Facelift Pain Management for U.S. Patients: Your Day 1–10 Comfort & Safety Guide

- Facelift pain management day 1–10: expect tightness/pressure peaks days 3–5, improving by day 8–10.
- What’s normal vs red flags: tightness/numbness OK; rapid one-sided swelling, fever, or escalating pain needs urgent contact.
- Medication safety for US travelers: follow surgeon plan, avoid unapproved OTC/supplements, keep ingredient list and dosing log.
- Comfort strategies to speed recovery: elevate head, sleep on back, short walks, hydration/protein, and optional HBOT/LLLT support.
Summary generated by AI, fact-checked by our medical experts
For the “expert patient” who wants specifics: this guide explains facelift pain management in practical, day-by-day terms—what “normal” discomfort feels like, what helps, and what should trigger a call to your surgeon.
Important: This content is educational and not a substitute for personalized medical advice. Your exact pain after facelift can vary based on technique (e.g., deep plane facelift pain may feel different from lighter lifts), anesthesia plan, your pain sensitivity, and how your tissues heal.
Real-patient perspective matters: One U.S. “expert patient” (Barbara, deep plane facelift + neck lift) described her recovery as “no pain” with minimal bruising—an encouraging example, but not a guarantee. Your goal is a plan that keeps you comfortable and safe.
Single-patient quotes are easy to dismiss as cherry-picked. The pattern across many patient narratives is harder to dismiss — and that pattern is what verifies whether one quote represents the typical experience or the unusual one.
For the cross-patient view, additional verified patient reviews cover recovery experiences across procedures and patient profiles, pain trajectory descriptions in patients’ own words (which often differ from clinical descriptions in useful ways), medication experiences, and the texture of long-term satisfaction that single testimonials can’t capture.
Reading 20 reviews tells you what reading one cannot — whether the headline experience is representative or exceptional.
If you’re traveling for surgery, the most reassuring question is not “Will I have facelift pain?”—it’s: “What is the exact pain management after facelift surgery plan from day 1 to day 10?” Surgeon-led teams typically combine (1) gentle surgical technique, (2) smart anesthesia/local comfort strategies, (3) a structured medication plan when appropriate, and (4) recovery protocols to reduce swelling-driven pressure (some clinics add advanced options like HBOT and LLLT to help speed up facelift recovery).
“Surgeon-led” is a phrase that gets used loosely. The version that matters in pain management is the one where the surgeon directly designs the medication plan, the anesthesia approach, and the aftercare protocol — not where a coordinator picks them from a menu.
For the care-model documentation, the AKM Clinic care model overview covers the surgeon-led decision architecture, the medical team structure that supports it, accountability standards across the patient journey, and the operating principles that determine how pain management decisions are made for any specific patient rather than from a default protocol.
Care models are easier to compare than marketing copy — and they’re usually documented somewhere, if the clinic actually has one.
Pain management is the part of facelift planning that gets the most search volume but the least context — and “what will I feel on day three” only makes sense once you understand what’s actually being done surgically.
For the procedural foundation underneath the day-by-day comfort timeline, the complete facelift procedure guide covers technique families, candidacy ranges, 3D planning, anesthesia options, and the structural decisions that determine which pain trajectory a specific patient is likely to follow.
The recovery conversation only becomes useful once the procedural conversation is properly anchored.
Table of Contents
What Pain Level to Expect (Day 1–10)
Most patients describe the first 10 days less as “sharp pain” and more as a mix of tightness, pressure, and “pulling” sensations—especially around the lower face and neck. In other words, the headline feeling is often discomfort rather than true “pain facelift.” The timeline below is a practical baseline for facelift pain level expectations, including common hot spots like pain behind ears after facelift surgery and neck pain after facelift, grounded in medical science and postoperative physiology.
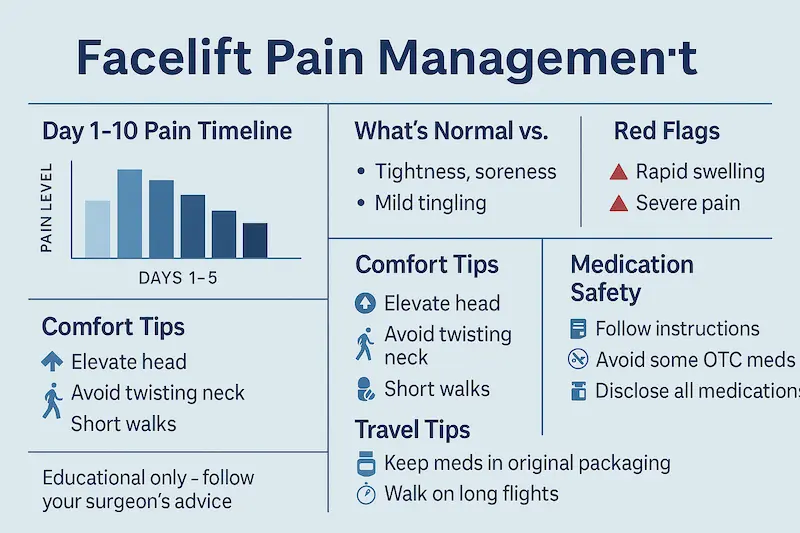
Day-by-day expectations (Day 1–3 vs Day 4–7 vs Day 8–10)
| Timeframe | Typical Sensation / Facelift Pain Level | What You May Notice | What Helps Most | When to Contact Your Surgeon |
|---|---|---|---|---|
| Day 1–2 | Usually mild to moderate discomfort (often more pressure than pain) | Tightness, swelling, “full” sensation, sore throat (if intubated), grogginess; possible ear pain after facelift surgery or tenderness behind the ears | Head elevation, strict rest, cold compresses if approved, hydration, short assisted walks, staying on schedule with your surgeon’s plan | Sudden one-sided swelling, rapidly escalating pain, bleeding, breathing issues, or severe nausea/vomiting |
| Day 3–4 | Discomfort often peaks as swelling “sets in” | More noticeable tightness along jawline/neck; tenderness around incision lines; pain behind ears after facelift can feel like “pressure” | Elevation while sleeping, gentle movement, protein-forward meals, avoiding bending/lifting, consistent aftercare | New fever, worsening redness, foul drainage, or pain that’s clearly getting worse (not just “different”) |
| Day 5–7 | Typically improving; many feel “tight” but less sore | Bruising shifts color; “zinging” or tingling can occur as nerves wake up; mild neck pain after facelift with turning | Continue elevation, avoid strenuous activity, follow compression/garment instructions exactly, keep incisions clean and dry as directed | Increasing tenderness + heat + swelling at one spot (possible infection) or a new hard expanding swelling |
| Day 8–10 | Mostly manageable; “numb + tight” is common | Residual swelling and stiffness; sensitivity near the ears and neck; itching as healing progresses | Gradual return to light routine, continue scar/skin protocol as directed, protect from sun | Any symptom that suddenly reverses your progress or feels “wrong” for your baseline |
Key point: A “comfortable” recovery is not an accident. It’s the result of structured facelift post operative care—and a clear plan for deep plane facelift pain management if you’re doing a more advanced lift.
“Pain” vs. Tightness, Pressure, and Nerve Sensations (what’s normal)
When patients search “pain after facelift surgery,” they often expect sharp pain. In reality, common sensations include:
- Tightness / pulling: especially along the jawline and neck. This is often the #1 sensation people label as “facelift pain.”
- Pressure behind the ears: the area where incisions may sit and where swelling can collect—often searched as pain behind ears after facelift or pain behind ears after facelift surgery.
- Numbness: very common; it can make the area feel “strange” rather than painful.
- Tingling / zaps: brief nerve “wake-up” sensations that can appear days into healing.
For the research-driven patient, the most useful mindset is this: swelling and tissue tension drive most discomfort. This is why strategies that reduce swelling (positioning, activity rules, and—when used—advanced recovery support) can meaningfully improve the overall facelift recovery experience.
Where discomfort is most common (jawline, neck, and behind the ears)
Most facelift pain is not “deep aching” in the face itself—it’s usually tension + swelling in predictable zones. Understanding the anatomy helps you interpret what you’re feeling and reduces anxiety about pain after facelift surgery.
- Behind the ears (very common): Searches like pain behind ears after facelift surgery and pain behind ears after facelift are common because this area can feel tight, tender, or “pressure-like” where incisions and dressings may sit.
- The neck and under the chin: Neck pain after facelift is often a stiffness sensation—especially with turning your head—because the neck skin and deeper tissues are healing and swelling can pool with gravity.
- Jawline and lower face: A “band-like” tightness is one of the most typical facelift pain level descriptions, particularly days 3–5.
- Temples/scalp (if incisions extend into the hairline): Numbness, tenderness, or a strange “pins and needles” feeling is common as sensory nerves recover.
Deep plane facelift pain: With a deep plane technique, discomfort can still be very manageable, but the “tightness” may feel more pronounced early on because deeper layers have been repositioned. A structured deep plane facelift pain management plan focuses on controlling swelling and protecting the repair—more than “chasing pain.”
Expert-patient reassurance: If your main sensation is tightness, pressure, or intermittent tingling, that often fits normal healing. The “not normal” scenarios are usually rapidly worsening pain or swelling—especially if it’s one-sided.
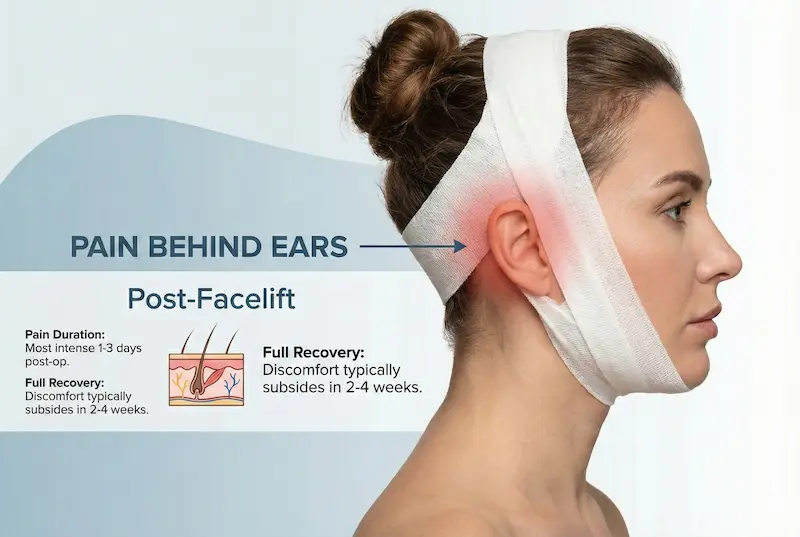
Ear Pain After Facelift Surgery: What It Usually Means
Ear pain after facelift surgery is usually not “ear pain” from inside the ear. It’s typically tenderness from nearby incisions, swelling, or dressings/garments that create pressure around the ear contours.
- Typical: soreness when you touch behind the ear, a “pressure” sensation, sensitivity when the garment is tight, mild burning/itching as nerves wake up.
- Less typical: pain that sharply escalates hour by hour, a rapidly expanding swelling behind the ear, or severe pain with a new firm lump (these need prompt assessment).
If you’re worried about pain behind ears after facelift, the best move is often simple: check garment fit and swelling control (with your surgeon’s guidance). Over-tight compression can create unnecessary discomfort.
Our philosophy is “Rejuvenation, Not Alteration.” Discover how our surgeons achieve subtle, revitalized results that honor your unique beauty.
Sleep positioning, compress timing, and activity rules that reduce pain
When patients ask how to speed up facelift recovery, what they often mean is: “How do I reduce swelling-driven discomfort and feel normal sooner?” The answer is not heroic toughness—it’s precision in the first 10–14 days of facelift post operative care.
| What to Do | Why It Helps (Pain & Swelling) | Common Mistake |
|---|---|---|
| Sleep on your back with your head elevated (often 30–45°) | Reduces fluid pooling in the face/neck, which lowers pressure and overall pain after facelift | Side-sleeping early → increased swelling and “pulling” sensation |
| Use a travel pillow or wedge setup to keep your head midline | Prevents sudden twisting that can spike neck pain after facelift and strain healing tissues | “Flat pillow + rolling over” during sleep |
| Short, frequent walks (as cleared) | Supports circulation and reduces stiffness without raising blood pressure | Long walks or stairs too early → swelling flare |
| Hydration + protein-forward meals | Supports tissue repair; dehydration can worsen headaches and fatigue that patients label as “pain” | Low appetite → low protein → slower recovery |
| Avoid bending, heavy lifting, and intense exercise | Limits blood pressure surges that can worsen swelling and discomfort | “Feeling good” on day 5 and overdoing it |
Cold vs. warm compresses: Many surgeons allow gentle cold support early to reduce swelling-related discomfort—but timing and placement must be surgeon-specific. Never place ice directly on skin, never wet your incisions unless instructed, and avoid aggressive heat early unless your surgeon explicitly recommends it.
- If approved: cool compresses (not ice) can help the “pressure” component of pain after facelift surgery.
- Always avoid: compressing directly over fresh incision lines or causing numb, overly cold skin.
Advanced Recovery Support (HBOT & LLLT) and Swelling-Related Discomfort
For the highly analytical patient, here’s the key concept: if swelling drives a large portion of discomfort, then therapies that reduce inflammation and support tissue oxygenation can indirectly improve the overall facelift pain management experience.
These are adjuncts—they do not replace your surgeon’s medical plan for pain management after facelift surgery, but they can support healing when used appropriately within a clinic protocol.
Hyperbaric Oxygen Therapy (HBOT): You breathe 100% oxygen in a pressurized chamber. The goal is to increase oxygen delivery beyond what normal circulation can provide—especially helpful when tissues are healing and blood flow is temporarily disrupted after a facelift.
- Why “expert patients” care: oxygen availability supports tissue survival, reduces inflammation-related swelling, and may help with scar quality.
- How it can affect comfort: less swelling often means less “tight pressure,” which many people experience as their main facelift pain level.
“Breathing 100% oxygen at pressure” is the headline mechanism, but the actual recovery effect comes from what that elevated oxygen delivery does to tissues that are temporarily oxygen-starved while bruising and swelling resolve.
For the mechanism, dose-response, and protocol layer, the hyperbaric oxygen therapy deep-dive covers chamber pressures, session lengths typically used in postoperative protocols, candidacy criteria (and contraindications worth knowing), and where the evidence is strongest for inflammation-driven discomfort versus marketing claims that outrun the data.
The most useful framing: HBOT is an adjunct that supports swelling resolution — not a substitute for the surgical-care plan above.
Low-Level Laser Therapy (LLLT): This is a non-heat “soft laser” approach designed to stimulate cellular activity without damaging tissue. In post-facelift recovery, the goal is to support cellular repair, collagen processes, and inflammation reduction.
- Why it matters for recovery: calmer inflammation can mean less redness and swelling—again, the big drivers of perceived pain facelift.
- Where it fits: typically as part of a structured aftercare plan, alongside incision care and swelling management.
Low-level laser therapy gets called “soft laser” or “cold laser” because there’s no thermal damage — the mechanism is photobiomodulation, where specific wavelengths trigger cellular responses rather than burning tissue.
For the wavelength specifics, session protocols, and outcome data, the low-level laser therapy breakdown covers what LLLT does at the cellular level, where it fits in postoperative timelines, what the evidence shows for scar maturation and inflammation, and how clinics integrate it with the rest of the aftercare plan rather than running it as a standalone “treatment.”
Like HBOT, the honest framing is “adjunct, not magic” — but adjuncts that target inflammation can meaningfully shift the perceived comfort experience.
Practical takeaway: If your discomfort feels like “pressure + tightness,” your biggest win is often swelling control (positioning + activity rules + surgeon-approved therapies), not stronger medication.
Medications Used in Turkey vs USA
For most U.S. patients, the biggest anxiety around pain management after facelift surgery is not “Will I get something strong enough?”—it’s “Will I understand exactly what I’m taking, and is it safe with my existing meds?” This section breaks down what’s typically used after a facelift, how to interpret Turkish prescriptions versus U.S. norms, and how to stay safe—especially if you’re flying home during early facelift recovery.
Safety first: Do not add, stop, or swap medications (including OTC pain relievers and supplements) without your surgeon’s approval. Most preventable complications after facial surgery come from “helpful” self-adjustments—especially with blood-thinning products.
Medication safety is not a single-surgeon concern — it’s a team-level discipline that includes the anesthesiologist, the surgical nurse, the postoperative coordinator, and any specialists pulled in for comorbidities or unusual histories.
For the team-level view, the full surgical and medical team profile covers the surgeons, anesthesia leadership, dedicated postoperative nursing, the patient-safety coordinator role, and the cross-discipline structure that medication safety, pain management, and recovery monitoring actually run through in day-to-day clinical operations.
A practice that names one surgeon and leaves the rest of the team invisible is harder to evaluate than a practice that documents the full chain of accountability.
Typical Post-Op Medication Categories (pain control, antibiotics, anti-nausea, stomach protection)
Most modern protocols aim for opioid-sparing pain control—meaning comfort is achieved with a layered plan, and stronger medications are reserved for short-term breakthrough discomfort (if needed). Common categories include:
- Baseline pain control: often acetaminophen/paracetamol-based options, sometimes combined with other non-opioid strategies. (Always follow your surgeon’s dosing plan and label maximums.)
- Anti-inflammatory pain control: some surgeons use NSAIDs selectively; others avoid them early due to bleeding/bruising risk. This is highly surgeon-specific.
- Antibiotics: when indicated, prescribed to reduce infection risk around incision lines.
- Anti-nausea medication: helpful if you’re sensitive to anesthesia or stronger pain meds.
- Stomach protection: sometimes used when certain pain medications or antibiotics irritate the stomach.
- Constipation prevention: if an opioid is prescribed, many teams proactively recommend a stool-softening strategy.
Because the dominant sensation after a facelift is often tightness/pressure rather than sharp pain, many patients find that consistent baseline comfort measures + swelling control (sleep position, activity rules, surgeon-directed aftercare) do most of the heavy lifting for facelift pain management.
What U.S. Patients Should Know About Brand Names vs. Generic Equivalents
In Turkey, you may see medication brand names that look unfamiliar—even when the active ingredient is the same as what you’d see in the U.S. The “expert patient” approach is simple:
- Match by active ingredient, not brand: ask your coordinator/nurse for a written list of active ingredients (and strengths) in English.
- Keep one master medication list: include your home meds + the clinic’s post-op meds + any OTC products you take.
- Watch for duplicates: the same active ingredient can appear in multiple products (for example, “cold/flu” combos that also contain acetaminophen).
- Don’t assume “stronger is better”: oversedation can increase fall risk, constipation, nausea, and dehydration—none of which helps speed up facelift recovery.
| What You See on the Box | What Actually Matters | What to Ask Your Clinic For |
|---|---|---|
| Unfamiliar Turkish brand name | Active ingredient + strength + schedule | English medication sheet listing ingredients and timing |
| “Painkiller” label | Is it non-opioid vs opioid? Any combined ingredients? | Whether it contains sedatives, acetaminophen, or NSAIDs |
| Multiple meds that “sound similar” | Risk of double-dosing an ingredient | A single consolidated timetable (morning/noon/evening) |
We use advanced Hyperbaric Oxygen Therapy (HBOT) to minimize downtime and supercharge your healing process. Safety is our #1 promise.
What you should avoid without surgeon approval (especially blood-thinning OTCs/supplements)
One of the most important risk-reduction steps in facelift post operative care is avoiding products that can increase bruising or bleeding unless your surgeon explicitly approves them.
- Common OTC blood-thinners: aspirin-containing products and some anti-inflammatory medications may increase bruising/bleeding risk for certain patients and timeframes.
- Supplements with “blood-thinning” potential: examples often include fish oil/omega-3s, vitamin E, ginkgo, garlic, turmeric/curcumin, and others. (This is exactly why you should disclose all supplements pre-op.)
- Alcohol: can worsen swelling, bruising, dehydration, and sleep quality—often making pain after facelift feel worse.
- Nicotine: not a “pain med” issue, but critical for healing—nicotine can compromise circulation and slow recovery.
Rule of thumb: If it’s not on your surgeon-approved list, don’t take it—especially in the first 10–14 days when small changes can have outsized effects on swelling and bruising.
A practical plan for flying home: timing doses, managing constipation, and refill logistics
If you’re returning to the U.S. while still in early facelift recovery, a good plan prevents “medication chaos” on travel day—a common trigger for unnecessary pain after facelift surgery.
- Build a travel-day schedule: ask your team to write a simple chart with local times and your destination time zone for the first 48 hours after landing.
- Keep meds in original packaging: and carry them in your personal item (not checked luggage).
- Ask for documentation: a brief clinic letter listing your surgery date, the medications prescribed, and that they are for personal post-op use.
- Plan for constipation: dehydration + reduced movement + certain pain meds can slow the gut. Hydrate, walk periodically (as cleared), and follow your surgeon’s constipation-prevention guidance.
- Don’t “save” pain meds for later: comfort is easier to maintain than to regain. Follow the plan proactively rather than waiting until you’re miserable.
- Refill reality check: if you might need additional medication after returning home, discuss this before you leave Turkey. Cross-border refills can be complicated, and your U.S. physician may want documentation.
“Flying home on day 10” is one waypoint in a longer choreography that starts before the flight to Istanbul and continues for months afterward — and pain management is one workstream among several that the larger plan has to coordinate.
For the end-to-end view, the full patient journey roadmap covers the pre-travel medical workup, arrival and clinic days, surgery day staging, day-by-day in-Istanbul recovery, the return flight, and the months-long follow-up cadence — including the touchpoints where pain management, medication continuity, and incision care all intersect.
Patients who treat travel-day logistics as a standalone task usually find seams that the journey-level plan would have prevented.
Medication safety checklist for “Expert Patients” (allergies, blood thinners, SSRIs, supplements)
Use this checklist to minimize risk and maximize clarity. This is particularly important if you take long-term medications or have prior anesthesia sensitivities.
- Allergies and intolerances: antibiotics, NSAIDs, opioids, adhesives, latex—document reactions (rash, swelling, nausea, breathing issues).
- Blood thinners / antiplatelets: if you take any, your surgeon must coordinate timing. Never restart on your own timeline.
- SSRIs/SNRIs and other psychiatric medications: disclose all; some combinations may influence bleeding risk or interact with certain pain medicines.
- Sleep medications, benzodiazepines, cannabis products: can compound sedation and safety risk.
- Supplements: list everything, even “natural” products.
- History of severe nausea: ask about a proactive anti-nausea plan—nausea can make pain feel worse and can stress healing tissues.
- One-page medication map: name → active ingredient → purpose → timing. Keep a copy on your phone.
Nerve Blocks & Local Techniques
For many U.S. patients, the most reassuring part of facelift pain management is learning that comfort often starts before you even wake up—through local anesthesia strategies, careful tissue handling, and (in some cases) nerve blocks. This is especially relevant if you’re comparing traditional approaches to newer protocols and wondering why some people report very manageable pain after facelift.
In surgeon-led care, pain control is not just “a prescription.” It’s a system: anesthesia plan + surgical technique + swelling control + structured aftercare. That’s also why two patients can have very different facelift pain level experiences even when they had “the same” procedure on paper.
“Awake facelift” gets discussed as a single category, but it’s really a family — different procedures, different sedation depths, different candidacy criteria. The umbrella term hides more variation than it reveals.
For the program-level view, the awake surgery program overview covers which facial and body procedures the awake approach extends to, the tumescent local anesthesia technique that makes most of these procedures feasible, candidate criteria across procedure families, and the safety framework underneath the marketing label of “awake.”
The category question deserves more time than the procedure question — patients tend to default to one over the other and miss whether awake is even the right vehicle for what they specifically want done.
Local/tumescent anesthesia basics and why it can reduce early discomfort
Many facelift techniques use local anesthetic solutions placed into targeted tissues. You may hear terms like local infiltration or tumescent solution. The purpose is to:
- Reduce immediate post-op pain: by numbing tissues during and after surgery.
- Support controlled swelling: swelling is a major driver of perceived pain after facelift surgery because it creates pressure and tightness.
- Improve comfort during early movement: such as the first walk, meals, and sleep transitions.
“Local plus sedation” versus “general anesthesia” is not a binary preference — it’s a structured decision shaped by candidacy criteria, intraoperative comfort thresholds, recovery profile, and which combinations a specific surgical team is set up to deliver safely.
For the side-by-side analysis, the anesthesia options comparison guide walks through what each approach actually involves physiologically, candidate criteria for tumescent local with sedation, cardiovascular load differences, postoperative pain trajectory differences (the part this article focuses on), and how anesthesia choice interacts with the medication plan described in the section above.
Reading the anesthesia comparison before the consultation is one of the highest-leverage preparation steps a patient can take.
For the “expert patient,” the important takeaway is that local techniques can make the first 12–24 hours feel more like pressure/tightness than true facelift pain. When this is paired with an opioid-sparing plan, many patients feel clear-headed sooner, which can help facelift recovery behaviors like hydration, gentle walking, and better sleep positioning.
Nerve safety in facelift surgery sits at the intersection of two patient anxieties: “Will I have permanent numbness or weakness?” and “How is that risk actually being managed during the procedure?” The honest answer requires data, not reassurance.
For the synthesis layer, 2025 systematic review of nerve injury rates across 67 facelift studies and 15,404 patients (Gandra, Silva, Horta, Aesthetic Plastic Surgery / Springer Nature) — searching PubMed, EMBASE, and Web of Science using DerSimonian-Laird random-effects modeling — reported pooled nerve injury rates that varied substantially by technique, surgeon experience, and patient anatomy, with most documented injuries being transient rather than permanent.
That distinction — transient versus permanent — is the one patients should hold onto when reading the section above about “zaps” and “wake-up” sensations during recovery.
Nerve blocks explained (what they do, how long they can last, what you feel as they wear off)
A nerve block is an injection of local anesthetic near specific nerves to reduce pain signals for a period of time. In facial surgery, the goal is to reduce discomfort in key zones (jawline/neck/around the ears) that patients often search as pain behind ears after facelift surgery or neck pain after facelift.
How long can it last? This depends on the medication used and your metabolism. Some patients feel significant numbness for many hours; others feel it fading sooner.
What it feels like when it wears off:
- A gradual “return of sensation”: often tingling or warmth rather than sudden sharp pain.
- Intermittent zaps: brief nerve “wake-up” sensations can occur as tissues heal.
- Increased tightness/pressure: sometimes mistaken for “worsening pain,” but often reflecting swelling patterns rather than a true complication.
Practical tip: If your surgeon provides a scheduled plan for baseline comfort (rather than “take only when it hurts”), following that schedule during the block-wearing-off window often prevents an avoidable pain spike.
What About Pain During the Actual Surgery?
This guide is entirely focused on your post-operative recovery (Days 1-10). But what if you are anxious about the operation itself? Many of our patients choose to bypass general anesthesia altogether.
If you want to know exactly what you will feel on the operating table, how twilight sedation works, and why patients describe the procedure as “pressure, not pain,” read our dedicated guide: Is an awake facelift painful?
Surgeon-led pain plan: how technique + gentle tissue handling affects inflammation-based pain
Patients often assume pain facelift is primarily about how “big” the surgery is. In reality, technique can strongly influence inflammation and swelling—two major drivers of discomfort.
- Precise dissection + controlled handling: less unnecessary trauma generally means less inflammatory swelling and less pressure-driven discomfort.
- Meticulous hemostasis: reducing oozing/bleeding lowers swelling and bruising, which can lower the “tight pressure” component of facelift pain level.
- Deep plane technique considerations: deep plane facelift pain is often manageable, but the post-op sensation may be more “structural tightness” early on. That’s why deep plane facelift pain management is frequently centered on swelling control, sleep posture, and guided activity more than high-dose medication.
At AKM Clinic, facial aesthetic procedures are approached with a team mindset that includes a Dermatosurgeon working alongside the plastic surgery team—an advantage for patients who want natural results while also prioritizing skin quality and healing behavior during facelift recovery.
Non-medication comfort strategies used in modern aftercare (compression, drainage, skincare support)
Non-medication strategies often make a bigger difference than patients expect—especially for the common discomfort patterns of pain behind ears after facelift, ear pain after facelift surgery, and neck pain after facelift.
- Compression/garments (when used): should support swelling control without creating excessive pressure around the ears. Over-tight garments can increase perceived pain.
- Drain management (if drains are used): proper care can reduce swelling and pressure-related discomfort. Many patients feel relief once drains are removed, but this varies by protocol.
- Incision care and skin support: clean, dry, protected incisions reduce irritation and “stinging” sensations. Your team’s skincare guidance matters—especially for sensitive skin types.
- HBOT & LLLT adjuncts (when included): may support tissue recovery and inflammation control—helpful for patients trying to speed up facelift recovery in a safe, structured way.
Facelift Pain Management Toolkit: What to Pack, Track, and Ask Before You Travel
A clear, practical toolkit can make facelift pain management feel far more predictable—especially for U.S. patients traveling for surgery. The goal is simple: reduce swelling-driven discomfort, avoid medication mistakes, and spot “not normal” changes early. This preparation is particularly helpful if you’re concerned about pain after facelift surgery, including pain behind ears after facelift surgery or neck pain after facelift.

Pre-Op: The 5-minute safety list your surgeon needs
Before surgery, send your team a one-page list of current medications, allergies, and supplements. This supports safer prescriptions and smoother recovery planning—especially if you want an opioid-sparing approach. Include any blood thinners, SSRIs/SNRIs, sleep aids, and “natural” supplements that could affect bruising. If you’re planning a deep plane lift, ask specifically about deep plane facelift pain management expectations and your day-by-day comfort plan.
Pack a comfort kit that supports swelling control
Most “facelift pain” is really tightness and pressure from swelling. Bring a wedge pillow or travel pillow for back-sleeping, easy-to-wear button-up tops, and surgeon-approved cold support supplies. Add protein-forward snacks, hydration support, and a simple timer app for medication schedules. Smart packing helps speed up facelift recovery by making it easier to follow your facelift post operative care routine consistently.
Post-Op: Track progress so you can get help fast
Use a daily log: pain score (0–10), exact location, swelling pattern (stable vs one-sided), temperature, and meds taken. Take the same-angle photos once daily. If pain suddenly escalates, swelling rapidly increases on one side, or redness/warmth worsens, contact your surgeon immediately—especially
Our surgery dates fill up quickly due to high international demand. Secure your consultation today to plan your ideal travel dates.
When Pain Is Not Normal
Most pain after facelift is predictable: tightness, pressure, tenderness around incision lines, and occasional tingling as nerves “wake up.” What you’re watching for is a different pattern—pain that is rapidly escalating, one-sided, or paired with new symptoms that suggest a complication.
For U.S. patients traveling for surgery, this section matters even more because it gives you a clear “what to do next” framework—especially if you’re already home and experiencing pain after facelift surgery that feels different from the day before.
Surgeon-led rule: “Normal” healing evolves gradually. A complication often shows up as a sharp change—a sudden jump in swelling, a new firm lump, or pain that’s getting worse instead of better.
Red flags in the first 24–72 hours (sudden one-sided swelling, rapidly worsening pain)
The first 3 days are when teams are most vigilant about bleeding-related issues and early pressure problems. Contact your surgical team urgently (or seek emergency care if you cannot reach them) if you notice:
- Sudden, rapidly increasing swelling—especially if it’s mostly on one side.
- Rapidly worsening pain that does not respond to your prescribed plan and feels “out of proportion.”
- Firm, expanding swelling (a new tight “balloon” sensation), sometimes associated with increasing neck pain after facelift or behind-the-ear pressure.
- Active bleeding that soaks dressings.
- Breathing or swallowing difficulty, severe dizziness, fainting, or chest symptoms (treat as an emergency).
Important: Do not press hard, massage, or “try to drain” anything yourself. If you suspect a complication, the safest move is immediate professional assessment.
Warning signs later in week 1–2 (infection signals, fever, foul drainage, escalating tenderness)
As days progress, discomfort should generally trend down—even if tightness and numbness linger. In week 1–2, reach out quickly if you have:
- Fever (especially if persistent) or chills.
- Increasing redness, warmth, and swelling concentrated around one incision area.
- Foul-smelling drainage or new pus-like discharge.
- Escalating tenderness at one spot after you had been improving.
- New severe ear-area pressure that feels like worsening pain behind ears after facelift surgery rather than steady healing soreness.
Infection is not the most common issue after a well-managed facelift—but early recognition is essential. If you’re already back in the U.S., your surgical team should still guide next steps (and coordinate local evaluation if needed).
Numbness vs. nerve injury: what timelines are typical
Numbness is extremely common after facelift surgery and often lasts longer than “pain.” Many patients interpret numbness, tingling, or brief “zaps” as facelift pain, but these sensations can be part of normal nerve recovery.
- Often normal: patchy numbness around the ears, jawline, and neck; mild tingling; sensitivity that comes and goes.
- Worth flagging: new weakness, a dramatic shift in sensation paired with rapidly increasing swelling, or symptoms that worsen rather than slowly improve.
If you’re unsure, treat it like an “expert patient” would: document it (photos + notes) and ask your surgeon whether your pattern fits typical healing for your procedure (including deep plane facelift pain profiles).
“Call now” vs. “Monitor” decision guide
This is a practical decision tool for facelift pain management anxiety reduction. When in doubt, contact your surgical team—especially if you’re traveling.
| Symptom | Pattern | What It May Suggest | Action |
|---|---|---|---|
| One-sided swelling + rapidly increasing pain | Sudden change over hours | Possible bleeding/collection creating pressure | Call now (urgent assessment) |
| New firm expanding lump (jaw/neck/behind ear) | Growing, tight, pressure-like | Fluid/pressure issue that may need evaluation | Call now |
| Fever + localized redness/warmth + worsening tenderness | Worsening day-to-day | Possible infection | Call within hours (same day) |
| Tightness, numbness, mild tingling | Stable or slowly improving | Typical healing sensations | Monitor and follow aftercare plan |
| Ear-area soreness / pressure | Improves with garment adjustment per instructions | Often dressing/garment pressure or swelling | Monitor, ask team if unsure |
| Neck stiffness with turning | Gradual improvement | Common early neck pain after facelift | Monitor, avoid strain, follow movement guidance |
What to document for your surgeon (photos, symptom timeline, meds taken)
If you report pain after facelift surgery, your surgeon can help faster when you send structured information. Use this checklist:
- Photos: front + both sides + close-up of the area (same lighting if possible).
- Timeline: when it started, whether it’s getting better/worse, and any trigger (activity, coughing, bending, travel day).
- Pain description: pressure vs burning vs sharp; constant vs intermittent; exact location (jawline, neck, pain behind ears after facelift).
- Swelling description: one-sided vs both; soft vs firm; new lump or expanding area.
- Temperature: your measured temperature if you feel feverish.
- Medication log: what you took, the dose, and the time (this is crucial for safe advice).
- Other symptoms: nausea/vomiting, dizziness, shortness of breath, drainage changes, new redness/warmth.
Experience a Truly Supported Recovery
At AKM Clinic, we don’t just perform surgery; we engineer your recovery. From continuous monitoring to advanced HBOT support, your comfort is our priority. If you are ready to entrust your face to a team that takes pain management as seriously as natural results, explore our comprehensive Facelift surgery in Turkey packages and secure your consultation today.
Facelift Pain Management Frequently Asked Questions (FAQ):
FAQ sections answer the most common questions, but patients flying for surgery usually carry a longer tail of specific concerns — about visas, refunds, partner accommodation, dietary restrictions, prescription refills, follow-up timing — that don’t fit a single-topic FAQ.
For the cross-topic answers, the broader patient FAQ resource covers logistics, payment, language support, accompanying companion arrangements, prescription continuity questions for international patients, and the operational questions that surface once the medical research is already done.
The medical questions usually get researched first; the operational questions usually decide whether the trip actually happens.
Is a facelift painful?
Most patients report facelift pain as tightness, pressure, and tenderness rather than sharp pain. The “pain facelift” experience is often driven by swelling and tissue tension—especially around the jawline, neck, and behind the ears.
How long does pain last after a facelift?
For many people, the most noticeable facelift pain level (pressure/tightness) is within the first week, often peaking around days 3–5 as swelling settles. By days 8–10, discomfort is usually more manageable, though tightness and numbness can linger longer than “pain after facelift.”
What is the best sleeping position after a facelift to reduce discomfort?
On your back, head elevated, and neck supported (often with a wedge or travel pillow) is the standard comfort strategy. This reduces swelling-related pressure and can significantly improve pain management after facelift surgery—especially if you’re experiencing neck pain after facelift.
Can I take ibuprofen/aspirin after a facelift?
Only if your surgeon approves. Many teams restrict aspirin-containing products and certain anti-inflammatories early because they can increase bruising/bleeding risk. For U.S. patients, this is a top cause of preventable issues during facelift post operative care, so don’t self-start or self-switch medications.
What if I feel burning, tingling, or shooting pain—normal or not?
Mild tingling, “zaps,” or burning sensations can be normal as nerves recover—especially near the jawline, neck, and ear area. However, if these sensations come with rapidly worsening swelling, a new firm lump, fever, or pain that is escalating rather than improving, treat it as “not normal” and contact your surgeon.
How do I manage nausea or constipation from pain medication?
Nausea and constipation are common side effects of stronger pain medications and can make pain after facelift surgery feel worse overall. Typical strategies include surgeon-approved anti-nausea medication, hydration, short frequent walks, and a constipation-prevention plan (often stool softener/fiber guidance). Do not add OTC products without your team’s OK—especially if you’re traveling.
What should U.S. patients do if pain worsens after returning home?
First, document the change (photos + a timeline + meds taken). Then contact your surgical team promptly—especially if you have one-sided swelling, rapidly increasing pain, fever, redness/warmth, foul drainage, or a new firm expanding area. If you cannot reach your team and symptoms are escalating, seek urgent in-person evaluation.
Why do I feel pressure or pain behind the ears after facelift surgery?
Pain behind ears after facelift surgery is often caused by normal incision-area tenderness, swelling, or compression garment pressure. If discomfort improves with surgeon-approved garment adjustments and doesn’t rapidly worsen, it’s usually part of healing. Sudden one-sided swelling or escalating pain should be reported immediately.
Can HBOT or LLLT help with facelift pain management?
These therapies are adjuncts, not replacements for medical care. By supporting inflammation control and tissue recovery, HBOT and LLLT may reduce swelling-driven tightness—helpful for overall facelift pain management and for patients aiming to speed up facelift recovery safely.
What’s the safest way to manage pain after facelift surgery once I’m back in the U.S.?
Stick to your surgeon’s plan, avoid adding OTC meds or supplements without approval, and keep a daily log (pain level, location, swelling pattern, temperature, meds taken). If pain after facelift surgery is rapidly worsening, one-sided, or paired with fever/redness/drainage, contact your surgical team promptly
Medical Disclaimer: This content is for educational purposes only and does not replace medical advice. Facelift outcomes, risks, and recovery vary by individual. Always consult a qualified, board-certified surgeon for diagnosis and treatment decisions. If you have a medical emergency, seek immediate local care.
Related Treatments
Ready to Start Your Own Transformation Journey?
Join the 2,000+ patients who trusted Dr. Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, revitalized you begins with a simple, no-obligation conversation. Contact us today from the USA for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. No hidden fees.
#2: Secure Your Date & VIP Booking
Once you're ready, our dedicated patient coordinators will help you secure your procedure date. We'll handle all your bookings, including your 5-star hotel and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you'll meet your specialist surgeon to finalise the details for your "natural, subtle, and revitalized" new look.











