Awake Tummy Tuck in Turkey




Awake Tummy Tuck: Quick Facts
Procedure Time
Anesthesia
Recovery Time
Hospital Stay
Back to Work
Awake Tummy Tuck Results: Before and After
An awake tummy tuck is a form of abdominoplasty performed with local anesthesia and, in many cases, twilight-style sedation—designed to help the right candidate avoid (or reduce reliance on) full general anesthesia. For the “expert patient,” the appeal is rarely about “being brave.” It’s about control: understanding the anesthesia spectrum, minimizing physiologic stress where appropriate, and building a recovery plan that prioritizes safety, comfort, and predictable outcomes.
That said, it’s essential to be clear: a tummy tuck is still a major body contouring procedure. “Awake” does not mean “no pain,” “no downtime,” or “no risk.” It means the surgical and anesthesia plan may be tailored so that you can remain comfortable and protected without requiring a fully unconscious anesthetic—when your anatomy, health profile, and procedure scope allow it.
This guide explains what a tummy tuck really changes anatomically, what “awake” means medically (and what it does not), and how to think like a clinician when evaluating candidacy, technique, and risk.
Table of Contents
Share your photos and medical history to receive a personalized assessment from our European board-certified facial surgery team.
What Is a Tummy Tuck, Really?
A tummy tuck (abdominoplasty) is often oversimplified as “tightening the stomach.” Medically, it’s a procedure that addresses excess skin, soft tissue laxity, and—when indicated—abdominal wall separation (commonly after pregnancy or major weight change). The goal is not a different body; it’s a more stable, smoother abdominal contour that matches your natural frame.
The Anatomy: Skin, Fat, Fascial Layers, and the Abdominal Wall
To understand outcomes (and scars), it helps to understand what’s being treated:
- Skin envelope: The outer layer that can remain stretched even after weight loss.
- Subcutaneous fat: The layer under the skin; sometimes selectively reduced with liposuction, depending on safety and goals.
- Fascial layer (the “inner girdle”): A strong connective tissue layer over the abdominal muscles. This is often what surgeons tighten when patients describe “muscle tightening.”
- Abdominal muscles: The rectus muscles themselves usually aren’t cut; when “repair” is done, it typically involves tightening the supportive fascia rather than changing the muscle tissue.
This matters because the procedure is not simply “pulling skin.” The most satisfying results come from aligning the correct layer with the correct problem—skin laxity, fascial laxity, or both—while preserving a natural contour.
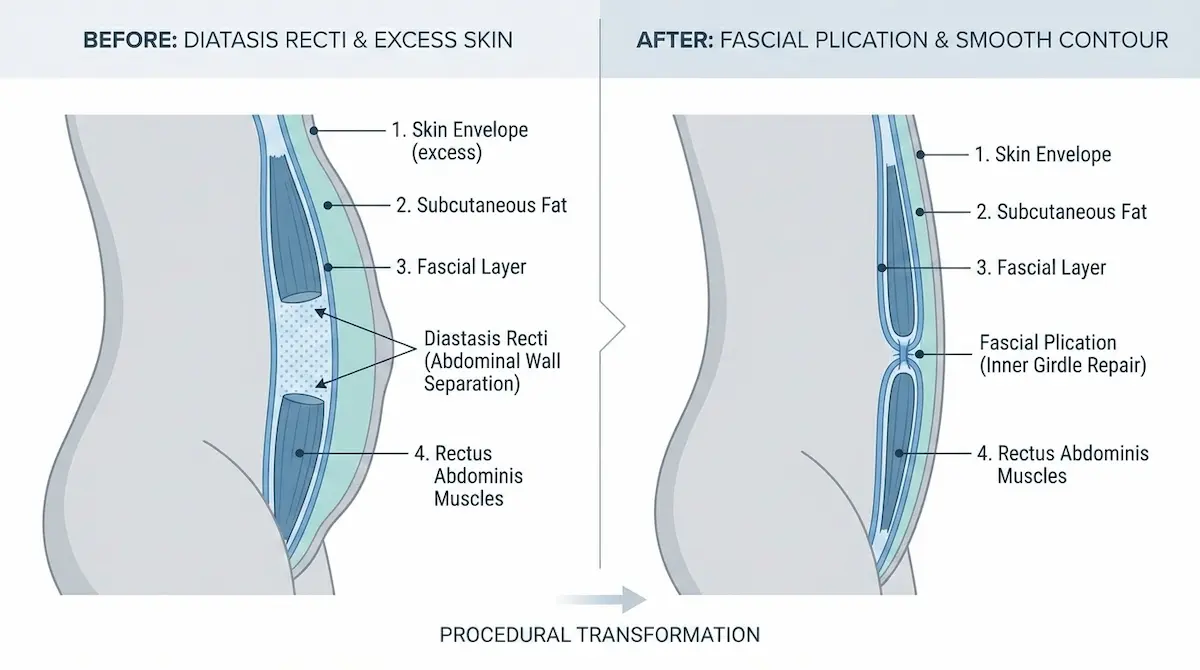
What a Tummy Tuck Can vs. Can’t Do
What it can do:
- Remove or reduce lower abdominal skin redundancy (the “apron” or overhang).
- Improve contour irregularities caused by lax skin and soft tissue.
- Flatten the abdomen when laxity is the primary issue (especially when combined with appropriate core/fascial tightening).
- Improve the look of some stretch marks if they are located on skin that is removed (commonly below the navel).
What it can’t reliably do:
- Act as a weight-loss procedure or substitute for long-term weight stability.
- Guarantee a “six-pack” appearance (that’s anatomy- and lifestyle-dependent).
- Eliminate all stretch marks (many remain, especially those above the resection line).
- Prevent future laxity if pregnancy or major weight fluctuation occurs after surgery.
Mini vs. Full Abdominoplasty: Core Conceptual Differences
Many patients search “what is a mini tummy tuck” and assume it’s simply a smaller scar. In reality, it’s a different scope of correction.
- Mini tummy tuck: Targets the lower abdomen (below the navel). Best for mild-to-moderate skin laxity with limited need for broader tightening.
- Full tummy tuck: Addresses the entire abdominal skin envelope and commonly involves navel repositioning and more comprehensive tightening when indicated.
Choosing between them is less about what you “prefer” and more about what your anatomy requires. The most common cause of dissatisfaction is selecting a smaller procedure that cannot realistically correct the true distribution of laxity.
Our surgery dates fill up quickly due to high international demand. Secure your consultation today to plan your ideal travel dates.
What Does “Awake” Mean in Surgery?
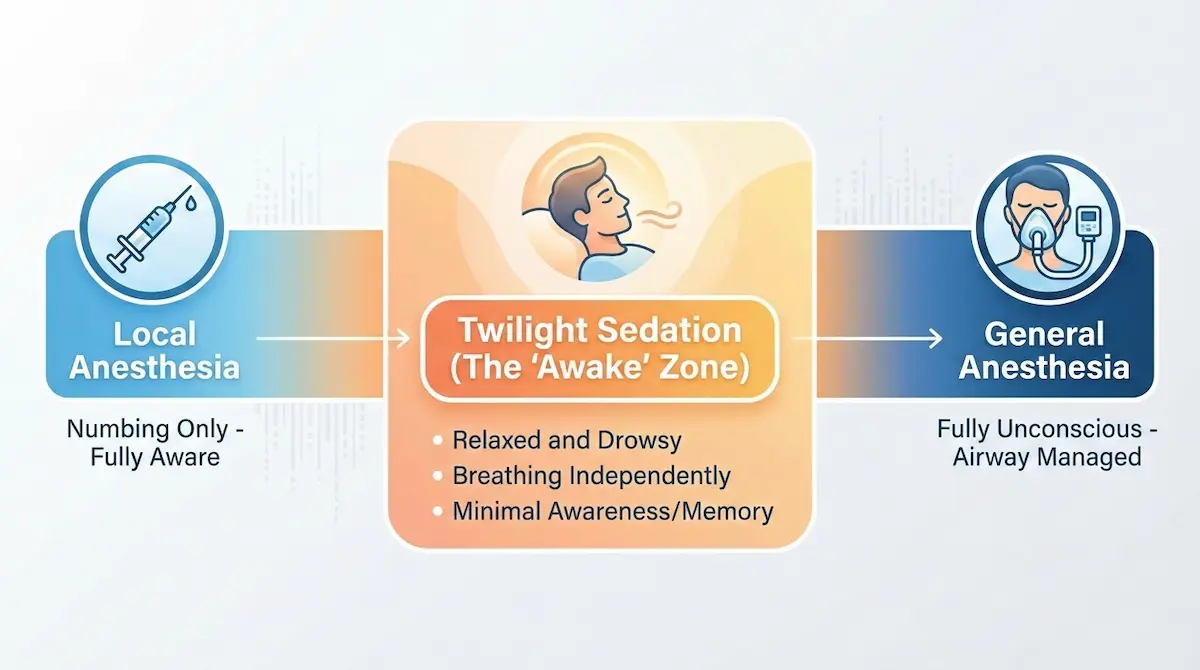
“Awake surgery” is a patient-friendly phrase, but clinically it refers to an anesthesia strategy—not a single fixed experience. Most “awake” body procedures exist on a continuum: from purely local anesthesia (numbing only) to local anesthesia with IV sedation (often described as “twilight”), where you may be relaxed, drowsy, and have limited memory—while still avoiding a fully general anesthetic.
Local Anesthesia, Tumescent Techniques, and Sedation: The Continuum
In practical terms, an awake tummy tuck plan may include:
- Local anesthesia: Numbing medication placed strategically to reduce pain in the surgical field.
- Adjunct techniques: Methods that expand and numb tissue planes to improve comfort and reduce bleeding in selected contexts.
- IV sedation (“twilight”): Medication to reduce anxiety and awareness, managed carefully so you remain stable and comfortable.
The right plan is individualized. It depends on the extent of correction, your medical history, anxiety profile, pain tolerance, and whether additional procedures are being combined.
Awake Surgery Benefits: What’s Realistic, What’s Marketing
Potential benefits that may be realistic for the right candidate include:
- Avoiding general anesthesia when appropriate: This can be meaningful for patients with significant anxiety around being fully unconscious or for those seeking a different recovery experience.
- Reduced post-anesthesia “hangover” for some patients: Less grogginess or nausea can occur, depending on the exact medications used.
- More controlled transitions: Some patients value a smoother wake-up experience and earlier return to baseline alertness.
What awake surgery does not automatically mean:
- No pain (comfort still depends on technique and anesthesia quality).
- No downtime (tummy tuck recovery is still measured in weeks, with scar maturation over months).
- Risk-free surgery (all abdominoplasty variants carry real complication profiles).
For the expert patient, the key is not “awake vs asleep” as a slogan—it’s whether the anesthesia plan matches the procedure’s intensity and your personal risk profile.
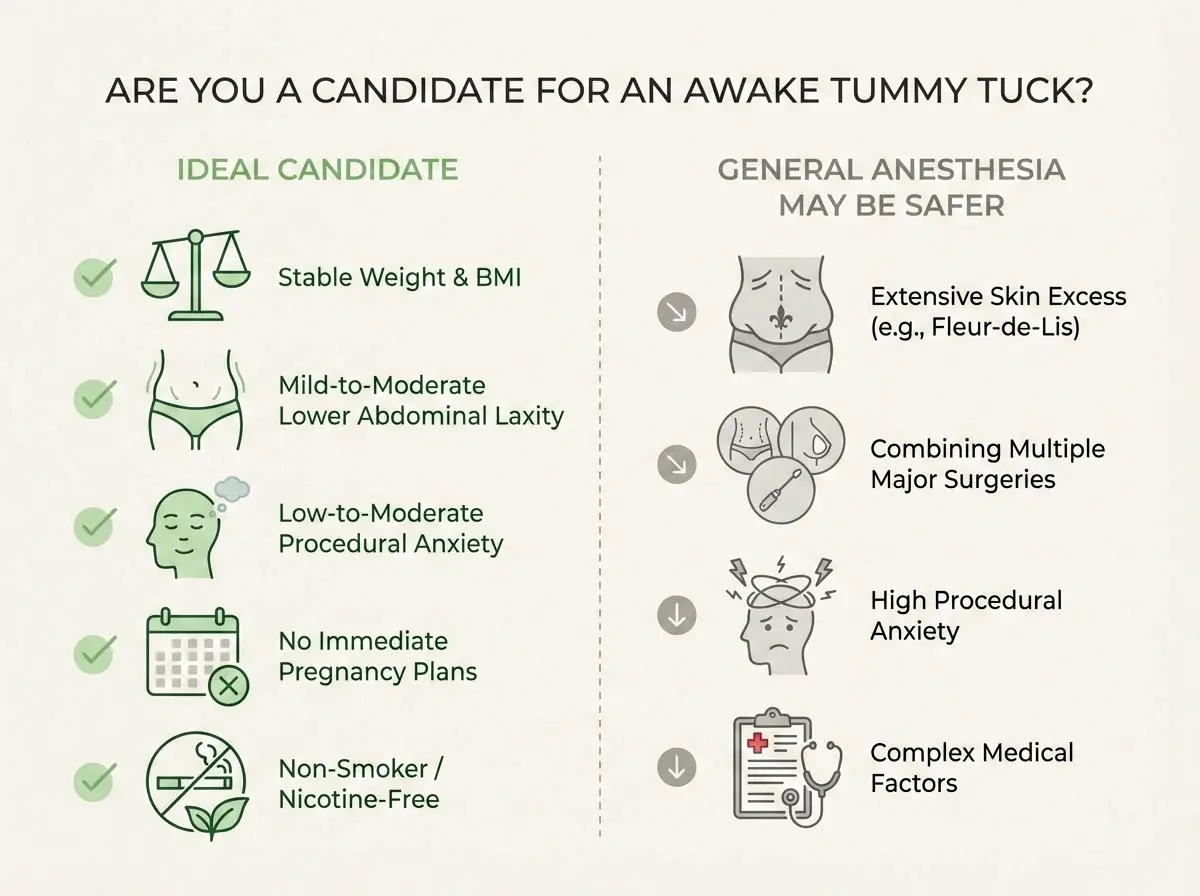
Who Is Not a Candidate for an Awake Approach?
An awake tummy tuck is not ideal for everyone. Common reasons a surgeon may recommend general anesthesia (or a different procedure plan) include:
- Very extensive correction needs: Large skin excess, complex revision cases, or prolonged operative time.
- Medical factors: Conditions where airway control, ventilation, or deeper anesthesia control is safer.
- High anxiety that cannot be managed safely with light sedation: If stress responses increase risk, “awake” may be counterproductive.
- Multiple major procedures in one session: Combining operations can change the safest anesthesia choice.
The safest plan is the one that a qualified surgical team can execute predictably—while keeping you stable, comfortable, and monitored appropriately from start to finish.
Ideal Candidate For Awake Tummy Tuck
The best awake tummy tuck results don’t come from “wanting it badly enough.” They come from the right match between your anatomy, your health profile, and the realistic scope of correction. A surgeon’s job is to identify which problems are structural (abdominal wall laxity), which are tissue-based (skin redundancy), and which are lifestyle-dependent (weight stability, activity level). Your job is to be brutally honest about goals, timeline, and risk tolerance—because abdominoplasty is elective, but safety is not.
Weight Stability, BMI, and Skin Quality
A tummy tuck is most predictable when your weight is stable. If your weight is still trending downward (or fluctuating), the skin envelope may keep changing, which can compromise how long results last and increase the likelihood of residual laxity.
- Weight stability: Many surgeons prefer a stable weight for several months before surgery.
- BMI considerations: BMI isn’t a moral score—it’s a risk and predictability variable. Higher BMI can increase anesthesia complexity, wound healing demands, and complication risks such as seroma or delayed healing.
- Skin quality: Elasticity, striae (stretch marks), and prior scars influence how smoothly skin redrapes and where tension concentrates.
For the “expert patient,” the key question is not “Can you do it?” but “Can you do it with a risk profile and scar strategy I’m willing to accept?”
Diastasis Recti & Core Function: When Muscle Repair Matters
Many patients describe a “pooch” that persists despite training. If this is caused by diastasis recti (separation of the rectus muscles along the midline), a tummy tuck may include abdominal wall tightening (often plication of the fascial layer) to restore a firmer core silhouette.
It’s important to separate three concepts:
- Fat distribution: Often best addressed with lifestyle changes and/or liposuction in select cases.
- Skin excess: Only surgery removes true redundant skin.
- Structural laxity (diastasis): Requires a surgical tightening approach when clinically indicated.
If core symptoms matter to you—back discomfort, reduced stability, bulging with strain—bring that into the consultation. A credible plan explains whether tightening is necessary, what it changes, and what it can’t change.
Smoking, Pregnancy Plans, Medical Conditions & Pre-Op Screening
Risk isn’t abstract in abdominoplasty. It shows up in blood flow, wound healing, clot risk, and infection risk. The most common avoidable reasons for complications include nicotine exposure, uncontrolled medical issues, and insufficient pre-op planning.
- Nicotine (including vaping): Nicotine constricts blood vessels and impairs healing. This can raise risks of delayed healing and skin compromise.
- Diabetes and metabolic health: Poorly controlled blood sugar can increase infection and healing problems.
- History of clotting: Past DVT/PE, strong family history, or certain medications can change prevention strategies.
- Pregnancy plans: A tummy tuck does not “prevent” pregnancy, but pregnancy can stretch repaired tissues and skin again. If pregnancy is planned soon, delaying surgery may be the more rational choice.
For awake tummy tuck specifically, candidacy also includes how you handle procedural stress. If anxiety causes spikes in blood pressure, rapid breathing, or panic, it can complicate an “awake” plan—sometimes making a deeper anesthetic approach safer.
Answer a few quick questions about your concerns, health, and goals to learn which treatment options may suit you best.
Types of Tummy Tuck
“Tummy tuck” is an umbrella term. The right type is determined by where your laxity lives (upper abdomen, lower abdomen, sides), how much skin must be removed, and whether the incision needs to extend to achieve a natural contour. A responsible surgical plan chooses the smallest procedure that can reliably achieve your goal—not the smallest scar at all costs.
Mini Tummy Tuck
A mini tummy tuck focuses primarily on the lower abdomen (typically below the navel). It may be appropriate when:
- Skin excess is mild-to-moderate and concentrated low on the abdomen.
- There is minimal upper abdominal laxity.
- Any needed tightening is limited and anatomically appropriate for the scope.
Because the correction range is smaller, a mini tummy tuck can have a shorter operative scope. However, it’s not “minor surgery.” If your laxity extends above the navel, a mini can under-correct and leave persistent upper abdominal looseness.
Extended Tummy Tuck
An extended tummy tuck expands the correction laterally to address laxity that extends toward the flanks/hips. It may be considered when:
- Skin and soft tissue laxity continues beyond the central abdomen.
- You want smoother transitions between abdomen and waist/hip contour.
- There is significant lower body skin redundancy after weight loss.
Extended approaches can improve contour harmony, but they typically involve longer incisions and a larger healing surface—factors that must be weighed carefully, especially in “awake” planning.
Fleur-de-Lis Tummy Tuck
A fleur-de-lis tummy tuck is a more specialized approach commonly considered after major weight loss, where laxity exists in both vertical and horizontal directions. It can tighten the abdomen more comprehensively by addressing:
- Horizontal excess (loose skin across the width of the abdomen)
- Vertical excess (loose skin from top to bottom)
The trade-off is scarring: fleur-de-lis typically adds a vertical scar component. The decision is deeply personal and should be made with a clear understanding of the scar pattern, clothing considerations, and long-term scar maturation timeline.
Reverse Tummy Tuck
A reverse tummy tuck targets laxity in the upper abdomen (above the navel) and is less common than traditional lower-abdominal approaches. It may be considered when:
- Upper abdominal skin looseness is the dominant concern.
- Lower abdominal skin is relatively acceptable.
- A scar strategy near the inframammary region (beneath the breasts) is acceptable for your anatomy and goals.
Reverse techniques are not “better” or “worse”—they are location-specific tools. The “best” tummy tuck type is the one that matches your laxity map and scar tolerance.
Clinical note: Many patients actually need a hybrid strategy—such as a full tummy tuck pattern with targeted liposuction, or an extended approach for better waist blending. This is why a consultation should involve a three-dimensional assessment, not a one-size-fits-all recommendation.
Surgical Technique Options That Change Outcomes
Two patients can both say they “got a tummy tuck” and still have wildly different scars, recovery experiences, and long-term contour—because the technique details matter. For an awake tummy tuck in particular, technique choices also influence comfort, operative efficiency, bleeding control, and how smoothly you move through the first few recovery weeks. The goal is not to chase trends (like “drainless” as a buzzword), but to choose a method that matches your anatomy and your risk profile.
Muscle Repair (Fascial Plication) vs. No Repair: How the Decision Is Actually Made
When patients ask for a “tummy tuck with muscle repair,” they are usually describing one of two things: (1) a desire for a flatter abdominal silhouette, or (2) functional symptoms of abdominal wall laxity (bulging, reduced core stability). In most cases, what is tightened is the fascial layer overlying the rectus muscles (often called plication), not the muscle itself.
When tightening is commonly beneficial:
- Diastasis recti confirmed on exam (and sometimes imaging) with visible midline bulge on exertion.
- Post-pregnancy laxity with a widened linea alba and reduced core support.
- Patients whose primary complaint is “I look pregnant after meals” even at a stable weight.
When “repair” may be unnecessary—or less helpful than expected:
- Abdominal prominence driven primarily by visceral fat (fat around organs), which surgery cannot remove.
- Minimal diastasis where the main problem is skin redundancy.
- Patients seeking an extreme “cinched” look that would require unnatural tension (often a setup for discomfort or contour issues).
Expert-patient checklist: Ask your surgeon to explain (a) whether you truly have clinically meaningful diastasis, (b) what layer will be tightened, (c) how tightening changes tension distribution on the incision, and (d) how the plan affects early mobility and discomfort.
Liposuction Integration: When It Helps vs. When It Adds Risk
Patients often assume that adding liposuction to a tummy tuck is always better. In reality, it’s a powerful tool that must be used intelligently. Liposuction can help refine contour transitions—especially at the waist and flanks—but aggressive liposuction in the wrong zones can compromise blood supply to the abdominal skin flap, increasing healing risk.
When liposuction can be a smart complement:
- To improve waist definition and reduce “boxiness,” particularly at the flanks.
- To smooth contour transitions so the abdomen blends naturally into the hips and back.
- When the plan is conservative and respects skin blood supply.
When liposuction may increase risk (or require a staged approach):
- Extensive skin elevation plus aggressive central-abdominal liposuction (higher risk to skin perfusion).
- Revision cases with prior scars that may already alter blood flow patterns.
- Patients with risk factors for delayed healing (e.g., nicotine exposure, poorly controlled diabetes).
Awake-specific note: Combining procedures can extend operative time and increase the “stress load” of surgery. Even when performed safely, longer duration can change what anesthesia strategy is most comfortable and appropriate. The best plan is the one that keeps the procedure within a scope your team can manage predictably.
Drains vs. Drainless Strategies: What Patients Should Ask
Drain placement is one of the most debated aspects of tummy tuck recovery because drains affect convenience, mobility, and the feeling of “being tethered.” But drains exist for a reason: they reduce fluid accumulation (seroma) by removing inflammatory fluid during the early healing phase. “Drainless” approaches aim to reduce or eliminate drains by using internal fixation techniques that reduce dead space.
There is no universal “best.” The best approach depends on your tissue characteristics, the extent of dissection, whether liposuction is added, and your surgeon’s method and outcomes.
| Topic | With Drains | Drainless (Internal Fixation) |
|---|---|---|
| Primary goal | Actively remove fluid during early healing | Reduce dead space to limit fluid formation |
| Patient experience | Drain care required; may feel restrictive temporarily | Less external management; may feel “cleaner” recovery |
| Seroma strategy | Continuous drainage lowers accumulation risk during drain period | Relies on technique quality; seroma can still occur |
| Follow-up needs | Drain removal visit(s), output tracking | Close monitoring still required; aspiration may be needed if fluid forms |
| Best fit | Higher-risk fluid formers, larger corrections, or surgeon preference based on outcomes | Selected patients and surgeons with consistent technique-specific results |
Expert-patient checklist: Ask your surgeon:
- What is your seroma rate with drains vs. drainless in cases like mine?
- How do you decide who qualifies for a drainless tummy tuck?
- If fluid develops, what’s the protocol (ultrasound, aspiration, compression, activity changes)?
- How does my plan (mini vs full vs extended, lipo or not, muscle tightening or not) change fluid risk?
Finally, remember that recovery is not only about “comfort.” It’s about protecting blood supply, minimizing tension, and keeping your incision environment stable—because the best scar is the one that heals smoothly without prolonged inflammation.
Awake vs General Anesthesia for Abdominoplasty
For most patients researching an awake tummy tuck, the anesthesia question isn’t philosophical—it’s practical. You’re trying to reduce avoidable risk, protect your recovery experience, and choose a plan you can tolerate physically and mentally. The safest approach is never “awake at all costs” or “general is always best.” It’s the approach that matches your procedure scope, your health profile, and your team’s ability to monitor and respond to changes in real time.
Pros/Cons Matrix: Safety, Nausea, Recovery Experience
Below is a clinical-style comparison that reflects typical trade-offs. Your personal experience may differ based on medications, procedure length, and individual sensitivity.
| Factor | Awake / Local + Sedation (Twilight) | General Anesthesia |
|---|---|---|
| Level of unconsciousness | Often drowsy/relaxed; may be minimally aware; many patients remember little | Fully unconscious, typically with airway management |
| Breathing/airway control | Usually breathing independently (team monitors closely) | Airway is controlled by anesthesia team (ventilation can be managed precisely) |
| Post-op grogginess | Can be lighter for some patients depending on medications used | Can be more pronounced for some patients, especially after longer cases |
| Nausea/vomiting risk | May be lower for some patients; varies by medication choice | Can be higher for some patients; anti-nausea protocols help significantly |
| Procedure scope flexibility | Best for appropriately selected cases; very extensive cases may be less suitable | Often preferred for long, complex, or multi-procedure sessions |
| Comfort during surgery | Depends heavily on technique quality and patient anxiety profile | Typically predictable for patient comfort (you’re fully asleep) |
| Recovery “feel” | Some patients describe a smoother, less disorienting wake-up | Some patients feel more “out of it” initially; varies widely |
Key takeaway: “Awake” can be an excellent option when it’s medically appropriate and expertly executed. General anesthesia remains the right choice in many scenarios—especially when the procedure is extensive or when deeper physiologic control is safer.
Pain Control Plan: What Patients Typically Feel During and After
A credible awake tummy tuck plan includes a concrete pain-control strategy. The goal is not to “tough it out.” The goal is to keep your body calm: stable breathing, stable heart rate, stable blood pressure, and minimal stress response—because stress physiology is not your friend in surgery.
During an awake/twilight tummy tuck:
- Numbing phase: You may feel pressure, vibration, or pushing, but sharp pain should be prevented by proper local anesthesia technique.
- Sedation support: Many patients feel sleepy and detached from the environment. Some drift in and out of light sleep.
- Communication: In a well-run setting, you’re monitored continuously, and comfort can be adjusted in real time.
After surgery (awake or general):
- Tightness and pulling: Especially if abdominal wall tightening is performed. This can feel like strong “core soreness” and tension when standing upright early on.
- Swelling and sensitivity: Normal and expected. The first 1–2 weeks typically feel the most restrictive.
- Movement discomfort: Getting in/out of bed, using core muscles, and standing fully upright can be uncomfortable initially.
How expert teams reduce pain without over-sedating you:
- Prioritizing local anesthesia quality (coverage and timing)
- Using sedation thoughtfully (enough to relax you, not so much that it destabilizes breathing)
- Building a layered post-op plan (scheduled meds early, then tapering; non-drug strategies like positioning, compression, and controlled walking)
One important nuance: if your anxiety is high, “awake” can become uncomfortable—not because of pain, but because stress amplifies sensation. This is why candidacy includes psychology and not just anatomy.
Who Benefits Most From Avoiding General Anesthesia?
Patients often search “is awake surgery safe” because they’re trying to reduce perceived anesthesia risk. In practice, the patients who may benefit most from an awake/twilight approach are those whose:
- Procedure scope is appropriate: Not overly prolonged, not overly complex, and technically suitable for local + sedation.
- Health profile supports it: No red flags that make deeper anesthesia control safer (your surgical team will screen this carefully).
- Recovery priorities include clarity and smoother transitions: Some patients strongly prefer avoiding a “hard wake-up” experience.
- Primary fear is general anesthesia itself: When fear is a barrier to treatment, an awake/twilight plan can be psychologically empowering—if it can be executed safely and comfortably.
Who may be better served by general anesthesia:
- Patients needing an extended, fleur-de-lis, or complex revision tummy tuck
- Patients combining multiple major procedures in one session
- Patients with high anxiety that cannot be managed safely with light sedation
- Cases where the anesthesia team determines that airway/ventilation control is the safer choice
Ultimately, anesthesia choice should feel like a medical decision—because it is one. The “best” plan is the one that balances surgical effectiveness, monitoring reliability, patient comfort, and a recovery pathway you can realistically follow.
Get a clear, day-by-day itinerary covering arrival, surgery, recovery, and fit-to-fly clearance tailored to your schedule.
Step-by-Step: What Happens on Procedure Day
One of the fastest ways to reduce surgical anxiety—especially for patients considering an awake tummy tuck—is to replace vague expectations with a clear, step-by-step timeline. While every surgeon has specific preferences, a high-quality abdominoplasty workflow is surprisingly consistent: pre-op planning, precise marking, controlled tissue handling, meticulous closure, and structured early mobilization. The details of your plan (mini vs full vs extended, muscle tightening vs no tightening, lipo integration, drains vs drainless) determine how long each phase takes and what you’ll feel afterward.

Pre-Op Marking & Surgical Planning
Before any anesthesia begins, most surgeons perform standing markings. This is not cosmetic “scribbling”—it’s an anatomical blueprint that accounts for how your tissue sits with gravity, where skin redundancy truly lives, and how incision placement can be aligned with clothing lines.
- Scar strategy is planned here: The incision pattern is designed based on tissue excess distribution, not just “lowest possible scar.”
- Symmetry is engineered early: Markings guide midline alignment and balanced tension.
- Procedure scope is confirmed: Whether your plan is mini, full, extended, or a specialized variant (fleur-de-lis, reverse) is reconfirmed with your anatomy in real time.
If you’re pursuing an awake/twilight approach, this is also the time to communicate your comfort preferences—music, temperature sensitivity, and what helps you stay calm. A good team treats these as legitimate inputs, because calm physiology is safer physiology.
Incisions, Tissue Tightening, and Umbilical Planning
After anesthesia is initiated and comfort is confirmed, the surgical steps typically follow a structured sequence:
- Incision and tissue elevation: The surgeon accesses the abdominal tissue plane required for the planned correction.
- Abdominal wall tightening (when indicated): If diastasis recti is present and the plan includes tightening, the supportive layer is reinforced to improve contour and stability.
- Skin redraping and resection: Excess skin is removed in a way that balances tension across the closure line—critical for scar quality.
- Navel positioning (full tummy tuck patterns): In a comprehensive abdominoplasty, the umbilicus is managed thoughtfully so the result looks natural rather than “operated.”
Awake-specific insight: You may feel pressure and movement, but sharp pain should be prevented. If you feel pain, the correct response is not “tolerate it”—it’s to inform the team so comfort can be adjusted.
Closure, Dressings, Compression, and First Mobilization
The closure phase strongly influences scar behavior and early recovery. High-quality closure is layered, tension-aware, and designed to protect blood supply. After closure:
- Dressings and garment: A compression garment helps reduce swelling and supports the healing contour.
- Drain management (if used): You’ll be taught how to measure output and keep the area clean.
- Early mobilization: Gentle walking is typically encouraged early (with guidance), because movement helps reduce clot risk and supports circulation.
Most patients are surprised by one thing: the procedure is only half the equation. Your outcome depends heavily on how intelligently you recover—movement, positioning, nutrition, compression compliance, and follow-up monitoring.
Recovery Timeline & Aftercare (Day 1 to 12 Months)
Tummy tuck recovery is often discussed in “weeks,” but healing happens in phases—each with different priorities. In the first phase, your goal is safety: circulation, wound stability, and controlled swelling. In the second phase, your goal is function: mobility, posture normalization, and a gradual return to daily life. In the third phase, your goal is refinement: scar maturation and contour settling. If you judge your results too early, you will almost always overestimate problems that simply need time.
First 72 Hours: Swelling, Walking, Sleep Position, Support
The first three days are usually the most restrictive. You may feel tight, hunched, and cautious with movement—especially if abdominal wall tightening was performed.
- Swelling and tightness: Expected. Swelling is part of normal inflammatory healing.
- Walking: Short, frequent walks are often recommended. The goal isn’t exercise—it’s circulation and clot prevention.
- Sleep position: Many patients do best on their back with knees supported (pillow under knees) to reduce tension.
- Hydration and nutrition: Protein intake supports tissue repair; constipation prevention is an often-overlooked comfort strategy.
What not to do: Overstretching upright too early, lifting heavy objects, or “testing” your incision with sudden movements.
Weeks 1–6: Return to Work, Driving, Exercise Progression
This phase is where expert patients sometimes overestimate their readiness—because pain may improve faster than tissue strength. Your incision and internal repair are still stabilizing even if you “feel okay.”
- Week 1–2: Many patients can do light household activity and short walks; fatigue is common. If drains are used, output typically guides removal timing.
- Week 2–4: Mobility improves. You may stand more upright gradually. Many desk-based patients consider returning to work, depending on comfort and travel demands.
- Week 4–6: Gentle exercise may resume with surgeon guidance. Core-heavy movements are usually delayed longer, especially after tightening.
Driving: Generally depends on comfort, mobility, and being off narcotic pain medications. Your surgeon should provide a clear policy that prioritizes safety.
Compression garments: Often continued during this window to help swelling control and contour stabilization. The “best” wear schedule varies—what matters is consistent compliance with your surgeon’s protocol.
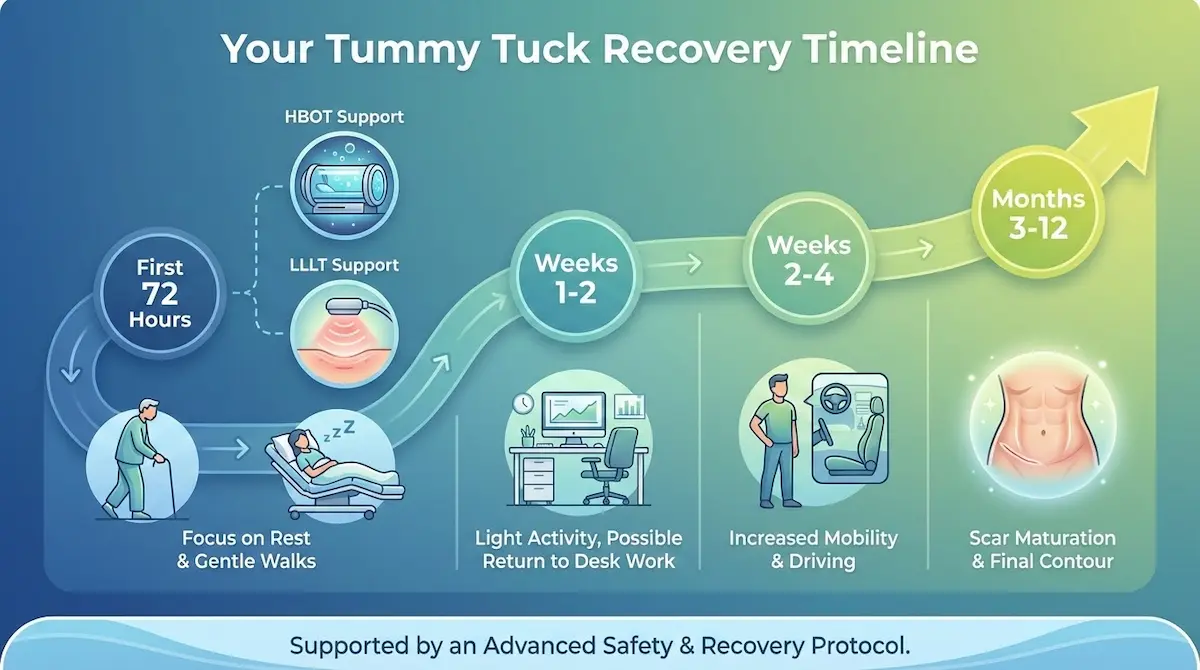
Months 3–12: Scar Maturation, Final Contour, Sensation Changes
At 6–12 weeks, many patients feel “mostly normal,” but final results keep evolving.
- Scar maturation: Scars typically transition from raised/red to flatter and lighter over months. The most important factor is uncomplicated healing in the first few weeks.
- Contour settling: Residual swelling can persist for months, especially later in the day or after activity.
- Sensation changes: Numbness or altered sensation near the lower abdomen is common and often improves gradually, but it can be prolonged.
Judge outcomes at the right timepoints: early healing (2–6 weeks), mid-term contour (3–6 months), and long-term refinement (9–12 months).
Accelerated Recovery & Safety Protocols: HBOT + LLLT as a Structured Aftercare Strategy
Recovery is not only about “waiting.” Many modern surgical programs treat recovery as an active phase where tissue oxygenation, inflammation control, and wound support are systematically optimized. Two adjunct technologies commonly used in advanced recovery protocols are Hyperbaric Oxygen Therapy (HBOT) and Low-Level Laser Therapy (LLLT).
Hyperbaric Oxygen Therapy (HBOT): HBOT involves breathing oxygen in a pressurized environment to increase oxygen delivery to tissues. In post-surgical recovery, the rationale is to support tissue oxygenation during a phase when swelling and healing demands are high. In structured protocols, HBOT may be used as part of a “rapid recovery and safety” strategy focused on:
- Supporting wound healing in the early post-op period
- Helping manage inflammation and swelling
- Enhancing tissue resilience when the body is under repair demands
Low-Level Laser Therapy (LLLT): LLLT is often positioned as a supportive modality aimed at cellular energy pathways and inflammation modulation. When integrated thoughtfully, it may be used to support:
- Swelling reduction and comfort as the early recovery phase progresses
- Soft tissue recovery support as bruising and tightness resolve
- Scar-care strategies in later phases (based on individual protocol)
Important clinical perspective: These modalities are adjuncts—not replacements—for the fundamentals: meticulous surgical technique, stable vitals monitoring, proper compression, early mobility, hydration, nutrition, and consistent follow-up. Used in that context, they can be framed as part of a comprehensive recovery system rather than standalone “machines.”
If you’re evaluating providers, an expert-patient question is: “What is your recovery protocol, session schedule, and monitoring plan—and how do you select which patients benefit most?” The best answer is structured, measurable, and personalized.
We use advanced Hyperbaric Oxygen Therapy (HBOT) to minimize downtime and supercharge your healing process. Safety is our #1 promise.
Risks, Complications, and How to Reduce Them
Every version of abdominoplasty—mini, full, extended, fleur-de-lis, reverse—has real risks. An awake tummy tuck is not a “no-risk” tummy tuck; it’s a different anesthesia strategy that may be appropriate for the right candidate and the right scope. The most responsible way to evaluate safety is to do two things at once: (1) understand the complication profile honestly, and (2) evaluate how your surgeon and facility systematically reduce risk through screening, monitoring, sterile standards, and structured aftercare.
Common Issues: Seroma, Infection, Delayed Healing, and Scar Concerns
Most tummy tuck complications are not dramatic—but they can be frustrating, delay recovery, and affect scar quality if not managed early.
- Seroma (fluid collection): Fluid can accumulate under the skin in the early healing phase. Drains (or drainless internal fixation strategies) exist largely to manage this risk. Seromas are often treatable but can require aspiration and extended compression protocols.
- Infection: Usually treatable when caught early, but prevention (sterile technique, careful wound care, and appropriate follow-up) is the real priority.
- Delayed wound healing: More likely with nicotine exposure, poorly controlled diabetes, high tension closures, or overly aggressive combined procedures. Delayed healing can widen scars and extend downtime.
- Scar problems: Hypertrophic scars or thickened scars can occur, especially in high-tension zones. Scar outcomes depend on genetics, incision planning, and how smoothly early healing proceeds.
- Swelling and contour irregularities: Swelling is normal; uneven swelling can mimic “lumps” early on. Many contour concerns settle gradually over months.
The expert-patient mindset here is simple: ask what the monitoring and intervention protocol is for each common issue—because having a plan is often the difference between “managed” and “spiraled.”
Serious (But Rare) Risks: Blood Clots, Bleeding, and Tissue Compromise
Serious risks are uncommon in properly selected patients, but they must be discussed clearly.
- DVT/PE (blood clots): Any major surgery can increase clot risk. Prevention strategies include early mobilization, hydration, and individualized risk assessment. If you have a personal/family clot history, this must be disclosed and addressed proactively.
- Bleeding/hematoma: Bleeding can occur during or after surgery and may require intervention. Blood pressure control, medication review, and careful surgical technique matter.
- Skin or tissue necrosis (tissue compromise): This is uncommon but can occur when blood supply is compromised—risk increases with nicotine exposure and sometimes with overly aggressive combined procedures.
- Anesthesia-related complications: “Awake” approaches are often sought by patients who fear general anesthesia; however, sedation still requires serious monitoring and an experienced team.
One reason “awake” options can be psychologically meaningful is that they can help some patients overcome a paralyzing fear of general anesthesia—this theme is reflected in AKM’s patient narratives around awake procedures (notably for major facial surgery). The critical point is that anesthesia choice should be made for safety and predictability—not for branding.
The Safety Framework That Matters More Than Any Marketing Claim
If you only evaluate “before/after photos,” you miss the most important safety variables. A credible provider can explain their safety infrastructure in plain language, with verifiable standards. At AKM Clinic, the clinic’s published framework emphasizes:
- Strict pre-operative health screenings to confirm candidacy and reduce avoidable risk.
- Advanced patient vitals monitoring throughout every procedure, which is especially relevant for sedation-based (twilight/awake) workflows.
- Rigorous sterilization standards (ISO/TÜV) as a baseline expectation—not an optional feature.
- JCI-accredited hospitals and FDA-approved materials to align with “USA-standard” quality expectations for international patients.
- European Board-equivalent surgeon credentialing (positioned as comparable to US boards) as an objective trust anchor for expert researchers.
This is what sophisticated patients should look for: screening, monitoring, standards, and a facility ecosystem designed to reduce both medical risk and “recovery chaos.”
Warning Signs After Tummy Tuck: When to Call Your Surgeon
Many patients worry about “botched tummy tuck” scenarios, when the more immediate risk is not aesthetic—it’s ignoring early warning signs. Contact your surgical team urgently if you develop any of the following:
- Shortness of breath, chest pain, or sudden dizziness (possible clot-related emergency)
- One-sided leg swelling or calf pain, especially with warmth/redness (possible DVT)
- Rapidly increasing swelling, severe asymmetry, or expanding bruising (possible bleeding/hematoma)
- Fever, chills, worsening redness, pus-like drainage, or foul odor (possible infection)
- Severe pain that escalates instead of gradually improving
- Darkening skin, blisters, or tissue changes around the incision (possible blood supply compromise)
If you’re traveling internationally for surgery, your follow-up structure matters. AKM Clinic’s published model includes long-term virtual follow-up care as part of the VIP package—designed to reduce the “fear of abandonment” many international patients have after returning home.
Scars, Aesthetics, and the “Natural-First” Philosophy
In tummy tuck surgery, aesthetics is not only about being “flat.” It’s about proportion, transition zones (abdomen-to-hip), and scar behavior over time. The most sophisticated results look inevitable—like your body simply returned to a healthier baseline. That’s why expert patients should evaluate scar strategy with the same seriousness as technique: scar placement, closure tension, early healing environment, and long-term scar maturation determine whether your result looks refined or “surgically obvious.”
What a Tummy Tuck Scar Looks Like Over Time (and Why Early Judgments Are Usually Wrong)
Scar maturation is a biological process, not a single event. Even with an excellent closure, scars tend to evolve through predictable phases:
| Timepoint | What You May See | What It Usually Means |
|---|---|---|
| 2–6 weeks | Redness, mild swelling, firmness, sensitivity | Normal inflammatory healing; avoid stretching/tension |
| 6–12 weeks | Scar may look “worse” before it looks better; itchiness common | Collagen remodeling; consistent scar care matters |
| 3–6 months | Redness gradually fades; texture begins softening | Early maturity phase; many scars flatten significantly |
| 9–12 months | Lighter color, flatter profile (most patients’ “final” scar look) | Maturation phase; results are most stable here |
Expert-patient principle: evaluate scar quality and contour at appropriate timepoints (3, 6, and 12 months), not in week two.
Scar Placement Strategy: Engineering a Scar You Can Live With
A tummy tuck scar is the price of removing redundant skin. The real question is not “Will I have a scar?” but “Is the scar planned, proportional, and positioned intelligently?” High-quality scar strategy includes:
- Incision planning in standing position: to match how the abdomen sits with gravity and how clothing lines fall.
- Tension-aware closure: distributing tension so that one segment of the incision doesn’t carry the entire load (a common reason for widened scars).
- Harmony with anatomy: ensuring the scar matches your pelvis/hip structure so it doesn’t look “too high” or visually unbalanced.
For procedures like extended or fleur-de-lis tummy tucks, scar acceptance must be part of the decision logic. A more comprehensive correction can be life-changing for the right candidate—but only if the scar pattern aligns with your personal priorities.
Reading Before/After Photos Like an Expert (So You Don’t Get Misled)
Most “bad decisions” happen because patients compare photos emotionally rather than clinically. If you want to evaluate results intelligently, look for:
- Consistent lighting and posture: a pelvis tilt or rib flare can create fake “improvement” or fake “problem areas.”
- Timepoint clarity: results shown at 2–6 weeks often include swelling; 3–6 months is a more stable comparison window.
- Natural transitions: the best tummy tucks don’t create a “stuck-on flat panel.” They create a smooth transition from abdomen to flanks and hips.
- Navel naturalness (full patterns): avoid “round hole” or overly tight, unnatural positioning.
- Scar realism: look for honest scar images at real timepoints, not only the “best angle” early.
Surgeon’s Insight: “Rejuvenation, Not Alteration” (Applied to Body Contouring)
The psychological goal for most high-intent patients is not a different identity—it’s alignment: your outside reflecting how you feel inside. AKM Clinic frames this as a “Natural-First” approach:
“The most successful aesthetic surgery is one that goes unnoticed… to look like the most confident and revitalized version of yourself.”
That philosophy matters in tummy tuck planning, because “overcorrection” can look unnatural: excessive tightness, overly high scars, or an abdomen that doesn’t blend with the waist. The best plan respects anatomy and creates refinement—not distortion.
Real Patient Perspective: Why “Awake” Can Be a Deciding Factor for the Right Person
Awake/twilight approaches exist because a subset of patients are not merely “nervous”—they have a genuine barrier: fear of general anesthesia. In AKM’s patient narratives, one US patient described being paralyzed by anxiety over general anesthesia until the team confirmed local anesthesia was the safest and most suitable approach for her—after which she reported an “easy, smooth” recovery and feeling “fantastic” within days.
That testimonial is about facial surgery, not tummy tuck—but the decision psychology is highly relevant. For expert patients considering an awake tummy tuck, the meaningful question becomes: Can my procedure scope be safely matched to a local + sedation plan, with continuous monitoring and a disciplined recovery protocol?
It’s also worth noting that not every patient story explicitly mentions recovery technologies. AKM’s internal materials describe HBOT + LLLT as an integrated recovery pathway, but patient testimonials may focus more on comfort, logistics, and overall experience.
You are never alone. Our 24/7 Patient Hosts and English-speaking staff will be by your side from arrival to departure.
Combining Procedures (Mommy Makeover Logic)
Many candidates for a tummy tuck are also evaluating a broader transformation—commonly referred to as a mommy makeover. The logic is straightforward: pregnancy and weight shifts often affect multiple regions (abdomen, breasts, waist, arms). The medical challenge is that combining procedures changes the risk profile, operative time, and recovery demands—especially if you’re pursuing an awake/twilight approach.
Tummy Tuck + Liposuction: When It’s a Smart Combo
Combining liposuction with abdominoplasty can improve contour transitions, particularly at the waist and flanks. The key is surgical judgment: contour refinement should not compromise tissue blood supply.
- Best use: waist definition, flank blending, contour smoothing
- Higher caution zones: aggressive central abdominal liposuction when extensive skin elevation is planned
- Recovery implication: swelling can be more widespread and last longer
Ask your surgeon to explain where liposuction is planned, why it’s necessary, and how the plan protects blood flow to the abdominal skin.
Mommy Makeover: Who It’s For (and Who Should Stage It)
A mommy makeover typically refers to a combination such as tummy tuck + breast surgery (lift and/or implants) with selective liposuction. AKM Clinic lists mommy makeover within its body contouring scope.
Medically, the best candidates are those with:
- Stable weight and completed pregnancies (ideally)
- Good baseline health and the ability to follow a structured recovery plan
- Realistic downtime availability (you cannot “power through” a tummy tuck)
Staging (separating into two surgeries) may be the safer option if the combined plan becomes too long, too extensive, or too physiologically demanding.
Staging vs One-Session Surgery: A Decision Framework
Here’s a rational way to think about it:
- One-session surgery may be reasonable when the combined scope is moderate and your risk profile is low, with a facility capable of continuous monitoring and structured aftercare.
- Staging is often wiser when the plan becomes extensive (extended or fleur-de-lis + multiple regions), when medical risk factors exist, or when an awake/twilight strategy is a high priority.
The “best” plan is not the one that finishes everything fastest. It’s the one that delivers your goals with the best safety margin and the most predictable recovery.
Awake Tummy Tuck Cost Analysis 2026 (US vs Turkey)
When patients search “awake tummy tuck cost” or compare “tummy tuck cost NYC vs Miami,” they’re rarely just looking for the lowest number. They’re trying to estimate the total cost of care: surgeon expertise, facility standards, anesthesia plan, recovery support, time off work, and the financial impact of a delayed or complicated recovery. The smartest cost decision is not the cheapest quote—it’s the plan with the best balance of outcome predictability, safety margin, and recovery efficiency.
What Actually Drives the Cost of a Tummy Tuck in the U.S.?
Even within the same city, two quotes can differ dramatically because “tummy tuck” isn’t a single uniform procedure. Common cost drivers include:
- Procedure type: mini vs full vs extended vs fleur-de-lis (more scope generally = more OR time and complexity)
- Facility fees: hospital vs accredited surgery center vs private facility
- Anesthesia fees: general anesthesia typically adds separate anesthesia costs; sedation plans can vary widely
- Combined procedures: lipo, breast procedures, body lifts, etc.
- Revision complexity: secondary tummy tucks often cost more due to scar tissue and altered anatomy
- Geography: higher cost-of-living markets (e.g., NYC) typically price higher
Important nuance: published “averages” often refer to surgeon fees only. Your actual total may be significantly higher once facility and anesthesia are included.
Typical Price Anchors: NYC vs Miami vs Istanbul (Directional, Not a Quote)
Because costs change over time and vary by surgeon, it’s better to use ranges as anchors rather than treat them like guarantees. Below is a practical comparison framework expert patients use to orient their research:
| Market | Typical Cost Reality | What’s Usually Included |
|---|---|---|
| New York City | Commonly higher due to overhead and demand; totals often rise with facility + anesthesia | Often surgeon fee quoted first; facility/anesthesia may be separate |
| Miami | Often marketed as more “competitive,” but scope and add-ons change totals quickly | Varies widely; read fine print on what’s included |
| Istanbul, Turkey | Often lower total package pricing compared to major US markets | Packages commonly bundle hospital, anesthesia, accommodation, transfers, and aftercare support |
Expert-patient rule: compare “total out-the-door cost,” not the headline number. Ask each provider to itemize surgeon fee, facility fee, anesthesia, garments, medications, follow-up, revisions policy, and complication management plan.
Why Turkey Can Be Lower Cost Without Lower Standards (When Done Correctly)
The reason some patients consider Istanbul is not a desire for bargain surgery—it’s the possibility of accessing premium standards at a lower operational cost base. In well-structured programs, cost advantage can come from:
- Lower operational overhead compared to NYC/LA/London
- Bundled “all-inclusive” logistics (which can reduce hidden costs and recovery friction)
- High procedural volume and standardized workflows (when paired with proper quality controls)
However, the risk with international surgery is not the passport stamp—it’s weak screening, weak monitoring, and weak follow-up. If you’re considering surgery abroad, the differentiator is whether the provider can demonstrate verifiable standards (hospital accreditation, sterilization protocols, continuous monitoring) and a structured long-term follow-up pathway.
At AKM Clinic, the model is positioned as a VIP, structured pathway for international patients, with an all-inclusive package concept that typically covers core logistics (hotel, transfers, medications/garments, coordinated follow-up). The goal is to reduce “recovery chaos”—a major reason expert patients fear overseas care.
Tummy Tuck Financing: How Smart Patients Think About It
In the United States, cosmetic surgery is typically self-pay, but financing options exist through third-party medical financing providers. If you’re evaluating financing, treat it like any other financial decision:
- Understand the interest rate structure (promotional vs standard APR)
- Calculate total repayment cost, not just monthly payment
- Do not choose a bigger surgery solely because you can “spread it out”
- Budget for recovery time (time off work can be a larger hidden cost than the procedure itself)
If you’re comparing US care to an international package, include travel, extended stay (if recommended), and contingency planning for follow-up care at home—because the true cost of complications is not just money, it’s time and disruption.
Get a 100% transparent, all-inclusive quote tailored to your needs. No hidden fees—just world-class care at an accessible price.
Choosing the Right Surgeon & Facility (The Expert Patient Checklist)
When people search “best tummy tuck surgeon,” they’re often hoping for a shortcut. There isn’t one. But there is a reliable checklist: surgeon credentialing, facility standards, complication readiness, and follow-up structure. If you apply those filters, your probability of a safe experience and a natural result improves dramatically—especially with awake/twilight strategies where continuous monitoring and team coordination are non-negotiable.
Credentials That Matter (and Why They Matter)
In abdominoplasty, aesthetic taste matters—but safety and technique maturity come first. Your consultation should clearly address:
- Board-level training and credentialing: seek objective credentials that signal structured surgical education and ongoing standards
- Procedure volume: surgeons who regularly perform tummy tucks (including your specific type) tend to have more refined scar and contour planning
- Revision approach: ask how the surgeon evaluates and manages complications or aesthetic refinements
- Natural result philosophy: does their work look proportional and anatomically believable?
At AKM Clinic, surgeons are positioned as European board-equivalent and internationally oriented specialists (without relying on celebrity branding). The value for the expert patient is clarity: credentials, systems, and outcomes—not hype.
Facility Standards & Monitoring: What You Should Verify
Many “bad outcomes” are not due to a lack of talent—they are due to weak systems. For awake/twilight strategies, the facility must be built around monitoring and rapid response.
- Continuous vitals monitoring: especially important for sedation-based anesthesia plans
- Sterilization and infection control: modern standards should be explicit and verifiable
- Hospital access for higher-acuity needs: where is surgery performed, and what escalation pathways exist?
- Materials standards: implants/materials (when applicable) should meet recognized quality benchmarks
AKM’s published infrastructure emphasizes strict pre-op screening, advanced vitals monitoring, rigorous sterilization standards, and the use of JCI-accredited hospitals with FDA-approved materials in its international-patient positioning.
How to Evaluate “Awake” Claims Without Being Misled
Because “awake tummy tuck” is a high-intent keyword, some marketing can over-simplify it. Use these questions to stay in control:
- What exactly do you mean by “awake”? (local only vs local + IV sedation vs other)
- What is the maximum scope you’ll do under this plan? (mini vs full vs extended vs combined procedures)
- Who monitors sedation and vitals continuously? (role clarity matters)
- What is your conversion policy? If comfort or safety requires deeper anesthesia, what happens?
- How do you select candidates? If they say “everyone qualifies,” that’s a red flag
Expert patients aren’t trying to “win” a certain anesthesia type—they’re trying to choose the plan that makes their surgery safer, calmer, and more predictable.
Perform your surgery with confidence. Meet our European Board Certified surgeons with over 2,000 successful facial surgeries.
The Medical Journey for International Patients (Logistics)
If you’re considering an awake tummy tuck in another country, your results won’t depend only on surgical skill—it will depend on how well the entire system supports you: pre-op screening, day-of monitoring, early recovery oversight, and structured follow-up after you return home. Expert patients should evaluate international care like a risk-managed project: clear timelines, clear responsibilities, clear escalation pathways, and a follow-up plan that doesn’t disappear the moment you board a flight.
Virtual Consultation → Personalized Surgical Plan (Before You Travel)
A legitimate international workflow starts with a real clinical assessment, not a sales conversation. Before travel, your plan should define:
- Procedure type: mini vs full vs extended vs fleur-de-lis vs reverse, based on your laxity distribution
- Anesthesia strategy: what “awake” means in your case (local-only vs local + IV sedation), including what would trigger a change in plan
- Muscle/fascial tightening: whether diastasis is clinically meaningful and whether plication is recommended
- Drain strategy: drains vs drainless approach and why
- Recovery roadmap: realistic downtime, garment protocol, mobility expectations, and follow-up timing
For patients prioritizing an awake/twilight approach, this is also where candidacy screening matters most. Your medical history, medication list, clot risk factors, nicotine exposure, and anxiety profile should be reviewed in a structured way.
Arrival, Transfers, Accommodation, and Surgery-Day Flow
From an expert-patient perspective, international logistics should reduce friction—because “logistics stress” can become medical stress. A high-quality program typically coordinates:
- Airport transfers with reliable timing and clear points of contact
- Hotel accommodation that is recovery-friendly (elevators, quiet environment, ability to rest)
- Pre-op testing and clearance in a defined window before surgery
- Clear surgery-day timeline: arrival time, marking, anesthesia plan confirmation, post-op monitoring period
AKM Clinic positions this as a VIP, all-inclusive pathway for international patients, often bundling hotel and transfers and coordinating the practical details so you can focus on recovery rather than administration.
Post-Op Monitoring in Istanbul + Long-Term Virtual Follow-Up After You Return Home
International surgery becomes risky when follow-up is vague. The safest model is the one that treats aftercare as a structured phase with clear checkpoints. A responsible plan includes:
- Early monitoring: scheduled wound checks, drain management (if used), swelling/seroma assessment, mobility guidance
- Clear “warning sign” escalation: who to contact, how quickly, and what the plan is if symptoms suggest clot risk, infection, bleeding, or fluid collections
- Defined long-term follow-up: virtual check-ins at meaningful timepoints (commonly 1, 3, 6, and 12 months) to support scar care, contour settling, and recovery questions
If your program includes adjunct recovery modalities such as HBOT and LLLT, expert patients should ask for the protocol structure: how many sessions, when they occur (early vs later), and what objective goals are being targeted (swelling control, tissue support, comfort, scar maturation strategy).
Expert-patient takeaway: Choosing a provider internationally isn’t only about “who is the best surgeon.” It’s about who provides the safest and most organized medical journey—before, during, and long after the operation.
From VIP airport transfers to 5-star hotel accommodations, we handle every detail. Enjoy a seamless medical travel experience in Istanbul.
Awake Tummy Tuck: Frequently Asked Questions
These are the most common, high-intent questions patients ask while researching an awake tummy tuck. The answers are written to be practical and decision-oriented—so you can translate research into a safe, realistic surgical plan.
Can you really do a tummy tuck “awake”?
In selected patients, yes—an “awake tummy tuck” can be performed using local anesthesia with IV sedation (twilight). But “awake” doesn’t mean you feel everything. Many patients are relaxed, drowsy, and remember little. The deciding factors are your procedure scope (mini vs full vs extended), your medical profile, and your ability to remain calm and stable during surgery.
How painful is an awake tummy tuck?
The goal is that you feel pressure and movement, not sharp pain. Comfort depends on (a) how well local anesthesia is placed, (b) how thoughtfully sedation is managed, and (c) whether abdominal wall tightening is performed (tightening often increases early “core soreness” afterward). If a provider implies “no pain,” that’s unrealistic; a credible plan explains exactly how discomfort is prevented and how pain is managed after surgery.
How long is tummy tuck recovery?
Most patients feel the most restricted in the first 1–2 weeks. Many desk-based patients plan a light return to work in roughly 2–4 weeks (individual variation is significant). Strenuous activity and core-heavy exercise are typically delayed longer, commonly around 6+ weeks depending on your surgeon’s protocol and whether muscle/fascial tightening was done. Scar maturation and final contour settling often continue for 6–12 months.
What are the warning signs after a tummy tuck?
Call your surgical team urgently (or seek emergency care) for: shortness of breath, chest pain, fainting, one-sided leg swelling/calf pain, rapidly increasing swelling or bruising, fever/chills, spreading redness, foul drainage, escalating severe pain, or darkening/blistering skin around the incision. These are not “normal recovery.” They require immediate evaluation.
Will I have drains?
Possibly. Drains are commonly used to reduce fluid accumulation (seroma). Some surgeons use drainless internal fixation strategies in selected patients. The best question isn’t “Can you do drainless?”—it’s “What is your seroma strategy for my exact plan, and what happens if fluid forms?”
What does a tummy tuck scar look like at 6 months?
At around 6 months, many scars are still in an “active remodeling” phase—often lighter and flatter than early on, but not fully matured. Final scar appearance typically becomes clearer closer to 9–12 months. Scar quality is strongly influenced by early healing (tension, infection prevention, and avoiding premature stretching).
Is a tummy tuck dangerous?
It is a major surgery, so it carries real risks. Most patients recover safely when they are appropriately screened and the procedure is performed in a properly monitored facility with structured aftercare. The biggest safety lever is not a buzzword (awake vs general)—it’s patient selection, procedure scope control, monitoring, and follow-up.
What’s the “risk of death” with a tummy tuck?
Serious complications are rare in properly selected patients, but no elective surgery is zero-risk. Your true risk depends on factors like smoking/nicotine exposure, clot risk, procedure extent, combined surgeries, and how strong the safety system is (screening, monitoring, early mobilization, escalation protocols). If you’re concerned, ask your surgeon to walk through your specific risk factors and prevention plan in detail.
Can I get pregnant after a tummy tuck?
Yes—pregnancy is still possible. However, pregnancy can stretch the repaired tissues and skin again, which may reduce the longevity of your result. If pregnancy is planned soon, many surgeons recommend postponing a tummy tuck to protect your investment and reduce the chance of needing revision.
How much does a tummy tuck cost in NYC vs Miami vs Turkey?
Costs vary widely based on procedure type (mini/full/extended), facility and anesthesia fees, whether you combine procedures, and surgeon experience. In the U.S., many “headline” prices exclude facility and anesthesia costs. In international settings, pricing is often packaged (hospital, hotel, transfers, aftercare), which can make totals easier to predict—but the correct comparison is still total cost of care plus the strength of safety standards and long-term follow-up.
How do I choose the best tummy tuck surgeon?
Use a checklist, not a vibe:
- Credentials and training you can verify
- High procedure volume in the tummy tuck type you need
- Before/after consistency with honest timepoints and scar visibility
- Facility standards + continuous monitoring (especially important for sedation-based surgery)
- Clear complication and revision policy (what happens if you develop seroma, infection, delayed healing?)
- Structured follow-up, including after you travel home (if international)
The “best” surgeon is the one whose plan matches your anatomy, whose results look natural and consistent, and whose safety system is built to prevent and manage complications—not deny them.
Awake Tummy Tuck: Patient Stories

Lisa

Awake Tummy Tuck Surgeons
Awake Tummy Tuck Cost in Turkey
Starting from $4800
* There are no hidden fees or unexpected charges.
- Your Personalised Awake Tummy Tuck Procedure
- All Specialist Surgeon & Anesthesia Fees
- All Pre-Op Tests & Post-Op Check-ups
- 5-Star Hotel Accommodation (incl. breakfast)
- All Private VIP Airport & Clinic Transfers
- 24/7 Dedicated Patient Coordinator & Translation Services
Awake Tummy Tuck: A Cost Comparison
| City | Cost |
|---|---|
| Miami, FL | ~$10,000 |
| New York, NY | ~$16,000 |
| Los Angeles, CA | ~$18,000 |
| Houston, TX | ~$12,600 |
| Atlanta, GA | ~$11,000 |
Awake Tummy Tuck: Patient Reviews
Jammal Canada
I have had face and neck lift with AKM Clinic they have been so good to me and my operation went so smoothly🥰 i would like to thank my doctor here and also to the team 💐

Ava Canada
Thank you AKM Clinic for giving me my confidence back! Had facelift + temporal lift 3 months ago and the outcome is already stunning. Special thanks to Hande!

Jakayla USA
Had a deep plane facelift and lower eyelid procedure at AKM Clinic 7 months ago. The results are fantastic - very subtle and natural. I didn’t expect the entire experience to be so comfortable. Hande managed everything and kept in contact even after I returned to USA. I’m beyond pleased with the outcome and the care I received. Would do it again in a heartbeat!

Barbara United Kingdom
It has been 4 months since my surgery. Everything is great, The most important thing is l love the way l look, l look exactly how l wanted. Meaning l look natural, just almost 40 years younger. I pulled Facebook - majority voted 37ys. I also had face, neck, chest, and hands CO2 laser. My skin is flawless.

Lisa Canada
I had a face, neck and arm lift at AKM. I’m just over 4 weeks post and couldn’t be happier with the results. The entire experience was wonderful! My coordinator, Khadija made me feel comfortable from beginning to end! I highly recommend AKM and will definitely go back for other procedures!

Julie USA
I am beyond grateful I went with AKM Clinic for my deep plane face and neck lift, upper eyelid, and co2 laser. Dr. Akif has magic hands and my results are truly incredible! I came from the US and assistant Emine was the best in assuring every detail was coordinated and communicated with me beyond my expectations every step of the way. 10 out of 10 to the entire team! I couldn’t be more pleased!

Ready to Start Your Own Transformation Journey?
Join the 2,000+ patients who trusted Dr. Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, revitalized you begins with a simple, no-obligation conversation. Contact us today from the USA for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. No hidden fees.
#2: Secure Your Date & VIP Booking
Once you're ready, our dedicated patient coordinators will help you secure your procedure date. We'll handle all your bookings, including your 5-star hotel and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you'll meet your specialist surgeon to finalise the details for your "natural, subtle, and revitalized" new look.











