailed in our facility evaluation guide.
Bottom line: In thick-skin cases, a trustworthy surgeon won’t “sell sharpness.” They’ll explain a strategy grounded in anatomy and scientific research, then guide you patiently through the longer definition timeline.
How to Track Progress After Thick Skin Rhinoplasty Without Second-Guessing
Patients researching rhinoplasty thick skin often feel anxious because the “after” doesn’t look crisp right away. A simple, structured tracking plan keeps you grounded in realistic milestones, helps your surgeon evaluate changes objectively, and reduces the temptation to judge results from day-to-day fluctuations. It also protects you from unfair comparisons to thin-skin timelines and from making revision decisions before swelling has stabilized.
Create a Consistent Photo Timeline
Take photos in the same lighting, angle, and distance: front, both obliques, and both profiles. Capture them at consistent checkpoints (e.g., 2 weeks, 6 weeks, 3 months, 6 months, 12 months). This makes it easier to see true trends in rhinoplasty thick skin swelling rather than temporary puffiness from sleep position, salt intake, travel, or a busy week.
Measure Progress Beyond Tip “Sharpness”
Instead of focusing only on tip definition, track overall balance: bridge smoothness, tip rotation, nostril symmetry, and how your nose fits your facial proportions. Many thick-skin noses look “softer” early but become more refined as tissue redrapes. Notes like “breathing feels clearer” or “profile hump reduced” can be more meaningful than chasing an early, ultra-defined tip.
Know When to Contact Your Surgeon
During rhinoplasty thick skin recovery, normal swelling usually improves gradually and may be uneven from side to side. Reach out promptly if you notice sudden rapid swelling, increasing pain, fever, unusual drainage/odor, or significant skin color changes. When in doubt, a quick check-in is safer than waiting—especially if you’re traveling for care. Bring your photo series to follow-ups for clearer, objective comparisons.
For international patients pursuing thick-skin rhinoplasty in Istanbul, the planning structure matters as much as the surgical technique itself — pre-arrival photo documentation, in-person measurement validation, day-of-surgery vector confirmation, and a structured 12-month remote follow-up cadence designed specifically to respect the longer thick-skin definition timeline. The complete step-by-step pathway — including pre-arrival WhatsApp coordination, splint removal protocol, in-Istanbul follow-up schedule, and remote photo-monitoring designed for the 6-month, 9-month, and 12-month thick-skin milestone reviews — is documented on our patient journey roadmap hub.
Frequently Asked Questions (FAQ): Thick Skin Rhinoplasty
Below are the most common questions patients ask during thick skin rhinoplasty recovery. Keep in mind that thick skin changes the timeline more than it changes the potential—so many “worries” are actually normal healing milestones.
How long does swelling last after thick skin rhinoplasty?
Thick skin rhinoplasty swelling duration is often longer than in thin-skin cases. Many patients see meaningful improvement in the first 3–6 months, but tip swelling can continue refining through 9–12+ months (and sometimes longer). The key is a gradual downward trend over time, not day-to-day consistency.
When will I see tip definition with thick skin?
Often later than you expect. The bridge may look improved earlier, while tip definition “arrives” more slowly. Many patients start noticing clearer definition between months 4–6, with the most representative results of thick skin rhinoplasty commonly visible around 9–12 months.
Does thick skin make rhinoplasty results less dramatic?
Not necessarily. Thick skin can soften very sharp detailing, but it can still produce a clearly improved, refined, and natural-looking nose. In fact, thick skin can sometimes hide tiny irregularities better than thin skin. The main difference is that the final look can be more “naturally refined” than “ultra-sculpted.”
Can steroid injections help swelling—and are there risks?
Beyond clinical evaluation, financial planning for a longer thick-skin recovery window can affect choices — including whether to factor in a potential follow-up Istanbul visit at the 12-month mark for steroid injection, refinement, or simply a comprehensive in-person re-evaluation. The complete rhinoplasty pricing transparency framework — including what's bundled in the all-inclusive Istanbul model versus what's itemized in US billing structures, how thick-skin extended-recovery follow-ups are handled, and the realistic budget for potential later refinement — is detailed on our rhinoplasty cost transparency page.
Is taping necessary for thick skin noses?
Not always, but it can be helpful for some patients—especially to support redraping and swelling control in thick skin cases. The key is using a surgeon-prescribed technique. Incorrect taping (too tight, wrong placement, too long) can irritate skin and may worsen inflammation.
What increases prolonged swelling (exercise, smoking, supplements)?
Common triggers include heavy exercise too early, high-sodium diets, alcohol, and nicotine exposure. Smoking and nicotine are especially important because they can impair microcirculation and healing. Also tell your surgeon about all supplements and medications—some may increase bruising or affect inflammation and recovery.
How do I know if my swelling is normal or a complication?
Normal swelling tends to fluctuate and slowly improve over weeks and months. Contact your surgeon promptly if you have sudden rapidly increasing swelling (especially one-sided), worsening pain, fever, concerning drainage/odor, or significant skin color changes. When in doubt, it’s always safer to check in—especially during the early phase of thick skin rhinoplasty recovery.
Can thick or oily (sebaceous) skin trigger breakouts after rhinoplasty?
Yes—temporary changes in cleansing, occlusive tape, and healing inflammation can contribute to breakouts. Use a gentle, fragrance-free cleanser, avoid harsh exfoliants early, and choose non-comedogenic moisturizer and sunscreen. If acne flares, ask your surgeon when it’s safe to restart targeted skincare.
When can I wear glasses after rhinoplasty if I have thick skin?
Glasses timing depends mainly on your nasal framework healing and your surgeon’s protocol, not skin thickness alone. If you must wear glasses early, your team may recommend alternatives like contact lenses or a protective support method to avoid pressure on the healing nose.
Does scientific evidence support different techniques for thick-skinned noses?
Yes—research emphasizes structured support and realistic expectation-setting. For deeper reading, clinicians often reference “rhinoplasty for thick-skinned noses: a systematic review” when discussing how thick tissue can affect definition and the longer settling phase.
How long does firmness and numbness last after thick-skin rhinoplasty?
Firmness and mild numbness can persist as tissues remodel and sensation returns, especially around the tip. Your exact thick skin rhinoplasty healing time varies, but gradual month-to-month softening is typical—follow your surgeon’s milestones before judging final texture or contour.
Medical Disclaimer: This page is provided for general educational purposes only and does not replace a face-to-face medical consultation, diagnosis, or personalized treatment plan. All surgery carries risks and outcomes vary between individuals. Suitability for a rhinoplasty (nose job), procedure selection, and anesthesia choice can only be determined after a full clinical assessment by a qualified surgeon. Always follow your clinician’s instructions and seek urgent medical attention if you develop concerning symptoms during recovery.
Related Treatments
Ready to Start Your Own Transformation Journey?
Join the 2,000+ patients who trusted Dr. Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, revitalized you begins with a simple, no-obligation conversation. Contact us today from the USA for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. No hidden fees.
#2: Secure Your Date & VIP Booking
Once you're ready, our dedicated patient coordinators will help you secure your procedure date. We'll handle all your bookings, including your 5-star hotel and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you'll meet your specialist surgeon to finalise the details for your "natural, subtle, and revitalized" new look.















