How to Speed Up Facelift Recovery: The Power of HBOT and Laser Therapy

If you’re researching how to speed up facelift recovery, you’re already thinking like an “expert patient”: you don’t just want a good result—you want a safe healing process, minimal downtime, and the lowest possible risk of complications or visible scarring.
In this guide, we’ll break down what facelift recovery typically looks like (including deep plane facelift recovery and SMAS facelift recovery), what really drives healing at a biological level, and why two recovery-support technologies—Hyperbaric Oxygen Therapy (HBOT) and Low-Level Laser Therapy (LLLT)—can be powerful additions to a surgeon-led aftercare plan.
Key takeaway: The goal isn’t to “hack” healing—it’s to give your body the right conditions to heal efficiently: oxygen delivery, controlled inflammation, protected incisions, and smart timing.
Throughout the article, you’ll also find practical facelift recovery tips, a realistic facelift recovery timeline, and a “day-by-day” framework so you can plan travel, work, and social downtime with fewer surprises.
Table of Contents
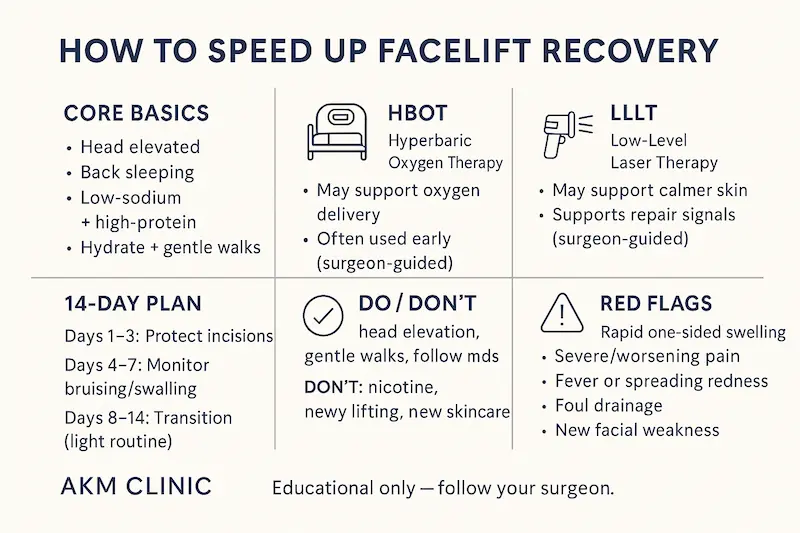
Facelift Recovery Basics: What “Normal” Healing Looks Like (and What’s Not)
Before you add any advanced support, you need a baseline: what is the stages of facelift recovery supposed to look like? Most anxiety comes from not knowing what’s normal—especially when comparing your swelling to someone else’s deep plane facelift recovery day by day photos online. Photos can be helpful, but they can also be misleading because lighting, angles, skin thickness, bruising tendency, and surgical technique all change the visual story.
Typical swelling & bruising timeline (what many patients experience)
Here’s a practical overview of facelift recovery time. Your surgeon’s plan and your individual biology matter most, but these ranges help answer “how long is facelift recovery?” in real-world terms:
| Timeframe | What You May Notice | What Usually Helps (Surgeon-Approved Basics) |
|---|---|---|
| Days 1–3 | Peak swelling, tightness, fatigue; bruising may start to appear | Head elevation, prescribed meds, cold compresses (if approved), hydration |
| Days 4–7 | Swelling slowly starts to shift; bruising can look “worse” before it looks better | Gentle walking, careful incision care, consistent sleep positioning |
| Days 8–14 | Visible improvement; lingering swelling (often along jawline/neck) | Follow-up checks, gradual return to light routines, sun avoidance |
| Weeks 3–6 | Most social bruising fades; swelling continues to refine | Scar care plan, gradual activity increase, skin support as advised |
| Months 3–12 | Scar maturation and deep tissue settling; “final” refinement | Long-term sun protection, consistent scar strategy, healthy habits |
Important: Deep plane and SMAS facelifts both involve deeper structural work than surface-only tightening. That can mean the early phase feels more “tight” and swollen, even though many patients also report a more natural, durable outcome when done well. Your recovery time for deep plane facelift can be similar to SMAS for many patients, but the first two weeks often require careful, structured aftercare.
Why facelifts can temporarily challenge blood flow (why recovery support matters)
Facelifts involve surgical dissection, repositioning, and tissue healing. In simple terms: your body must deliver enough oxygen and nutrients to recovering tissues while also managing inflammation and rebuilding collagen. During early recovery, tissues can be swollen and “demand” more support. That’s why structured aftercare is not optional—it’s the foundation of a smoother day by day facelift recovery.
Factors that can slow healing (even if surgery was technically perfect)
- Nicotine exposure (including vaping and patches) can impair circulation and wound healing.
- Unmanaged swelling triggers: high sodium intake, dehydration, poor sleep positioning.
- Medication/supplement conflicts: some increase bruising risk; never self-adjust—ask your surgeon.
- Underlying conditions (thyroid issues, diabetes, anemia) can change recovery patterns.
- Overactivity too soon: raising blood pressure and increasing swelling or bleeding risk.
Clinical mindset: When patients ask for “faster healing,” what they usually want is lower swelling, less bruising, calmer skin, and confidence that the tissues are safe. That’s exactly where targeted recovery support can be useful—when it complements (not replaces) surgeon-led care.
Our philosophy is “Rejuvenation, Not Alteration.” Discover how our surgeons achieve subtle, revitalized results that honor your unique beauty.
The Science of Faster Healing: What Your Body Needs After a Facelift
Whether your procedure was a classic facelift, recovery from deep plane facelift, or SMAS facelift recovery, the biology of healing is consistent. If you want to speed up facelift recovery safely, focus on the three drivers below—because HBOT and laser therapy are designed to support these exact mechanisms, as supported by medical science.
1) Oxygen delivery & tissue perfusion
Oxygen supports cellular repair and helps tissues meet the demands of recovery. When swelling and inflammation are present, oxygen delivery can be less efficient. Strategies that optimize oxygen availability (clinically and safely) may support smoother healing—especially for patients who prioritize minimizing downtime.
2) Inflammation control (without “over-suppressing” healing)
Inflammation is not the enemy—it’s part of healing. The goal is controlled inflammation: enough to repair, not so much that swelling and discomfort linger. Your surgeon’s plan (medications, positioning, activity limits) is the baseline, and supportive therapies can be layered appropriately.
3) Collagen remodeling & scar maturation
Collagen remodeling is the long game of facelift recovery. Early on, you want incisions protected and calm. Later, you want scars to mature flatter and less visible. This is also where surgeon-guided skincare and (when appropriate) energy-based support can play a role.
Next, we’ll get very specific about the two recovery tools you asked about—HBOT and laser therapy (LLLT)—including what a session feels like, who it’s for, who should avoid it, and how it fits into a real-world recovery schedule.
HBOT Explained: How Hyperbaric Oxygen Therapy Can Accelerate Recovery
When patients search for how to speed up facelift recovery, they’re usually trying to reduce three things: swelling, bruising, and the “long tail” of downtime that can stretch the facelift recovery timeline longer than expected. HBOT (Hyperbaric Oxygen Therapy) is one of the most evidence-backed medical tools used in wound-care settings to support tissue healing—and in a facelift context, it’s used as an adjunct to surgeon-led aftercare (not a replacement for it).
Whether you’re planning deep plane facelift recovery or SMAS facelift recovery, the early healing environment matters. In the first days, tissues are swollen and metabolically “hungry.” This is where HBOT can be strategically valuable for patients who want a smoother day by day facelift recovery experience.
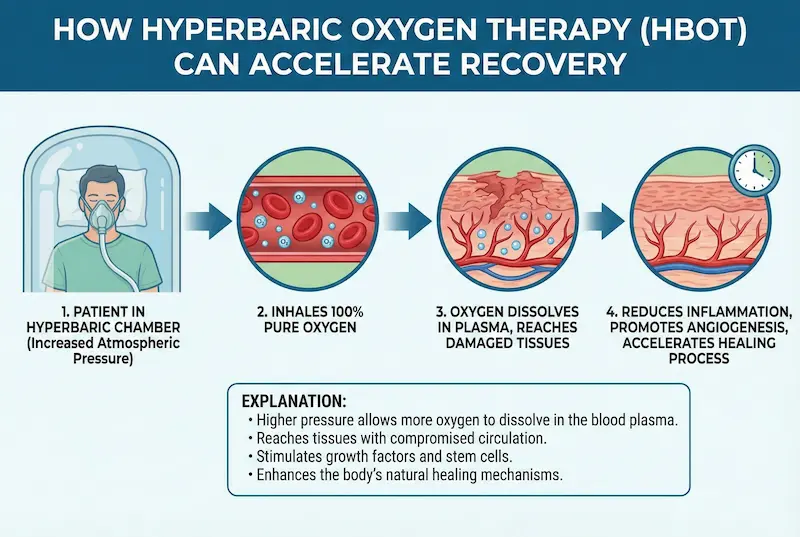
What HBOT is (and what a session feels like)
HBOT is a treatment where you breathe 100% oxygen in a pressurized chamber. The experience is often described as similar to airplane takeoff/landing pressure changes: you may need to equalize your ears (swallowing, yawning, gentle techniques your provider teaches). During the session, you typically rest comfortably—many patients listen to music or simply relax.
- Before: You’re screened for safety (ear/sinus issues, lung history, certain medications).
- During: The chamber pressure increases gradually; you breathe oxygen under pressure.
- After: You may feel relaxed; some people notice temporary ear “fullness.”
Recovery mindset: HBOT is not about “forcing” healing. It’s about giving healing tissue more oxygen availability during a period when it can be harder for the body to deliver it efficiently.
The mechanism: why oxygen under pressure matters after surgery
Here’s the key concept: under pressure, oxygen can dissolve more effectively into the liquid portion of your blood (plasma). This helps oxygen reach tissues even when swelling temporarily affects microcirculation. In post-surgical recovery, that can support:
- Tissue resilience during peak swelling
- Cellular repair processes that rely on oxygen availability
- Healthy collagen remodeling and scar maturation support
This is especially relevant for patients who are tracking stages of facelift recovery closely and want to reduce the “uncertain” phase where swelling makes results look uneven or tight.
Practical benefits after facelift: swelling, downtime, scars, and tissue support
In a facelift setting, HBOT is commonly chosen to support the recovery goals most patients care about:
- Swelling management: By supporting oxygen availability to healing tissues, HBOT may help the body resolve postoperative swelling more efficiently.
- Downtime reduction: Many patients define “faster recovery” as returning to normal routines sooner—even if subtle swelling continues for weeks.
- Incision and scar support: Oxygen is a major input for tissue repair; HBOT may support healthier wound healing and collagen organization over time.
- Risk-awareness benefit: In surgical wound care, oxygen-rich environments can support the body’s defenses; this is one reason HBOT has a long history in complex wound support (your surgeon will decide if it’s appropriate for you).
A note for “comparison shoppers”: if you’ve been looking at deep plane facelift recovery day by day photos, remember that photos rarely show the whole picture (lighting, angles, skin thickness, bruising tendency, and even makeup). HBOT isn’t a guarantee of “photo-perfect” recovery—think of it as stacking the odds toward calmer tissue conditions.
A realistic HBOT schedule: what patients often do (and why timing matters)
Patients often ask, “How many sessions will I need?” The honest answer is: it depends on your surgical plan, your healing biology, and your surgeon’s protocol. But to help you plan travel and expectations, here’s a realistic framework used in many recovery-focused programs.
| Recovery Window | Why It Matters | HBOT Goal | Typical Session Logic (Example) |
|---|---|---|---|
| Days 1–3 | Peak swelling begins; tissue demand is high | Support oxygen availability during the most “reactive” phase | 1 session/day if medically appropriate |
| Days 4–7 | Bruising/swelling can shift and look uneven | Encourage smoother progression through early stages | Several sessions across the week |
| Days 8–14 | Visible improvement accelerates; scars are still “fresh” and active | Support repair consistency and calm tissue environment | Selective sessions based on swelling/bruising pattern |
This structure can be especially helpful for patients traveling for surgery, because the first 7–10 days are often the “highest value” window for hands-on monitoring and structured support. It also aligns well with the most common question: how long is facelift recovery if you need to be “socially present” again?
Practical expectation: Even with excellent care, a facelift can have a long refinement phase. HBOT is most relevant for improving the early recovery experience—when swelling, bruising, and tissue sensitivity are highest.
Who may benefit most (and who should avoid HBOT)
HBOT is not “for everyone,” and any ethical clinic should screen properly. In general, patients who may be considered for HBOT as part of facelift recovery tips and planning include:
- Patients who want a structured, medically supervised recovery plan
- Patients with higher anxiety about prolonged swelling/bruising
- Patients focused on minimizing downtime during recovery from deep plane facelift or SMAS procedures
However, HBOT can be inappropriate in certain situations. A proper medical screen commonly evaluates:
- Ear/sinus issues that make pressure equalization difficult
- Lung history (HBOT is contraindicated in specific conditions)
- Uncontrolled claustrophobia (often manageable, but needs planning)
- Medication considerations (your provider reviews this carefully)
Bottom line: HBOT should be used only when it is medically appropriate and integrated into a surgeon-led plan. If any clinic suggests HBOT as a “magic guarantee,” that’s a red flag—not a benefit.
Laser Therapy (LLLT) Explained: How “Cold Laser” Supports Skin Repair
When people search for facelift recovery tips, they often focus on “what to do” (sleep upright, avoid salt, take meds correctly). But there’s also a second layer: how to support the biology of healing—especially skin recovery, redness, bruising, and scar quality. That’s where Low-Level Laser Therapy (LLLT)—sometimes called “cold laser”—can be a smart, surgeon-guided add-on during facelift recovery.
LLLT is not the same as aggressive resurfacing lasers. It’s designed to be non-ablative, low-intensity light therapy that supports cellular energy and inflammation control. For patients tracking a facelift recovery timeline day by day, LLLT is often used to help the skin look calmer sooner—while deeper tissues continue their natural settling process.
What LLLT is (and why medical-grade matters)
LLLT uses targeted light energy to encourage cellular repair. You’ll often see at-home LED masks marketed for “post-procedure glow,” but recovery-focused LLLT is typically different in three practical ways:
- Power and consistency: medical-grade systems deliver controlled output with clinical protocols.
- Coverage: larger, evenly distributed diode arrays can treat broader areas consistently.
- Timing and supervision: it’s integrated into a surgeon-led plan so it doesn’t interfere with incision care.
| Option | Typical Goal | Best Use Case | Limitations |
|---|---|---|---|
| Medical-grade LLLT | Support repair + calm inflammation | Post-surgical recovery support (surgeon-directed) | Requires proper screening + protocol |
| At-home LED masks | General skincare maintenance | Non-surgical routine, long-term skin habits | Lower power; inconsistent dosing; not a substitute for medical aftercare |
Important: In early recovery, “more” is not better. The right timing and the right settings matter more than intensity.
How LLLT works: the “cellular energy” effect (ATP support)
LLLT is often explained as photobiomodulation—light energy influences cellular processes. In practical terms, one key goal is supporting the cell’s energy system (often discussed as ATP production). When tissues have more efficient cellular energy availability, they can better manage repair tasks like:
- Reducing excessive inflammatory signaling (helping redness and “heat”)
- Supporting collagen organization during healing
- Encouraging a calmer skin appearance while deeper healing continues
This matters for patients who are comparing their own progress to deep plane facelift recovery day by day photos online. Those photos tend to focus on visible skin changes, but healing is happening at multiple layers—LLLT is aimed at supporting that surface recovery layer in a controlled way.
What a session feels like (and what it should NOT feel like)
A properly delivered LLLT session is usually comfortable. Many patients describe it as gentle warmth or simply “nothing at all.” What you should not experience is significant heat, burning, or irritation—those can be signs the modality is not appropriate for early recovery or is not being used correctly.
- Duration: often a short, protocol-based session
- Comfort: relaxed; no downtime added
- After: skin may appear temporarily brighter or calmer
Why it’s relevant for deep plane and SMAS facelift recovery
Patients researching deep plane facelift recovery or SMAS facelift recovery often worry about two things at once: “Is my deeper healing on track?” and “When will I look normal in photos?” Deep plane and SMAS techniques focus on structural support; that’s excellent for natural results, but it means recovery has layers:
- Deep tissue settling (structure + swelling resolution)
- Skin recovery (redness, texture, bruise visibility)
- Scar maturation (weeks to months)
LLLT is primarily a “skin recovery support” tool that can make the visible phase feel smoother—while you still respect the true recovery time for deep plane facelift and don’t rush activity too soon.
A realistic LLLT timeline: when it may be added
Patients ask for a day by day facelift recovery plan, but the safest answer is always: “Follow your surgeon’s timing.” Still, here’s a practical framework many surgeon-led protocols use to think about it:
| Recovery Window | Typical Priority | Where LLLT May Fit |
|---|---|---|
| Days 1–3 | Protect incisions, control swelling | Often delayed or used selectively depending on incision status |
| Days 4–7 | Calm inflammation; manage bruising visibility | Common window to introduce gentle, supervised sessions |
| Days 8–14 | Improve “camera readiness” while healing continues | Often continued to support calm skin appearance |
| Weeks 3–6+ | Scar strategy, long-term refinement | May be used as part of a broader scar/skin protocol |
If you’re trying to plan “how long is facelift recovery until I look presentable?” the most honest answer is: most patients look socially acceptable in weeks, but subtle swelling can last longer. LLLT can help improve the visible phase, but it doesn’t replace time-dependent deep healing—especially in recovery from deep plane facelift.
Dermatosurgeon perspective: why skin quality matters as much as structure
For truly natural facelift outcomes, it’s not enough to reposition deeper tissues—you also need to respect and support skin quality during healing. A dermatosurgeon-led viewpoint emphasizes that recovery isn’t only “swelling going down”; it’s also:
- Minimizing prolonged redness and irritation
- Supporting healthy collagen remodeling
- Protecting pigment (especially with strict sun avoidance)
- Using energy-based support only when it’s safe and timed correctly
Good recovery is quiet recovery: calm skin, stable incisions, controlled swelling, and steady improvement—without “pushing” the tissue.
HBOT vs LLLT vs Standard Aftercare: What Each One Does Best
Let’s be clear: the fastest, safest facelift recovery still starts with excellent surgery and disciplined aftercare. HBOT and laser therapy (LLLT) are not “shortcuts.” They’re support tools that can improve the recovery environment—especially for patients who want to speed up facelift recovery in a medically responsible way.
This section will help you decide what’s actually doing the heavy lifting during deep plane facelift recovery or SMAS facelift recovery, and how each option fits into a realistic facelift recovery timeline.
What standard aftercare does best (the non-negotiables)
Standard aftercare is the foundation. If this is weak, no technology will “save” recovery. The basics that most surgeon protocols emphasize include:
- Incision protection: cleaning, ointments, dressings, and zero “DIY” products without approval
- Swelling control: head elevation, medication adherence, activity limits
- Complication prevention: recognizing early warning signs and getting fast clinical assessment
- Scar strategy: timing-based scar care + strict sun protection
If you want the best facelift recovery tips in one sentence: protect incisions, control swelling, keep blood pressure stable, and follow your surgeon—not the internet.
What HBOT does best (oxygenation + tissue resilience during peak swelling)
HBOT’s “lane” is oxygen support when healing demand is high—especially early in recovery. Because it uses 100% oxygen in a pressurized environment, the goal is to increase oxygen availability to recovering tissues during the most reactive period.
Patients who are anxious about prolonged swelling or who want the most structured path through the early stages of facelift recovery often see HBOT as a “recovery stabilizer”—not a cosmetic add-on.
- Best for: early swelling/downtime support, tissue resilience, structured recovery planning
- Most relevant window: typically the first 1–2 weeks (surgeon-directed)
- Not for: replacing proper wound care, “speed running” activity, or skipping follow-ups
What LLLT does best (calmer-looking skin + cellular repair support)
LLLT’s “lane” is supporting a calmer visible recovery—helping the skin look less reactive while deeper tissues continue to settle. It’s especially appealing for patients who care about returning to video calls, social settings, and normal routines without feeling “obviously post-op.”
In AKM Clinic’s recovery approach, LLLT is delivered using a medical-grade system with 650nm wavelength and a 424-diode array—designed to support cellular energy (often discussed as ATP support), collagen signaling, and inflammation control as part of a supervised aftercare plan.
- Best for: calming redness/inflammation, supporting skin repair, helping the “camera-ready” phase
- Most relevant window: often introduced after the very earliest incision-critical stage (surgeon-directed)
- Not for: aggressive resurfacing in early recovery, pushing heat into healing tissues, or DIY devices used too soon
Why combining HBOT + LLLT can be synergistic (different problems, different solutions)
Think of HBOT and LLLT as addressing two different layers of recovery:
- HBOT supports the “internal healing environment” (oxygen availability and tissue resilience during swelling-heavy days).
- LLLT supports the “surface recovery experience” (calmer skin behavior and repair signaling over time).
When integrated properly, the combination can make day by day facelift recovery feel more predictable: fewer “why do I look worse today?” moments, and a steadier progression through the early timeline—while still respecting the true biological pace of healing, especially in recovery time for deep plane facelift.
| Recovery Tool | Primary Role | Best Timing (General) | What It Can’t Do |
|---|---|---|---|
| Standard Aftercare | Protect incisions + prevent complications | Immediately, throughout recovery | It can’t change biology overnight—healing still takes time |
| HBOT | Oxygen support during high-demand healing | Often most useful in Weeks 0–2 | It can’t replace proper wound care or fix poor surgical technique |
| LLLT | Skin repair support + calmer inflammation | Often added after the earliest incision-critical phase | It can’t “erase” swelling instantly or substitute for time-dependent deep healing |
Bottom line: If your question is “how long is facelift recovery,” the honest answer is that recovery has phases. Technology can improve the quality and predictability of recovery, but it must be paired with excellent surgery, monitoring, and disciplined aftercare—especially in deep plane facelift recovery where deeper tissues are doing real structural work.
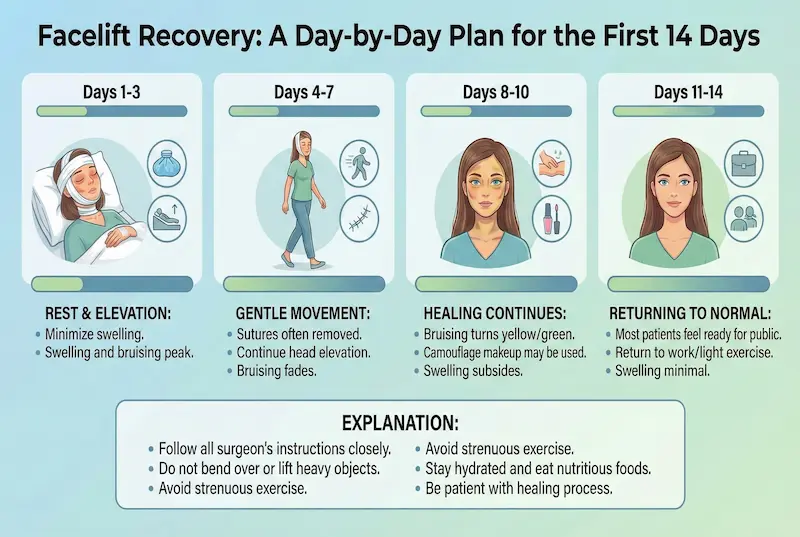
A Practical Recovery Protocol: A Day-by-Day Plan for the First 14 Days
If you want a realistic, actionable answer to how to speed up facelift recovery, the “secret” is not a single product—it’s a tight first-14-day protocol. This is the window where most of the visible swelling and bruising behavior is determined, and it’s the phase that shapes your experience of the overall facelift recovery timeline.
This plan is designed for patients who want structure—especially those planning deep plane facelift recovery or SMAS facelift recovery. Use it as a framework, then follow your surgeon’s personalized instructions as the final authority.
Reality check: “Fast recovery” usually means faster comfort and social readiness—not instant healing. Deep tissues still need time to settle, especially in recovery from deep plane facelift.
Before you start: set up a “recovery tracking system” (so you don’t spiral)
Many patients compare themselves to deep plane facelift recovery day by day photos online. That can be helpful—but only if you standardize your own tracking the same way.
- Take daily photos in the same lighting, same distance, same angles (front/left/right/45°), same time of day.
- Track symptoms (tightness, swelling, bruising color, pain score) with a simple notes app.
- Log your “inputs”: sleep position, sodium intake, hydration, walking, medications.
This reduces anxiety and helps your surgeon interpret what’s happening—especially if you’re traveling and relying on remote follow-up.
We use advanced Hyperbaric Oxygen Therapy (HBOT) to minimize downtime and supercharge your healing process. Safety is our #1 promise.
Day 0–2: Protect incisions, control swelling, keep blood pressure stable
These first 48 hours are where you earn a smoother facelift recovery time. Your main job is to be predictable: rest, elevate, hydrate, and avoid anything that spikes swelling.
| Goal | Do This | Avoid This |
|---|---|---|
| Minimize swelling | Sleep with head elevated; stay consistent with meds; gentle hydration | Bending over, heavy talking/laughing, salty meals, alcohol |
| Protect incisions | Follow cleaning/dressing instructions exactly; keep hands off | Applying “healing creams” not approved by your surgeon |
| Prevent pressure spikes | Short walks at home; stool softener if prescribed; calm breathing | Straining, heavy lifting, intense emotions or overheating |
Where HBOT/LLLT may fit: Some surgeon-led recovery programs consider HBOT very early (when medically appropriate) to support oxygen availability during peak swelling. Laser therapy (LLLT) is often introduced more selectively depending on incision status.
Day 3–7: Bruising shifts, swelling can look “uneven,” and this is normal
This is the stage that confuses patients the most. Bruising can migrate downward, swelling can look asymmetric, and your face can feel tight. This is often still well within normal stages of facelift recovery.
- Keep walking (gentle, frequent). Movement supports circulation and reduces “stagnant” swelling.
- Stay strict on sleep positioning. One bad night flat on your side can noticeably change swelling the next day.
- Keep sodium low and hydration steady. Swelling is extremely sensitive to this.
| Common Concern | What It Often Means | What You Should Do |
|---|---|---|
| Bruising looks darker or “moves” | Normal bruise breakdown and gravity shift | Don’t panic; continue gentle walking and follow aftercare |
| One side looks more swollen | Normal variability + sleep positioning effects | Return to strict head elevation; monitor with standardized photos |
| Tightness/firmness | Swelling + healing tissues settling | Follow surgeon guidance; avoid aggressive massage unless approved |
Where HBOT/LLLT may fit: This is a common window for structured recovery support—HBOT can still be relevant for swelling-heavy days, and LLLT is often introduced to help calm visible skin inflammation (only when your surgeon confirms it’s appropriate).
Day 8–14: Social readiness improves, but deep healing continues
By the second week, most patients see a noticeable improvement in “public appearance,” which is why many people ask: how long is facelift recovery until I look normal? For many, this is the phase where you feel more like yourself—yet subtle swelling can still persist for weeks, particularly along the jawline and neck.
- Transition carefully back to light routines (not workouts).
- Stay sun-avoidant. UV exposure can worsen redness and scar pigmentation.
- Follow scar guidance exactly (timing matters more than products).
If you’re tracking day by day facelift recovery, Week 2 is usually when improvements become “compounding.” But this is also when patients get overconfident and overdo activity—one of the most common reasons swelling lingers and the facelift recovery timeline feels longer.
The 14-day recovery checklist (printable mindset)
- Head elevation: consistent every night for at least the first 10–14 days (or per your surgeon).
- Steps > stairs > workouts: walking is your friend; exercise waits for clearance.
- Salt discipline: low sodium is one of the highest-impact “small” habits.
- No nicotine: not even “just one” (it can compromise healing).
- Incision minimalism: only what your surgeon approves, nothing extra.
- Standardized photos: daily for 2 weeks, then 2–3x/week.
If you want one strategy that truly speeds up recovery: avoid setbacks. Most “slow recoveries” are not a lack of healing—they’re small preventable flare-ups (salt, poor sleep positioning, early exertion, unapproved products).
Deep plane vs SMAS: what changes in the first 14 days?
Patients often ask if recovery time for deep plane facelift is longer than SMAS. In practice, the first 14 days can look similar on a calendar, but the experience can differ:
- Deep plane facelift recovery: more structural work can mean a “deeper” tightness feeling early on, with steady refinement as swelling resolves.
- SMAS facelift recovery: also involves deeper layers; swelling patterns can still vary significantly by patient and technique.
In both cases, your “visible” improvement can outpace your “deep tissue” healing. That’s why Week 2 often looks good in photos but still requires caution.
Our philosophy is “Rejuvenation, Not Alteration.” Discover how our surgeons achieve subtle, revitalized results that honor your unique beauty.
At-Home Steps That Speed Up Facelift Recovery (Surgeon-Logic, Not Myths)
The best facelift recovery tips are often unglamorous: positioning, hydration, controlled activity, incision minimalism, and sun discipline. These habits don’t “feel” high-tech, but they consistently shape the early facelift recovery timeline—especially in deep plane facelift recovery and SMAS facelift recovery, where deeper layers are healing and settling.
Below is a surgeon-logic checklist you can follow at home to support a smoother facelift recovery time without risking setbacks.
The recovery rule: Don’t chase speed—chase stability. Most “slow recoveries” happen because of preventable flare-ups (salt, overactivity, side-sleeping, unapproved skincare).
1) Sleep position: the simplest way to reduce swelling day by day
If you’re tracking day by day facelift recovery photos, sleep position is one of the most common reasons your swelling looks different from one day to the next. Your goal is to keep fluid from pooling.
- Head elevation: Use pillows or a wedge so your head is consistently elevated.
- Back sleeping: Side sleeping early on often worsens swelling and can create asymmetry.
- Consistency matters: One “flat night” can set back the next 24–48 hours visually.
| Habit | Why It Matters | What to Do Instead |
|---|---|---|
| Side sleeping | Encourages one-sided swelling | Back sleeping + head elevation |
| Sleeping flat | Fluid pooling increases puffiness | Use a wedge or stacked pillows |
| Frequent position changes | Micro-trauma + pressure shifts | Stabilize with supportive pillows |
Deep plane note: During recovery from deep plane facelift, patients often report deeper “tightness” early on. Stable sleep positioning helps keep that tightness from being amplified by extra swelling.
2) Nutrition & hydration: how to reduce bruising and swelling without “supplements roulette”
Patients often ask how long swelling lasts and how to shorten the stages of facelift recovery. Food choices can make a measurable difference—especially sodium and protein.
- Prioritize protein: Healing is repair work. Protein supports tissue rebuilding.
- Keep sodium low: Salt is one of the fastest ways to prolong swelling.
- Hydrate consistently: Dehydration can worsen fatigue and slow recovery momentum.
- Avoid alcohol early: It can increase swelling and interfere with medication routines.
Expert-patient tip: Don’t start new supplements “because TikTok said so.” Many supplements can increase bruising risk or conflict with medications. Ask your surgeon first.
| Recovery Goal | High-Impact Habit | Common Mistake |
|---|---|---|
| Less swelling | Low sodium + steady hydration | “Healthy” salty soups / restaurant meals |
| Better energy | Protein at every meal | Skipping meals due to low appetite |
| Fewer setbacks | Medication schedule discipline | Self-adjusting doses without approval |
3) Movement: the right activity speeds recovery; the wrong activity extends it
Many patients want an exact answer to how long is facelift recovery, but recovery speed is strongly influenced by whether you trigger swelling spikes. Gentle movement helps circulation; intense activity raises blood pressure and can worsen swelling or bruising.
- Do: short, frequent, easy walks (as cleared by your surgeon).
- Don’t: workouts, heavy lifting, bending over repeatedly, hot yoga/sauna.
- Watch: facial flushing and throbbing—often a sign you’re overdoing it.
Deep plane recovery time perspective: recovery time for deep plane facelift is often similar on a calendar to other facelift types, but the “don’t force it” rule is even more important because deeper tissues are settling. If you push too soon, you may extend swelling and feel like your facelift recovery timeline is dragging.
4) Scar care & sun protection: the “quiet” path to the best-looking incisions
Scar outcomes depend on incision handling early and protection for months. Patients focused on “natural” results often forget that incision quality is part of what makes a facelift look refined.
- Incision minimalism: use only surgeon-approved products.
- Sun avoidance: UV can worsen redness and pigment in healing scars.
- Timing matters: scar strategies are phase-based; what helps at Week 6 may be wrong at Day 6.
From a dermatosurgeon perspective, skin quality is not an “extra”—it’s part of the final result. When facelift recovery is guided with both structural planning (plastic surgery technique) and skin-focused expertise (dermatosurgeon-level understanding of healing, inflammation, and collagen behavior), patients often experience more natural refinement because both the underlying structure and the skin’s healing response are respected.
Skin quality matters: A well-executed facelift can look less “operated” when recovery protects the skin barrier, controls inflammation, and avoids pigment triggers.
5) Your “photo expectations” (why day-by-day photos can mislead)
It’s normal to look at deep plane facelift recovery day by day photos and wonder why your bruising looks different. But bruising intensity is highly individual. Two patients can have identical surgeries and very different visible healing.
- Lighting changes everything: overhead vs. window light can exaggerate swelling.
- Angles distort symmetry: keep a standardized distance and head position.
- Swelling is not linear: “two steps forward, one step back” days are common.
If you want a calmer experience, use standardized photos as a tool for your surgeon—not as a scoreboard against strangers on the internet.
Where HBOT and LLLT fit at home: If your plan includes them, think of HBOT as early-phase support for oxygen availability during high swelling days, and LLLT as a controlled way to support calmer skin behavior and repair signaling. In AKM Clinic’s protocol, LLLT is delivered using medical-grade parameters (650nm, 424 diode array) designed to support cellular energy (ATP), collagen support, and inflammation reduction—always integrated with surgeon-led incision care, not competing with it.

Red Flags: When “Normal Swelling” Might Be a Problem
Most patients expect swelling, tightness, and bruising during facelift recovery. That’s normal. What creates real risk is missing the small number of warning signs that suggest a complication is developing—especially in the first days of deep plane facelift recovery or SMAS facelift recovery, when tissues are most reactive.
This section is written for the “expert patient” mindset: you’re not trying to diagnose yourself—you’re trying to know when to escalate quickly and appropriately. If something feels “off,” it’s always better to contact your surgeon early than to wait.
Safety principle: A smooth facelift recovery timeline is rarely about doing more. It’s about preventing avoidable delays by catching problems early.
Hematoma: the “time-sensitive” complication you should know
A hematoma is a collection of blood under the skin that can develop after surgery. It’s one of the reasons surgeons take early recovery so seriously—because timing matters. While bruising is expected, a hematoma tends to look and feel different.
- What can be normal: bruising that spreads and changes color, mild-to-moderate swelling that slowly improves
- What’s more concerning: rapidly increasing swelling on one side, significant pressure/tightness that escalates, severe pain that feels “different,” sudden firmness that wasn’t there before
What to do: contact your surgical team immediately. If you’re unable to reach them and symptoms are escalating, seek urgent in-person evaluation.
Infection or poor wound healing: signs you shouldn’t ignore
Incisions can look slightly pink as they heal. That’s common. But certain patterns suggest infection or delayed healing and deserve prompt medical review—especially if you’re trying to speed up facelift recovery without setbacks.
| Possible Warning Sign | Why It Matters | What to Do |
|---|---|---|
| Increasing redness that spreads (not just a thin pink line) | May indicate infection or inflammation beyond normal healing | Contact your surgeon with standardized photos |
| Fever or feeling systemically unwell | May suggest a body-wide response needing medical assessment | Call your team; seek urgent care if severe |
| Drainage that is foul-smelling, thick, or increasing | Could indicate infection or wound breakdown | Do not self-treat; contact surgeon promptly |
| Worsening pain after initial improvement | Pain should trend down, not ramp up unexpectedly | Report the change and timing to your team |
Do not “experiment” on incisions. Unapproved creams, alcohol-based solutions, and aggressive cleaning are common reasons small issues become bigger ones during facelift recovery.
Nerve-related symptoms or asymmetry: what can be normal vs. urgent
Temporary asymmetry is common in the early stages of facelift recovery. Swelling is rarely perfectly even, and sleeping position alone can create day-to-day changes. But there’s a line between “normal variability” and “needs evaluation.”
- Often normal early on: mild uneven swelling, tightness, numbness around incisions, one side improving faster than the other
- More concerning patterns: sudden new drooping, rapidly worsening asymmetry, inability to move part of the face that wasn’t present before, severe or escalating pain on one side
What to do: document it with standardized photos/video and contact your surgeon. Early, calm assessment is part of safe recovery—especially if you’re tracking day by day facelift recovery.
When “normal bruising” isn’t normal: blood pressure spikes and risky activity
One of the fastest ways to lengthen facelift recovery time is to trigger swelling spikes: heavy lifting, bending over, overheating, or returning to workouts too early. These don’t just slow healing—they can increase risk.
- Avoid: gym workouts, sauna/steam, hot yoga, heavy lifting, long hot showers (early on)
- Watch for: throbbing, flushing, pressure, or swelling increases after activity
- Do instead: frequent gentle walks and strict head elevation
If you traveled for surgery: your escalation plan matters
If you’re having surgery abroad, the most important “advanced recovery tool” is a clear escalation pathway. A reputable surgical team should give you:
- 24/7 contact guidance for urgent questions during the high-risk early window
- Clear photo instructions (what angles, what lighting) for remote assessment
- Structured follow-up so you don’t feel alone once you’re home
Expert-patient move: Before surgery, ask: “If I have sudden swelling at night, who do I contact, and what happens next?” The answer should be specific—not vague.
From VIP airport transfers to 5-star hotel accommodations, we handle every detail. Enjoy a seamless medical travel experience in Istanbul.
If You’re Traveling for Surgery: Minimizing Downtime in Istanbul (and After You Fly Home)
For international patients, the biggest variable in facelift recovery isn’t just technique—it’s logistics. A well-planned schedule can make your facelift recovery timeline feel calmer and more predictable, while a rushed itinerary can create avoidable stress (and sometimes avoidable swelling setbacks).
This section is especially relevant if you’re planning deep plane facelift recovery or SMAS facelift recovery in Istanbul and want to know what “smart travel recovery” actually looks like—without relying on random day by day facelift recovery posts online.
Travel recovery truth: The goal is not to fly home as fast as possible. The goal is to get through the highest-value monitoring window safely, then transition to structured remote follow-up.
Why the first 7–10 days are the “high-value” monitoring window
The early phase is when swelling peaks, bruising patterns evolve, and the small number of time-sensitive issues (like unexpected bleeding or wound concerns) are most likely to appear. This doesn’t mean complications are common—it means that if something needs a surgeon’s assessment, it’s far easier and faster when you’re still local and being monitored.
- Days 1–3: swelling control and incision protection are the priority
- Days 4–7: bruising shifts; asymmetry from swelling can look dramatic but is often temporary
- Days 8–10+: many patients feel “public-presentable,” but still need discipline
If your goal is to speed up facelift recovery (in the sense of comfort and confidence), this window is where structured support—like HBOT and/or LLLT when medically appropriate—can be layered in a supervised way rather than improvised at home.
Flying considerations: swelling, comfort, timing, and a safety checklist
Patients often ask: “Will flying make swelling worse?” Travel can contribute to puffiness for some people due to prolonged sitting, disrupted sleep, and dehydration. That doesn’t mean flying is “unsafe” by default—it means you should plan for it like an expert patient.
Comfort + swelling checklist (general guidance):
- Hydration strategy: consistent water intake; avoid alcohol before and during travel
- Movement: short walks during the journey when possible; gentle leg movement while seated
- Sleep positioning: protect your head/neck alignment; avoid pressure on healing areas
- Medication schedule: keep a simple written plan for time zone changes (never self-adjust doses)
- Sun protection: healing skin and scars are vulnerable—UV discipline matters even while traveling
- “No surprises” bag: surgeon-approved wound care items only (no new products)
Important: Exact timing of when it’s appropriate to fly depends on your procedure details and your surgeon’s clearance. If you’re optimizing facelift recovery time, the safest approach is planning enough time for early reviews before departure.
What a travel-optimized recovery schedule can look like (example framework)
Every surgeon has a different protocol, but here’s a practical structure many international patients use to reduce stress and protect the first two weeks of healing:
| Time in Istanbul | Main Goal | What You Typically Focus On |
|---|---|---|
| Days 0–3 | Stability | Rest, swelling control, incision protection, calm routine |
| Days 4–7 | Predictable progress | Gentle walking, structured check-ins, managing bruising shifts |
| Days 8–10+ | Transition readiness | Travel planning, “what’s normal now,” remote follow-up setup |
If your plan includes advanced recovery support, this is also where it fits logically:
- HBOT: often most relevant in the early swelling-heavy phase (Weeks 0–2, surgeon-directed)
- LLLT (laser therapy): typically integrated when incision status and skin condition make it appropriate, often to support calmer visible recovery
Remote follow-up done right: what it should include (so you don’t feel alone)
For patients returning home, remote follow-up is part of safe recovery—especially if you’re tracking stages of facelift recovery and want reassurance that what you’re seeing is normal.
A strong remote follow-up system usually includes:
- Standardized photo protocol: exact angles + lighting instructions (front/left/right/45°)
- Defined check-in schedule: not just “message us if needed,” but planned touchpoints
- Clear escalation rules: what symptoms require immediate contact (and what to do if you can’t reach the team)
- Scar-care timeline guidance: phase-based recommendations (not product dumping)
Expert patient question to ask before surgery: “If I develop sudden one-sided swelling at home, what’s the exact step-by-step plan for evaluation?” The answer should be specific.
How travel planning changes expectations for deep plane facelift recovery
If you’re researching recovery time for deep plane facelift, travel planning matters because deep plane work is structural and the early phase can feel tight and swollen even when everything is going perfectly. You can absolutely travel safely with the right planning—but rushing the early window can make recovery feel longer (mostly because it increases anxiety and reduces easy access to assessment).
In other words: smart travel planning doesn’t necessarily make biology faster, but it often makes the whole day by day facelift recovery experience smoother, safer, and less stressful—especially for patients who want predictable downtime.
Speed Up Facelift Recovery Frequently Asked Questions (FAQ):
How can I speed up facelift recovery safely?
The safest way to speed up facelift recovery is to prevent setbacks: follow incision care exactly, keep your head elevated, stay low-sodium, hydrate consistently, walk gently (no workouts), and avoid nicotine. If your surgeon offers it, structured recovery support such as HBOT and LLLT (laser therapy) may help optimize the healing environment—especially during the first two weeks.
How many HBOT sessions do facelift patients usually need?
There isn’t one universal number. Many surgeon-led protocols concentrate HBOT sessions in the first 1–2 weeks, then adjust based on swelling, bruising patterns, and how quickly you’re moving through the stages of facelift recovery. Your medical screening and surgical plan determine what’s appropriate.
When should HBOT start after a facelift?
Timing is surgeon-dependent. In recovery-focused programs, HBOT is often considered during the early “high-demand” phase (Days 1–7) when swelling peaks and tissues are most reactive. The purpose is oxygen support in a pressurized environment to help the body heal efficiently—without replacing standard aftercare.
Is HBOT safe after facial surgery—who should avoid it?
HBOT can be safe when medically screened and supervised, but it’s not for everyone. Patients with certain ear/sinus issues (pressure equalization problems), specific lung conditions, uncontrolled claustrophobia, or medication conflicts may not be candidates. A proper clinic will always do a medical clearance before scheduling sessions.
How does LLLT (laser therapy) help swelling and bruising?
LLLT (often called “cold laser”) is designed to support healing without heat or tissue damage. In clinical protocols, the goal is to support cellular energy (often discussed as ATP support), collagen signaling, and inflammation control—helping the skin look calmer while deeper tissues continue settling during facelift recovery.
When can I start laser therapy after a facelift?
Most surgeons introduce LLLT only when incision status and skin condition make it appropriate—often after the earliest incision-critical phase. Starting too soon (or using the wrong device) can irritate healing skin. Always follow your surgeon’s timing, especially in deep plane facelift recovery and SMAS facelift recovery.
Can HBOT and LLLT reduce scarring after a facelift?
They can support the biology of healing (oxygen delivery, inflammation control, collagen behavior), which may support better tissue quality. But scars still depend heavily on: incision technique, genetics, sun avoidance, and a phase-based scar care plan. Think “support,” not “guarantee.”
What’s the fastest realistic “social downtime” after a facelift?
Social downtime varies, but many patients look significantly more “public-presentable” around the 2–3 week mark, while subtle swelling can continue improving for months. Some recovery-focused protocols aim to help selected patients look more “camera-ready” around Day 14, but that depends on your bruising tendency, skin quality, and how disciplined your first 2 weeks are.
What should I avoid to prevent prolonged swelling after facelift?
Nicotine (including vaping)
High sodium meals (restaurant food is a common trigger)
Side sleeping and sleeping flat
Early workouts, heavy lifting, bending over repeatedly
Heat exposure (sauna/steam/hot yoga early on)
Unapproved skincare or “healing creams” on incisions
When should I contact my surgeon during recovery?
Contact your surgeon urgently if you have rapidly increasing one-sided swelling, severe or escalating pain that feels “different,” spreading redness, fever, foul or increasing drainage, sudden new facial weakness, or anything that feels like a major change in your baseline. Early assessment protects your outcome and your safety.
Patient perspective: “I actually look like nothing happened but probably 20 years younger.”
Related Treatments
Ready to Start Your Own Transformation Journey?
Join the 2,000+ patients who trusted Dr. Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, revitalized you begins with a simple, no-obligation conversation. Contact us today from the USA for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. No hidden fees.
#2: Secure Your Date & VIP Booking
Once you're ready, our dedicated patient coordinators will help you secure your procedure date. We'll handle all your bookings, including your 5-star hotel and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you'll meet your specialist surgeon to finalise the details for your "natural, subtle, and revitalized" new look.













