Awake Gynecomastia Surgery in Turkey




Awake Gynecomastia: Quick Facts
Procedure Time
Anesthesia
Recovery Time
Hospital Stay
Back to Work
Awake Gynecomastia Results: Before and After
Gynecomastia—often described by patients as a “puffy nipple” look or a soft, rounded chest contour—is one of the most common male body concerns. The issue is rarely just cosmetic. It can change how you dress, how you train, and how you carry yourself in social settings. The good news is that modern surgical planning makes gynecomastia highly treatable, and the “awake” approach (local anesthesia with optional twilight sedation) has become a logical choice for the research-driven patient who prioritizes safety, a predictable experience, and a smoother recovery pathway.
In this guide, you’ll learn what gynecomastia truly is (and what it isn’t), how surgeons decide between liposuction and gland removal, and what “awake gynecomastia surgery” actually feels like in real life. The goal is clarity: if you understand your tissue type, your anatomy, and your anesthesia options, you can make a decision that feels medically sound—not emotionally rushed.
Table of Contents
What Is Gynecomastia? Anatomy, “Puffy Nipples,” and Root Causes
Gynecomastia is an enlargement of male breast tissue that can involve glandular tissue, fatty tissue, or a combination of both. Many men assume it’s simply “fat on the chest,” but the underlying anatomy is more nuanced. The most effective surgical plan depends on one question: what exactly is creating the shape you see in the mirror?
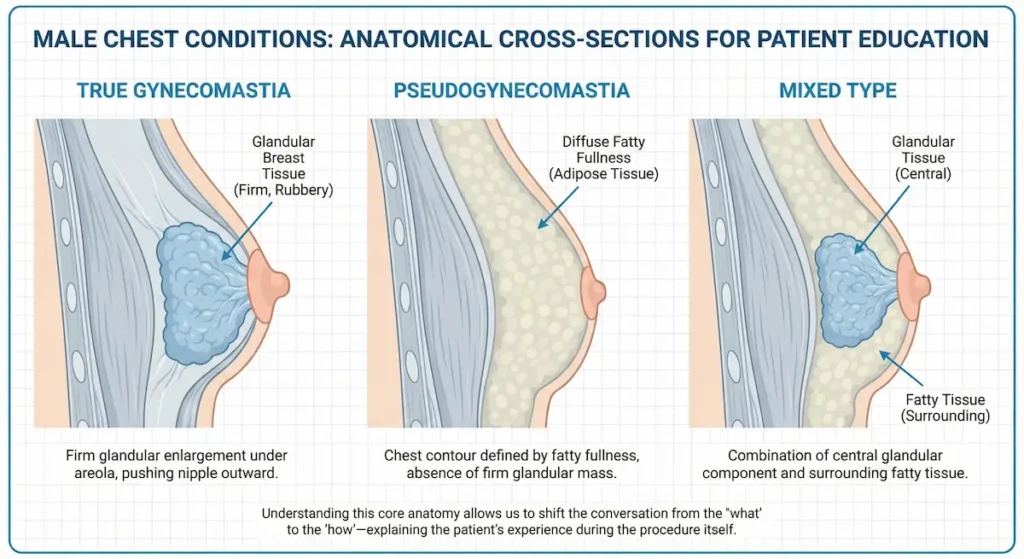
True Gynecomastia vs. Pseudogynecomastia (Gland vs. Fat)
True gynecomastia refers to a firm, rubbery enlargement of glandular breast tissue—often most noticeable directly under the areola. This gland can create a distinct “puffy nipple” profile, especially when the surrounding chest is relatively lean.
Pseudogynecomastia is primarily fatty fullness of the chest. It may look similar in clothing, but the tissue behavior is different. Fatty tissue can respond more predictably to contouring (liposuction), while firm glandular tissue often requires direct excision (removal) to achieve a flatter, more masculine contour.
Most real-world cases are mixed: a combination of fat and gland that requires a combination approach. This is why “one-size-fits-all” promises don’t belong in gynecomastia surgery—your tissue determines the technique.
The 3 Outcome Drivers: Gland, Fat, and Skin Elasticity
Three physical factors shape both your surgical plan and your final result:
- Gland size and density: A firm gland beneath the areola can “push” the nipple-areola complex outward. If gland is the dominant issue, liposuction alone may improve the chest but leave residual puffiness.
- Fat distribution: Some patients carry fat diffusely across the chest and toward the armpit area. Strategic contouring can create a smoother transition from the upper chest to the lower pectoral border.
- Skin elasticity and laxity: Skin that retracts well typically conforms beautifully after tissue removal. If the skin is significantly loose (often after major weight loss or long-standing gynecomastia), additional tightening strategies may be required to avoid residual sagging.
From an outcomes perspective, “flat” is not the real goal. The goal is a natural male chest contour: defined but not hollow, smooth but not over-suctioned, and consistent from multiple angles.
Common Causes: Hormones, Weight Changes, Medications, Lifestyle
Gynecomastia can occur at different life stages. Puberty-related gynecomastia may resolve on its own, while adult gynecomastia is more likely to persist. Common contributing factors include:
- Hormonal shifts: An imbalance between estrogenic and androgenic activity can promote gland growth.
- Weight changes: Fat gain can increase chest fullness; weight loss can reveal glandular tissue that was “hidden” beneath fat.
- Medications and substances: Certain medications and anabolic-androgenic steroid use can contribute to breast tissue changes in men.
- Underlying medical conditions: In select cases, additional evaluation may be appropriate—especially when gynecomastia appears suddenly, is painful, or is associated with other systemic symptoms.
A high-quality consultation doesn’t treat the chest like an isolated “problem area.” It treats it as anatomy with a cause, a tissue profile, and a surgical solution that must be personalized.
What Does “Awake Surgery” Mean? Local Anesthesia, Tumescent Technique, and Twilight Sedation
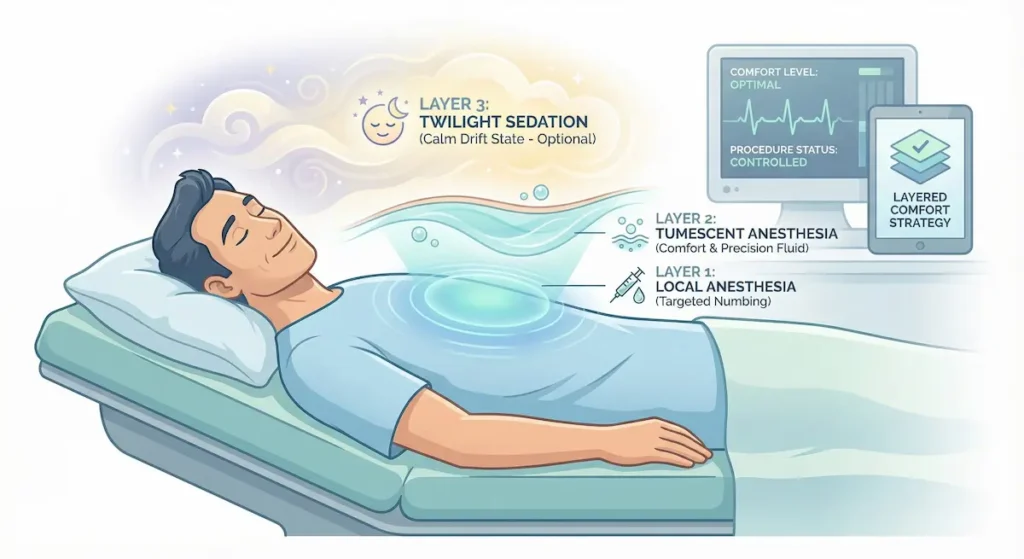
“Awake gynecomastia surgery” does not mean you are fully alert, uncomfortable, or “white-knuckling” your way through a procedure. In modern practice, the awake approach is best understood as a layered comfort strategy: local anesthesia for numbness, tumescent anesthesia to support both comfort and contouring, and optional twilight sedation to help you feel calm and relaxed while maintaining a lighter anesthesia profile than general anesthesia.
How Local Anesthesia Works (Mechanism + What You Actually Feel)
Local anesthesia works by temporarily blocking nerve signaling in the treated area. In practical terms, the goal is straightforward: you should not feel sharp pain in the surgical field. Patients often describe initial numbing as pressure or brief stinging, followed by a progressive “deadening” of sensation.
During the procedure, what you may feel is typically limited to pressure, movement, and gentle tugging—not pain. If you feel discomfort, the team can adjust the anesthesia in real time. This ability to titrate comfort is one reason many “expert patients” appreciate the awake approach: the experience is controlled, responsive, and closely monitored.
What Is Tumescent Anesthesia—and Why It Matters in Gyno Surgery
Tumescent anesthesia refers to the infiltration of a specialized fluid mixture into the targeted tissue plane. From a surgical planning standpoint, it matters for several reasons:
- Comfort support: It enhances the numbing effect across a broader tissue area.
- Cleaner contouring: It helps create a more controlled tissue environment for liposuction-based contouring.
- Reduced bleeding potential: By supporting a more controlled field, it can contribute to a smoother operative experience and recovery.
In other words, tumescent technique is not “just an extra step.” It is part of the engineering of awake surgery: comfort, precision, and recovery strategy built into the method.
What Does Twilight Sedation Feel Like? (Awake, Relaxed, Comfortable)
Twilight sedation—often described as a “calm drift” state—can help patients feel significantly more relaxed while still avoiding the full depth of general anesthesia. Experiences vary, but many patients report:
- Feeling drowsy and peaceful, with reduced procedural awareness
- Minimal memory of the procedure, even though they were not under full general anesthesia
- A smoother emotional experience—less anticipatory anxiety, less “time awareness”
The key point is that “awake” exists on a spectrum. Some patients prefer minimal sedation and a stronger sense of control; others prefer deeper twilight sedation for a more detached experience. A well-structured surgical team will match the anesthesia plan to your medical profile, anxiety level, and procedural complexity.
In the next sections, we’ll define who is an ideal candidate for awake gynecomastia surgery, how surgeons plan the technique (liposuction vs gland excision vs combination), and how anesthesia choice compares to general anesthesia from a risk-management and recovery standpoint.
Ideal Candidates for Awake Gynecomastia Surgery
Not every patient with chest fullness needs the same surgical approach—and not every patient is an ideal fit for an “awake” plan. The best candidates tend to share three traits: a tissue profile that can be treated predictably, a medical history that supports local anesthesia with (optional) twilight sedation, and a mindset that values a controlled, safety-forward experience. In practice, candidacy is less about “toughness” and more about anatomy, planning, and medical appropriateness.
Mild to Moderate Cases with Good Skin Retraction
Many of the strongest candidates for awake gynecomastia surgery fall into the mild-to-moderate category, where the goals are contour refinement and areolar flattening without the need for major skin excision. Typical features include:
- Localized fullness under the areola (often the “puffy nipple” pattern)
- Small to moderate gland component, sometimes combined with a layer of fat
- Skin that still has good elasticity and is likely to retract after tissue removal
- Stable weight (or close to your long-term maintenance range)
When skin quality is good, the chest often “settles” into a more masculine contour as swelling resolves and the skin redrapes. This is one reason surgeons emphasize patience: early postoperative swelling can temporarily hide the final shape, especially around the areola.
Advanced Cases: Skin Laxity, Larger Glands, and When Lifts Are Needed
Awake surgery can still be an option for select advanced cases, but the decision becomes more nuanced. Patients with long-standing gynecomastia or significant weight changes may have:
- More skin laxity (the chest may hang or fold, especially when bending)
- Larger or denser gland tissue that drives projection and areolar puffiness
- Wider chest distribution extending toward the lateral chest (near the armpit)
In these situations, a surgeon may recommend a combination plan that addresses both tissue volume and skin behavior. Sometimes contouring plus gland removal achieves a strong result; other times, skin excision or repositioning strategies may be necessary for the chest to look proportionate and natural. The important point is not the label (“awake” or “general”)—it’s whether the chosen plan produces a predictable outcome with an appropriate safety profile for your medical situation.
Who Should Wait or Get Further Workup (Red Flags + Medical Considerations)
High-quality gynecomastia care includes knowing when to pause. In some scenarios, it may be safer—or simply smarter—to delay surgery until the underlying picture is clearer. Common reasons to “slow down and evaluate” include:
- Rapid onset or sudden growth of breast tissue (especially if one-sided)
- Persistent pain, tenderness, or nipple discharge
- New lumps that feel different from typical glandular fullness
- Use of anabolic-androgenic steroids or other substances that may continue driving tissue growth
- Unstable weight (ongoing weight loss or frequent cycles of gain/loss)
- Medical history that requires additional clearance (bleeding disorders, uncontrolled hypertension, certain cardiac or pulmonary conditions)
Some patients also benefit from an endocrine or medication review—especially if the gynecomastia appears with other systemic symptoms. This isn’t meant to create friction; it’s how a responsible plan is built. When the goal is a stable, long-term result, the best surgical timing is the one that aligns with your health and your biology.
If you’re an “expert patient” who wants maximum control, candidacy is good news: it means the procedure can be planned with fewer unknowns. And fewer unknowns generally translates into a smoother operative experience and a more predictable recovery.
Answer a few quick questions about your concerns, health, and goals to learn which treatment options may suit you best.
Pre-Op Evaluation and Surgical Planning (Safety First)
Gynecomastia surgery is often described as “straightforward,” but excellent results are rarely an accident. They come from pre-operative clarity: understanding your tissue profile, defining what “natural” means on your frame, and choosing the technique and anesthesia plan that fits both your anatomy and your medical risk profile. The pre-op phase is where outcomes are engineered.
Physical Exam and Tissue Mapping (Asymmetry, Areola, Chest Wall)
In a proper evaluation, the surgeon is not only looking at “size.” They are mapping shape. Common planning checkpoints include:
- Tissue composition: how much is gland, how much is fat, and how “fixed” the tissue feels under the areola
- Asymmetry analysis: most chests are not perfectly symmetric; the plan should account for realistic balance rather than chasing artificial perfection
- Areola position and projection: areolar “puffiness” often reflects gland prominence, skin laxity, or both
- Chest wall anatomy: pectoral development, ribcage shape, and the desired contour line
This mapping is what determines whether liposuction alone can meet the goal, whether direct gland removal is needed, and how aggressive contouring should be to avoid an over-skeletonized or “operated” look.
Labs/Screening When Indicated (A Safe Candidate Checklist)
Even when gynecomastia surgery is performed under local anesthesia with twilight sedation, pre-op screening matters. The exact workup varies by patient, but a safety-forward checklist often includes:
- Medical history review: anesthesia reactions, clotting issues, previous surgeries, allergies
- Medication review: blood thinners, hormones, supplements that may affect bleeding or swelling
- Vitals and baseline health assessment: blood pressure, general fitness, relevant chronic conditions
- Targeted lab work when your history suggests it is appropriate
The goal is simple: minimize preventable risks. “Awake” is not a shortcut around safety—it’s a different anesthesia strategy that still requires a disciplined medical process.
Medications, Supplements, Nicotine, and Bleeding Risk
A surprisingly large portion of postoperative issues—excess bruising, prolonged swelling, delayed healing—can be influenced by what happens before surgery. Common pre-op guidance (always individualized to your clinician’s instructions) may include:
- Blood-thinning agents: certain medications and supplements can increase bruising/bleeding risk; your team will advise what to pause and when
- Nicotine management: nicotine can impair microcirculation and slow healing; stopping is one of the most meaningful “outcome upgrades” you can control
- Alcohol and dehydration: both can increase inflammation and complicate recovery comfort
- Fitness and nutrition: stable protein intake, reasonable activity, and adequate sleep support tissue recovery
Pre-op planning is also where you align expectations with reality. For example, many patients want to know: “Will my nipples be perfectly flat immediately?” Often, the most accurate answer is: not on day one. Swelling and tissue settling take time, and early contours can look deceptive. A good plan prepares you for what’s normal, what’s temporary, and what would be a reason to contact your care team.
Next, we’ll move into the surgical techniques themselves—liposuction, gland excision, and combination methods—so you can understand what your surgeon is actually doing (and why) during awake gynecomastia surgery.
Get a clear, day-by-day itinerary covering arrival, surgery, recovery, and fit-to-fly clearance tailored to your schedule.
Surgical Techniques: Liposuction, Gland Excision, and Combination Approaches
Gynecomastia surgery is not a single technique—it’s a surgical strategy tailored to tissue type. The most consistent, natural-looking outcomes come from correctly identifying what is driving projection (fat, gland, or both) and then choosing the least invasive method that reliably corrects the contour. In awake gynecomastia surgery, the same technical standards apply as in surgery under general anesthesia: precision matters, and over-treatment can look just as unnatural as under-treatment.
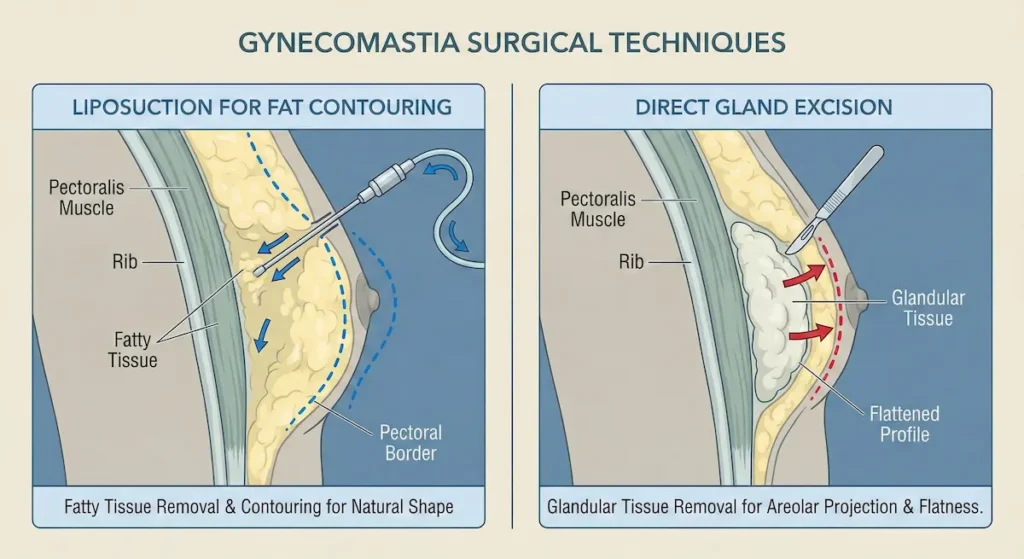
Liposuction-Dominant Gynecomastia (Fat-Predominant)
When chest fullness is primarily fatty, liposuction can be the workhorse technique. The goal isn’t simply “removing volume.” It’s sculpting a natural male chest line—typically creating a smooth transition from the upper chest to the lower pectoral border without dips, ridges, or sharp edges.
In fat-dominant cases, the surgeon focuses on:
- Even contour transitions: avoiding a “suctioned-out” or hollow center
- Lateral chest blending: reducing fullness that extends toward the armpit area
- Areolar behavior: understanding whether the areola projection is driven by fat or underlying gland
A key limitation: if a firm gland is present under the areola, liposuction may improve the chest globally but leave a residual “puffy nipple” profile. That’s not a failure of liposuction—it’s a mismatch between technique and tissue.
Gland Excision-Dominant Gynecomastia (Firm Tissue Under the Areola)
If the dominant problem is a dense gland beneath the areola, direct excision is often required to achieve a flatter, more masculine contour. Patients frequently describe gland tissue as a “rubbery disc” or “lump” that doesn’t change even with weight loss and training.
In gland-dominant cases, surgeons typically plan:
- Targeted removal: removing enough gland to flatten projection while avoiding an overly hollow areola
- Contour preservation: maintaining a natural thickness so the chest doesn’t look “scooped out”
- Scar placement strategy: placing incisions in discreet locations when possible
Because the areola is the visual focal point of the chest, gland handling is one of the biggest determinants of whether results look natural. The technical goal is not “maximum removal.” It’s balanced removal—enough to correct the contour while preserving a believable male anatomy.
Combined Technique for Natural Contour (Feathering + Flat-to-Masculine Transition)
Many patients benefit most from a combined approach: liposuction to contour the broader chest and excision to address the central gland. This strategy often produces the best “from all angles” result because it corrects both the global fullness and the localized areolar projection.
A combined plan typically emphasizes:
- Layered contouring: treating the chest as a gradient, not a single “problem spot”
- Edge feathering: smoothing transitions to reduce contour irregularities
- Symmetry engineering: addressing natural left-right differences with realistic balance
It’s worth noting that the word “combined” can sound bigger or scarier than it is. In practice, it means the surgeon is using the right tool for each tissue layer—fat gets contoured, gland gets corrected, and skin is managed through careful planning and postoperative support.
| Technique | Best For | Main Advantage | Common Limitation | Typical Scar Consideration |
|---|---|---|---|---|
| Liposuction | Fat-predominant chest fullness | Smooth contouring over a broad area | May not fully correct puffy areola if gland is present | Small entry points, often discreet |
| Gland Excision | Firm gland under the areola | Direct correction of areolar projection | Requires precision to avoid “crater” deformity | Often placed at the areolar border for camouflage |
| Combined Approach | Mixed fat + gland (most common scenario) | Addresses both global contour and central projection | Requires careful blending to avoid irregularities | Small liposuction entry points + discreet excision scar |
Anesthesia Options: Awake (Local + Sedation) vs. General Anesthesia
Anesthesia choice is not a badge of bravery—it’s a medical decision. The “awake” approach can be highly appealing because it avoids the full depth of general anesthesia, often supports a quicker sense of “back to yourself,” and aligns with a control-focused patient mindset. However, the right answer depends on procedure complexity, patient anatomy, medical history, and comfort needs. The safest anesthesia is the one that is appropriately selected, properly dosed, and professionally monitored.
When Awake Gynecomastia Surgery Makes the Most Sense
Awake gynecomastia surgery (local anesthesia with optional twilight sedation) is often a strong fit when:
- The planned correction is mild to moderate and does not require extensive skin excision
- The patient is medically appropriate for local anesthesia and sedation-based monitoring
- The patient values reduced “system load” compared to general anesthesia (less deep anesthesia, often less grogginess)
- Anxiety is manageable with a tailored sedation plan and clear expectations
From the “expert patient” perspective, one of the most compelling aspects is real-time adjustability: local anesthesia can be reinforced if needed, and sedation depth can be tuned for comfort. For many patients, this creates a calmer experience than they expect.
When General Anesthesia May Be the Better Choice
General anesthesia may be more appropriate when:
- The procedure is more extensive, especially if significant skin tightening or complex revisions are planned
- Patient comfort would be compromised by remaining partially aware, even with sedation
- Medical considerations suggest that a controlled airway and deeper anesthesia plan is preferable
- Operative time and complexity are expected to be higher
For some patients, general anesthesia is the most psychologically comfortable option. The point is not to “sell” one method—it’s to match the method to the real-world scenario. A provider you can trust will explain the reasoning clearly and will not force-fit you into an anesthesia plan that doesn’t suit your needs.
Direct Safety Questions Answered: “Is Local Anesthesia Dangerous?” “Can It Kill You?”
These are not dramatic questions—they are rational questions from a patient who values safety. The responsible answer is: any anesthesia has risk, but serious complications are uncommon when local anesthesia and sedation are used appropriately, with correct dosing and professional monitoring. Risk rises when protocols are ignored, dosing is mishandled, patient selection is poor, or monitoring is inadequate.
Here’s what “safety” really means in the awake context:
- Proper dosing and technique: Local anesthetics must be dosed within safe limits for body weight and technique. Experienced teams follow strict dosing protocols.
- Monitoring: Sedation and patient physiology should be monitored throughout the procedure. Safety is not “being awake.” Safety is being observed and supported continuously.
- Medical screening: Identifying risk factors before surgery (cardiac history, medication interactions, uncontrolled blood pressure, etc.) is part of risk reduction.
- Emergency preparedness: A professional setting is prepared to respond to unexpected reactions—this is one reason facility standards matter.
In other words, the awake approach is not inherently “risk-free,” and it should never be framed that way. Its advantage is that, for many appropriate candidates, it can offer a more conservative anesthesia depth while still maintaining comfort—particularly when the procedure is well-suited to local anesthesia and the provider follows disciplined protocols.
| Factor | Awake (Local + Twilight Sedation) | General Anesthesia |
|---|---|---|
| Level of unconsciousness | Light to moderate sedation; often drowsy/relaxed | Fully unconscious |
| Airway management | Typically no airway tube (depends on sedation depth) | Airway support is standard |
| Recovery “feel” | Often quicker return to baseline alertness | Can involve more grogginess and nausea in some patients |
| Best suited for | Mild–moderate cases; control-focused patients | More extensive cases; complex revisions; deeper comfort needs |
| Key requirement | Strict dosing + continuous monitoring + appropriate candidate selection | Comprehensive anesthesia team + facility standards |
Next, we’ll walk through the procedure step-by-step so you know what happens from marking to compression—and how the awake approach changes (and does not change) the surgical fundamentals.
Step-by-Step: How Awake Gynecomastia Surgery Is Performed
When patients hear “awake surgery,” they often imagine a fundamentally different operation. In reality, the surgical fundamentals are the same: the surgeon still needs to create a natural male chest contour, manage bleeding and swelling, and protect the nipple-areola complex while correcting projection. What changes is the anesthesia strategy and—often—the recovery “feel.” A clear step-by-step walkthrough reduces uncertainty and helps you evaluate whether a provider’s process is structured, safety-forward, and predictable.
Marking and Surgical Design (What the Surgeon Measures and Why)
Before any anesthesia is administered, the surgeon typically performs careful markings while you’re standing. This matters because the chest shape changes with posture and gravity. Marking is where the plan becomes visual and measurable, including:
- Areas of fullness: central (subareolar), lower chest, and lateral chest (toward the armpit)
- Asymmetry mapping: subtle left-right differences that can affect areola position and contour
- Contour targets: where a flatter plane is desired and where gentle thickness should be preserved for a natural look
For the “expert patient,” this is also the moment to confirm priorities: is your primary goal a flatter areola, a more athletic chest line, or both? Good planning is not only technical—it aligns surgical actions with your definition of “natural.”
Tumescent Infiltration → Liposuction → Gland Removal (If Needed)
After sterile preparation, the team administers local anesthesia and then infiltrates tumescent solution into the planned treatment zones. The sequence typically follows your tissue profile:
- Tumescent infiltration: enhances comfort and creates a controlled tissue environment for contouring
- Liposuction contouring: targets fatty fullness, blends the chest into the lateral zone, and smooths transitions
- Direct gland correction: if a firm gland is present under the areola, it may be reduced or removed through a discreet incision strategy
A key technical point: surgeons aim to avoid over-resection beneath the areola. The chest should look masculine—not “hollowed out.” A natural male chest has a subtle thickness gradient; the best results preserve that anatomy while eliminating the unwanted projection.
If twilight sedation is used, many patients feel calm and detached during this phase—often describing it as “time passing quickly” with minimal procedural memory. If minimal sedation is used, patients commonly report pressure sensations rather than pain, with comfort adjusted as needed.
Closure, Dressings, Compression Garment, and the First 24 Hours
After contour goals are achieved, the surgeon closes incision points and applies dressings. A compression garment is typically placed to support swelling control and help the skin conform to the new contour. In some cases, drains may be used; in other cases, a drain-free strategy may be appropriate depending on tissue volume, technique, and surgeon preference.
The first 24 hours are about stability:
- Swelling management: compression + rest + structured movement (light walking)
- Comfort management: a clear pain-control plan and guidelines for what is normal vs. what is not
- Hydration and mobility: gentle movement supports circulation; heavy activity is avoided
Patients often underestimate how much “normal” swelling can temporarily distort the look of the areola. Early changes are not the final result. The recovery section below explains what to expect and when.
Our surgery dates fill up quickly due to high international demand. Secure your consultation today to plan your ideal travel dates.
Awake Gynecomastia Recovery Timeline and Aftercare
Recovery is where most anxiety lives—especially for the expert patient who wants to plan downtime precisely. The most helpful way to think about gynecomastia recovery is as a sequence of phases: early stabilization (first days), functional recovery (weeks 1–2), and contour maturation (weeks 6–12 and beyond). Swelling is not just “a nuisance”; it’s a biological process that resolves gradually. A structured aftercare plan helps you avoid setbacks and supports a cleaner final contour.
The First 72 Hours: Swelling, Drainage, Pain Control, Walking
In the first three days, your body responds to the procedure with inflammation—this is normal. Typical experiences include:
- Swelling and bruising: often more noticeable around the areola and lower chest
- Firmness: the chest can feel tight, thick, or “puffy,” which can be frustrating but is expected early on
- Drainage: if tumescent fluid was used, mild leakage from small entry points may occur for a short period
- Discomfort: commonly described as soreness or pressure rather than sharp pain
What helps most in this phase is consistency: wearing compression as instructed, keeping movements gentle, and walking lightly to support circulation. You’ll also receive guidance on sleeping position (often on your back), hydration, and what symptoms should prompt you to contact your care team.
Weeks 1–2: Return to Work, Compression, Bruising and Swelling Strategy
Many patients can return to desk work and light daily activity within the first 1–2 weeks, depending on the extent of surgery and their recovery comfort. This is the phase where bruising fades and swelling begins to shift and soften—but it can be uneven.
Common realities in weeks 1–2 include:
- Fluctuating swelling: you may look better one day and “puffier” the next
- Areolar irregularity: temporary wrinkling, firmness, or unevenness can occur while tissues settle
- Compression is doing work: consistent wear supports swelling control and skin redraping
Light walking is usually encouraged. Heavy lifting and chest workouts are typically delayed to reduce swelling spikes and protect the surgical contour while internal healing progresses.
Weeks 6–12: Training, Final Contour, Scar Maturation, Tissue Softening
By 6 weeks, many patients can gradually return to more structured training, depending on surgeon guidance and how the chest is healing. However, “feeling normal” does not always mean “fully matured contour.” The chest continues to change as tissues soften and swelling resolves at a deeper level.
In this maturation phase, patients often notice:
- Improving contour definition: the chest looks more stable across different postures and lighting
- Softening of firmness: small areas of tightness gradually settle
- Scar evolution: scars typically look more noticeable early, then improve with time and proper care

The most important long-term concept is patience. A natural chest contour is the product of surgery plus biologic remodeling. If you evaluate too early, you risk misreading normal swelling as “the final outcome.”
Accelerated Recovery & Safety Protocol: HBOT + LLLT
Recovery technologies can be marketed like gadgets, but in a serious clinical setting they should function as part of a structured protocol. At AKM Clinic, Hyperbaric Oxygen Therapy (HBOT) and Low-Level Laser Therapy (LLLT) are framed as an integrated “Rapid Recovery & Safety Protocol”—a pathway designed to support tissue recovery, comfort, and overall healing quality rather than a superficial add-on. The underlying idea is straightforward: better tissue environment can support better recovery behavior.
How HBOT Supports Healing (Oxygenation, Inflammation, Tissue Recovery)
HBOT involves breathing oxygen in a pressurized environment. The recovery rationale is to support tissue oxygenation during a period when inflammation and healing demands are elevated. When used appropriately in a medical protocol, the goal is to support:
- Tissue recovery efficiency: optimizing the healing environment
- Inflammation control: supporting the body’s recovery response
- Overall comfort trajectory: helping some patients feel “back to baseline” sooner
In a recovery-first framework, HBOT is less about a single session and more about integrating supportive care at the time window when tissues are actively remodeling.
How LLLT Supports Healing (Cellular Energy, Comfort, Skin Quality)
LLLT (often referred to as “cold laser”) is used in some recovery protocols to support cellular-level responses associated with tissue repair. From a patient-centered perspective, the goals typically include:
- Comfort support: improving how recovery feels in the early phase
- Swelling management support: assisting the body’s return toward baseline
- Skin and tissue quality support: helping the treated area settle smoothly over time
For an expert patient, the value is not a promise of “instant results.” It’s a structured attempt to make recovery more efficient and less disruptive—especially in the first two weeks when swelling and sensitivity can fluctuate.
Who Benefits Most from a Recovery Protocol (Risk Profiles + Goals)
Not every patient needs the same level of recovery support. A protocol approach may be most valuable for patients who:
- Want to minimize downtime and return to daily life with fewer recovery “swings”
- Have a higher swelling tendency or a demanding schedule that makes recovery planning critical
- Prefer a structured, medically supervised pathway rather than “wait and see” recovery
Recovery technologies are not magic. But when they are positioned as part of a disciplined care pathway—rather than a marketing feature—they can align well with the expert patient’s mindset: reduce uncertainty, support predictable healing, and prioritize safety and tissue quality.
Next, we’ll cover risks and complications with full transparency—then explain how risk is reduced through screening, technique, monitoring, and structured postoperative follow-up.
We use advanced Hyperbaric Oxygen Therapy (HBOT) to minimize downtime and supercharge your healing process. Safety is our #1 promise.
Risks, Complications, and How They’re Managed
Any surgery—even when performed under local anesthesia with twilight sedation—comes with risk. A trustworthy provider doesn’t minimize this; they explain the risk profile clearly, outline prevention strategies, and tell you what “normal” looks like versus what requires urgent attention. In gynecomastia surgery, the most meaningful safety advantages come from disciplined candidate selection, precise technique, and structured follow-up—not from marketing language.
Early Risks: Hematoma, Seroma, Infection, Contour Irregularities
Hematoma (a collection of blood under the skin) is one of the more urgent early complications in chest surgery. It’s uncommon, but important because it can affect both comfort and results. Warning signs may include rapid swelling, escalating pain, firmness that worsens quickly, or asymmetric tightness. A serious hematoma may require prompt evaluation and, in some cases, intervention.
Seroma (a collection of fluid) can occur as the body responds to tissue movement and healing. It may feel like sloshing or a soft, shifting pocket. Some seromas resolve with compression and time; others may require drainage in a clinical setting. This is one reason compression and early follow-up matter—early identification helps prevent prolonged swelling and contour distortion.
Infection is typically uncommon when sterile technique and aftercare are followed. Signs can include increasing redness, warmth, fever, or drainage with an unpleasant odor. Providers should give you clear thresholds for when to contact the team rather than leaving you guessing.
Contour irregularities can appear early because swelling is rarely uniform. A chest can look “lumpy,” “puffy,” or uneven in the first weeks, especially around the areola. The key is time: early contour is not mature contour. Persistent irregularities after the maturation window are a separate conversation and may relate to tissue behavior, scar remodeling, or technique-specific factors.
Late Risks: Scar Quality, Nipple Sensation Changes, Asymmetry
Late-stage concerns are usually about aesthetics and tissue behavior rather than acute medical safety, but they are still important.
- Scar quality: Most gynecomastia scars are designed to be discreet, but scar behavior varies. Genetics, skin type, and aftercare can influence whether scars fade smoothly or remain more visible.
- Nipple sensation changes: Some patients notice temporary sensitivity changes as nerves recover. Permanent changes are less common, but possible, and should be discussed honestly during consent.
- Residual asymmetry: Perfect symmetry is not a realistic standard—human anatomy isn’t perfectly symmetric to begin with. The objective is balanced, natural symmetry that looks correct in real life, not only under perfect lighting.
- Under-correction or over-correction: Under-correction can leave persistent puffiness. Over-correction can create a “crater” under the areola. Both are avoidable more often than not when gland handling is conservative and contour blending is precise.
The most “expert patient” approach is to evaluate these risks as probabilities and management plans—not as fears. Ask your provider how often they see these events, what their prevention strategy is, and what their structured follow-up looks like.
What Reduces Risk: Screening, Sterility, Monitoring, Surgical Experience
Risk reduction in awake gynecomastia surgery is a system. The system typically includes:
- Appropriate screening: identifying medication interactions, bleeding risks, and candidates who need additional clearance
- Disciplined anesthesia protocols: safe dosing, monitoring, and clear escalation plans
- Meticulous technique: controlled tissue handling, balanced gland reduction, and smooth contour transitions
- Facility standards and preparedness: reliable monitoring and emergency readiness
- Structured follow-up: early checks that catch hematoma/seroma/infection signals before they become major problems
At AKM Clinic, the philosophy is built around safety-forward planning and modern recovery pathways—designed to help the patient heal efficiently without unnecessary disruption. That same mindset should guide how you judge any provider: not by slogans, but by process quality and safety discipline.
Awake Gynecomastia Results: How to Judge Before/After Photos
Gynecomastia results are not just about “removing tissue.” They’re about how the chest reads in everyday life: in a T-shirt, in a fitted shirt, under overhead lighting at the gym, and when your shoulders roll forward naturally. The best outcomes look unremarkable in the best way—like your chest was always that way. That is the heart of a natural-first approach.
Realistic Expectations: Why Final Results Take Time
It’s normal to want immediate confirmation that the surgery “worked.” But the chest is a swelling-prone area, and gynecomastia correction involves multiple tissue layers settling over time. A realistic timeline looks like this:
- Early phase (first 2–3 weeks): swelling, firmness, and fluctuating areolar appearance are common; the chest can look temporarily uneven.
- Intermediate phase (weeks 4–8): swelling starts to stabilize; the chest begins to look more consistent from day to day.
- Maturation phase (2–6 months): tissue softens, scars improve, and the final contour becomes clearer—especially at the areola border.
Because of this, “final result” conversations too early can be misleading. A high-integrity surgical plan sets expectations upfront so you don’t interpret normal healing as a problem.
“Rejuvenation, Not Alteration”: Building a Natural Male Chest Contour
A natural chest result is not a perfectly flat sheet of skin. A healthy male chest typically has:
- Subtle thickness beneath the areola (not a hollow crater)
- Smooth contour gradients from the sternum to the lateral chest
- Balanced projection that matches your pectoral structure and body frame
Over-aggressive tissue removal can create an “operated” look that is more noticeable than gynecomastia itself. The better target is a chest that looks naturally masculine—consistent with your anatomy and proportionate to your shoulders, arms, and torso.
Surgeon’s Insight: The most convincing results are the ones that don’t announce themselves. A natural-first plan aims for a chest contour that looks right in real life—under normal lighting, normal posture, and normal movement—rather than chasing an artificial “perfect flatness.”
How to Read Before/After Photos (Lighting, Posture, Timeline)
Before/after photos can be informative—but only if you know how to interpret them. When evaluating results (for any provider), use this checklist:
- Lighting consistency: overhead lighting can exaggerate shadows and make the “after” look sharper than it is.
- Posture and shoulder position: shoulders rolled forward can make the chest look fuller; a chest pushed up can make the “after” appear more dramatic.
- Time point: photos at 2–4 weeks are not “final.” Look for mature timelines when possible.
- Areola detail: focus on areolar projection and the transition zone around it—not only the overall chest size.
- Multiple angles: side and oblique views reveal contour quality better than straight-on photos alone.
Finally, measure results against your own anatomy. A natural outcome on a lean athletic frame may look different than a natural outcome on a broader or higher-body-fat frame. The best provider is the one who explains what “natural” looks like on you—not the one who shows a one-template gallery.
Next, we’ll get practical: what cost and value really mean for awake gynecomastia surgery, how to compare like-for-like pricing, and how to avoid hidden cost traps when evaluating providers.
Our philosophy is “Rejuvenation, Not Alteration.” Discover how our surgeons achieve subtle, revitalized results that honor your unique beauty.
Awake Gynecomastia Costs: US vs. Turkey (Value-Based, Not “Cheap”)
Cost is often where research becomes emotionally loaded—especially when you discover how wide the pricing spread can be across providers and cities. The most useful way to evaluate cost is not to chase the lowest number; it’s to compare like-for-like medical value: the surgical plan, anesthesia strategy, facility standards, recovery support, follow-up structure, and what’s actually included. For the expert patient, “value” means predictable outcomes, safety discipline, and transparency—without hidden cost traps.
Why US Pricing Is Higher (Overhead, Facility Costs, Insurance Structure)
In premium US markets (for example, major coastal cities), gynecomastia surgery pricing is typically influenced by:
- Higher facility and staffing overhead (OR costs, anesthesia staffing, compliance costs)
- Higher malpractice and operational expenses associated with metro medical environments
- Bundled vs. unbundled billing (surgeon fee may not include anesthesia, garments, medications, or follow-ups)
- Market pricing dynamics in well-known aesthetic hubs
This doesn’t automatically mean “better quality”—it often reflects the economics of operating in a high-cost healthcare environment. That’s why a rational comparison should focus on what you’re actually receiving, not only on the headline price.
What an All-Inclusive Model Typically Covers (Transparency Checklist)
All-inclusive care models can reduce uncertainty by bundling the most common costs into a single, predictable structure. When comparing providers, use this checklist to confirm what “included” really means:
- Surgeon’s fee and procedural planning
- Anesthesia plan (local + twilight sedation vs general) and professional monitoring
- Facility fees (where the procedure is performed and what standards apply)
- Compression garment(s) and postoperative dressings
- Medications used immediately post-op (as applicable)
- Follow-up visits in the early recovery window
- Structured remote follow-up for international patients
In Istanbul, the value proposition many international patients seek is the ability to access a premium level of care—often with a more predictable total cost—because operational expenses differ from those in high-overhead US cities. The key is to ensure the value difference comes from economics, not compromises in safety or standards.
| Comparison Factor | Typical Unbundled Model (Common in US Markets) | All-Inclusive Model (Common for International Packages) |
|---|---|---|
| Pricing transparency | May require multiple quotes (surgeon + anesthesia + facility) | Often consolidated into one predictable total |
| Post-op essentials | Garments/meds may be separate line items | Often included or pre-arranged |
| Logistics support | Patient coordinates many details independently | Transfers/hotel coordination often structured (varies) |
| Follow-up structure | Local visits may be easier; remote follow-up varies | Often formalized with remote check-ins for travelers |
| Main risk to watch | Hidden add-ons and incomplete quotes | Ambiguity about standards, facility level, and revision policy |
Hidden Costs to Watch For (Flights, Garments, Meds, Revisions, Time Off)
Hidden costs are where “cheap” becomes expensive. When evaluating any provider—local or international—confirm these points:
- Is anesthesia included? If you’re choosing awake surgery, confirm whether twilight sedation and monitoring are included or billed separately.
- Are garments included? Many patients need a compression garment; sometimes more than one size over the recovery course.
- What is the follow-up structure? How many visits are included? What happens if swelling/seroma concerns appear?
- What is the revision policy? While most patients don’t need revision, you should understand how it is handled if needed.
- Time cost: time off work, training pause, travel days, and recovery variability.
A rational cost evaluation asks: “What is the total cost of a safe, predictable result?”—not “What’s the lowest advertised number?”
Get a 100% transparent, all-inclusive quote tailored to your needs. No hidden fees—just world-class care at an accessible price.
How to Choose the Right Surgeon and Facility (A Verification Checklist)
Awake gynecomastia surgery can be an excellent option—but only when it’s performed in a medically disciplined setting. The difference between a smooth, predictable experience and a stressful one often comes down to provider selection: credentials, facility standards, anesthesia monitoring, and the quality of planning. This section is designed to help you verify what matters, not just what sounds impressive.
Credentials That Matter: Board Certification and Specialized Training
Start with credentials and scope. Gynecomastia surgery is a contouring procedure that demands aesthetic judgment and technical control. When evaluating surgeons, look for:
- Recognized board certification and a track record in aesthetic body contouring
- Documented experience with gynecomastia cases (including gland-dominant and mixed cases)
- Comfort with anesthesia strategy selection (awake/local + sedation vs general, and clear explanations of why)
Credentials alone aren’t enough, but they are a baseline filter. The next filter is process quality.
Facility Standards: Accreditation, Sterility Systems, Monitoring
“Awake” does not mean “casual.” A high-standard setting should demonstrate:
- Reliable patient monitoring throughout the procedure (especially if twilight sedation is used)
- Strong sterility protocols and a controlled operative environment
- Emergency readiness appropriate for any anesthesia-supported procedure
In AKM Clinic’s model, the emphasis is on structured care pathways and safety-forward planning—principles that should exist regardless of geography. When comparing providers, ask direct questions about monitoring, protocols, and who is responsible for each part of care.
Consultation Quality: Plan Clarity, Risk Transparency, Photo Analysis
A strong consultation is one where the surgeon can explain the “why,” not just the “what.” You should leave with clarity on:
- Your tissue diagnosis (fat-dominant, gland-dominant, or mixed)
- The proposed technique (lipo, excision, combined) and how areolar contour will be managed
- Anesthesia rationale (why awake is suitable—or why general is safer for your case)
- Risks in plain language and exactly how the team manages early complications (hematoma/seroma)
- Recovery timeline specific to your lifestyle and training goals
If a provider cannot explain these points clearly, you’re not being given a plan—you’re being given a pitch.
Perform your surgery with confidence. Meet our European Board Certified surgeons with over 2,000 successful facial surgeries.
The Medical Journey for International Patients
If you’re traveling for awake gynecomastia surgery, the medical plan should be supported by a logistics plan that reduces stress—not adds it. International care works best when the journey is structured: remote assessment, clear scheduling, coordinated transfers, and defined follow-up milestones. The goal is to protect recovery quality while you’re away from home.
Remote Assessment and Personalized Planning
The journey typically begins with a remote evaluation. In a serious model, this step is not just collecting photos—it’s building a plan. Key elements may include:
- Photo/video review to estimate tissue type and asymmetry pattern
- Medical history screening to assess anesthesia appropriateness
- Preliminary surgical strategy (lipo vs excision vs combined) and recovery timeline planning
At AKM Clinic, international planning is structured to reduce uncertainty and organize the patient experience into clear steps—from initial review to post-op follow-up—so patients can make decisions with information rather than guesswork.
In-Country Schedule: Transfers, Pre-Op, Procedure, Follow-Ups
Once in Istanbul, a structured schedule usually includes:
- In-person confirmation consultation and pre-op verification
- The procedure day with a defined anesthesia plan and monitoring
- Early post-op check(s) to ensure swelling behavior is normal and the garment is fitted correctly
- Clear discharge instructions (medications, showering, activity, warning signs)
For the expert patient, the important question is: “What happens if something is unclear on day 2?” A strong system provides direct access and a defined pathway for evaluation rather than leaving you to self-diagnose.
Returning Home: Virtual Follow-Up at Key Milestones
International care must not end at the airport. A well-run program typically includes remote check-ins at key healing phases (for example, early swelling phase and later maturation phase). This allows the clinical team to:
- Confirm what is normal (swelling fluctuations, firmness, temporary asymmetry)
- Identify early issues that may need local evaluation (e.g., suspected seroma)
- Guide scar and contour care as healing progresses
Traveling for surgery should feel organized. When it is structured properly, it becomes a controlled medical journey rather than a medical gamble.
Frequently Asked Questions: Awake Gynecomastia Surgery
If you’re researching awake gynecomastia surgery, your questions are usually practical and safety-driven: “Will I feel pain?”, “Is local anesthesia dangerous?”, “How long is recovery?”, and “How do I know if I’m a candidate?” The answers below are written to be direct, medically grounded, and easy to skim—without oversimplifying what matters.
Are you awake during gynecomastia surgery under local anesthesia?
Yes—if your procedure is performed under local anesthesia, you are technically awake in the sense that you are not fully unconscious. However, many patients choose twilight sedation on top of local anesthesia, which often makes you feel deeply relaxed and drowsy. In that case, you may have little awareness of time passing and minimal memory of the procedure, while still avoiding the full depth of general anesthesia.
What does twilight sedation feel like?
Most patients describe twilight sedation as a calm, “floaty” state. You may feel sleepy and relaxed, and you may drift in and out of light sleep. You’re typically able to respond if spoken to, but you’re not in a fully alert, anxious state. The experience varies based on dosage and your sensitivity, which is why it’s important that sedation is professionally monitored and tailored to your comfort needs.
Do you feel pain with twilight sedation?
The goal of awake gynecomastia surgery is that you should not feel sharp pain in the surgical area. Comfort is achieved by local anesthesia (numbing) and often supported by tumescent technique (which enhances comfort across the treatment zone). Twilight sedation is an added layer that reduces anxiety and awareness. Some patients feel pressure or movement, but pain should be controllable—and the team can reinforce anesthesia if needed.
Is local anesthesia dangerous?
Local anesthesia is widely used in medicine and is considered safe when administered within appropriate dosing limits and with proper monitoring. Like any medication, it has risks—especially if dosing protocols are ignored, interactions are missed, or patient selection is poor. A safety-forward process includes pre-op screening, strict dosing protocols, and continuous monitoring (particularly if sedation is used).
Can local anesthesia kill you?
This question reflects a real safety fear. Serious, life-threatening reactions to local anesthesia are uncommon, especially in appropriate candidates and in professional settings with proper dosing and monitoring. The practical takeaway is not “no risk”—it’s that risk is minimized through medical screening, safe dosing, continuous observation, and facility preparedness. If you have cardiac issues, medication concerns, or a history of anesthesia reactions, discuss this in detail during consultation.
Gynecomastia surgery: local or general anesthesia—what’s safer?
“Safer” depends on your anatomy, your medical profile, and procedure complexity. Awake surgery (local anesthesia with optional twilight sedation) can be an excellent option for many mild-to-moderate cases because it avoids full unconsciousness and often supports a smoother post-op “feel.” General anesthesia may be a better choice for more extensive cases, complex revisions, or when deeper comfort is medically or psychologically appropriate. The best provider is the one who explains why a specific anesthesia plan fits your case rather than pushing a one-size-fits-all approach.
How long is recovery after awake gynecomastia surgery?
Many patients return to desk work and light daily activity within about 1–2 weeks, depending on the extent of surgery and personal healing response. Swelling and firmness typically improve steadily, but the chest can continue “settling” for several months. Most patients can gradually return to training later in recovery under surgeon guidance, with the understanding that contour maturation continues as tissues soften and scars evolve.
Will I need drains—and when can I fly?
Drain use varies by technique, tissue volume, and surgeon preference. Some cases use drains to reduce fluid buildup risk, while other cases can be managed without drains through technique and compression strategy. Flying depends on your recovery stability and your surgeon’s protocol. For international patients, the safest plan is one that includes a defined post-op check window before travel, plus remote follow-up milestones after you return home.
Will scars be visible—and where are the incisions?
Incision placement depends on whether your case requires liposuction only, gland excision, or a combined approach. When gland removal is needed, incisions are often designed to be discreet and strategically placed to reduce visibility in normal lighting and distance. Scar visibility is influenced by your skin type, genetics, aftercare, and time—scars typically look more noticeable early and improve as they mature.
How much does awake gynecomastia surgery cost?
Pricing varies widely based on region, facility standards, anesthesia strategy, technique complexity (liposuction vs excision vs combined), and what’s included (garments, medications, follow-ups, logistics). A smart comparison focuses on total cost and total value rather than a single headline price. If you’re comparing US city pricing to international options, verify inclusion details carefully—especially anesthesia, facility level, compression garments, follow-up structure, and revision policy transparency.
Awake Gynecomastia: Patient Stories
Awake Gynecomastia Surgeons
Awake Gynecomastia Cost in Turkey
Starting from $3700
* There are no hidden fees or unexpected charges.
- Your Personalised Awake Gynecomastia Procedure
- All Specialist Surgeon & Anesthesia Fees
- All Pre-Op Tests & Post-Op Check-ups
- 5-Star Hotel Accommodation (incl. breakfast)
- All Private VIP Airport & Clinic Transfers
- 24/7 Dedicated Patient Coordinator & Translation Services
Awake Gynecomastia: A Cost Comparison
| City | Cost |
|---|---|
| Austin, TX | $9,000 |
| New York, NY | $12,500 |
| Chicago, IL | $7,250 |
| Los Angeles, CA | $11,500 |
| Miami, FL | $5,800 |
Awake Gynecomastia: Patient Reviews
Jammal Canada
I have had face and neck lift with AKM Clinic they have been so good to me and my operation went so smoothly🥰 i would like to thank my doctor here and also to the team 💐

Ava Canada
Thank you AKM Clinic for giving me my confidence back! Had facelift + temporal lift 3 months ago and the outcome is already stunning. Special thanks to Hande!

Jakayla USA
Had a deep plane facelift and lower eyelid procedure at AKM Clinic 7 months ago. The results are fantastic - very subtle and natural. I didn’t expect the entire experience to be so comfortable. Hande managed everything and kept in contact even after I returned to USA. I’m beyond pleased with the outcome and the care I received. Would do it again in a heartbeat!

Barbara United Kingdom
It has been 4 months since my surgery. Everything is great, The most important thing is l love the way l look, l look exactly how l wanted. Meaning l look natural, just almost 40 years younger. I pulled Facebook - majority voted 37ys. I also had face, neck, chest, and hands CO2 laser. My skin is flawless.

Lisa Canada
I had a face, neck and arm lift at AKM. I’m just over 4 weeks post and couldn’t be happier with the results. The entire experience was wonderful! My coordinator, Khadija made me feel comfortable from beginning to end! I highly recommend AKM and will definitely go back for other procedures!

Julie USA
I am beyond grateful I went with AKM Clinic for my deep plane face and neck lift, upper eyelid, and co2 laser. Dr. Akif has magic hands and my results are truly incredible! I came from the US and assistant Emine was the best in assuring every detail was coordinated and communicated with me beyond my expectations every step of the way. 10 out of 10 to the entire team! I couldn’t be more pleased!

Ready to Start Your Own Transformation Journey?
Join the 2,000+ patients who trusted Dr. Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, revitalized you begins with a simple, no-obligation conversation. Contact us today from the USA for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. No hidden fees.
#2: Secure Your Date & VIP Booking
Once you're ready, our dedicated patient coordinators will help you secure your procedure date. We'll handle all your bookings, including your 5-star hotel and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you'll meet your specialist surgeon to finalise the details for your "natural, subtle, and revitalized" new look.













