The “Aftercare” Experience: What Happens When You Fly Back Home?

- Post op care after flying home relies on a structured plan: routine check-ins, clear instructions, and continuity of care.
- First 72 hours back home focus on practical recovery: medications, swelling control, safe movement, and simple post op home care.
- Red flags require immediate action: rapid worsening swelling, severe pain, fever, heavy bleeding—know when to seek urgent care/ER.
- Remote follow-up plus local backup supports safety: photo updates, symptom tracking, and coordinated in-person contingency care.
Summary generated by AI, fact-checked by our medical experts
If you’re considering surgery abroad, the real question isn’t only “How will my surgery go?”—it’s “What happens after I land back home?” This is where post-op care after flying home becomes the deciding factor for many international patients. You want clear instructions, real access to your team, and a plan that covers normal healing, unexpected changes, and the practical realities of life back in the US.
This article is designed for the “expert patient” mindset: detail-oriented, risk-aware, and allergic to vague promises. We’ll walk through what responsible post-op care looks like once you leave Istanbul, how postoperative care after flying home should be structured, and how to protect your results with a realistic aftercare plan you can follow.
Key idea: In medical science, outcomes improve when patients have (1) a standardized care routine, (2) early recognition of warning signs, and (3) fast communication pathways. Your aftercare should be built around those three pillars—whether your procedure was a facelift or another form of plastic surgery.
Note: This content is educational and cannot replace medical advice. Your surgeon’s instructions always come first. If you experience urgent symptoms (difficulty breathing, chest pain, sudden severe swelling, uncontrolled bleeding), seek emergency care immediately.
Table of Contents
What “Post-Op Care After Flying Home” Actually Means (and What It Doesn’t)
When people say “aftercare,” they often imagine a single follow-up message or a quick check-in. In reality, strong plastic surgery post-op care is a structured system: clear instructions, scheduled check-ins, symptom triage, and contingency planning for local in-person evaluation if needed. This is especially true for postoperative care after international surgery, where distance can magnify anxiety if expectations aren’t defined.
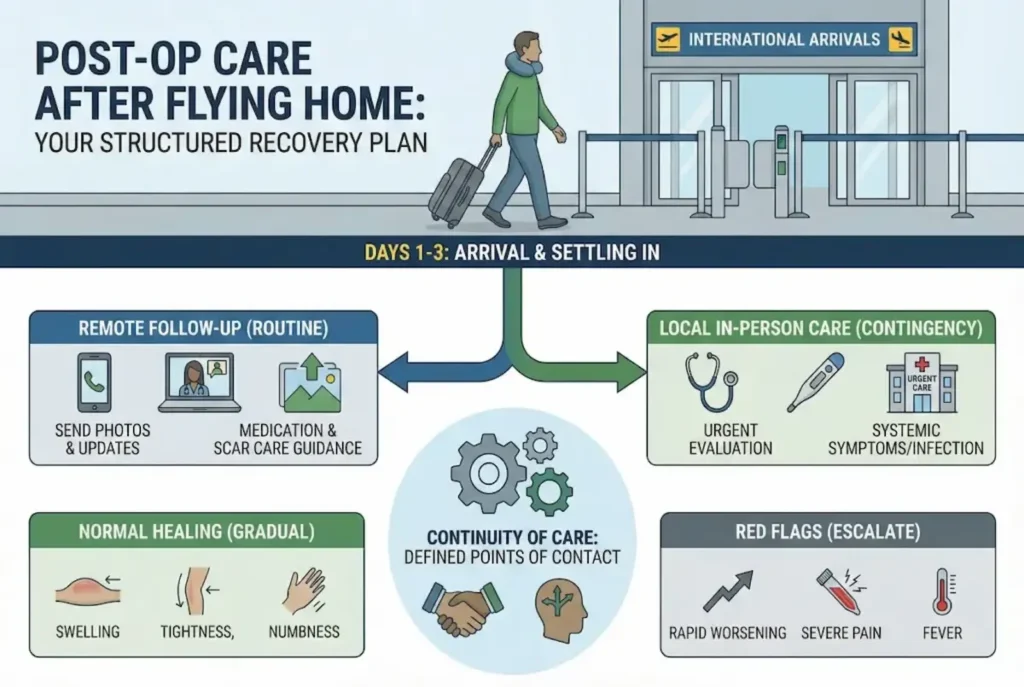
What your surgical team can manage remotely vs. what requires local in-person care
Remote follow-up is effective for many routine questions and visual checks—especially when you send consistent photos and short videos. Typical “remote-manageable” topics include:
- Normal swelling and bruising patterns (and whether they fit your timeline)
- Scar care adjustments (silicone use, dryness, mild irritation)
- Medication questions (timing, common side effects, what’s expected)
- Sleep positioning and activity pacing during healing
Some situations are best handled locally in person—because they require hands-on assessment, vital signs, or immediate intervention. Examples include suspected infection with systemic symptoms, significant bleeding, rapidly expanding swelling, or breathing concerns. The safest approach is a clear “decision pathway” so you know when to message your team and when to go straight to urgent care or the ER.
What’s “normal healing” vs. what’s a warning sign
Patients often underestimate how “weird” normal healing can feel: tightness, temporary numbness, uneven swelling, and day-to-day changes can be part of a normal recovery arc—particularly in facelift post-op care. That said, responsible post-op facelift care focuses on patterns:
- Normal tends to be gradual (slow improvement with ups and downs).
- Red flags tend to escalate (rapid worsening, severe pain, fever, foul drainage, or sudden asymmetry that keeps increasing).
The goal of a solid aftercare plan isn’t to make you worry—it’s to help you respond early and appropriately if something deviates from the expected course.
The #1 fear: “Will I be on my own after I leave?” (and how continuity of care works)
For international patients, the most common fear is “abandonment” after returning home. High-quality post-op care for international patients defines continuity up front:
- Who you contact (patient host/coordinator vs. clinical team)
- How you contact them (secure messaging, WhatsApp, email, scheduled video calls)
- What to send (photos, symptom notes, temperature, medication list)
- What happens next (home-care adjustment vs. urgent evaluation guidance)
The “will I be on my own after I leave?” fear is rational — it tracks directly to whether the clinic publishes who’s responsible at each stage of post-op communication. What protects against the abandonment scenario is documentation: named coordinators, named clinical escalation routes, written response time expectations, and a clear policy on what’s handled remotely versus what triggers an in-person referral. Vague reassurance is not a substitute for any of that.
The clinic-level accountability structure — named team, escalation pathway, written policy — is documented under the clinic accountability framework.
Continuity of care begins long before the flight home — the question is whether your trip is structured as a one-off transaction or as one stage of a coordinated international patient timeline. The well-structured version connects the pre-op consultation pathway, the in-Istanbul surgical days, the hotel-based early recovery, the fit-to-fly clearance, the travel-home logistics, and the post-arrival aftercare plan into one continuous arc with named handoffs at each stage. When any of those stages is treated as an isolated step, that’s where international patients tend to fall through the cracks.
The full stage-by-stage handoff structure, including remote follow-up cadence after return, is mapped in the international patient pathway.
This is also where surgeon-led care matters. For facelift patients, a team that blends plastic surgery expertise with a Dermatosurgeon’s perspective can be especially helpful in aftercare—because recovery isn’t only about deeper structures; it’s also about skin quality, inflammation control, and scar behavior over time.
“A team that blends plastic surgery expertise with a Dermatosurgeon’s perspective” — the phrase from the section above is not generic. Dermatosurgery is a defined subspecialty pathway: skin-focused surgical training layered on top of dermatology, useful in aftercare specifically because scar behavior, inflammation control, and skin-quality trajectory are managed differently when the lead surgeon has both lenses. What this actually changes in remote follow-up: the photo review focuses on early scar mottling, the silicone protocol is tuned to the specific incision type, and the skin-quality conversation runs alongside the structural-healing conversation rather than as an afterthought.
The dual-track training and credentialing record is documented under the dermatosurgery-trained surgeon profile.
Your First 72 Hours Back Home: A Practical Checklist
The first three days after you return are where routines either solidify—or fall apart. Travel fatigue, jet lag, and “I just want to be normal again” pressure can lead to skipped steps. A clear post-op home care checklist reduces mistakes and gives you a calm baseline. The details may differ depending on your procedure, but the structure is consistent across facelift post-op instructions and many other cosmetic surgeries.
| Time Window | Priority | What to Do (Example Checklist) | What to Avoid |
|---|---|---|---|
| 0–24 hours | Stability & setup | Set alarms for meds as prescribed Prep clean supplies for wound/scar care Elevate head/upper body for rest | Heavy lifting or bending Alcohol and smoking “Pushing through” fatigue |
| 24–48 hours | Consistency | Short, gentle walks (as tolerated) Hydration + protein-forward meals Photo update if instructed (same lighting/angles) | Skipping compression/garment rules (if prescribed) Random topical products on scars/incisions |
| 48–72 hours | Monitoring | Track swelling patterns and comfort level Note temperature if you feel “off” Confirm next check-in window | Returning to workouts early Over-checking the mirror (stress increases) |
Medications, garments, and wound-care routine you can actually follow
The best post-op care is the one you can follow consistently. Before you travel, make sure your post-op kit is organized for real life back home: labeled medications, a simple schedule, and a minimal set of approved wound-care products. For facelift recovery, facelift post-op care often includes specific instructions on cleaning, ointment use (if prescribed), and when to start silicone-based scar management.
Two practical rules:
- Don’t improvise products on incisions or scars (especially acids, retinoids, or “miracle creams”).
- Don’t change medication timing because you “feel fine.” Consistency prevents avoidable flare-ups.
Swelling control at home: sleep position, comfort measures, and pacing activity
Swelling is not a character flaw; it’s biology. In post-op facelift care, swelling can look uneven and can shift—especially after flights and changes in routine. Most patients do better when they treat recovery like a structured sprint:
- Sleep elevated (as instructed) to reduce fluid accumulation.
- Move gently (short walks) instead of long periods of bed rest.
- Pace social activity: “feeling normal” often arrives before tissues are truly ready.
Hydration + safe movement basics to reduce avoidable risks
Hydration and gentle mobility are foundational parts of postoperative care after flying home. You don’t need to “train through” recovery—but you do need circulation, regular fluids, and nutrition that supports tissue repair (adequate protein, micronutrients, and sleep).
If you had an operation involving the face/neck, your surgeon may also advise when it’s safe to resume specific movements or massage techniques—follow facelift post-op instructions precisely rather than copying general internet advice.
Remote Follow-Up: How Virtual Check-Ins Work (Step-by-Step)
The strongest predictor of peace of mind after medical travel isn’t luck—it’s structure. A well-designed remote follow-up system turns post-op care from “message us if you need us” into an organized workflow: scheduled check-ins, consistent photo documentation, and a clear escalation pathway. In scientific research on postoperative recovery, early recognition + timely guidance is a recurring theme—especially when patients are recovering at home rather than under direct daily clinical supervision.
The evidence base on telemedicine-led postoperative follow-up in plastic surgery is now structured around concrete operational findings — not aspirational claims.
A December 2024 J Plast Reconstr Surg study from a Japan Society of Plastic and Reconstructive Surgery group documented a hybrid model where face-to-face and telemedicine consultations alternated on a one-week cadence, with the lead plastic surgeon remotely guiding local clinicians on the patient’s side: plastic surgery telemedicine review. The study confirms the same operational pattern repeated across earlier systematic reviews — telemedicine consistently extends postoperative monitoring efficiency, reduces unnecessary in-person visits, and improves access to specialist guidance when patients are geographically distant from the operating team.
Worth flagging the boundary clearly: this is a pilot framework using a 5G infrastructure, not a randomized trial on cosmetic facelift recovery specifically. The takeaway that does transfer is structural — a defined cadence, named local-clinician handoff, and standardized photo/video documentation make remote aftercare workable; the absence of those elements is what makes it fragile.
If you’re evaluating postoperative care after international surgery, ask one simple question: “What is the plan once I’m back home?” A real aftercare plan should be predictable, written down, and easy to follow—particularly for facelift post-op care where swelling, tightness, and scar behavior evolve over weeks.
“What is the plan once I’m back home?” — the question above sits inside a larger question: how was the clinic chosen in the first place? Aftercare quality almost always traces back to clinic-selection quality. The factors that determine whether the post-flight plan is actually executable — named team, transparent escalation, surgeon-led care rather than coordinator-led care, written 12-month follow-up structure — are the same factors used to evaluate whether to book in the first place. Patients who run that evaluation early get a coherent aftercare experience; patients who skip it tend to discover the gaps after they’ve already flown home.
The 12-criterion methodology that connects clinic vetting to aftercare expectations is on the clinic vetting framework.
Follow-up timeline: what’s assessed at 1 month, 3 months, 6 months, and 1 year
Many reputable clinics set milestone check-ins (often including 1 month, 3 months, 6 months, and 12 months) because “feeling better” and “tissue healing” are not the same thing. A typical remote framework can look like this:
| Milestone | What you’ll typically review | Why it matters |
|---|---|---|
| ~1 Month | Incision/scar status Swelling pattern & symmetry Medication/skin-care tolerance | Early scar habits + swelling management can shape your long-term result. |
| ~3 Months | Scar maturation progress Residual swelling & tightness Return-to-activity plan | This is where “it’s improving but not perfect yet” becomes normal—and guided adjustments help. |
| ~6 Months | Shape settling & skin quality Any persistent numbness Refinement questions (if any) | Many facelift-related changes continue to evolve; decisions should not be rushed. |
| ~1 Year | Final scar appearance Long-term maintenance guidance Before/after consistency review | One-year follow-up is a “true outcome” checkpoint in many surgical protocols. |
This timeline is a foundation—not a substitute for urgent evaluation when symptoms are concerning. It works best when combined with clear facelift post-op instructions and a practical post-op home care routine.
How to take and send “useful” photos/videos (angles, lighting, consistency)
Remote care rises or falls on the quality of what your team can see. To make post-op facelift care guidance more accurate, standardize your documentation:
- Lighting: face a window or bright lamp; avoid yellow bathroom lighting.
- Background: plain wall; remove distracting shadows.
- Angles: front, left profile, right profile, 45° left, 45° right; add close-ups of incision lines if instructed.
- Consistency: take photos at the same time of day whenever possible.
- Short video (10–15 sec): slow head turn + natural facial expression if your surgeon requests it.
Include a brief symptom note with each update: pain level (0–10), temperature if you feel unwell, new drainage (yes/no), and what medications you took that day. This small habit makes your plastic surgery post-op care communication dramatically more efficient.
Response expectations: communication flow + escalation pathway
For international patients, clarity matters more than constant messaging. A safe system defines:
- Primary contact route: who you message first for routine questions.
- Clinical escalation: how your message reaches the nurse/surgeon when symptoms are time-sensitive.
- What’s urgent: a short list of “don’t wait” symptoms (see next section).
If you’re searching for post-op care for international patients (sometimes even typed as “post-op car efor international patients”), make sure the clinic can explain their escalation pathway in plain language. Vague answers are a red flag.
“Vague answers are a red flag” — the line in the previous section is a credentialing test in disguise. The same vagueness that hides escalation pathway gaps also hides credential gaps. A clinic that can’t describe what happens at 1 month, 3 months, 6 months, and 12 months in writing is often also a clinic that can’t produce verifiable registry entries, named anesthesia accountability, or hospital accreditation documentation when asked directly. The two failure modes correlate.
The pre-booking credential audit framework — registries, hospital licensing, named clinician verification — is on the surgeon credential verification.
Practical standard: A good aftercare system doesn’t promise “24/7 everything.” It provides a realistic channel for routine guidance and a clear, immediate plan for true emergencies.
When to Worry: Red Flags and What to Do Immediately
Most post-op concerns are benign, but the small percentage that aren’t can move fast. This section is designed to reduce panic and increase safety: you’ll learn the “watch and document” symptoms versus the “act now” symptoms. This is essential for postoperative care after flying home, where you may be hours away from your original surgical team.

The non-negotiable red flags (don’t wait)
If you experience any of the following, seek urgent in-person care immediately (urgent care or ER depending on severity), then notify your surgical team as soon as possible:
- Breathing difficulty, chest pain, fainting, or severe shortness of breath
- Rapidly expanding swelling, especially if one-sided and painful
- Uncontrolled bleeding or sudden large-volume drainage
- High fever with worsening pain, redness, or foul-smelling drainage
- Severe, escalating pain that feels out of proportion to your recovery timeline
For facelift recovery, rapidly increasing one-sided swelling can be especially concerning and should not be “waited out.” Always follow your surgeon’s specific facelift post-op instructions, because the urgency threshold can differ by technique and individual risk factors.
The decision tree: message your team vs. urgent care vs. ER
Use the simple pathway below as a general guide for post-op care after flying home:
| Situation | Best first step | What to send / bring |
|---|---|---|
| Mild, stable swelling; mild bruising; expected tightness | Message your team (routine channel) | Standard photos + symptom note + medication schedule |
| New redness, increasing warmth, mild drainage, low-grade fever | Message your team same day; consider local evaluation | Close-up incision photos + temperature + medication list |
| Rapidly increasing swelling, heavy bleeding, severe pain, breathing issues | ER now (do not wait for messaging) | Operation summary (if provided), surgeon contact info, current meds |
This is not meant to replace clinical judgment. It’s meant to prevent the two biggest mistakes in post-op home care: ignoring true danger signs or panicking over normal healing.
What to document so your team can guide you safely
When something changes, your surgical team can help most effectively if you send:
- Photos: consistent angles + close-up of the area
- Timing: when the symptom started and whether it’s worsening
- Temperature: if you feel feverish
- Medication log: what you took, when, and any side effects
- Functional changes: difficulty swallowing, dizziness, shortness of breath (urgent)
This kind of documentation is a core part of responsible post-op facelift care and plastic surgery post-op care—especially when you’re recovering at a distance.
Patient video accounts of the post-flight recovery week tend to surface details that text testimonials can’t — the day they hit the “what have I done?” moment, how they handled the swelling plateau around week 3, and what they actually messaged their team about when something felt off. The footage covers what the structured timeline can’t quite predict: the emotional texture of each week, the practical adjustments patients made on their own, and how the remote check-in cadence felt in real time.
Week-by-week recovery footage from US, UK, and Canadian patients sits in the patient story videos.
Coordinating With Your Local Doctor (Before You Even Travel)
One of the most overlooked parts of safe post-op care is planning for what happens if you need an in-person assessment once you’re home. This is not pessimism—it’s good medical planning. The smartest approach to postoperative care after international surgery is a “two-layer system”: your surgical team provides primary guidance remotely, while a local clinician can serve as a practical backup for hands-on checks if needed.
This coordination matters even more for procedures with nuanced healing, like facelift post-op care, where swelling patterns, scar behavior, and skin sensitivity can change week-to-week. A clear aftercare plan reduces uncertainty and helps you avoid rushed, stressful decisions if something feels off.
How to choose a local provider for “backup” care
You don’t need to “book a surgeon” at home in advance for most cases. But you do want a realistic option if you need an exam. Good candidates include:
- Your Primary Care Physician (PCP): helpful for basic evaluations, vitals, and referrals.
- Dermatologist: useful for scar-related questions, irritation, or skin-barrier issues after a facelift.
- ENT / urgent care clinician: sometimes helpful depending on symptoms and location of discomfort.
For post-op facelift care, the goal is not to “transfer your aftercare” to a local provider. It’s to ensure you can get an in-person exam quickly if your remote team advises it.
What to share: the minimum documents you should request
Before you leave Istanbul, ask for a simple post-op packet (digital is fine). This helps your local provider understand what was done and what “normal” looks like for your specific procedure. A practical packet for plastic surgery post-op care often includes:
- Procedure summary: what was performed (and on what date)
- Medication list: including antibiotics/pain relief and duration
- Wound/scar care instructions: what products are allowed and when
- Restrictions: lifting, exercise, travel, sun exposure
- Red-flag symptoms: what requires urgent evaluation
| Item | Why it helps at home | When you’ll likely need it |
|---|---|---|
| Medication schedule | Prevents missed doses and confusion after travel fatigue | First 7–14 days |
| Incision/scar protocol | Reduces irritation and “trial-and-error” product use | Weeks 1–12 |
| Red-flag list | Helps you act quickly and appropriately | Anytime something worsens fast |
| Surgeon/team contact pathway | Ensures fast escalation when needed | Routine questions + urgent concerns |
Cost/insurance reality: what patients should plan for and why
Even when your surgery is planned abroad, it’s wise to budget for the possibility of a local visit at home—especially for post-op care after flying home. Some clinics can advise you on what a local provider should check, but they can’t control local billing rules. Planning ahead reduces stress and prevents delays in getting evaluated when time matters.
Medical science mindset: A strong aftercare plan isn’t based on “hoping nothing happens.” It’s based on having a clear pathway if something happens—and using it early rather than late.
Common “Back Home” Problems and Simple Fixes
Most patients don’t run into major complications. What they do face are “high-annoyance, low-danger” issues: swelling that looks uneven, tightness that comes and goes, sleep challenges, and scar sensitivity. These are normal topics in post-op home care—and they can feel bigger when you’re recovering away from the clinic that performed your procedure.
The key is knowing what’s typical, what’s improvable with simple changes, and what should trigger a check-in. This section also supports people searching variations like postoperative care after flying home and post-op care for international patients (including the common typo “post-op car efor international patients”).

Pain, tightness, numbness: what’s typical and what isn’t
After a facelift, it’s common to experience:
- Tightness that fluctuates (often worse later in the day)
- Temporary numbness near incision lines or areas of skin elevation
- Mild asymmetry from uneven swelling that slowly normalizes
What is less typical (and worth same-day messaging or in-person assessment depending on severity) includes rapidly escalating pain, increasing one-sided swelling, or symptoms paired with fever or foul drainage. When in doubt, treat it as a post-op care question and follow your team’s escalation guidance.
Scar care basics: sun, silicone, irritation triggers, and timeline expectations
Scar management is a long game. In facelift post-op care, scars often mature for months, not weeks. Basic principles that often appear in facelift post-op instructions include:
- Sun protection: UV exposure can darken scars and slow cosmetic improvement.
- Approved silicone protocol: if your surgeon recommends silicone, follow timing and duration.
- Keep it simple: avoid rotating through new skincare actives (acids, retinoids) too early.
If you notice new redness, warmth, increasing tenderness, or drainage, don’t self-treat with random creams. That’s a classic way patients unintentionally complicate post-op facelift care. Use your planned communication pathway instead.
The emotional rollercoaster: why weeks 2–6 can feel worse before it looks better
Many patients hit a “what have I done?” moment after returning home—often when bruising fades but swelling persists, or when you’re tired of sleeping elevated. This is normal in plastic surgery post-op care. Healing isn’t linear, and short-term appearance doesn’t predict long-term outcome.
A practical tactic is to reduce mirror-checking and track progress with standardized photos once a week. It’s not about vanity—it’s about replacing anxiety with measurable trends.
Frequently Asked Questions (FAQ): Post-Op Care After Flying Home
This FAQ section is built for the questions that typically surface once you’re back home and the “real-life recovery” begins. If you’re navigating post-op care, post-op home care, or specifically postoperative care after flying home following a facelift, use these answers as a structured guide—then always default to your surgeon’s personalized instructions.
The same six or seven operational questions surface for almost every international patient back home — typically about garment timing, what counts as normal swelling, when to escalate, when to book a local check, and what each photo should look like. Having those answers in front of you in a single categorized place reduces the messaging-back-and-forth cycle and helps you act on routine concerns without waiting for time-zone overlap.
The structured answer set for international aftercare logistics lives on the aftercare question list.
Who do I contact if I have a problem after I’m home?
Your aftercare plan should define a primary contact channel (patient coordinator/host) and a clinical escalation route (nurse/surgeon). For routine questions (mild swelling, scar dryness, medication timing), message through the standard channel. For time-sensitive concerns (increasing redness, new drainage, feverish feeling), request escalation the same day. For true emergencies (breathing issues, uncontrolled bleeding, rapidly expanding swelling), go to the ER first—then notify your surgical team.
What if swelling looks uneven after I fly?
Uneven swelling can be common after travel, especially in facelift post-op care. The key is the pattern: mild asymmetry that changes slowly is often normal; swelling that increases rapidly on one side, becomes very painful, or continues to worsen is not something to “watch for a week.” Send standardized photos (front + both profiles + 45° angles) and a short symptom note. If it’s escalating quickly, seek local evaluation.
Can I see my primary care doctor for post-op checks?
Yes—your PCP can be a helpful part of postoperative care after international surgery, especially for basic assessments like vitals, general wound appearance, or referrals if a specialist is needed. Ideally, bring your procedure summary, medication list, and your clinic’s facelift post-op instructions so your doctor understands the context. Your surgical team remains the best source for procedure-specific decisions (scar protocol, activity progression, and what’s “expected” for your technique).
What should I do if I think I have an infection?
Don’t self-treat with random topical products or leftover antibiotics. Message your team the same day with close-up photos, your temperature, and a symptom timeline (when it started, whether it’s worsening). Signs that merit urgent in-person evaluation include fever, increasing redness/warmth, worsening pain, foul-smelling drainage, or feeling systemically unwell. Infection concerns are a core reason a clear plastic surgery post-op care escalation pathway matters.
Will I need to return to Turkey for a follow-up?
Most patients do not need to return for routine follow-ups, because structured virtual check-ins can cover standard healing milestones. However, whether a return is needed depends on your individual situation, the procedure performed, and the type of issue (if any). A responsible clinic will outline what can be managed remotely versus what requires in-person intervention—this is fundamental to post-op care for international patients.
What photos should I send to my surgeon—and how often?
Follow your clinic’s instructions, but a helpful standard for post-op facelift care often includes: front, left profile, right profile, 45° left, 45° right—plus close-ups of incision lines if requested. Keep lighting consistent and avoid filters. Frequency varies: some clinics request early updates soon after return, then milestone check-ins (e.g., around 1 month, 3 months, 6 months, and 12 months). Consistency makes remote guidance more accurate—an approach aligned with scientific research principles of standardized monitoring.
What’s the biggest mistake patients make after flying home?
The most common mistake is “normal life too soon”—returning to exercise, social events, alcohol, sun exposure, or complex skincare before tissues are ready. The second is changing products or routines impulsively (new creams, aggressive cleansers, strong actives) when irritation or swelling appears. Strong post-op home care is boring by design: simple, consistent, and aligned with your surgeon’s plan.
If you’d like to go beyond what we covered here, you can also explore our practical guides on Fly After Facelift, Solo Travel Surgery Istanbul, What to Pack For Surgery Abroad, and Flight Safety After Surgery. These resources expand on timing your return flight, traveling alone with confidence, packing the right essentials for post-op home care, and reducing avoidable travel-related risks—so you feel prepared at every step of your recovery journey.
Medical Disclaimer: This content is for educational purposes only and does not replace medical advice, diagnosis, or treatment. Surgical options, anesthesia choices, risks, costs, and recovery vary by individual. Always consult a qualified, board-certified clinician for personalized guidance. If you have urgent symptoms, seek emergency care.
Related Treatments
Ready to Start Your Own Transformation Journey?
Join the 2,000+ patients who trusted Dr. Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, revitalized you begins with a simple, no-obligation conversation. Contact us today from the USA for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. No hidden fees.
#2: Secure Your Date & VIP Booking
Once you're ready, our dedicated patient coordinators will help you secure your procedure date. We'll handle all your bookings, including your 5-star hotel and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you'll meet your specialist surgeon to finalise the details for your "natural, subtle, and revitalized" new look.











