Awake Breast Augmentation in Turkey




- Awake breast augmentation with twilight sedation offers calm comfort, local pain control, and individualized anesthesia selection.
- Natural-looking results come from anatomy-based planning: base width, tissue coverage, fold control, and precise pocket design.
- Clear recovery roadmap covers first 72 hours through weeks 6+, plus optional HBOT/LLLT accelerated recovery support.
- USA vs Istanbul value comparison emphasizes verified standards, all-inclusive care, and structured long-term follow-up.
Summary generated by AI, fact-checked by our medical experts.
Awake Breast Augmentation: Quick Facts
Procedure Time
Anesthesia
Recovery Time
Hospital Stay
Back to Work
Awake Breast Augmentation Results: Before and After
Awake breast augmentation is a modern approach to breast implant surgery designed for patients who want a more controlled anesthesia experience while still receiving a full surgical-quality result. The term “awake” can be misleading: most patients are not “wide awake” in the way you would be during a dentist visit. Instead, the procedure is typically built around a carefully planned comfort strategy that combines local numbing with a sedation plan tailored to the individual.
This guide explains what awake breast augmentation is, how it differs from “fully asleep” surgery, how surgeons plan a natural-looking result, and what you should evaluate when deciding whether an awake approach is right for you. The goal is not “bigger at any cost,” but a result that looks proportional, feels cohesive with your body, and stays aligned with your long-term comfort and lifestyle.
Surgeon’s Insight: The most successful aesthetic surgery doesn’t announce itself. The priority is refinement and balance—enhancement that still looks like you.
Table of Contents
Share your photos and medical history to receive a personalized assessment from our European board-certified facial surgery team.
What Is Awake Breast Augmentation?
Awake breast augmentation refers to breast implant surgery performed without traditional general anesthesia, using local anesthesia (numbing medicine) and a form of sedation that keeps you comfortable and calm. The experience is often described as “sleepy,” “relaxed,” and “unbothered,” rather than alert. The defining feature is that airway management and deep unconsciousness are typically not the central components of the anesthetic plan.
Defining “Awake”: Local Anesthesia + Sedation vs “Fully Asleep”
In a conventional breast augmentation under general anesthesia, you are rendered fully unconscious and typically require airway support while anesthetic gases or IV agents maintain deep anesthesia. In an awake approach, the primary pain control comes from local anesthesia delivered to the surgical area, while sedation is used to reduce anxiety, soften awareness, and improve overall comfort.
Depending on your plan and your medical profile, you may:
- Remain responsive to simple instructions (for example, taking a deep breath),
- Feel drowsy and have limited memory of the procedure,
- Perceive time as moving quickly,
- Experience little to no pain because the surgical field is thoroughly numbed.
“Awake” is best understood as a spectrum. Some patients prefer minimal sedation and want to feel more aware. Others want deeper sedation while still avoiding general anesthesia. A high-quality surgical team will discuss that spectrum with you, rather than forcing a one-size-fits-all approach.
Why Patients Consider an Awake Approach
Patients exploring “awake” options tend to share a similar mindset: they want maximum safety transparency and a predictable recovery experience. Common reasons include:
- Anesthesia anxiety: fear of being fully unconscious or concerns about nausea, grogginess, or a “lost day” feeling.
- Recovery preferences: interest in smoother immediate recovery and clearer mental state after surgery.
- Medical considerations: in select cases, an awake approach may be evaluated as part of a broader risk-management strategy (always individualized).
Importantly, an awake approach is not “less real surgery.” The procedure still requires advanced surgical planning, meticulous technique, and a sterile operating environment. The difference is the anesthesia pathway—not the standard of surgical outcome.
What Awake Breast Augmentation Is Not
Because online information can be confusing, it helps to clarify what this procedure is not:
- Not a shortcut: awake surgery is not a “quick fix” or a lower-grade version of augmentation.
- Not automatically safer for everyone: the best anesthesia choice depends on your health profile, anatomy, and procedure complexity.
- Not pain without planning: success requires disciplined local anesthesia technique and a sedation plan built around your tolerance and comfort goals.
Our surgery dates fill up quickly due to high international demand. Secure your consultation today to plan your ideal travel dates.
Breast Anatomy & Aesthetic Planning: How Results Are Designed
Natural-looking breast augmentation starts long before surgery day. The most important decisions are made during planning: how the breast footprint is shaped, how projection is created, and how the implant interacts with your existing tissue and skin envelope. A high-authority plan focuses on anatomy, proportion, and long-term harmony—not just cup size.
Key Anatomy That Determines Your Outcome
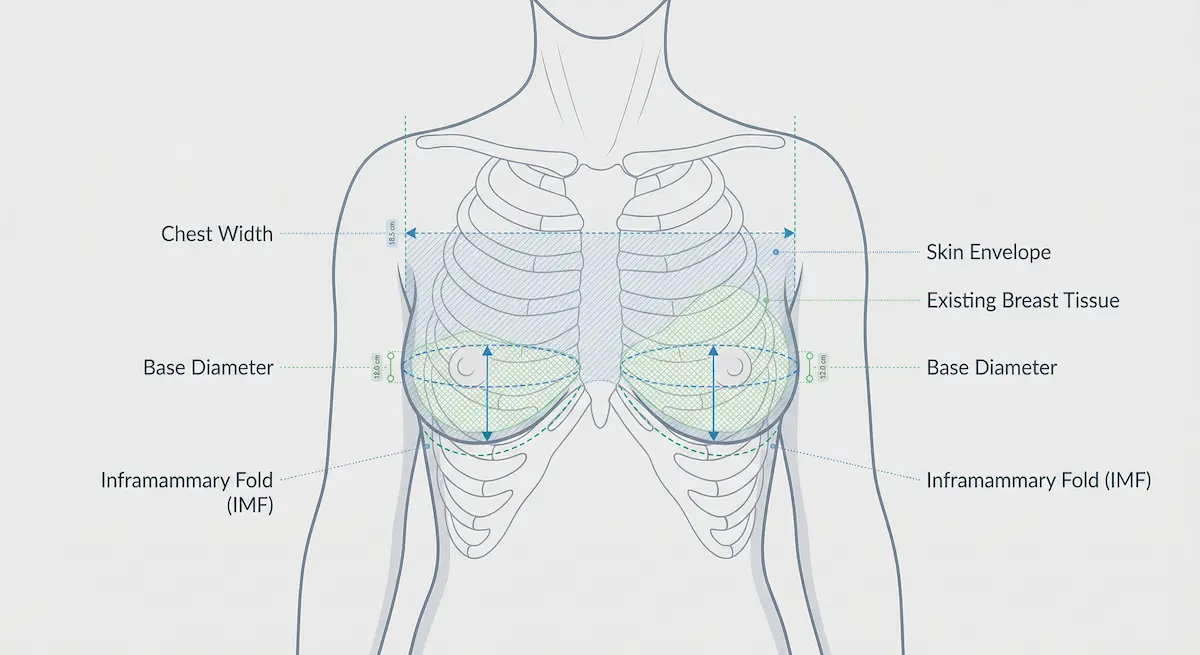
Even small anatomical differences can dramatically change what looks “natural” on different bodies. Surgical planning typically centers around:
- Skin envelope: how much natural stretch your skin has and whether it can accommodate the desired volume smoothly.
- Breast tissue (gland): how much native tissue you have to cover and support an implant.
- Chest width and base diameter: a core driver of implant selection—choosing an implant too wide can look unnatural or feel uncomfortable.
- Inframammary fold (IMF): the natural crease under the breast; this is a key landmark for symmetry and stable breast shape.
- Pectoral muscle relationship: impacts pocket selection (over/under muscle strategies) and movement dynamics.
When planning is anatomy-first, the goal becomes clear: select an implant and technique that respects your natural footprint, enhances projection in the right places, and avoids long-term distortion.
Proportion & Balance: What “Natural” Actually Means
“Natural” is not one look—it’s a relationship between your breast shape and your overall frame. In aesthetic planning, surgeons often evaluate:
- Upper pole fullness: how much volume sits in the top portion of the breast (subtle vs more pronounced).
- Projection: how far the breast comes forward from the chest wall, which changes your profile view and clothing fit.
- Cleavage behavior: how close the breasts sit depends on anatomy; forcing cleavage with oversized implants can look unnatural and feel tight.
- Symmetry goals: perfect symmetry is rare naturally; the plan aims for balanced, harmonious asymmetries.
For many “expert patients,” the best outcome is the one that looks refined in daily life: in a fitted t-shirt, in professional clothing, and in natural posture—without an obvious “operated” signature.
Consultation Inputs: Measurements, Goals, and Predictability
The most credible consultations rely on measurable data. A thorough planning session typically includes:
- Chest and breast measurements (base width, tissue thickness, nipple position, fold position),
- Skin quality and stretch evaluation,
- Discussion of lifestyle (training, posture, sleep preferences, long-term maintenance expectations),
- Goal alignment: “how you want to look” and “how you want to feel.”
When advanced planning tools are available, they can support clearer communication and help align expectations before surgery. The objective is predictability: choosing a plan you can say “yes” to with confidence because you understand the tradeoffs as well as the benefits.
Contextual next step: If you’re researching awake breast augmentation, your best first move is a structured consultation that evaluates candidacy, anatomy, and anesthesia suitability—before you ever discuss a specific implant size.
Ideal Candidates (And Who Should Avoid Awake Options)
Awake breast augmentation can be an excellent fit for the right patient—but it is not “automatically best” for everyone. The most reliable way to decide is to evaluate three factors together: your anatomy, your goals, and your anesthesia tolerance profile. A responsible plan prioritizes safety and predictability over ideology (for example, insisting on “awake only” even when it’s not appropriate).
Who Is Typically a Good Candidate?
Patients who do well with an awake or twilight-sedation approach often share several characteristics:
- Clear, realistic goals: you can describe what you want (shape, proportion, clothing fit) and accept that there are anatomical limits.
- Stable health profile: no uncontrolled medical conditions that increase surgical or anesthesia risk.
- Comfort with a “sleepy but not fully asleep” experience: you prefer calm sedation and local numbing rather than deep general anesthesia.
- Procedure scope matches the anesthesia plan: straightforward augmentation tends to be more compatible than complex multi-procedure plans.
Just as important is psychological fit. Many “expert patients” prefer awake options because they want a sense of control and reduced anxiety around deep anesthesia. That preference is valid—but it should still be filtered through clinical judgment and individualized risk assessment.
Medical Screening & Safety Criteria
High-standard clinics treat anesthesia selection as a medical decision, not a marketing choice. A proper preoperative evaluation generally reviews:
- Medical history: prior anesthesia experiences, medication sensitivities, nausea/vomiting tendency, sleep quality, and airway concerns.
- Current medications and supplements: including blood thinners and agents that increase bleeding risk.
- Baseline health parameters: blood pressure stability, respiratory health, and any conditions that affect healing.
- Procedure-specific risk factors: smoking/vaping, recent infections, or poor wound-healing history.
In a well-run surgical pathway, these screenings are not “box-checking.” They guide how your anesthesia plan is built, how your intraoperative monitoring is structured, and how your postoperative recovery is supported.
Who Should Avoid Awake/Twilight Sedation (Or Consider General Anesthesia)?
Sometimes, general anesthesia is the better choice—even for patients who dislike the idea. Examples may include:
- High anxiety with low tolerance for intraoperative awareness: if the possibility of hearing sounds or sensing pressure would cause panic, deeper anesthesia may be safer overall.
- Complex surgery scope: when the planned procedure is longer or technically more demanding, a different anesthesia strategy may be recommended for stability and comfort.
- Medical factors requiring deeper airway control: this is individualized and assessed by the anesthesia team.
The most “advanced” option is the one that matches your body, your goals, and your risk profile. A credible provider will explain that tradeoff clearly and document the reasoning.
Answer a few quick questions about your concerns, health, and goals to learn which treatment options may suit you best.
Implant Choices & Types of Awake Breast Augmentation
Breast augmentation is not a single product decision—it’s a system decision. The implant (or alternative method) interacts with your tissue coverage, skin envelope, chest width, and chosen surgical plane. The best plans start with what your anatomy can support, then select the method that produces the most stable long-term shape with the most natural feel for your body.
Implant Strategy: Choosing Volume Without Guesswork
One of the most common planning errors is selecting volume primarily by “desired cup size.” Cup size varies by brand, bra style, and body frame, making it an unreliable surgical target. Instead, surgeons typically prioritize:
- Base width compatibility: an implant that matches your chest and breast footprint helps avoid an unnatural “side spill” look.
- Tissue coverage: thinner tissue may require a strategy that better conceals implant edges and reduces visible rippling risk.
- Projection goals: how far you want the breast to project forward, balanced with your lifestyle and comfort preferences.
- Skin stretch tolerance: choosing a size that your skin can accommodate smoothly reduces long-term distortion risk.
For an “expert patient,” the smartest selection is usually the one that looks intentional in real life: standing naturally, moving naturally, and fitting naturally in your clothing—without looking “operated” in your day-to-day posture.
Shape, Profile, and the “Natural Look”
“Natural” can mean different things. Some patients want subtle enhancement with gentle upper pole fullness; others want a more noticeable roundness. The surgical plan typically considers:
- Upper pole fullness: subtle vs pronounced.
- Side profile contour: how the breast transitions from chest to projection.
- Cleavage behavior: largely anatomy-dependent; forcing it through oversizing can create tightness or unnatural spacing.
- Movement dynamics: how the breast looks and feels when you walk, reach, or exercise.
When your goal is a refined, “no obvious surgery signature” result, the plan usually emphasizes proportionality, controlled projection, and stable positioning—rather than maximum volume.
Alternative Option: Fat Transfer Breast Augmentation
Fat transfer breast augmentation uses your own purified fat to add volume and shape. It can be appealing to patients who want a smaller enhancement and prefer avoiding implants. However, it is not interchangeable with implant augmentation.
Key considerations include:
- Volume limits: fat transfer typically delivers more modest size increases compared with implants.
- Variability: not all transferred fat survives long-term; some resorption is expected.
- Donor-site requirement: you need adequate harvestable fat.
- Staging: some patients require more than one session to reach their desired outcome.
For many patients, fat transfer is best viewed as a tool for subtle refinement, contour smoothing, or incremental enhancement—not a direct substitute for implant-based augmentation when a larger or more predictable size increase is desired.
Awake Breast Augmentation Surgical Technique Options
Technique is where natural outcomes are won or lost. Even the “right” implant can look unnatural if the pocket is poorly designed, the fold is not respected, or symmetry is not managed with precision. In this section, you’ll learn the key technique choices surgeons make—especially incision placement and implant pocket selection—and how those choices affect scar appearance, feel, and long-term stability.
Incision Options: Why the Inframammary Fold Is Often Preferred
Incision choice is guided by access, precision, and scar concealment. While several incision sites exist, many surgeons favor an inframammary fold (under-breast crease) approach for the control it provides during pocket creation and implant placement.
When evaluating incision options, consider:
- Control and precision: the ability to create a symmetrical pocket and manage hemostasis (bleeding control).
- Scar position: how well the incision can be hidden in natural anatomy and typical clothing.
- Long-term aesthetics: how scars tend to mature and how visible they may be in different postures.
A credible consultation should include a scar strategy: where the incision will sit, how it will be closed, and how scar care will be handled during recovery.
Pocket Placement: Over the Muscle vs Under the Muscle vs Dual-Plane
Pocket placement describes where the implant sits relative to your breast tissue and pectoral muscle. This choice affects edge visibility, movement, athletic comfort, and how “natural” the implant looks and feels.
- Over the muscle (subglandular): may be considered when there is sufficient tissue coverage and when muscle movement concerns are high, but it requires careful candidacy selection.
- Under the muscle (submuscular): can improve upper pole coverage in thinner patients and may reduce visible implant edges, but may introduce movement dynamics in very athletic patients.
- Dual-plane strategies: a tailored approach that can balance coverage and shape in select anatomies.
There is no universally “best” placement—only the best match for your anatomy, tissue thickness, goals, and lifestyle.
Natural Result Drivers: Symmetry, Fold Respect, and Soft Tissue Management
Natural-looking augmentation is less about chasing perfection and more about mastering controllable variables. High-level technique typically focuses on:
- Fold management: respecting the inframammary fold and adjusting it conservatively when needed for stable breast shape.
- Symmetry engineering: recognizing natural asymmetries and planning pocket dimensions accordingly.
- Soft tissue handling: gentle technique to reduce trauma, swelling, and prolonged tightness.
- Position stability: ensuring the implant sits in a pocket designed to keep the breast centered and balanced over time.
For patients seeking a refined, “rejuvenation-not-alteration” aesthetic, the technique goal is harmony: a shape that looks coherent with your frame and remains aesthetically stable as your tissues settle during recovery.
Get a clear, day-by-day itinerary covering arrival, surgery, recovery, and fit-to-fly clearance tailored to your schedule.
Anesthesia Options: Twilight Sedation vs General Anesthesia
For many expert patients, the anesthesia plan is the single biggest decision-driver—sometimes even more than implant selection. The choice is not about “bravery” or “toughness.” It’s about matching the anesthesia method to your medical profile, anxiety tolerance, and the complexity of the surgical plan. A responsible team will present the pros and cons transparently and explain why a specific approach is recommended for you.
What Is Twilight Sedation, and What Does It Feel Like?
“Twilight sedation” is a patient-friendly term for a sedation approach that aims to keep you calm, comfortable, and drowsy while local anesthesia provides targeted pain control at the surgical site. Most patients describe the experience as:
- deeply relaxed and sleepy,
- unbothered by time passing,
- aware of very little (and often not remembering much afterward),
- feeling pressure or movement rather than sharp pain (because the area is numbed).
What you feel depends on your sedation depth and your personal sensitivity. Some patients prefer lighter sedation; others prefer deeper sedation while still avoiding the full “fully asleep” pathway.
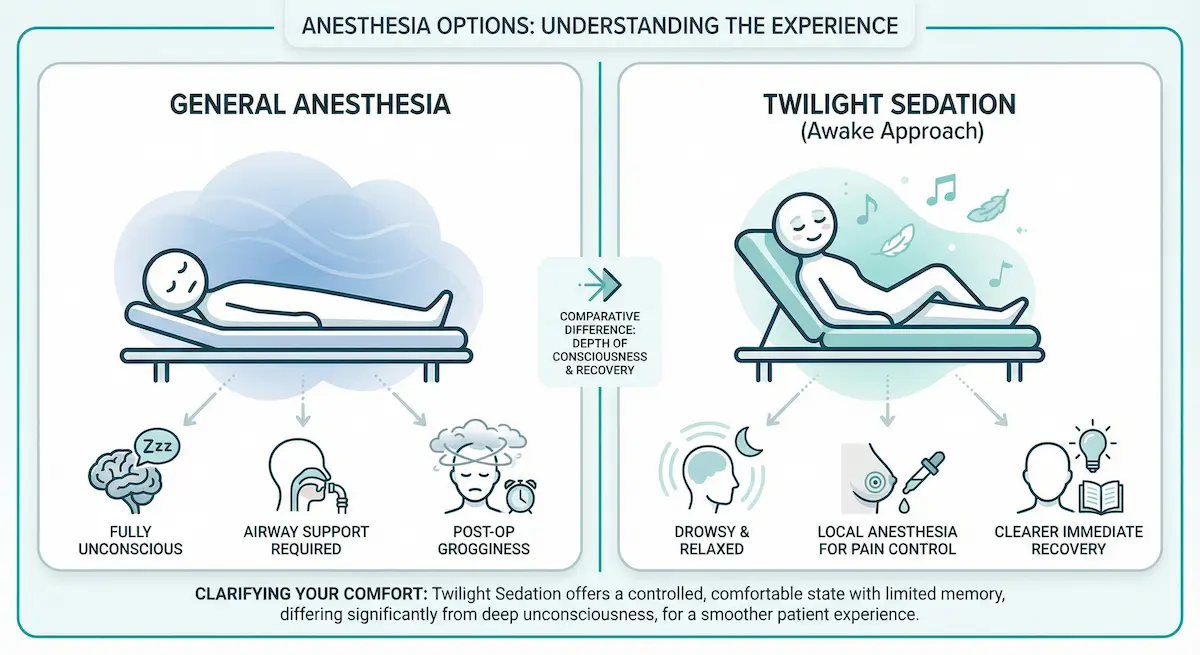
Twilight Sedation vs General Anesthesia: Key Differences
The simplest way to compare is to look at what each approach prioritizes. General anesthesia prioritizes deep unconsciousness and airway control. Twilight sedation prioritizes comfort and calmness while local anesthesia manages pain at the surgical site. Both can be safe when properly selected and monitored.
| Factor | Local + Twilight Sedation (“Awake”) | General Anesthesia |
|---|---|---|
| Level of consciousness | Drowsy/relaxed; may respond to simple cues; often little memory | Fully unconscious |
| Pain control | Local numbing is central; sedation supports comfort | Deep anesthesia; pain control managed within full anesthesia plan |
| Recovery experience | Often perceived as “clearer” sooner; varies by person | May feel more groggy initially; nausea risk varies by patient |
| Best fit for | Patients who want to avoid deep anesthesia and fit candidacy criteria | Patients needing deeper control, longer/complex plans, or better anxiety coverage |
| Not ideal for | Patients prone to panic with awareness or needing deeper airway control | Not “wrong,” but may be more than some patients want for straightforward cases |
A key principle: the “best” option is individualized. If you’re a high-anxiety patient who would panic with any awareness, general anesthesia may be safer overall. If your goals and anatomy are well-matched to a controlled, straightforward plan, an awake pathway may be a strong consideration.
Pain Control Strategy Under Awake/Twilight
Patients often worry, “Will I feel everything?” In high-quality awake breast augmentation, pain control is engineered in layers. Your comfort typically depends on:
- Thorough local anesthesia technique: careful numbing of the surgical field.
- Strategic sedation depth: enough to blunt anxiety and reduce awareness of pressure or movement.
- Communication during surgery: a calm environment, gentle handling, and responsive adjustments.
It’s normal to feel sensations like pressure, tugging, or shifting—these are not the same as pain. If you’re a patient who finds any sensation distressing, that should be discussed early, because comfort tolerance is part of candidacy.
Safety and Patient Selection: The Non-Negotiables
Awake breast augmentation should only be offered within a disciplined safety framework. This includes preoperative screening, appropriate monitoring, and a team experienced in tailoring sedation depth to the individual. The most important safety practice is not a single medication or machine—it’s the decision-making process that selects the right anesthesia for the right patient.
From VIP airport transfers to 5-star hotel accommodations, we handle every detail. Enjoy a seamless medical travel experience in Istanbul.
Awake Breast Augmentation Step-by-Step: How Awake Breast Augmentation Is Performed
While each surgeon has their own workflow, the high-level sequence of breast augmentation is consistent across modern surgical standards. Understanding the steps helps you ask better questions, evaluate provider quality, and set realistic expectations for recovery. Awake surgery does not change the fundamentals of the operation—it changes how comfort is managed during those steps.
Pre-Op Planning: Markings, Measurements, and Final Sizing
On surgery day, the plan becomes precise. Typical preoperative steps include:
- Pre-op markings: guiding fold position, midline, and symmetry references.
- Final confirmation of goals: ensuring your desired shape aligns with what your anatomy can support.
- Safety checklist: reviewing medications, allergies, and any last-minute health updates.
This is also the moment to confirm scar placement strategy and the pocket approach, so you understand exactly what is being done and why.
Intra-Op Sequence: Pocket Creation, Placement, and Symmetry Control
Once you are comfortable and the surgical field is numbed, the operation typically follows a controlled sequence:
- Incision and access: using the planned incision site to reach the pocket.
- Pocket creation: shaping the space where the implant will sit (the “engineering” of the result).
- Hemostasis: careful bleeding control to reduce swelling and support smoother recovery.
- Implant placement: positioning to center the breast footprint and create balanced projection.
- Symmetry checks: repeated evaluation to refine pocket dimensions and overall balance.
For patients pursuing a natural-looking result, symmetry control and pocket design are often more important than the brand or the exact “cc” number. This is where experienced technique is most visible in the final outcome.
Closing, Dressings, and Immediate Recovery
After implant placement is finalized, the surgeon closes the incision in layers and applies dressings that support early healing. In immediate recovery, the goals are comfort, stability, and clarity about what to do next.
Before you leave the surgical environment, you should receive clear instructions on:
- how to sleep and position your upper body,
- how to use prescribed medications safely,
- what is normal (tightness, swelling, pressure) vs what is not,
- how and when to contact your team for concerns.
Combined Procedures: When Augmentation Is Paired With a Lift
Some patients aren’t only seeking more volume—they also need the breast envelope reshaped for a more lifted, stable contour. In those cases, surgeons may recommend combining augmentation with a breast lift (mastopexy), commonly referred to as a breast lift with implants. This combined plan can be highly effective, but it requires careful technique and conservative decision-making because the goals can pull in opposite directions: a lift tightens and re-drapes skin, while an implant adds volume and weight.
A credible consultation will explain whether a single-stage breast lift with implants is safe and predictable for your tissue quality, skin elasticity, and nipple position—or whether staging the procedures would reduce risk and improve long-term stability.
Combination planning becomes even more important when breast augmentation is part of a broader body contouring strategy, such as a mommy makeover, where breast surgery may be paired with abdominal tightening and contour correction. If an abdominoplasty (a tummy tuck) is also planned, your surgeon should discuss how combining procedures affects operative time, recovery logistics, activity restrictions, and the safest timeline for returning to full movement and exercise.
Awake Breast Augmentation Recovery Timeline & Aftercare (Day-by-Day)
Recovery after breast augmentation is not just “waiting for swelling to go down.” It’s an active process of protecting the surgical pocket, controlling inflammation, supporting tissue healing, and guiding the implants as they settle. Most patients feel a predictable sequence: early tightness and pressure, a gradual return of mobility, and then a longer “settling phase” where shape softens and scars mature. Your job is to follow the biomechanics of healing—because the earliest weeks influence long-term positioning and comfort.
The First 72 Hours: Tightness, Swelling, and Sleep Strategy
The first few days are usually the most intense—mostly because tissues are adapting to a new volume and because the chest wall can feel tight or “worked.” It’s common to experience:
- Pressure and upper chest tightness (often more noticeable when rising from bed or changing posture),
- Swelling and a “high, firm” appearance early on,
- Soreness when using arms for leverage (especially if implants are placed under or partially under muscle),
- Fatigue from surgery, medication, and disrupted sleep.
Early aftercare is about stability and comfort:
- Sleep on your back with your upper body slightly elevated (this can reduce swelling and protect positioning).
- Use your legs and core to get out of bed—avoid pushing up aggressively with your arms.
- Follow medication instructions exactly and avoid unapproved supplements that increase bleeding risk.
- Hydrate and eat protein-forward meals to support tissue repair.
Many patients ask, “Will I be able to shower?” This depends on your surgeon’s dressing plan, incision management, and early wound instructions. Always follow the specific protocol you’re given rather than generic internet timelines.
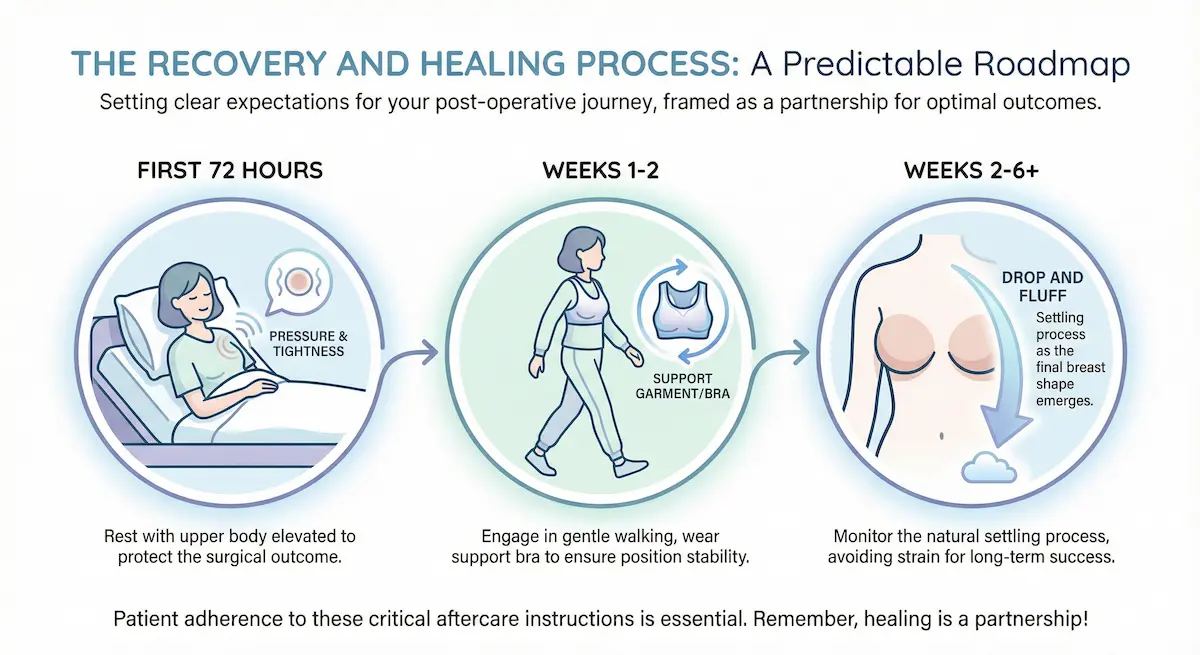
Week 1: Mobility Returns, but the Pocket Is Still Vulnerable
By the end of the first week, many patients feel noticeably better—especially in daily mobility—but this is also when overconfidence can cause setbacks. Your discomfort may decrease faster than your internal healing. In Week 1, the priorities are:
- Protect the pocket: avoid lifting, heavy carrying, overhead reaching, or sudden upper-body strain.
- Incision care: keep the area clean and dry as instructed and watch for abnormal redness, heat, drainage, or worsening pain.
- Support garments: wear the recommended bra/compression exactly as directed.
- Walking: gentle walking is usually encouraged for circulation and wellbeing.
If you chose an awake/twilight-sedation pathway, you may find that your immediate post-op mental clarity feels smoother than you expected. That said, your tissue healing timeline remains the same—so a “better-than-expected Day 2” does not mean “normal activity Day 2.”
Weeks 2–6: Settling Phase, “Drop and Fluff,” and Return to Activity
Most patients enter a transition phase after Week 2. Swelling continues to improve, the chest feels less tight, and the implants gradually settle into a more natural position. This is often called a “drop and fluff” period—where the breast shape becomes softer and more natural over time.
During this period, your surgeon may guide you on:
- Activity progression: when to reintroduce light workouts, then more intense training.
- Upper body movement: how and when overhead motion is safe.
- Scar strategy: the timing of scar treatments and how to minimize discoloration and thickening.
- Shape expectations: what “normal settling” looks like versus what needs evaluation.
It’s also common for sensation to fluctuate—nipple sensitivity may feel increased, decreased, or “tingly.” These changes often improve gradually, but timelines vary.
Long-Term Healing: Scar Maturation, Softening, and Follow-Up
Breast augmentation healing doesn’t “finish” at Week 6. Many patients see ongoing refinement for months as scars mature and tissues soften. The long-term focus areas include:
- Scar maturation: scars often change color and texture over time; good protocols emphasize consistency and patience.
- Soft tissue adaptation: breasts can continue to soften and feel more natural as the body adjusts.
- Position stability: implant position and shape typically become more predictable as swelling resolves and the pocket stabilizes.
A strong provider will also define a follow-up cadence—because long-term quality care is not just about the operation, but about the monitoring and guidance that follows it.
Accelerated Recovery & Safety Protocol: HBOT + LLLT (Where Technology Fits)
Some clinics integrate structured recovery technologies as part of a broader “rapid recovery and safety” philosophy. At AKM Clinic, two technologies are positioned as an integrated protocol rather than a cosmetic add-on: Hyperbaric Oxygen Therapy (HBOT) and Low-Level Laser Therapy (LLLT).
In a recovery pathway, these technologies are used with the intention of supporting tissue healing and comfort:
- HBOT (Hyperbaric Oxygen Therapy): delivered in a controlled chamber environment, positioned to support oxygenation-focused recovery goals within a structured protocol.
- LLLT (Low-Level Laser Therapy): positioned as a non-invasive therapy intended to support healing and comfort as part of a broader aftercare plan.
Transparency note: Patient testimonials don’t always mention every recovery technology by name, even when it is part of a clinic’s protocol. The correct way to evaluate these tools is to ask how they’re used (timing, number of sessions, selection criteria) and how they fit into standard medical aftercare—not to rely solely on whether a review lists the device name.
Contextual next step: If you’re comparing awake breast augmentation providers, ask for a written recovery roadmap (day-by-day for the first week, then week-by-week through week 6) and which interventions are standard protocol versus optional add-ons.
We use advanced Hyperbaric Oxygen Therapy (HBOT) to minimize downtime and supercharge your healing process. Safety is our #1 promise.
Awake Breast Augmentation Risks, Complications & How They’re Managed
No ethical guide on breast augmentation should minimize risk. A high-quality result comes from two equally important pillars: surgical technique and a safety system that detects, prevents, and responds to complications early. In awake breast augmentation, the anesthesia pathway changes—but the need for rigorous screening, sterile technique, and postoperative vigilance does not.
Short-Term Surgical Risks (Early Post-Op)
Most early risks are uncommon when surgery is performed in a properly controlled environment, but they are still real and should be understood before you consent. Key early risks include:
- Bleeding / hematoma: a collection of blood that can cause swelling, pain, and asymmetry; may require prompt evaluation and sometimes return to the operating room.
- Infection: may present as increasing redness, warmth, fever, worsening pain, or drainage; treatment can range from antibiotics to implant removal in severe cases.
- Seroma (fluid collection): may require monitoring or drainage depending on size and symptoms.
- Wound healing problems: delayed healing or incision separation, often linked to smoking/vaping, poor nutrition, tension on the incision, or early over-activity.
Most early issues are most safely addressed when they are caught quickly. That is why clear aftercare instructions and accessible postoperative support are not “nice extras”—they are part of risk management.
Medium- to Long-Term Risks (Months to Years)
Breast implants are medical devices, and long-term considerations should be part of your decision-making process. Common longer-term topics include:
- Capsular contracture: tightening of the scar capsule around the implant that can change shape or cause firmness/discomfort.
- Asymmetry: subtle asymmetry is normal in humans; significant asymmetry may require evaluation of implant position, pocket shape, or tissue changes.
- Implant malposition: shifting of implant position (too high, too low, too lateral), often related to pocket design, tissue quality, or early activity.
- Rippling/edge visibility: more common in thinner tissues; strongly influenced by pocket selection and tissue coverage strategy.
- Sensation changes: nipple or breast sensation can increase, decrease, or fluctuate; improvement is common but not guaranteed.
- Revision surgery risk: some patients may need a revision over a lifetime due to anatomy, goals changing, implant aging, or pregnancy/weight changes.
The best preventive strategy is an anatomy-respecting plan: an implant size and pocket choice that your tissues can support without chronic tension.
Anesthesia-Related Risks: Awake/Twilight vs General
All anesthesia pathways carry some risk, and those risks vary by individual health factors. With sedation-based approaches, common concerns include nausea, medication sensitivity, and variability in how “aware” you may feel. With general anesthesia, risks can include deeper airway-related management and stronger postoperative grogginess or nausea in some patients. The most important safety principle is that anesthesia is tailored to you—not chosen as a trend.
Two practical questions to ask any provider are:
- How do you decide whether I’m a good candidate for twilight sedation?
- What is your plan if my comfort or anxiety requires a different depth of anesthesia?
Safety Systems: What High-Standard Care Looks Like
Complication rates drop when safety is treated as a system rather than a single promise. In a high-standard pathway, you should expect:
- Preoperative screening: structured evaluation that informs anesthesia and recovery planning.
- Continuous vital monitoring: disciplined intraoperative monitoring appropriate to the anesthesia plan.
- Strict sterilization protocols: consistent, audited sterile workflows that reduce infection risk.
- Clear escalation pathways: explicit instructions for what to do if symptoms change after discharge.
At AKM Clinic, safety claims are supported with tangible standards and environment controls—such as monitored operating conditions, defined preoperative screening, and sterilization protocols described within their systems approach. When you compare providers, look for this kind of operational clarity rather than generic reassurance.
Red Flags and “When to Call” After Surgery
Many symptoms after augmentation are normal (tightness, swelling, mild asymmetry early on). However, you should seek urgent evaluation if you experience:
- Rapid one-sided swelling or a sudden change in breast size/shape,
- Worsening pain that does not respond to your prescribed plan,
- Fever, chills, or increasing redness/warmth around an incision,
- Shortness of breath, chest pain, or fainting,
- Drainage that is thick, foul-smelling, or increasing.
Expert patients often focus on “what could go wrong.” A better question is: “If something goes wrong, what is the response system?” A credible provider will answer that without defensiveness.
Awake Breast Augmentation Before and After Results: What “Natural” Looks Like
When patients say they want “natural,” they usually mean three things: (1) the breasts look proportional to their frame, (2) the shape behaves naturally in clothing and posture, and (3) the result does not look like a single surgical template applied to everyone. The most reliable way to judge outcomes is not by a single before/after image, but by how consistently a provider achieves balance across different body types.
The “Natural-First” Philosophy in Breast Augmentation
A natural-first approach prioritizes refinement over transformation. In practical surgical terms, that means:
- selecting an implant that matches your base width and tissue tolerance,
- building a pocket that centers the breast footprint and avoids chronic tension,
- planning for long-term comfort (movement, exercise, sleep),
- respecting your anatomy rather than forcing a dramatic silhouette that your tissues cannot support.
This philosophy aligns with a broader principle: the best aesthetic surgery looks like you—just more balanced and refreshed.
How to Evaluate Before/After Photos Like an Expert Patient
When reviewing results, avoid being hypnotized by “bigger.” Instead, look for repeatable markers of quality:
- Proportion: does the result fit the patient’s shoulders, waist, and overall frame?
- Implant edge visibility: do you see harsh lines or rippling, especially in thinner patients?
- Fold stability: does the inframammary fold look natural and symmetrical?
- Nipple/areola position: does it sit in a natural location relative to the new breast shape?
- Side profile transition: does the upper pole look smooth and cohesive?
Also ask: are the photos taken at consistent time points? Early post-op images can be misleading because swelling and “high-riding” implants are normal at first.
Real-World Experience: What Patients Commonly Notice After Healing
Beyond appearance, most patients care about how their result feels and functions. Common “real life” observations after the settling phase include:
- clothing fits differently (especially bras, fitted tops, swimwear),
- posture awareness improves as the body adapts to new volume,
- breast softness increases gradually over time,
- scar visibility decreases as scars mature, provided scar care is consistent.
From a provider standpoint, long-term satisfaction is driven less by a dramatic day-one reveal and more by stable positioning, comfortable movement, and a shape that still feels like “you” months later.
Our philosophy is “Rejuvenation, Not Alteration.” Discover how our surgeons achieve subtle, revitalized results that honor your unique beauty.
Awake Breast Augmentation Cost 2026 : USA vs Turkey
Cost is a legitimate part of the decision—especially for expert patients who want premium standards without paying premium-city markups. The most important concept is this: a lower price in another country does not automatically mean lower quality. In many cases, the price difference is driven by macroeconomic factors (exchange rates and operational costs), while quality is protected by the standards you verify: facility accreditation, materials, surgeon credentials, and the completeness of the care pathway.
What Drives the Price Difference?
In major U.S. markets, breast augmentation pricing is shaped by high overhead (facility costs, staffing, insurance structures), geographic demand, and local cost-of-living. In Turkey, overall operational costs can be lower, and favorable exchange-rate dynamics can amplify the gap for patients paying in USD. The correct way to interpret that difference is to audit the quality anchors—not to assume the lowest number is the goal.
Quality Anchors to Verify (Regardless of Location)
If you are comparing a premium U.S. market (such as NYC or Los Angeles) to an international option (such as Istanbul), ask for objective, verifiable markers:
- Materials standard: are the same FDA-approved materials used as in high-cost markets?
- Hospital standards: is surgery performed in a JCI-accredited hospital environment that meets Western expectations?
- Sterilization and safety systems: are there audited sterilization standards (e.g., ISO/TÜV) and continuous vital monitoring?
- Surgeon credentials: are surgeons board certified, with European board equivalents (e.g., EBOPRAS) that align with U.S. board rigor?
- Financial transparency: is pricing all-inclusive or are there hidden facility/anesthesia/aftercare fees?
All-Inclusive vs “Itemized Surprise”: What to Compare
Many patients underestimate how quickly “itemized” care grows. A meaningful comparison looks at the full care episode: pre-op testing, operating room fees, garments, medications, and follow-up care—plus the logistics burden if you are traveling.
| Cost Component | Often Itemized (Common in Premium Markets) | All-Inclusive Model (Common in International VIP Pathways) |
|---|---|---|
| Surgeon + Facility + Anesthesia | Frequently separated | Often bundled |
| Pre-op Tests | May be separate | Often included |
| Medications & Garments | Often separate | Often included |
| Post-op Follow-Up | Varies by practice | Often structured, including virtual follow-up |
| Travel Logistics | Not applicable locally | May include VIP transfers + hotel coordination |
What’s Typically Included in AKM Clinic’s VIP Package
For patients traveling to Istanbul, AKM Clinic positions its offering around a transparent, all-inclusive model designed to remove uncertainty and reduce logistical friction. In this structure, inclusions typically cover:
- Your complete surgical procedure
- Anesthesia and operating room fees
- All pre-operative tests
- 5-star hotel accommodation (with curated partners)
- All VIP airport and clinic transfers
- 24/7 dedicated Patient Host (WhatsApp access)
- All post-operative medications and garments
- First post-op meal
- Long-term virtual follow-up care
What is commonly not included in international packages: international flight tickets, personal travel insurance, visa fees (if applicable), additional hotel nights (if extending), and personal expenses (such as meals beyond the first post-op meal).
Get a 100% transparent, all-inclusive quote tailored to your needs. No hidden fees—just world-class care at an accessible price.
Choosing the Best Awake Breast Augmentation Surgeon & Facility
Awake breast augmentation demands two kinds of expertise: aesthetic planning and anesthesia pathway discipline. The best outcomes come from teams that can produce a natural result consistently and can prove they have a structured safety system for sedation-based surgery. Use the checklist below to evaluate providers with the same rigor you would apply in a high-cost market.
Credentials That Matter (And How to Verify Them)
Start with credentials and standards you can independently confirm:
- Board certification: verify the surgeon’s board pathway and continuing education.
- European board equivalents: for international options, ask about European board certifications (e.g., EBOPRAS equivalents where applicable).
- Facility accreditation: confirm surgery is performed in a fully accredited environment with audited standards.
- Safety systems: ask about sterilization standards (e.g., ISO/TÜV) and continuous patient vital monitoring during procedures.
- Confidentiality and privacy standards: confirm patient data protection protocols that meet U.S.-standard expectations.
Questions to Ask Specifically About Awake/Twilight Sedation
Because anesthesia is a major decision-driver, ask direct, practical questions:
- How do you determine candidacy for twilight sedation?
- Who is present during surgery, and what monitoring is continuous?
- How do you manage anxiety, comfort, and breakthrough discomfort?
- What is the escalation plan if my comfort requires deeper anesthesia?
- What is your discharge protocol, and how do you support patients after they return home?
Expert patients should view these as non-negotiable. A trustworthy provider will answer with clarity and specifics, not reassurance-only language.
How to Evaluate Results and Social Proof
Reviews and testimonials are not a substitute for credentials, but they can validate consistency and the patient experience. Look for:
- Consistency across body types: not just one “perfect” before/after.
- Mentions of communication quality: planning, responsiveness, and clarity.
- Details about recovery support: what happens after discharge, especially for international patients.
For example, a U.S. patient shared that their partner had surgery while they had breast implants—and described the overall care as exceptional, noting attentiveness throughout the process. This kind of detail is useful because it reflects the operational experience, not just the aesthetic outcome.
Perform your surgery with confidence. Meet our European Board Certified surgeons with over 2,000 successful facial surgeries.
The Medical Journey (International Patient Logistics)
If you are traveling for surgery, your outcome depends on more than the operating room. Logistics can either reduce anxiety and support recovery—or add stress at the exact time your body needs calm and consistency. A reliable international pathway is structured, transparent, and built to eliminate decision fatigue so you can focus on preparation and healing.

Step 1: Free Virtual Consultation (From Home)
The journey typically begins with a no-obligation video consultation. You discuss goals, share photos for review, and receive a personalized treatment plan with a transparent all-inclusive quote. For expert patients, this is also the stage where candidacy for an awake/twilight approach should be discussed in detail.
Step 2–4: VIP Planning, Airport Welcome, and Procedure Day
In a well-run VIP model, once you proceed, a dedicated Patient Host coordinates the core logistics: procedure date, 5-star hotel planning, and VIP transfers. On arrival in Istanbul (IST or SAW), you are met personally and transferred to the hotel. On procedure day, your host coordinates transport to the clinic, you have a final in-person consultation, and pre-op tests are completed before surgery in a fully accredited environment.
Step 5–6: Post-Op Support in Istanbul and Long-Term Follow-Up at Home
After surgery, you are monitored closely, and your Patient Host remains available 24/7 via WhatsApp for questions or needs. Before departure, you have a final in-person check to confirm recovery progress and flight readiness. After you return home, structured virtual follow-up appointments are scheduled at 1, 3, 6, and 12 months to support continuity of care—an important concern for international patients who fear being “on their own” after returning.
From VIP airport transfers to 5-star hotel accommodations, we handle every detail. Enjoy a seamless medical travel experience in Istanbul.
Frequently Asked Questions
This FAQ section answers the most common “expert patient” questions in a direct, voice-search-friendly format. These answers are general education and not a substitute for an individualized medical evaluation. Your best decisions will come from matching your anatomy, goals, and health profile to the right surgical and anesthesia plan.
Can you be awake for breast augmentation?
Yes—many patients can undergo breast augmentation without traditional general anesthesia, using a plan that combines local anesthesia (to numb the surgical area) with twilight sedation (to keep you calm, sleepy, and comfortable). “Awake” usually does not mean fully alert. Most patients are drowsy, relaxed, and often remember very little. The key is candidacy: your medical profile, anxiety tolerance, and procedure complexity must match the awake/twilight approach. A responsible provider will never “force” awake surgery if your comfort or safety would be better served by general anesthesia.
What is twilight sedation and what does it feel like?
Twilight sedation is a sedation technique designed to reduce anxiety and awareness while you remain in a comfortable, sleepy state. Many patients describe it as feeling like drifting in and out of light sleep—calm, relaxed, and unconcerned about time passing. You may still hear muffled sounds or sense gentle pressure (not sharp pain if local anesthesia is done properly), and you may respond to simple cues if needed. Afterward, some patients feel clearer sooner than they expect, while others feel mildly groggy for a short period. Your experience depends on the depth of sedation, your sensitivity to medications, and your baseline anxiety level.
Is twilight sedation safe?
Twilight sedation can be safe when it is selected appropriately and delivered within a disciplined safety system. “Safe” is not just the medication—it’s the entire process: preoperative screening, appropriate monitoring during surgery, a team experienced in sedation-based procedures, and a clear plan for adjusting sedation depth if needed. The most important question is not “Is twilight sedation safe in general?” but “Is twilight sedation safe for me given my health profile and my comfort needs?” If you have significant anxiety, certain medical conditions, or a procedure plan that is expected to be longer or more complex, your provider may recommend a different anesthesia approach for stability and comfort.
Twilight sedation vs general anesthesia: which is better for recovery?
Recovery experiences vary widely by individual, but many patients exploring awake breast augmentation do so because they want to avoid the “fully asleep” pathway and may hope for a smoother immediate recovery experience. With twilight sedation, patients often report a calmer transition out of surgery and, in some cases, less intense grogginess—though this is not guaranteed. General anesthesia can also be very safe and well-tolerated, and it may be the best choice for patients who would find any awareness distressing, or for surgical plans that require deeper control. The most reliable way to choose is to discuss your nausea history, anxiety tolerance, and medical profile with the anesthesia team and surgeon. The best recovery is the one supported by the safest and most predictable plan for you.
Will I feel pain or remember anything during awake breast augmentation?
Most patients should not feel sharp pain when local anesthesia is performed thoroughly and sedation is appropriately tailored. However, you may feel non-painful sensations such as pressure, movement, or gentle pulling. Memory varies: some patients remember almost nothing; others recall brief moments. If the idea of sensing anything (even pressure without pain) would cause you distress, that is important to disclose early—because comfort tolerance is part of candidacy. High-quality teams also build flexibility into the plan so that if you need deeper sedation for comfort, they can adjust safely.
How long is the awake breast augmentation recovery timeline?
Most patients move through recovery in phases. In the first 72 hours, tightness, swelling, and soreness are common. By the end of week 1, many patients feel significantly better in daily mobility—but internal healing is still early, and overactivity can set you back. Weeks 2–6 are typically the “settling phase,” when swelling continues to improve and the implants gradually sit in a more natural position. Full softening and scar maturation can continue for months. Your surgeon will provide a personalized timeline for returning to exercise, lifting, and overhead movement based on your pocket placement and tissue response. If you’re traveling, you should also plan for follow-up structure and a clear “when to call” pathway after you return home.
What are the risks of awake breast augmentation?
The risks of breast augmentation are primarily surgical—regardless of anesthesia method. These include bleeding (hematoma), infection, fluid collection (seroma), wound-healing issues, asymmetry, implant malposition, rippling/edge visibility, capsular contracture, and possible sensation changes. Anesthesia-related risks differ by pathway and by individual; with sedation-based plans, concerns may include nausea, medication sensitivity, and variability in awareness. The most meaningful way to reduce risk is choosing a provider with (1) disciplined pre-op screening, (2) a sterile, accredited facility environment, (3) strong intraoperative monitoring, and (4) accessible post-op support. Ask specifically what the response plan is if a complication occurs—because outcomes depend on early detection and correct escalation.
How much does awake breast augmentation cost?
Cost varies by geography, surgeon experience, facility standards, anesthesia model, and what is included. In premium U.S. cities, pricing often reflects high overhead and may be itemized (surgeon fee, facility fee, anesthesia fee, garments, medications, follow-ups). In Istanbul, many high-standard clinics offer an all-inclusive model that can reduce surprise costs and simplify planning—especially for international patients. The right comparison is not “lowest price,” but “best value with verified standards.” When comparing quotes, request a written breakdown of what’s included, where surgery takes place, which materials are used, what follow-up looks like after you return home, and what happens if you need urgent advice post-travel.
When can I fly after awake breast augmentation?
Flying after surgery depends on your recovery progress, the distance of travel, and your personal risk factors. International travel adds complexity because prolonged sitting and dehydration can increase discomfort and, in some cases, clotting risk. Your provider should give you a specific flight-readiness assessment before you travel, including guidance on mobility, hydration, compression strategy (if recommended), and what symptoms require urgent evaluation. If you are an international patient, choose a clinic that provides a structured in-country recovery plan and clearly scheduled follow-up after you return home so you are not left without guidance.
How do I choose the right surgeon for awake breast augmentation?
Choose the surgeon and facility the same way you would in a premium U.S. market: verify credentials, evaluate safety systems, and assess consistency of results. Ask about board certification pathways (or European board equivalents), the accreditation standard of the facility where surgery is performed, sterilization and monitoring protocols, and candidacy criteria for twilight sedation. Then evaluate the process quality: do they take measurements, discuss tissue limitations honestly, explain tradeoffs clearly, and provide a written recovery roadmap? Finally, look at results with a critical eye—proportion, fold stability, edge visibility, and how outcomes look across different body types—not just one standout case.
Medical Disclaimer: This content is for educational purposes only and does not replace medical advice, diagnosis, or treatment. Surgical outcomes and anesthesia suitability vary by individual. Always consult a qualified, board-certified surgeon and anesthesia team for personalized evaluation, risks, benefits, and recovery guidance. Seek urgent care for severe symptoms.
Awake Breast Augmentation: Patient Stories

Lisa

Awake Breast Augmentation Surgeons
Awake Breast Augmentation Cost in Turkey
Starting from $5400
* There are no hidden fees or unexpected charges.
- Your Personalised Awake Breast Augmentation Procedure
- All Specialist Surgeon & Anesthesia Fees
- All Pre-Op Tests & Post-Op Check-ups
- 5-Star Hotel Accommodation (incl. breakfast)
- All Private VIP Airport & Clinic Transfers
- 24/7 Dedicated Patient Coordinator & Translation Services
Awake Breast Augmentation: A Cost Comparison
| City | Cost |
|---|---|
| Miami, FL | ~$10,000 |
| New York, NY | ~$13,500 |
| Los Angeles, CA | ~$12,800 |
| Houston, TX | ~$9,500 |
Discover Our All-Inclusive Packages in Turkey
Awake Breast Augmentation: Patient Reviews
Jammal Canada
I have had face and neck lift with AKM Clinic they have been so good to me and my operation went so smoothly🥰 i would like to thank my doctor here and also to the team 💐

Ava Canada
Thank you AKM Clinic for giving me my confidence back! Had facelift + temporal lift 3 months ago and the outcome is already stunning. Special thanks to Hande!

Jakayla USA
Had a deep plane facelift and lower eyelid procedure at AKM Clinic 7 months ago. The results are fantastic - very subtle and natural. I didn’t expect the entire experience to be so comfortable. Hande managed everything and kept in contact even after I returned to USA. I’m beyond pleased with the outcome and the care I received. Would do it again in a heartbeat!

Barbara United Kingdom
It has been 4 months since my surgery. Everything is great, The most important thing is l love the way l look, l look exactly how l wanted. Meaning l look natural, just almost 40 years younger. I pulled Facebook - majority voted 37ys. I also had face, neck, chest, and hands CO2 laser. My skin is flawless.

Lisa Canada
I had a face, neck and arm lift at AKM. I’m just over 4 weeks post and couldn’t be happier with the results. The entire experience was wonderful! My coordinator, Khadija made me feel comfortable from beginning to end! I highly recommend AKM and will definitely go back for other procedures!

Julie USA
I am beyond grateful I went with AKM Clinic for my deep plane face and neck lift, upper eyelid, and co2 laser. Dr. Akif has magic hands and my results are truly incredible! I came from the US and assistant Emine was the best in assuring every detail was coordinated and communicated with me beyond my expectations every step of the way. 10 out of 10 to the entire team! I couldn’t be more pleased!

Ready to Start Your Own Transformation Journey?
Join the 2,000+ patients who trusted Dr. Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, revitalized you begins with a simple, no-obligation conversation. Contact us today from the USA for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. No hidden fees.
#2: Secure Your Date & VIP Booking
Once you're ready, our dedicated patient coordinators will help you secure your procedure date. We'll handle all your bookings, including your 5-star hotel and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you'll meet your specialist surgeon to finalise the details for your "natural, subtle, and revitalized" new look.

















