Gynecomastia Surgery in Turkey




- Gynecomastia surgery reduces excess male breast tissue for a flatter, natural chest contour.
- Recovery is structured with compression, staged activity return, and realistic healing expectations over months.
- Safety-first planning covers technique choice, anesthesia options, risk awareness, and clear follow-up support.
- Cost varies widely by technique, location, and what’s included; transparent quotes enable true comparisons.
Summary generated by AI, fact-checked by our medical experts.
Gynecomastia Surgery: Quick Facts
Procedure Time
Anesthesia
Recovery Time
Hospital Stay
Back to Work
Gynecomastia Surgery Results: Before and After
Gynecomastia surgery (often called male breast reduction) is a procedure designed to restore a flatter, more masculine chest contour when excess breast tissue persists despite training, diet, and healthy body weight. For many men, the issue is not “lack of effort”—it’s anatomy. The goal of surgery is to correct the underlying tissue imbalance and reshape the chest in a way that looks natural in motion, in clothing, and up close.
A high-quality result is not about looking “operated on.” It’s about looking like yourself—just with a chest that finally matches the rest of your physique. That mindset is central to AKM Clinic’s brand philosophy: Rejuvenation, Not Alteration.
The best gynecomastia result is the one that doesn’t announce itself—your chest simply looks naturally masculine, balanced, and proportional.
Table of Contents

What Is Gynecomastia Surgery?
Gynecomastia surgery is a procedure that reduces enlarged male breast tissue. It removes gland tissue, excess fat, or both. In advanced cases, it also removes extra skin to restore a flatter, firmer chest. The goal is a natural-looking contour that fits your frame.
Most men who research this procedure are trying to answer one question: “Is what I’m seeing fat, gland, or both?” That distinction matters because the treatment plan changes. Fat-dominant fullness can respond well to contouring, while firm glandular tissue often needs direct removal. A good surgical plan starts with anatomy, not assumptions.
Gynecomastia vs. pseudogynecomastia (fat vs. gland)
Gynecomastia is an overdevelopment of breast gland tissue in males. Pseudogynecomastia is fullness that is mainly fat. Many patients have a mix of both. That’s why you’ll also see the procedure described as male breast reduction surgery—it’s a practical term that covers multiple tissue patterns.
- Fat-dominant chest: softer, more diffuse fullness; often improves with weight change, but not always evenly.
- Gland-dominant chest: firmer “rubbery” tissue, often centered under the areola; usually doesn’t disappear with training alone.
- Mixed pattern: the most common real-world scenario; typically needs a combined plan.
Chest anatomy in plain English
Your chest contour is shaped by three layers working together: skin, fat, and glandular tissue. The areola–nipple complex sits on top, and the transition zone toward the armpit affects how “athletic” the chest looks. Skin quality matters too. If the skin is tight, it can re-drape smoothly after tissue reduction. If it’s stretched, the plan may need to address skin excess directly.
What surgery actually changes (and what it does not)
Surgery changes projection and contour. It reduces the forward bulge and improves the outline of the chest from the front and side. It also improves how the lower chest blends into the upper abdomen. What it does not do is “change your genetics,” erase every small asymmetry, or replace lifestyle fundamentals. A precise plan aims for balance—flat enough to look natural, not over-corrected.
Our surgery dates fill up quickly due to high international demand. Secure your consultation today to plan your ideal travel dates.
Benefits: What Changes After The Procedure?
Most patients don’t want a dramatic “new body.” They want their chest to match the rest of them. When the plan is right, the result looks unforced: cleaner lines, better definition, and clothing that sits normally across the chest. The best outcomes feel like relief—physically and mentally—because the chest stops being the center of attention.
Aesthetic goals: flatter chest, sharper definition
The aesthetic goal is not simply “smaller.” It’s a smoother contour with natural transitions: chest to shoulder, chest to underarm, and chest to upper abdomen. Good technique also respects the areola so it sits naturally on a flat surface rather than projecting forward.
Lifestyle impact: clothes, gym confidence, posture
Patients often describe the biggest change as “not thinking about it anymore.” T-shirts fit without strategizing. Posture becomes more open. Training the upper body becomes more motivating because the silhouette finally reflects the effort you put in.
Physical comfort in everyday life
Beyond appearance, some patients experience practical improvements. Less rubbing during exercise. Less sensitivity in certain movements. Less irritation from compression athletic wear. These are not guaranteed outcomes, but they’re common reasons men decide that surgery is worth the commitment.
Expectation setting: natural-first results
We plan for a chest that looks like it belongs to you—your age, your build, your skin quality. That means we focus on proportion and long-term harmony, not extremes. It’s the same guiding principle behind everything we do.
The goal is “Rejuvenation, Not Alteration.”

Am I a Good Candidate?
The best candidates for gynecomastia surgery are men who are medically stable, close to a sustainable weight, and bothered by chest fullness that doesn’t resolve with training or time. A strong plan is built on clarity: what tissue is driving the shape (fat, gland, or both), how your skin behaves, and what you want the chest to look like in real life—not just in a filtered “after” photo.
Who tends to do well
- Stable weight: You don’t need to be “shredded,” but large weight swings before or after surgery can affect skin re-draping and symmetry.
- True gland component or mixed tissue: Especially when there’s firm tissue behind the areola that doesn’t respond to dieting.
- Realistic expectations: You understand that “natural” includes minor asymmetry and a settling period as swelling resolves.
- Healthy baseline: You can safely undergo anesthesia/sedation and follow post-op instructions.
Answer a few quick questions about your concerns, health, and goals to learn which treatment options may suit you best.
When it’s smarter to pause (or investigate further)
Some scenarios don’t mean “no forever,” but they do mean “not yet.” A responsible surgeon will often recommend addressing the underlying driver first.
- Unstable weight or active bulking/cutting cycles
- Suspected hormonal imbalance (especially if breast growth is recent or progressing)
- Medication-related breast changes (your prescribing doctor may need to review options)
- Uncontrolled medical conditions (e.g., poorly controlled diabetes, uncontrolled blood pressure)
If you have a new, rapidly changing lump, nipple discharge, or significant one-sided change, you should seek medical evaluation promptly. Surgery is not a substitute for a proper diagnosis.
Smoking, supplements, and medication planning
Your healing quality is not only about the surgeon’s hands—it’s also about circulation, inflammation control, and compliance. Nicotine is one of the most common avoidable factors that increases risks around wound healing. Many clinics advise stopping nicotine well before surgery and avoiding it during early recovery.
Likewise, some supplements and medications can increase bleeding risk or affect anesthesia. Always disclose everything you take—even “natural” products—and follow your surgical team’s instructions about what to pause and when. Don’t stop prescription medications on your own without guidance.
What a serious pre-op assessment usually includes
While protocols vary, an “expert-level” workup typically covers:
- History + physical exam: timeline, triggers, tenderness, weight changes, medication use
- Tissue assessment: fat vs gland dominance, skin elasticity, nipple–areola position
- Medical screening: basic labs when indicated; additional tests if there are risk factors
- Plan confirmation: technique selection, scar strategy, and recovery timeline aligned with your lifestyle
Understanding The Condition: Causes, “Grades,” and Why Fat Loss Isn’t Always Enough
Gynecomastia is common—and often misunderstood. Many men assume it’s purely a fitness problem. But if gland tissue is driving the projection, no amount of chest presses will erase it. Understanding the “why” matters for two reasons: it helps you rule out avoidable causes, and it prevents you from wasting months (or years) chasing a result that can’t happen without tissue removal.
Common drivers (and why you shouldn’t self-diagnose)
Gynecomastia can be influenced by hormone shifts, genetics, weight changes, and certain medications. It often appears during puberty and may improve over time. In adults, persistent or progressive changes may require a more structured evaluation—especially if the onset is sudden or associated with other symptoms.
This guide can help you understand patterns, but it can’t replace a medical assessment. If you suspect a medication or hormonal issue, the right step is a clinician-led review, not guesswork.
How “severity” changes the surgical plan
Most grading frameworks look at two practical variables:
- How much tissue volume is present (mild vs moderate vs significant fullness)
- How much skin excess exists (tight skin vs stretched skin that won’t re-drape)
Mild cases with tight skin can often be treated with smaller access points and contouring-focused techniques. More advanced cases may need additional steps to address skin redundancy and nipple–areola positioning. The plan is not about chasing a “perfectly flat” chest; it’s about achieving a natural contour with stable long-term proportions.
When weight loss helps—and when it can’t
Weight loss can reduce fat volume and improve chest shape in fat-dominant cases. However, three common limitations show up in real patients:
- Gland tissue remains: the chest still projects under the areola even at low body fat.
- Skin doesn’t bounce back: after weight loss, loose skin can still create a “folded” look.
- Distribution is uneven: your body may lose fat from other areas first, leaving the chest lagging behind.
If you’ve reached a stable, healthy weight and the problem persists, surgery becomes a more direct solution—because it addresses the actual tissue creating the contour.
Why a tailored plan beats “one-size-fits-all”
Two men can have the same cup-like appearance in a shirt and need completely different approaches in the operating room. A tailored plan considers:
- tissue mix (fat vs gland)
- skin quality and elasticity
- areola size/position and nipple projection
- chest width, muscle definition, and symmetry
This is where “expert patient” research pays off: the more precisely you can describe your goals and concerns, the more refined (and realistic) the plan becomes.
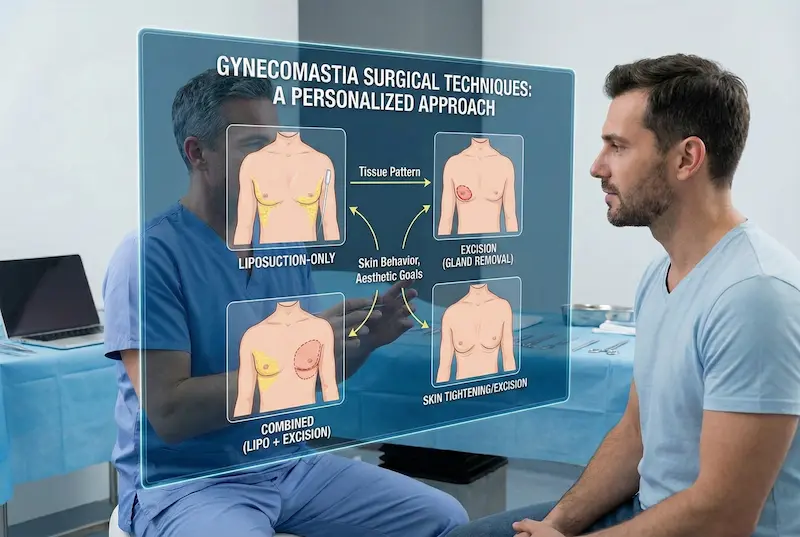
Procedures to Combine Gynecomastia Surgery
For the right candidate, combining procedures can create a more balanced, athletic silhouette in a single treatment plan. The key is to prioritize safety, limit operative time when needed, and match the surgical “stack” to your anatomy—especially the tissue pattern driving gynecomastia and the way your skin re-drapes after reduction.
Why combine procedures?
Patients often choose combination surgery to align the chest with the rest of the torso. When gynecomastia surgery improves the upper body contour, concerns like abdominal fullness or arm laxity can feel more noticeable. A combined approach can address these areas cohesively, rather than in isolated steps.
Most common combinations
- Six pack surgery + gynecomastia surgery: targets abdominal definition and chest contour for a proportional, “V-shape” look.
- Tummy tuck + gynecomastia surgery: considered when significant skin laxity or abdominal excess is present, especially after weight loss.
- Arm lift + gynecomastia surgery: helps patients with loose upper-arm skin or heaviness that doesn’t respond to training.
- Daddy makeover: a tailored combination that may include gynecomastia surgery plus abdominal contouring (and, in selected cases, an arm lift), customized to the patient’s goals.
How surgeons decide what’s appropriate
Combination plans depend on medical screening, BMI/weight stability, skin quality, and recovery logistics. If the overall surgical scope becomes too extensive for a single day, a staged approach may be safer and can still deliver a refined, natural result.
Surgical Techniques Explained
There isn’t one universal technique for gynecomastia surgery. The best approach is chosen based on your tissue pattern and skin behavior—then refined around your scar tolerance, downtime needs, and aesthetic goals.
Liposuction-only approach (fat-dominant cases)
When fullness is primarily fatty, liposuction for male breast reduction can sculpt the chest through small access points. The surgeon removes fat strategically to improve contour and blend the chest into the underarm area. The key word is “strategically”—aggressive suction in the wrong areas can create dents or an unnatural “scooped” look.
Limitations: liposuction alone cannot reliably remove firm gland tissue. If a dense gland component is left behind, the chest may still project under the areola.
Excision (gland removal) and periareolar access
When gland tissue is significant, direct excision is often required. A common strategy is a discreet incision along the lower border of the areola (where color transitions can camouflage the scar). Through that access, gland tissue can be removed and the contour can be shaped more precisely than with suction alone.
Trade-off: while periareolar scars often heal well, scar quality varies by skin type, tension, and aftercare.
Combined technique (most common in practice)
Many patients benefit from a combined approach: liposuction for broad sculpting and blending, plus excision for the firm tissue that liposuction can’t fully address. This is frequently the “best of both worlds” plan because it targets the full tissue mix and helps the surgeon create a smoother transition across the chest.
Skin tightening or skin excision (when skin excess is the main obstacle)
If the skin is stretched and unlikely to re-drape after tissue reduction, the plan may need to include skin management. This can range from conservative tightening strategies to more direct skin excision in advanced cases. The more skin you remove, the more visible the scars can become—so the decision is always a balance between contour improvement and scar burden.
A “natural contour” plan isn’t about making the chest as flat as possible. It’s about proportion, smooth transitions, and avoiding over-correction that looks surgical.
Technique comparison (quick expert overview)
| Approach | Best for | Typical scars/incisions | Main advantages | Key trade-offs |
|---|---|---|---|---|
| Liposuction only | Fat-dominant fullness, good skin elasticity | Small access points (often a few mm) | Minimal scarring, good blending and contouring | May not fully correct firm gland projection |
| Excision only | Gland-dominant cases with less diffuse fat | Often periareolar (around areola border) | Direct removal of dense gland tissue | Can leave contour irregularity if blending isn’t addressed |
| Combined (lipo + excision) | Mixed tissue (very common), shape-focused outcomes | Small access points + periareolar incision (if needed) | Targets both fat and gland; smoother, more natural contour | More steps, potentially slightly longer recovery |
| Skin management | Significant skin excess / advanced cases | Varies (can be more visible depending on technique) | Addresses loose skin that won’t re-drape | Greater scar burden; decision must be individualized |
Male Breast Reduction Without Surgery: Honest Alternatives
Many men do the right thing first: diet, training, and time. In some cases, that’s enough—especially when the issue is mainly fat. But it’s also common to hit a ceiling where the chest shape doesn’t match the rest of your progress. That’s where honest alternative analysis matters: it prevents false hope and helps you choose the right tool for the actual problem.
Lifestyle + training (when it helps)
Body fat reduction can improve chest fullness when fat is the dominant component. Strength training can improve upper-body proportions and help the chest look more defined. But neither can reliably remove gland tissue. If the areola still projects at low body fat, that’s often a clue that gland is part of the picture.
Medical management (when an underlying driver exists)
If gynecomastia is linked to a medication, supplement, or hormonal imbalance, medical management may help—especially when the change is recent. This is not something to “DIY.” The right path is clinician-led evaluation, because the priority is safety and correct diagnosis.
Device-based options (and realistic limits)
Non-surgical fat reduction devices (such as cryolipolysis—often searched as coolsculpting for male breast reduction) can reduce localized fat in selected patients. However:
- They do not remove gland tissue.
- They cannot reposition the nipple–areola complex.
- They don’t correct significant skin excess.
For the “expert patient,” the decision often comes down to efficiency: if the driver is gland or skin, devices can become a slow, expensive detour.
Compression garments and “camouflage” strategies
Compression shirts can help temporarily with appearance and comfort, but they don’t treat the underlying tissue. If you find yourself building your wardrobe around concealment, that’s often the moment patients decide a definitive solution is worth it.
Anesthesia Choices: Comfort, Control, and Safety
One of the most common “expert patient” questions is about anesthesia: what’s safest, what’s most comfortable, and what makes sense for your specific case. In reality, anesthesia is not a one-size-fits-all decision. It’s selected based on your surgical plan (lipo-only vs combined vs skin management), your medical profile, and your comfort level.
Local anesthesia and the role of tumescent technique
For many contouring procedures, surgeons use a local anesthetic approach supported by a tumescent solution. In simple terms, this helps numb the area, reduce bleeding, and make fat removal smoother. When appropriate, it can support a more controlled experience and a calmer early recovery.
However, “local” doesn’t automatically mean “easy.” The right question is whether local anesthesia is appropriate for your case and whether it can deliver a predictable, comfortable experience without compromising precision.
Twilight sedation: why many patients prefer it
Twilight sedation (often called “conscious sedation”) sits between fully awake and fully asleep. Many patients like it because it can reduce anxiety and discomfort while avoiding some of the downsides associated with deeper anesthesia. You’re typically very relaxed and may not remember much of the procedure, while your team continues to monitor you closely throughout.
For the safety-conscious patient asking, “is male breast reduction surgery safe?” the most honest answer is that safety is multi-factorial: the right anesthesia plan is the one that matches your body, your medical history, and the surgical steps required—supported by strict screening and monitoring.
When general anesthesia can be the better choice
General anesthesia may be recommended when the surgical plan is more complex, when extensive work is required, or when it’s the safest and most predictable way to maintain comfort and stillness for precision. Some patients also prefer it for personal comfort reasons. The key is not the label (twilight vs general), but whether the plan creates the best balance of safety, comfort, and surgical control for your specific anatomy.
Safety infrastructure: what matters more than the anesthesia “type”
Regardless of the anesthesia approach, a responsible protocol typically includes:
- Pre-op screening: medical history review, risk-factor assessment, and appropriate tests when indicated
- Intra-op monitoring: continuous tracking of vital signs
- Standardized sterility and safety steps: to reduce infection and complication risks
- Clear post-op instructions: so swelling control, garment use, and activity restrictions are followed correctly
The anesthesia plan should never be chosen for marketing reasons. It should be chosen because it is medically appropriate for you.
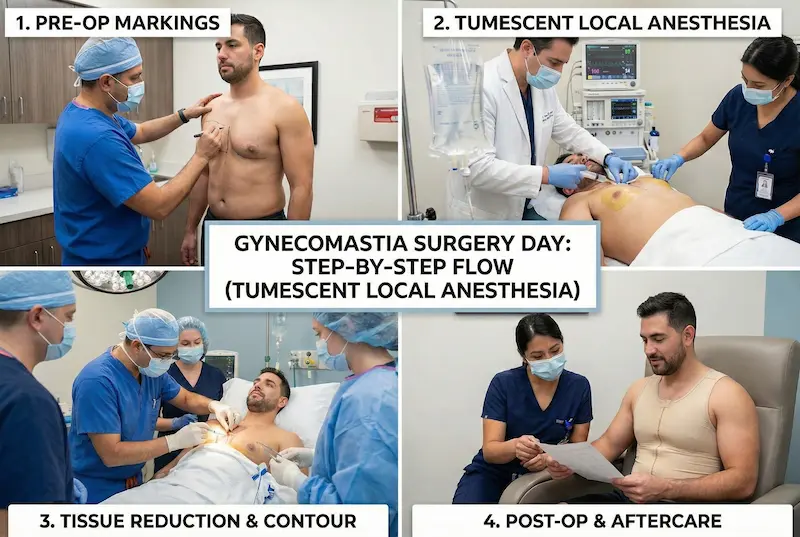
Step-By-Step: What Happens On Surgery Day?
Knowing the flow of surgery day reduces anxiety and helps you plan logistics—especially if you’re traveling. While details vary by technique, most gynecomastia surgery days follow a predictable sequence built around safety, precision, and controlled recovery.
Pre-op markings and final plan confirmation
Before surgery, your surgeon typically marks the chest while you’re standing. This matters because gravity, skin tension, and natural asymmetry are most visible in an upright position. This is also the final moment to confirm goals like how “athletic” vs “soft natural” you want the contour to look.
Anesthesia/sedation and sterile preparation
Once you’re in the operating environment, the team focuses on comfort and safety: anesthesia/sedation is administered as planned, the skin is cleaned, and sterile draping is applied. These steps are not glamorous—but they’re foundational for reducing risk.
Tissue reduction and contour sculpting sequence
The procedure itself typically follows a contour-first logic:
- Contour shaping: when liposuction is part of the plan, it’s used to sculpt broadly and blend the chest into surrounding areas
- Gland management: if firm gland tissue is present, excision may be performed to reduce projection—especially under the areola
- Balance and symmetry checks: fine-tuning to keep the chest natural-looking from multiple angles
High-quality results come from restraint and precision—removing what needs to go, while protecting natural transitions so the outcome doesn’t look “operated on.”
Hemostasis, drains (when needed), and closure
Controlling bleeding (hemostasis) is a key step for lowering the risk of hematoma and supporting smoother healing. Some cases may require drains, especially if the tissue removal is more extensive or if the surgeon feels it will help reduce fluid collection. Many straightforward cases do not require drains, but the decision should be individualized.
Incisions are closed with a focus on minimizing tension—because tension is one factor that can worsen scar quality.
Compression garment and immediate aftercare checklist
After surgery, you’ll typically be placed in a compression garment. This isn’t just for “support”—it helps manage swelling, encourages smoother re-draping, and protects the early contour while tissues settle.
Most patients leave with a clear checklist that covers:
- how to wear the garment and for how long
- how to sleep and move safely
- what level of swelling/bruising is expected
- which symptoms require immediate contact
- when to return for follow-up (or how virtual follow-up works if you’re traveling)
Expert tip: The first week is about protecting the result—not testing it. Consistent compression and smart activity limits usually pay off in smoother contour settling.
You are never alone. Our 24/7 Patient Hosts and English-speaking staff will be by your side from arrival to departure.
Does Gynecomastia Surgery Leave Scars?
Yes—all surgery leaves scars because an incision is how the surgeon accesses tissue. The more useful question is: where are the scars placed, how visible are they likely to be, and what can be done to help them heal well? In most standard cases, scars are designed to be discreet and placed in natural transitions (like the border of the areola) or through very small access points used for contouring.
Typical incision patterns (and why they’re chosen)
- Periareolar incision: Often placed along the edge of the areola when gland excision is needed. The color change at the areola border can help camouflage healing.
- Small liposuction access points: Tiny incisions (often only a few millimeters) placed in less noticeable areas for contouring and blending.
- Skin-management incisions (advanced cases): When significant skin needs to be addressed, incision patterns can be more extensive. This is the trade-off: better skin tightening vs potentially more visible scarring.
What determines how visible scars become
When patients search “gynecomastia surgery scars”, they’re usually worried about two things: scar color and scar thickness. Several factors influence both:
- Skin type and genetics: Some people are more prone to thick or raised scars.
- Tension on the incision: High tension can worsen scar quality. Closure technique and aftercare matter.
- Aftercare and activity: Early heavy movement, friction, or poor compression compliance can stress healing tissue.
- Sun exposure: UV exposure on new scars can lead to prolonged discoloration.
Scar healing timeline (what “normal” looks like)
Scar maturation is gradual. A common pattern looks like this:
- Weeks 1–4: incisions seal and early redness is normal.
- Weeks 4–12: scars may look pink/red and feel firmer as remodeling begins.
- Months 3–12: scars typically soften and fade; final appearance often continues improving over time.
Individual healing varies, and that variability is exactly why scar strategy should be discussed before surgery—not after.
Our scar-optimization logic (realistic, not “scar-free” marketing)
We approach scars with a simple philosophy: place incisions intelligently, close with low tension, and protect healing during the most sensitive window. That includes clear guidance on compression garment use, activity limits, and skin care during recovery. We avoid “no-scar” promises because they’re not medically honest.
Scar outcomes are shaped as much by planning and aftercare as by the incision itself. Discreet placement and low-tension closure matter—but so does protecting the healing phase.

Recovery Timeline: How Long Does Healing Take?
Gynecomastia surgery recovery time depends on your technique (lipo-only vs combined vs skin management), your baseline health, and how closely you follow aftercare. Most patients can return to light daily activity quickly, but full athletic recovery is staged. The goal is not just “getting back to normal,” but protecting the contour while swelling resolves and tissues settle.
Important: The timelines below are typical ranges—not guarantees. Your surgeon’s instructions should always override generic timelines.
The first 72 hours (swelling control and protection)
- Expect swelling, bruising, and soreness.
- Compression is usually continuous (unless your team instructs otherwise).
- Short walks are encouraged; heavy lifting and chest-focused movement are not.
- Sleep positioning matters—many patients do best on the back with upper body slightly elevated.
Week 1–2 (return to desk life, smart movement)
- Many patients can return to desk work within days to about a week, depending on comfort and job demands.
- Light daily activity is fine; strenuous exercise is still restricted.
- Garment discipline continues—this is a key period for smooth contour settling.
- Swelling can fluctuate throughout the day; this is normal.
Weeks 3–6 (structured return to training)
- Lower-body cardio and gentle conditioning are often reintroduced first.
- Upper-body and chest training typically returns later and gradually.
- If you push too hard too early, you can prolong swelling and compromise comfort.
Months 3–12 (final definition and scar maturation)
- Definition becomes clearer as swelling continues to resolve.
- Scar color and texture continue to evolve—often improving for many months.
- Minor asymmetries often become less noticeable as tissues fully settle.
Compression garments, swelling, and why “patience” is part of the plan
Compression garments are not an accessory—they’re a recovery tool. They help:
- manage swelling
- support skin re-draping
- protect the early contour
- reduce friction and discomfort during daily movement
Most recovery “setbacks” are not dramatic complications—they’re small issues like inconsistent compression or returning to intense activity too soon. The most efficient recovery is usually the most disciplined one.
Our recovery support approach (HBOT + LLLT, case-dependent)
For patients who are appropriate candidates, we may support recovery using a staged “macro-to-micro” approach:
- HBOT (Hyperbaric Oxygen Therapy): used in some protocols to support oxygen delivery and overall recovery physiology.
- LLLT (Low-Level Laser Therapy): used in some protocols to support tissue recovery at a local level.
These modalities are not a substitute for surgical technique or proper aftercare, and they are not presented as guaranteed accelerators. They are supportive tools that can be integrated into a broader safety-first recovery protocol when clinically appropriate.
Quick recovery milestones (at-a-glance)
| Timeframe | What you’ll likely be doing | What you should avoid |
|---|---|---|
| 0–3 days | Rest, short walks, compression focus | Lifting, chest strain, “testing” range of motion |
| 1–2 weeks | Desk work (often), light daily activity | Gym, heavy carrying, intense cardio |
| 3–6 weeks | Gradual activity return (structured) | Aggressive chest workouts too early |
| 3–12 months | Final contour settling + scar maturation | Judging “final result” too early |
We use advanced Hyperbaric Oxygen Therapy (HBOT) to minimize downtime and supercharge your healing process. Safety is our #1 promise.
Gynecomastia Complications, Safety & Risks: Is The Procedure Dangerous?
When patients ask whether gynecomastia surgery is “dangerous,” they’re usually asking a more specific question: What can go wrong, how likely is it, and what does a responsible clinic do to reduce those risks? Male breast reduction is generally considered a routine procedure in experienced hands, but it is still surgery—meaning it carries real, predictable risks that should be discussed clearly, without fear-mongering and without sales language.
Common short-term effects (expected and temporary)
Most patients experience a normal set of post-op effects that improve as the body heals. These are not usually “complications,” but they can feel intense if you weren’t prepared.
- Swelling and bruising: typically peaks early, then gradually reduces over weeks.
- Soreness or tightness: common, especially with compression.
- Numbness or altered sensation: may occur around the areola/chest; often improves over time.
- Firmness/lumpiness: early scar tissue remodeling can create temporary firmness.
Potential complications (what we watch for)
When patients search “side effects of gynecomastia surgery”, they’re usually trying to understand these higher-stakes possibilities. Not everyone experiences them, but you should know what they are:
- Hematoma (bleeding collection): can require urgent assessment and, in some cases, intervention.
- Seroma (fluid collection): may require drainage and monitoring.
- Infection: uncommon but possible; requires prompt treatment.
- Contour irregularity: dents, residual fullness, or asymmetry—sometimes improves as swelling resolves, sometimes needs revision.
- Nipple–areola concerns: changes in sensation, shape, or position; risk varies by technique and severity.
- Scarring issues: thickened or pigmented scars in some skin types.
Most “problem stories” online come down to two categories: incomplete planning (wrong technique for the tissue type) or poor recovery discipline (compression/activity mistakes). That’s why a detailed plan and structured follow-up matter.
Risk mitigation framework (how we reduce risk)
No clinic can guarantee “zero risk.” What matters is a systematic approach designed to reduce avoidable problems:
- Pre-op screening: identifying medical risks, medication/supplement issues, and lifestyle factors like nicotine use.
- Technique selection: choosing lipo vs excision vs combined based on tissue reality—not preference.
- Bleeding control and sterility: disciplined intra-op protocols to reduce hematoma and infection risk.
- Compression and recovery structure: clear timelines, checklists, and early intervention if swelling/fluid behaves unusually.
When to contact your team urgently
During recovery from gynecomastia surgery, you should contact your team immediately if you experience:
- rapid, one-sided swelling or severe tightness
- significant bleeding through dressings
- fever, worsening redness, or foul drainage
- shortness of breath, chest pain, or sudden leg swelling (urgent medical evaluation)
Revision surgery: what it is (and what it isn’t)
Revision does not automatically mean “failure.” In some cases, a small refinement is needed for contour balance—especially in complex anatomy or advanced grades. A responsible consultation includes an honest discussion of what revision would look like, what triggers it, and how long you should wait before judging your final shape (often months, not weeks).
The safest surgery is rarely the fastest decision. Thorough assessment, the right technique, and structured follow-up are what turn “routine” into reliably safe.
Is Gynecomastia Surgery Safe in Turkey?
This is the question that determines whether a safety-conscious US patient moves forward: “Is it actually safe to do this abroad?” The honest answer is that safety is not a country label—it’s a standards-and-systems question. Turkey can offer excellent outcomes when the clinic operates with strict screening, modern facilities, experienced surgeons, and a clear continuity-of-care model.
Facility standards: what to look for (regardless of country)
When evaluating a clinic abroad, prioritize verifiable infrastructure over marketing promises. Key markers include:
- Modern operating environment: sterile protocols, controlled surgical workflow, and appropriate equipment.
- Anesthesia safety and monitoring: continuous vitals tracking and a team trained for prompt response.
- Pre-op testing pathways: not “optional,” but structured when indicated.
- Post-op monitoring: clear discharge criteria and accessible support.
Surgeon vetting: how to evaluate expertise as an “expert patient”
For a patient comparing options internationally, “best” should mean qualified + consistent + transparent. Look for:
- Specialization and case familiarity: gynecomastia requires aesthetic judgment, not just tissue removal.
- Planning discipline: clear explanation of tissue type, scar strategy, and why a chosen technique fits your anatomy.
- Before/after realism: results that match your body type and severity grade, not only “easy cases.”
- Clear risk discussion: a surgeon who acknowledges trade-offs tends to be safer than one who overpromises.
Privacy and confidentiality (especially for international patients)
Many patients want discretion. A professional clinic should treat privacy as a standard—not a premium feature. That includes secure handling of consultation photos, confidential communication, and respectful, patient-first service throughout your visit.
Continuity of care after you fly home
One of the biggest fears about medical travel is, “What happens if I have a question at home?” A responsible international model includes:
- Structured follow-ups: scheduled check-ins (often virtual) with clear timelines.
- Clear escalation pathways: what’s normal, what’s not, and when to seek local assessment.
- Recovery documentation: instructions that are specific, not generic.
This is also why you should avoid clinics that minimize recovery guidance or treat follow-up as an afterthought.
What you can do to make your trip safer
- Plan realistic downtime: don’t schedule intense tourism immediately after surgery.
- Follow garment and activity rules: recovery discipline protects contour and reduces complications.
- Be honest in your medical history: the safest plan depends on accurate information.
- Choose value, not the lowest price: the “expert patient” wins by selecting systems, not bargains.
If you’d like an expert-level review of your case, we offer a virtual consultation where we evaluate your tissue pattern, scar tolerance, downtime needs, and the most appropriate technique—then provide a clear plan and a transparent quote.
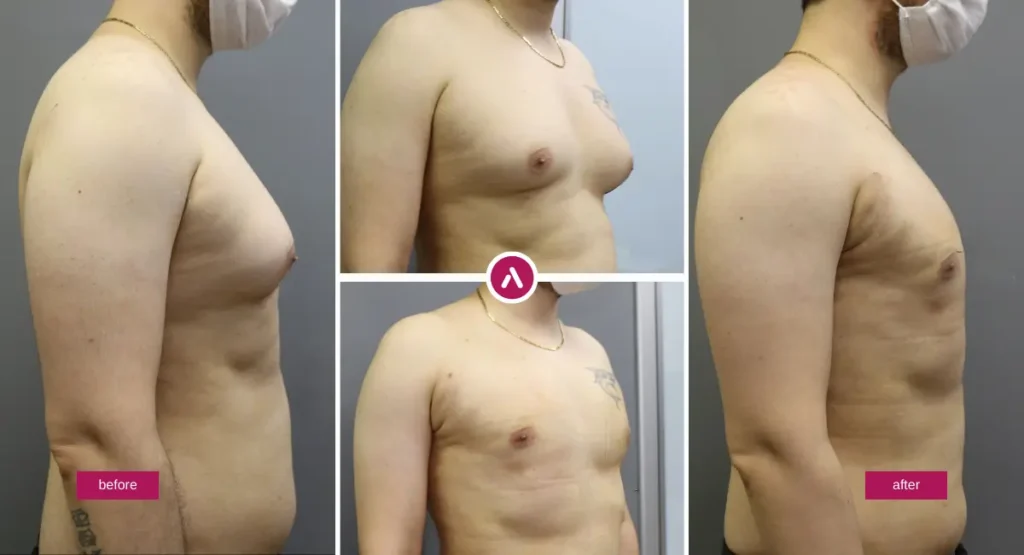
Gynecomastia Surgery Before and After Results: What “before and after” Really Means
“Before and after” photos are useful—but only when you read them like an expert. The most impressive image isn’t always the most relevant one. The best comparison is a patient with a similar tissue pattern (fat vs gland vs mixed), similar skin quality, and a similar severity level. That’s how you set expectations that feel realistic on your body, not just in someone else’s lighting.
When results look “final” (and why early photos can be misleading)
Most patients feel noticeably better early, but the chest continues to evolve. Swelling, firmness, and subtle contour changes are normal parts of healing.
- Early phase (weeks): swelling and bruising dominate; the chest may look “better” but not settled.
- Mid phase (months): swelling reduces, contour becomes clearer, and the chest starts to feel more natural.
- Later phase (up to a year): scars mature and fine details continue to refine.
This is why a responsible clinic discourages judging the final outcome in the first few weeks.
What surgery can and cannot do
Gynecomastia surgery can reduce projection and reshape the chest to a more masculine contour. But it does have limits. Being clear about those limits protects you from disappointment.
- It can: remove gland tissue, reduce fat, improve chest outline, and address skin excess when appropriate.
- It cannot: guarantee perfect symmetry, permanently prevent all future tissue changes, or override poor skin quality without trade-offs.
If you have significant skin laxity, the best contour may require accepting more visible scars. If you prioritize minimal scarring, you may accept a softer result. That’s not a flaw—it’s aesthetic decision-making.
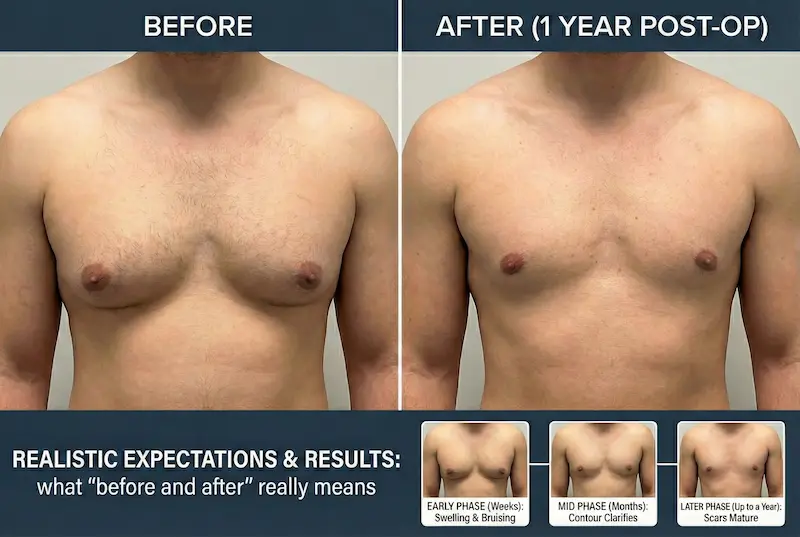
How to evaluate “before and after” photos like an expert
- Match the case: look for similar severity and skin quality, not just the “best looking” outcome.
- Check angles: front and side views matter; side views show projection changes clearly.
- Look for natural transitions: chest to underarm blending should be smooth (no dents, no sharp “step-offs”).
- Watch the areola: a natural outcome usually keeps the nipple–areola complex looking proportional and undistorted.
Our “Natural-First” philosophy applied to male chest shaping
We plan for results that look unforced—like your chest should have always looked that way. That means we prioritize proportion, smooth blending, and a contour that matches your frame and skin behavior.
Great results don’t announce themselves. They blend into your physique so the outcome looks natural from every angle—especially in normal lighting.
Get a 100% transparent, all-inclusive quote tailored to your needs. No hidden fees—just world-class care at an accessible price.
Cost Analysis: Gynecomastia Surgery Prices (Turkey vs USA) — 2026
Cost is one of the most searched topics for this procedure because prices vary widely by location and case complexity. The most useful approach is to understand what drives the price, then compare value based on what’s included, what standards are in place, and how continuity of care is structured.
What drives the cost of gynecomastia surgery
- Severity and technique: lipo-only, excision, combined approaches, and whether skin management is needed
- Anesthesia plan: local/tumescent, twilight sedation, or general anesthesia (case-dependent)
- Facility standards and safety protocols: operating environment, monitoring, and staff expertise
- Pre-op testing and post-op support: screenings, garments, medications, follow-up structure
- Revision risk and complexity: advanced cases may require more planning and a longer surgical time
USA cost reality (why the range is so wide)
In the US, pricing can vary dramatically by city (especially premium markets), surgeon demand, facility fees, and whether the case needs excision, skin work, or revision-level refinement. That’s why “gynecomastia surgery cost US” and “gynecomastia surgery cost NYC” searches are so common—patients are trying to benchmark.
Rather than focusing on a single number, a better question is: What am I paying for, and what is included? Transparent quotes should clearly separate surgeon fees, anesthesia, facility costs, garments, and follow-up.
Why Turkey can be a high-value option (without “cheap surgery” positioning)
Turkey is often more cost-efficient because operational costs and local pricing structures differ—not because safety or technique should be lower. For the expert patient, “value” means: qualified surgical planning, modern facilities, structured aftercare, and a clear continuity-of-care model—at a total cost that can be meaningfully lower than many US markets.
What’s typically included in our VIP approach (and what is not)
To make planning easier for international patients, we structure a consolidated experience. In practice, details can vary by case, so your quote should always specify exactly what’s included.
| Cost Component | Typically Included | Typically Not Included / Varies |
|---|---|---|
| Surgeon evaluation + planning | ✓ | — |
| Pre-op checks (as indicated) | ✓ (case-dependent) | Additional specialty tests if required |
| Procedure + operating facility | ✓ | — |
| Anesthesia / sedation | ✓ (as planned) | Changes if the plan changes clinically |
| Compression garment | ✓ | Extra garments (optional) |
| Medications (standard post-op) | ✓ | Non-standard or extended prescriptions |
| Hotel + transfers | ✓ (package-dependent) | Upgrades or extended stay |
| Follow-up (including virtual) | ✓ | Local care in your home country (if needed) |
| Flights | — | Typically not included |
Insurance coverage (USA): what patients should know
Many patients ask, “Is gynecomastia surgery covered by insurance?” In the US, coverage depends on whether the case is considered medically necessary under your plan’s criteria (and documentation). Some plans view it as cosmetic unless strict medical-necessity standards are met. If insurance coverage is important to you, request your plan’s written criteria and discuss documentation requirements with a qualified medical provider.
How to compare quotes ethically (and safely)
- Demand clarity: ask for an itemized list or a clear “included/not included” breakdown.
- Compare like-for-like: technique, anesthesia, facility standards, and follow-up must be comparable.
- Don’t chase the lowest price: the expert patient optimizes for safety systems and consistent outcomes.
If you want a precise quote, the most accurate next step is a virtual consultation. We evaluate your tissue pattern, skin behavior, scar tolerance, and downtime needs—then outline the recommended technique and provide transparent pricing based on your case.

Finding The Right Surgeon: How To Vet Expertise
If you’re the kind of patient who reads studies, compares techniques, and audits reviews, you’re already doing the right thing: you’re treating this like a medical decision, not a shopping decision. The goal isn’t to find the loudest marketing. It’s to find a best surgeon (and a system) that consistently produces natural outcomes—and can explain why a specific plan fits your anatomy.
Credentials are the starting line, not the finish line
Credentials matter, but they’re not the entire story. Look for a surgeon who operates in a properly equipped facility, follows structured screening, and demonstrates clear surgical judgment. In an expert consultation, you should hear precise reasoning—not vague reassurance.
Case familiarity: why gynecomastia is not “just liposuction”
Gynecomastia correction is part contouring, part tissue management, part aesthetic restraint. The surgeon must know when liposuction is enough, when gland removal is necessary, and when skin management is required. The difference between an average result and a great one often comes down to:
- how smoothly the chest blends into the underarm area
- how the areola sits on the new contour
- how over-resection (dents) is avoided
- how symmetry is respected without chasing impossible perfection
Perform your surgery with confidence. Meet our European Board Certified surgeons with over 2,000 successful facial surgeries.
What to ask in a consultation (expert-level questions)
These questions are designed to force clarity—so you’re not left with generic promises:
- “Is my issue mostly fat, gland, or mixed?” Ask for a clear explanation of why.
- “Which technique do you recommend—and what’s the trade-off?” (Scars vs skin tightening vs downtime.)
- “Where will incisions be placed, and what’s your scar strategy?”
- “How do you prevent dents or contour irregularities?”
- “How long should I wait before judging the final result?”
- “What does follow-up look like if I’m traveling?” (This is a big safety filter.)
How to read reviews and results without getting misled
- Watch for consistency: one amazing result is less meaningful than repeated, predictable outcomes.
- Look for your “match”: similar severity, skin quality, and body type matter more than “best photo.”
- Beware perfection language: clinics that promise flawless symmetry or “no scars” are not speaking medically.
Red flags that experienced patients don’t ignore
- Overpromising: “scar-free,” “zero risk,” “guaranteed perfect symmetry.”
- Vague planning: no clear explanation of why a technique fits your tissue type.
- Weak follow-up structure: unclear instructions, no scheduled check-ins, or “you’ll be fine” messaging.
- Price-first pressure: discount urgency instead of medical clarity.
Plan first, operate second. The best outcomes come from precise diagnosis, a tailored technique, and a recovery structure that protects the result.
Get a clear, day-by-day itinerary covering arrival, surgery, recovery, and fit-to-fly clearance tailored to your schedule.
Your Medical Journey With Us: Arrival To Departure (and beyond)
For international patients, a successful experience is not only about the operation—it’s about medical journey, logistics, safety checks, and continuity of care. Our process is designed to feel structured and calm, with clear steps before you travel, during your stay in Istanbul, and after you return home.
Step 1: Virtual consultation (expert-level case review)
We start with a virtual consultation so you can get clarity before committing to travel. The aim is to answer the questions that actually matter:
- your likely tissue pattern (fat vs gland vs mixed)
- the most appropriate technique (lipo-only, excision, combined, or skin management)
- scar expectations and placement strategy
- a realistic recovery timeline based on your lifestyle
- transparent pricing and what’s included
If you’ve done your research, this step should feel like a “final synthesis” rather than a sales call.
Step 2: VIP planning (travel, scheduling, and simplicity)
Once your surgical plan is confirmed, the next step is making the trip feel effortless and predictable—especially for patients flying in from the US. Our VIP planning is designed to remove logistical stress so you can focus on recovery, not coordination.
Depending on your selected package and your timeline, VIP planning may include:
- Date coordination: aligning consultation, pre-op checks, surgery, and follow-up checks into a clear itinerary
- Hotel planning support: arranging a comfortable recovery-friendly stay (and upgrades/extended nights if requested)
- Private transfers: airport-to-hotel, hotel-to-clinic, and clinic-to-hotel logistics to keep travel smooth and discreet
- Pre-travel checklist: guidance on medications/supplements to disclose, nicotine considerations, and what to pack for recovery (compression-friendly clothing, etc.)
For the “expert patient,” the key value of VIP planning is not luxury—it’s risk reduction through structure. A clear schedule, reliable transport, and a recovery-oriented setup help you protect the result and avoid unnecessary strain in the first days.
Step 3: Arrival in Istanbul (airport welcome and private transfer)
On arrival, patients are typically met and transferred privately to the hotel. This reduces friction—especially after a long flight—and supports a calm start to your medical trip. If you prefer maximum discretion, private transfers also help you avoid unnecessary delays and crowded routes.
Step 4: Pre-op checks and final confirmation
Before surgery, we confirm the plan in person: your goals, technique choice (lipo vs excision vs combined, and whether any skin management is needed), incision/scar strategy, and your recovery timeline. If anything has changed since your virtual consultation—new medications, recent illness, or new symptoms—this is where we reassess and adjust. Safety always comes first.
Step 5: Surgery day + post-op monitoring
After the procedure, you’ll receive a clear aftercare plan (compression, activity limits, sleep positioning, and warning signs to watch for). Early monitoring focuses on patterns that matter: unusual swelling, fluid behavior, discomfort that doesn’t match the expected recovery curve, or anything that suggests a complication needs evaluation.
Step 6: Final check before flight
International patients often ask, “When can I fly?” The answer depends on your surgery details and how your early recovery is progressing. A final check helps confirm you’re comfortable for travel, swelling is within expectations, and you fully understand the next phase of recovery once you return home.
Step 7: Follow-up after you return home (continuity of care)
Continuity is one of the biggest safety differentiators in medical travel. After you return home, we continue with structured remote follow-ups (often at milestones such as 1, 3, 6, and 12 months). These check-ins help track contour settling, scar maturation, and recovery progress—so you’re not left guessing whether something is “normal.”
If anything looks outside the expected range, we guide you on the next step—whether that’s a simple adjustment to your routine, an additional virtual review, or local evaluation when appropriate.
Gynecomastia Surgery Frequently Asked Questions (FAQ):
What is gynecomastia surgery?
Gynecomastia surgery is a procedure that reduces enlarged male breast tissue by removing gland tissue, excess fat, or both. In some cases, it also addresses loose skin to restore a flatter, more masculine chest contour.
What’s the typical gynecomastia surgery recovery time?
Recovery varies based on technique (lipo-only vs combined vs skin management) and your healing profile. Many patients return to desk work within days to about a week, while full athletic activity is typically reintroduced gradually over several weeks. Final contour settling and scar maturation can continue for months.
Does gynecomastia surgery leave scars?
Yes—any surgical incision creates a scar. In most standard cases, scars are designed to be discreet (often at the areola border and/or tiny access points for contouring). Visibility depends on incision placement, skin type, tension, and aftercare. Scars typically continue to fade and soften over time.
Is male breast reduction surgery safe?
In experienced hands and in an appropriate medical setting, male breast reduction is generally considered a routine procedure. That said, it is still surgery and carries real risks (bleeding, infection, fluid collection, contour issues). Safety depends on proper screening, the right technique for your tissue type, careful intra-operative control, and structured follow-up.
What are the side effects of gynecomastia surgery?
Common short-term effects include swelling, bruising, soreness/tightness, and temporary numbness or altered sensation. Potential complications can include hematoma, seroma, infection, scarring issues, contour irregularities, and changes in nipple–areola sensation. Your surgeon should explain which risks are most relevant to your anatomy and plan.
Can gynecomastia come back after surgery?
True recurrence is not common, but future changes can happen depending on underlying causes (hormonal shifts, certain medications, significant weight change, or anabolic steroid use). A thorough evaluation and addressing avoidable triggers helps reduce recurrence risk.
Is gynecomastia surgery covered by insurance?
In the US, coverage depends on your plan and whether the surgery is classified as medically necessary (based on specific documentation criteria). Many plans consider it cosmetic unless strict requirements are met. If insurance matters to you, request your plan’s written criteria and discuss documentation with a qualified medical provider.
How much does gynecomastia surgery cost in the USA vs Turkey?
Pricing varies widely by city and case complexity in the USA, and it also varies internationally based on technique, facility standards, anesthesia plan, and the level of post-op support. The most reliable comparison is based on a transparent, itemized quote that clarifies what is included (facility, anesthesia, garments, follow-up, and—if traveling—transfers/hotel if offered).
How long do I need to stay in Istanbul for gynecomastia surgery?
Length of stay depends on your surgical plan and early recovery progress. Many international patients plan several days to allow for surgery, early check-ups, and a final assessment before flying. Your team should advise a realistic timeline based on your case and travel needs.
Do I need drains?
Some patients do, many do not. Drains may be used if tissue removal is more extensive or if your surgeon believes it will help reduce fluid accumulation. The decision is individualized and should be discussed in your consultation.
When can I go back to the gym?
Return to training is gradual. Light activity and walking start early, while upper-body and chest-focused training typically comes later and is reintroduced in stages. Pushing too hard too soon can prolong swelling and compromise comfort. Follow your surgeon’s specific timeline.
What should I ask during a virtual consultation?
Ask what tissue type is driving your chest shape (fat vs gland vs mixed), which technique is recommended and why, where incisions will be placed, what scarring should realistically look like, what your recovery timeline is, and how follow-up works once you’re back home.
Medical Disclaimer: Information on this page is for educational purposes only and does not replace medical advice. Gynecomastia Surgery outcomes, risks, recovery, and costs vary. Only a qualified surgeon can determine suitability after an in-person evaluation. If you have urgent symptoms, seek emergency care immediately.
Gynecomastia Surgery: Patient Stories

Mrs. Giordano
Gynecomastia Surgery Surgeons
Gynecomastia Surgery Cost in Turkey
Starting from $3700
* There are no hidden fees or unexpected charges.
- Your Personalised Gynecomastia Surgery Procedure
- All Specialist Surgeon & Anesthesia Fees
- All Pre-Op Tests & Post-Op Check-ups
- 5-Star Hotel Accommodation (incl. breakfast)
- All Private VIP Airport & Clinic Transfers
- 24/7 Dedicated Patient Coordinator & Translation Services
Gynecomastia Surgery: A Cost Comparison
| City | Cost |
|---|---|
| New York City | 8.500 USD |
| Los Angeles | 11.000 USD |
| San Francisco | 12.000 USD |
| Seattle (Seattle–Tacoma) | 8.000 USD |
| Houston | 10.000 USD |
Discover Our All-Inclusive Packages in Turkey
Gynecomastia Surgery: Patient Reviews
Jammal Canada
I have had face and neck lift with AKM Clinic they have been so good to me and my operation went so smoothly🥰 i would like to thank my doctor here and also to the team 💐

Ava Canada
Thank you AKM Clinic for giving me my confidence back! Had facelift + temporal lift 3 months ago and the outcome is already stunning. Special thanks to Hande!

Jakayla USA
Had a deep plane facelift and lower eyelid procedure at AKM Clinic 7 months ago. The results are fantastic - very subtle and natural. I didn’t expect the entire experience to be so comfortable. Hande managed everything and kept in contact even after I returned to USA. I’m beyond pleased with the outcome and the care I received. Would do it again in a heartbeat!

Barbara United Kingdom
It has been 4 months since my surgery. Everything is great, The most important thing is l love the way l look, l look exactly how l wanted. Meaning l look natural, just almost 40 years younger. I pulled Facebook - majority voted 37ys. I also had face, neck, chest, and hands CO2 laser. My skin is flawless.

Lisa Canada
I had a face, neck and arm lift at AKM. I’m just over 4 weeks post and couldn’t be happier with the results. The entire experience was wonderful! My coordinator, Khadija made me feel comfortable from beginning to end! I highly recommend AKM and will definitely go back for other procedures!

Julie USA
I am beyond grateful I went with AKM Clinic for my deep plane face and neck lift, upper eyelid, and co2 laser. Dr. Akif has magic hands and my results are truly incredible! I came from the US and assistant Emine was the best in assuring every detail was coordinated and communicated with me beyond my expectations every step of the way. 10 out of 10 to the entire team! I couldn’t be more pleased!

Ready to Start Your Own Transformation Journey?
Join the 2,000+ patients who trusted Dr. Akif Mehmetoğlu and the AKM Clinic team. Your journey to a more confident, revitalized you begins with a simple, no-obligation conversation. Contact us today from the USA for your free virtual consultation.
#1: Get Your Free Personalised Quote
Start with a free, no-obligation online consultation. Share your photos, and our surgical team will provide a fully personalised treatment plan and a transparent, all-inclusive price package. No hidden fees.
#2: Secure Your Date & VIP Booking
Once you're ready, our dedicated patient coordinators will help you secure your procedure date. We'll handle all your bookings, including your 5-star hotel and private VIP airport transfers.
#3: Arrive in Istanbul & Meet Your Surgeon
Arrive at Istanbul Airport (IST) and be greeted by your private driver. Settle into your hotel and prepare for your in-person consultation, where you'll meet your specialist surgeon to finalise the details for your "natural, subtle, and revitalized" new look.
















